
Snakebites kill tens of thousands of Africans a year
An antivenom shortage is spurring global experts to collaborate on treatment and prevention.
Simon Isolomo awoke around 5 a.m., said goodbye to his wife and seven children, and climbed into his dugout canoe. That Tuesday in December 2018 had begun like many others in Isolomo’s 30 years of fishing in the province of Équateur, in the Democratic Republic of the Congo. Paddling on the Ikelemba River toward his fishing camp with a couple of friends, Isolomo, a 52-year-old French teacher, snacked on kwanga, a popular manioc dish, and enjoyed the cool morning air.
Three hours later they arrived at the camp, and Isolomo began checking the fishing lines he’d set up the day before. Feeling resistance on one, he thrust his hand into the murky water.
A sharp pain sent him reeling. Blood oozed from two puncture wounds on his hand. Just below the surface, a yellowish snake with black rings—probably a banded water cobra—slithered from view.


Isolomo’s companions helped him into the canoe and paddled frantically back to their village of Iteli. By the time they arrived, about three hours after Isolomo was bitten, he was slipping in and out of consciousness.
“His eyes had changed color, and he was vomiting,” his wife, Marie, recalls, starting to cry. After a traditional healer applied a tourniquet, they set out by canoe for the hospital in Mbandaka, the provincial capital, some 60 miles away. But before they arrived, Isolomo stopped breathing and died.
Isolomo’s story encapsulates the global snakebite crisis: Bitten in a remote area, hours from the closest hospital, he didn’t have a chance. As many as 138,000 people around the world die from snakebites each year, according to the World Health Organization (WHO), and roughly 95 percent of those deaths occur in poor, rural communities in developing nations. Another 400,000 people survive with amputated limbs and other permanent disabilities.
One of the worst-hit locations is sub-Saharan Africa, where up to 30,000 deaths from snakebites are believed to occur each year. But some doctors and snakebite experts say the true toll may be double that. A major factor is a severe shortage of the only medicine that can neutralize the toxins of dangerous snakes: antivenom. Complicating matters is that many victims, for lack of money or transportation, or because of distrust of Western medicine, don’t go to hospitals—or don’t get there in time. Staff at many health centers are insufficiently trained to treat snakebites, and even if the drug is on hand, it’s too expensive for many victims. Additionally, most of the more reliable African antivenoms need to be kept refrigerated to stay stable and effective. With frequent power cuts, even in cities, keeping them cold can be nearly impossible.
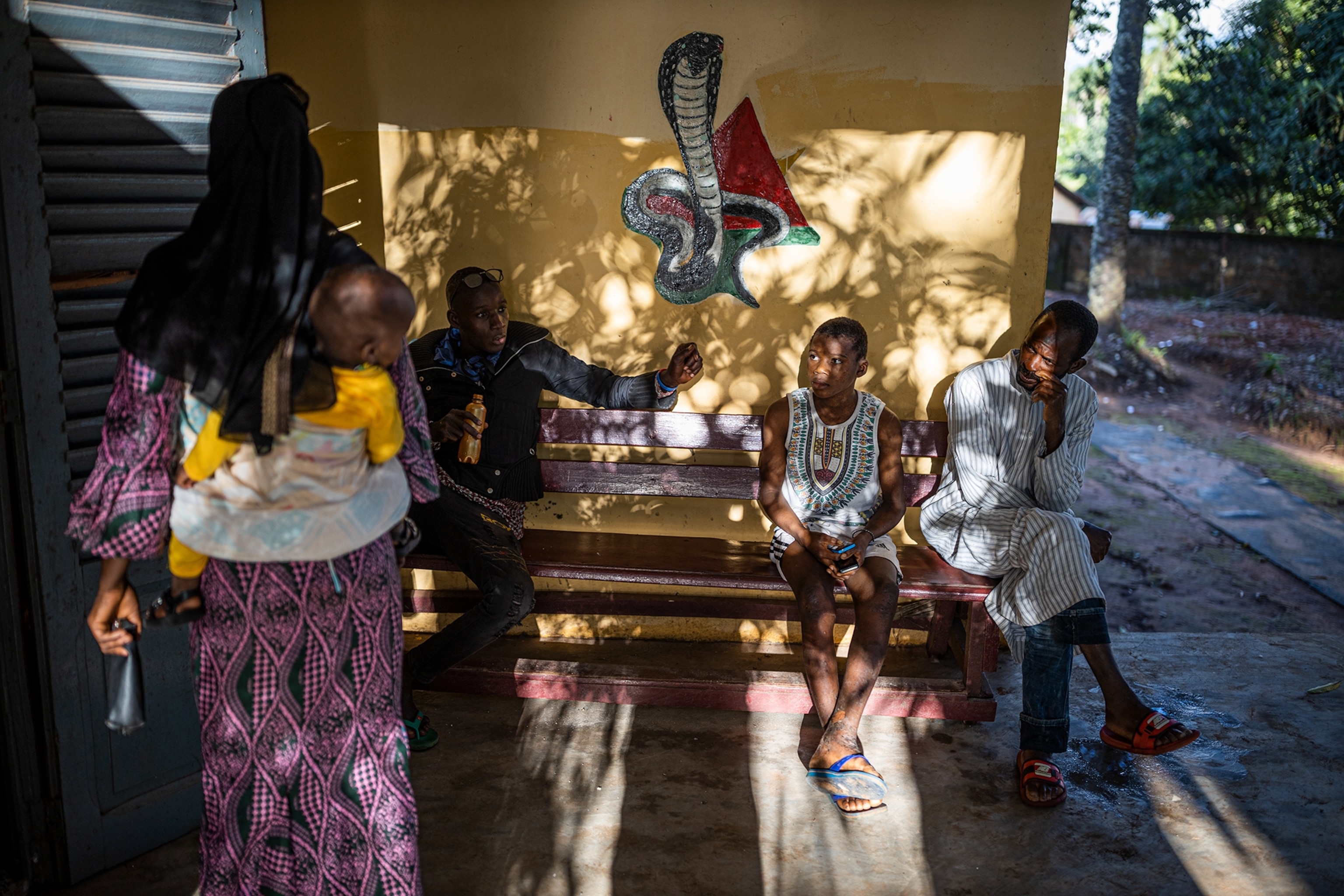
To draw attention to the snakebite crisis and to attract funding for research and treatment, in 2017 WHO added snakebite envenomation to its roster of neglected tropical diseases, which includes rabies, dengue, and leprosy. In 2019 it announced a goal of slashing the number of annual deaths and disabilities from envenomation by 50 percent by 2030—an undertaking that could cost nearly $140 million.
Elevating snakebites to this level of concern will serve as a wake-up call to Africa’s health ministers, says Mamadou Cellou Baldé, 66, a Guinean biologist and research director at the Guinean Institute for Applied Biological Research (IRBAG), in Kindia, which runs a snakebite clinic. Baldé and other experts have long tried to alert authorities to the severity of this deadly crisis and the desperate need for antivenom research and development—with little success.
“We see millions being spent to rig even local elections, while in the meantime African scientists lack money to do lifesaving research,” Baldé says.
Most African snakebite victims are farmers who work in remote fields barefoot or in sandals, making them particularly vulnerable. Once a venomous snake strikes, a race against the clock begins. Transport to the nearest hospital can take hours, even days. By then it may be too late.
The venom of elapids, a family of snakes that includes mambas and cobras, can kill within hours. Their neurotoxins rapidly paralyze respiratory muscles, making breathing impossible. The venom of vipers, however, can take several days to kill, interfering with clotting and leading to inflammation, bleeding, and tissue death. (Learn more: What’s the most venomous snake in the world?)
Once the victim is at a treatment center, survival depends on two vital points: Is a reliable antivenom available? And if so, does the medical staff know how to administer it? Often in sub-Saharan Africa the answer to both is no.
Some people aren’t taken to a hospital at all. Families may seek help instead from a traditional healer, who may apply leaves or ash from burned animal bones, or tie a tourniquet around the bitten limb, which can dangerously restrict blood flow. Some botanical treatments do ease pain and reduce swelling, but they can’t save a victim’s life, Baldé says.


Even so, snakebite survivors may credit traditional healers with saving their lives. About half of the bites from venomous snakes are dry, with no venom injected, says Eugene Erulu, a physician at Watamu Hospital in southern Kenya, “so these patients get well, and the traditional healer believes that he has healed the patients.”
About 25 years ago Baldé was taking a break under a mango tree at IRBAG when a frantic man ran up to him carrying an unconscious child. She’d been bitten by a snake, he said.
Baldé, then an entomologist studying vector-borne diseases, brought the 12-year-old into the clinic, but there was no hope. The institute had been a snakebite treatment center in the early 1900s, but by mid-century its focus had shifted. No one knew how to help the child.
“I was naturally shocked,” Baldé says. It was a failure of duty to let people die like this.
He vowed this girl would be the last such victim. He turned his focus from insects to snakes and began learning all he could about snakebites.
In his search for treatments through the years, Baldé, now a world-renowned herpetologist and lecturer on snakebites, has experimented with products available locally: Chinese-made pills and inexpensive injections of Indian-made antivenoms. He says the best he found was Fav-Afrique, an antivenom made by French pharmaceutical company Sanofi, which was effective against the venom of 10 of Africa’s most dangerous snakes. But in 2014 Sanofi discontinued production because the medicine wasn’t profitable.
More than 100,000 people die each year from snakebites. About 95 percent of those deaths occur in poor, rural communities in developing nations.


Producing antivenoms is a long, expensive process, and because the vast majority of people who need them live in developing countries, such drugs are not big moneymakers.
Antivenom production requires actual venom. This comes from labs that may house thousands of snakes in captivity. They’re milked about once a month for their venom. Depending on the species, venom can cost a pharmaceutical company up to several thousand dollars a gram.
Then the venom—in amounts too small to have deleterious effects—is injected into horses or other large mammals, whose blood develops antibodies. Blood is drawn, and lab technicians separate out the antibodies and purify them to make antivenoms.
Even with a high-quality antivenom, treating snakebites can be hit or miss: The chemical makeup of venom and its effects can vary from snake to snake, even within a species. “There’s a huge lack of published data and research,” says Jordan Benjamin, founder of the U.S.-based Asclepius Snakebite Foundation, which provides supplies and training to African clinics.
“Sometimes antivenoms that are supposed to treat certain species don’t even work in some areas,” says Colorado-based medical toxicologist Nick Brandehoff, the foundation’s medical director. For example, “the puff adder’s venom can change from one area to another. It’s extremely complicated.”

By 2013, a company in Mexico, Inosan Biopharma, was marketing a new antivenom, one that can neutralize the toxins of at least 18 snake species—more than almost any other available antivenom in Africa.
“You can treat even if you’re not sure which snake caused the bite,” Benjamin says. And it has an extremely low rate of severe side effects, which is a common problem with other antivenoms.
The drug, Inoserp Pan-Africa, also is advantageous in that it’s freeze-dried. Not needing refrigeration is “a game changer,” says Baldé, one of the first health-care providers to test it in the field. (Learn more about a promising multispecies antivenom for Asian snake species.)
For all its effectiveness, Inoserp is not being produced in sufficient quantities. There’s a severe shortage of antivenoms more broadly: The number of vials in circulation is less than 5 percent of the one million to two million needed yearly in sub-Saharan Africa. And even if Inoserp were widely available, rural Africans—whose earnings may be no more than a few dollars a day—couldn’t afford it. Hospitals and pharmacies might charge $80 to $120 or more a vial, and most snakebite victims require several vials. (Read about the challenges of treating snakebites in the Amazon.)
Cheaper antivenoms are available but often are unreliable. “In several African countries we came across antivenom designed to treat bites from Indian snakes,” says Jean-Philippe Chippaux, a tropical diseases expert at the French National Research Institute for Sustainable Development, who helped write WHO’s snakebite strategy and has contributed to the development of antivenoms, including Inoserp.

“Governments should offer financial support,” Chippaux says. “They should make antivenom cheaper so that people can be treated—the cost is a major problem.”
Inosan Biopharma is investing millions of dollars to ramp up production of Inoserp, hoping African governments eventually commit to buying sufficient amounts to counter the crisis. “So far, we’re not making a profit on Inoserp,” CEO Juan Silanes says. “Someone had to start investing, and we took that on, but we’re proud of what we’re doing because it’s an important cause.”
Other companies around the world also are researching new treatments, but nothing is as far along or as promising as Inoserp at the moment, Benjamin says. Some philanthropic organizations are stepping in where government support lags. Asclepius Snakebite Foundation, for example, provides free Inoserp and medical training to health centers in Guinea, Kenya, and Sierra Leone. The James Ashe Antivenom Trust buys antivenoms for hospitals in Kenya’s Kilifi County so patients can get free treatment.
But, as Baldé says, preventing snakebites is better than having to treat them. Public awareness campaigns in Guinea and elsewhere echo what he tells his patients: Wear shoes when walking in places likely to have snakes, and use a flashlight at night.
“Snakebite has been a disease of the poor, so the policymakers don’t care,” Watamu Hospital’s Erulu says. But he hopes WHO’s new global investment in snakebite prevention will be effective. “Governments are going to be forced to look at it as a serious problem,” he says. “That is a very, very important step.”
The nonprofit National Geographic Society helped fund this article.
This story was updated on November 17, 2020.



