
In Nairobi, quarantine is a luxury few can afford
As COVID-19 takes hold in Kenya’s capital, hundreds of thousands living in cramped informal settlements are especially vulnerable.
Nairobi, Kenya — Driving through Kenya’s capital city during the time of coronavirus is like moving between two disconnected realities. Neighborhoods such as Muthaiga and Karen are silent—their streets deserted, their occupants invisible inside lush compounds, their houses well stocked with food and other necessities. A few miles southwest of downtown is Kibera, home to a quarter of a million people surviving together beneath tin roofs. Kibera is the largest of the more than a hundred informal settlements in Nairobi, where the vast majority of people scrape by on no more than a few dollars a day.

Kenya is one of the world’s most unequal societies. Less than 0.1 percent of the country’s 53 million people own more wealth than the other 99.9 percent.
Each morning in Kibera, Zedekia Agure wakes before the sun in the windowless, one-room home he shares with his wife and five children. White, rose-lace curtains cover the bare walls; the wood of the family’s single table has been polished until it gleams. Like most other families in this sprawling community, the Agures have no running water and must use a communal toilet. Zedekia and his wife, Sarah, run a small stand outside their home where they sell hand soap, packaged sweets, used clothing, and other items.
For Zedekia and Sarah, antibacterial sanitizers and protective masks are an expense beyond their reach, and self-quarantining against the coronavirus simply isn’t a choice. “How will we earn our daily bread?” Zedekia asks. “What happens if one of us falls sick?”


The Agures are participants in the vibrant, informal Kenyan marketplace, which in Kiswahili is called jua kali (“fierce sun”). Eight out of 10 citizens depend on the marketplace for food, medicine, housing, and schooling. Jua kali is all hustle—high-speed, small-scale, day-to-day transactions between people. This way of life offers no social safety net, no systematic protection against a disaster such as a novel coronavirus.
Though COVID-19 hit richer parts of the world first, cases across Africa are rising fast. Egypt was the first country in this continent of 1.2 billion people to confirm a case, on February 14. Less than two months later, the outbreak appears to have reached almost every other African nation. On April 10, Kenya reported a cumulative total of 184 cases and seven deaths. How many people in Nairobi—and Kenya as a whole—may actually be infected is unknown because only about 5,500 people have been tested. (See how the virus has spread around the world.)

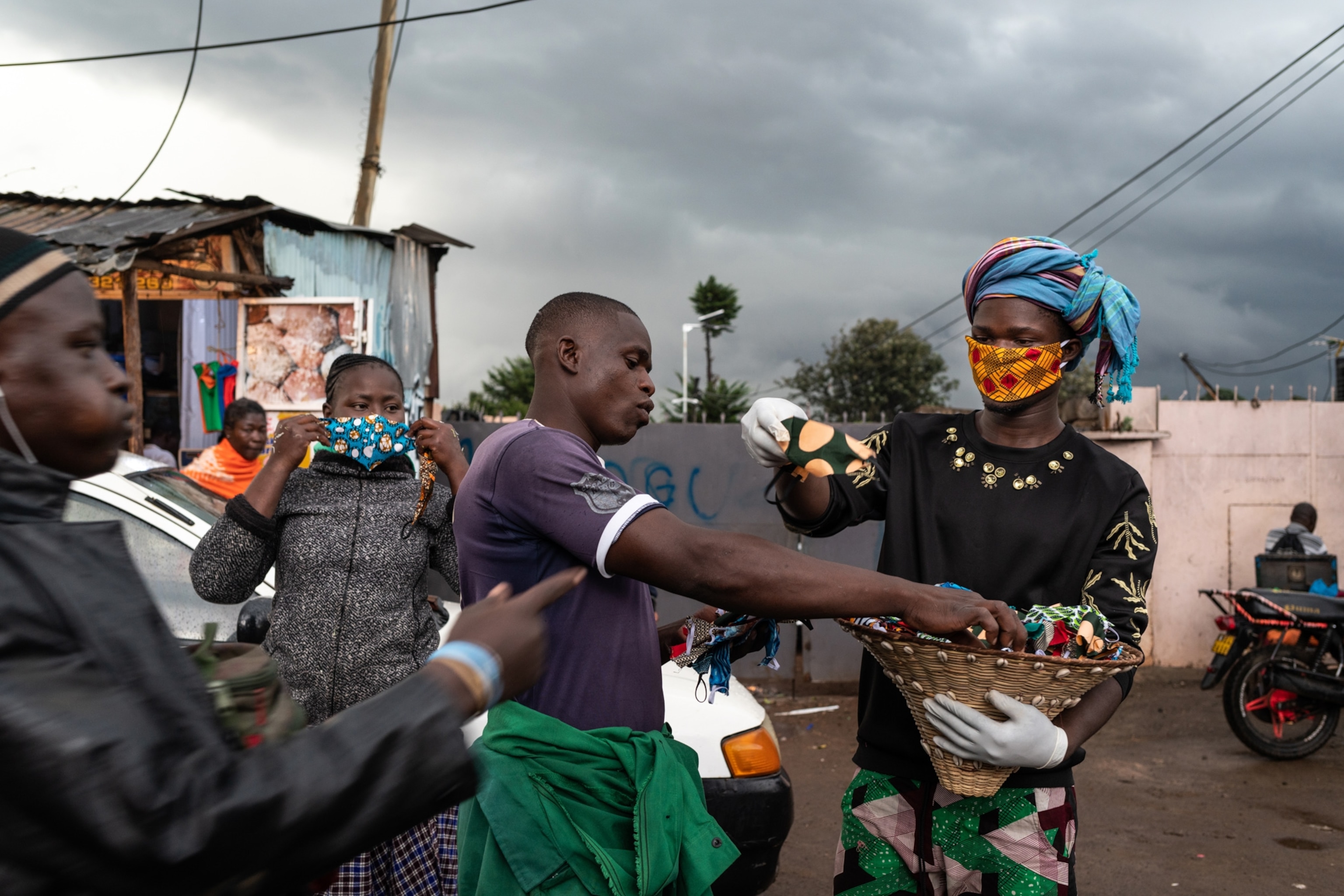

“Even these small number of [reported] cases are more than we can handle,” one paramedic in the city told me. “When the numbers really start to rise, people will be dying in the streets.”
Places like Kibera “are high-risk areas,” said Rudi Eggers, Kenya’s World Health Organization representative. “In informal settlements, and also refugee camps, where you have lots of people really close together, and limited means of hand washing, it stands to reason that the virus would be worse there.” Kenya has two refugee camps that hold hundreds of thousands of vulnerable people: Dadaab in the east, near Kenya’s border with Somalia, and Kakuma in the northwest, near South Sudan and Uganda. (Here's why other developing countries are especially at risk.)



Nairobi has been my home base for eight years, my sanctuary from long, often difficult, reporting trips. I’ve visited the refugee camps countless times. I’ve photographed the effects of climate change in Somalia and war in South Sudan. Exactly a year ago, I was in eastern Democratic Republic of Congo documenting the battle against Ebola. Now, a new crisis has come here, and I’m trying to tell the story of my adopted home as it is being transformed by the coronavirus pandemic.
Walking in Kibera to meet Zedekia Agure, it was difficult to keep from bumping into people—a constant reminder of how easily the virus can spread here. The air, thick with the smell of frying fish, resounded with a symphony of hawker’s cries, the low roar of motorbikes, the shouts of children chasing a handmade ball. Kibera’s alleys still are bustling not for lack of knowledge of COVID-19, but for lack of options as to how to defend against it.
‘Weaker health systems get overwhelmed’
Last week, I spent the day with a group of paramedics whose dangerous task is to ferry coronavirus patients to Nairobi’s hospitals. For hours, we didn’t move as the sun blazed off the metal of the ambulances. An EMT lounged on a gurney. Beds at Mbagathi Hospital—the institution designated as the isolation center for COVID-19—and the Kenyatta National Hospital were full. Other hospitals were refusing to take patients because their staff lack masks, gloves, and gowns. Already, many doctors and nurses in Nairobi have separated from their families to keep them safe. (A vaccine could take longer than a year to develop.)



“Time is vital now,” Eggers told me, emphasizing the urgent need to acquire more protective equipment and lab kits, and to train health workers and set up facilities for treatment and quarantine. “Weaker health systems get overwhelmed more quickly,” he said, “so I anticipate that that will happen here.”

After the first case in Kenya was identified, on March 12, the government put in place sweeping measures to slow the spread of COVID-19. It closed the country’s borders and airspace and later imposed a three-week ban on movement in and out of Nairobi and three other “infected” regions of the country. Government institutions and private companies have asked staff to work from home. There’s a dusk-to-dawn curfew.
During the first five nights of the curfew, at least seven Kenyans were killed by the police, including 13-year-old Yasin Hussein Moyo, who was shot in the abdomen as he stood on the balcony of his home in Nairobi’s Mathare neighborhood. In the port city of Mombasa, police fired tear gas at hundreds of commuters trying to reach a ferry, and social media posts have shown footage of officers striking people with batons.

“We were horrified by the excessive use of police force,” Amnesty International Kenya and 19 other human rights groups said in a statement on March 28. “We continue to receive testimonies from victims, eyewitnesses and video footage showing police gleefully assaulting members of the public in other parts of the country.” On April 1, spurred by the public outcry, President Uhuru Kenyatta issued an apology “to all Kenyans for… some excesses that were conducted."
I recently visited fashion designer David Avido in his home in Kibera. Anxiety about the pandemic had been keeping him awake at night, he said. To help, he began making colorful face masks. His sewing machine purrs constantly alongside the clatter of traffic and commerce outside his door. So far, he’s handed out more than 6,000 masks in neighborhoods across Kibera, and he says he uses these interactions to advise people on how to stay safe from the virus.
“I believe that all of us, even those who can’t afford to buy a mask, or sanitizers, deserve the same chance to protect themselves,” Avido told me. “We’re all responsible for one another.”




