
In the U.K., families of the dead still wonder: was it COVID-19?
The United Kingdom's death toll is now Europe's highest, and shifting diagnoses leave loved ones without answers.
On March 21, when COVID-19 cases were soaring in England, 68-year-old Ibrahim Kinay was so worried about his 91-year-old father, Ali Kinay, that he sent him a message to post on the door of his home in southeast London: “Please don’t enter without mask and gloves because of Corona 19.”
A month later, Ali had a fall in his house, and was admitted to Lewisham Hospital. He had fallen before, so Ibrahim wasn’t too concerned about his recovery. But on the afternoon of Tuesday, May 19, he received a call from Dr. Patel. Ali’s condition was deteriorating: he had developed an infection—and the doctor suspected he had coronavirus. Dr. Patel invited Ibrahim to visit the following day to say goodbye.
Ibrahim demanded to know how Ali had gotten coronavirus. Dr. Patel didn’t have an answer. (Lewisham Hospital declined to comment, citing patient confidentiality.) The next afternoon, Ibrahim donned a mask and gloves, and followed a nurse to the door of room 18. He stood roughly 10 feet from his unconscious father and called to him futilely, “Baba? Baba?” Ibrahim turned to the nurse and asked again how his father had contracted coronavirus.
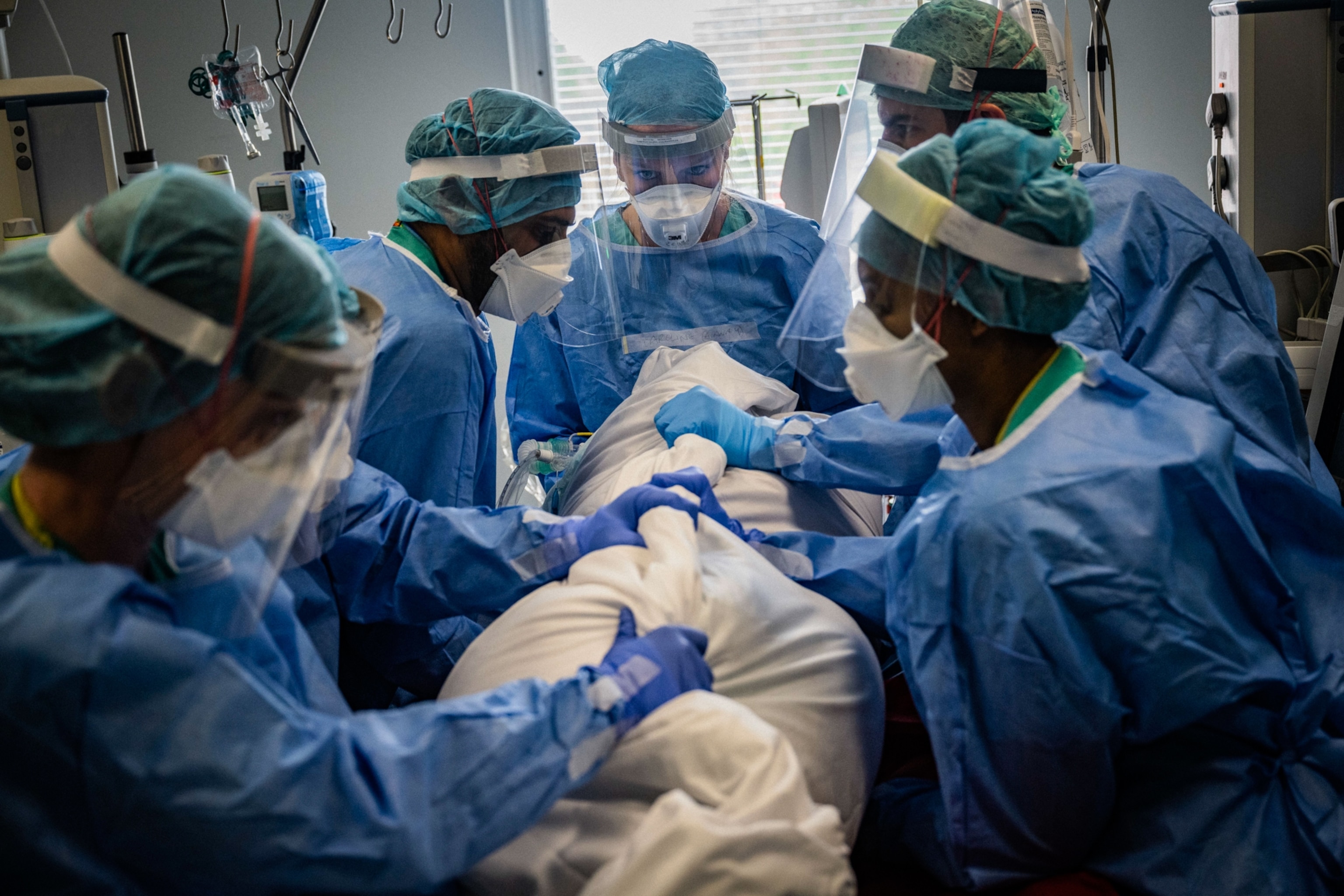
Ali died the following day. “Two days ago, I was talking to him,” Ibrahim says. “I tried to protect him. If I knew it was going to get like this…” His voice trailed off. When he picked up the death certificate, the primary cause of death listed was pneumonia, and the secondary cause was coronary heart disease. As Ibrahim and his brother Irfan said a prayer beside their father’s freshly dug grave in the Muslim section of Grove Park Cemetery in London, they wondered whether coronavirus had killed him.
The United Kingdom currently has the highest number of COVID-19 fatalities in Europe, and one of the top five death tolls in the world. But because of the novelty of coronavirus and the rapidly changing information about testing and treatment, determining coronavirus as the cause of death in victims remains opaque. So, by the time family members have been able to bury their dead, many aren’t sure exactly how they died.
As of July 9, Public Health England has registered 44,602 deaths in the U.K. But death counts are complicated and Ibrahim Kinay’s experience encapsulates so many of the scenes I witnessed and interviews I conducted in England over the past two months. At the beginning of the pandemic those who fell ill and passed away in nursing homes or private homes were rarely—if ever—tested. To make matters more complicated, even those with textbook coronavirus symptoms often tested negative. (The false negative rate is at least one in five, and possibly as high as one in three.)
The shape-shifting rules and guidelines have created a pandemic even more mysterious and deadly than it should have been.
From the dead to the living
In April, when it became clear the United Kingdom might be destined for the same nightmare trajectory as northern Italy and New York, I was in rural England, where rolling hills dotted with puffy sheep and sleeping cows gave way to quaint little villages. The only hint of something amiss was the shuttered shops.
I was desperately trying to access hospitals to photograph the pandemic. Nightly newscasters catalogued the mounting numbers of infected and dead, but there were very few visuals to illustrate the toll. The pandemic felt sanitized. I believed powerful images of how coronavirus ravaged its victims would force the public to take the lockdown seriously and hold leaders of various nations accountable for their response. But my requests to hospitals across England went unanswered or politely declined.
So I began covering the pandemic backwards: from the dead to the living. One of the first funerals I went to was under an uncharacteristically blue sky in southwest England, in the picturesque village of Bathealton. Roughly 10 people, divided into pairs, stood scattered among the tombstones beside the Church of St. Bartholomew as they bid goodbye to Joan Fudge.



The Church of England closed churches, and restrictions on burials were in place nationwide, but small, outdoor funerals were permitted. In the county of Somerset, where the official death toll was among the lowest in England, rules were relatively relaxed, and Fudge’s loved ones were enabled the rare privilege of a graveside burial—and closure.
When Fudge passed away in a nursing home on April 1, few believed COVID-19 had made its way to remote Somerset. The nursing home told Fudge’s niece that she had died suddenly from a “horrible chest infection.” The primary cause of death was listed as pneumonia. Like thousands of others who died in nursing homes in the United Kingdom, she was never tested for coronavirus.
As I continued reporting and hearing stories of the dead, I was increasingly confused. Early on, suspected COVID-19 cases were seemingly labeled otherwise. Later, COVID-19 seemed to be too quickly listed as a cause of death and was rarely investigated further. For the families of Joan Fudge and Ali Kinay, there were questions, sometimes unspoken, that lingered.
An overwhelmed death industry
Simon Albin Dyer, co-managing director of F. A. Albin & Sons, a 200-year-old funeral home in south London, says that many doctors he spoke with about determining the cause of death told him that elderly patients in nursing homes with an acceleration of pneumonia-like symptoms leading to death would likely be attributed to coronavirus.
The procedure for registering deaths outside of a hospital temporarily changed under the U.K.’s “Coronavirus Act.” Now, only one doctor, rather than two, is required to view the deceased and certify the cause of death, and doctors can do so via video, or over the phone with the family, even without having seen the patient in 14 days—as normally required. (If the doctor hadn’t seen them in 28 days, they must speak with the coroner.)
Public Health England’s tally of U.K. deaths initially included only those who passed away in a hospital with a positive coronavirus test. Then, at the end of April, that changed to include cases without a test confirmation, “but where COVID-19 is documented as a direct or underlying cause of death.” At the same time, nursing home deaths were finally included in the U.K.’s official toll. Now, they are estimated to be one-third of total deaths.



This lapse of nearly two months without clear information was deadly for those on the frontlines.
The undertakers called to collect bodies were rarely told the cause of death. Even during a pandemic, when, according to Public Health England, the virus can live for at least 72 hours after death, there is no legal obligation for mortuaries or nursing homes to disclose the cause of death to those handling bodies. Some mortuaries put little red crosses next to the names of those with COVID-19 or suspicious symptoms to alert funeral workers.
The National Association for Funeral Directors offers guidance and advice to those handling the dead—from how to dress the deceased to whether pall bearers need to wear gloves and masks—but each funeral director can ultimately do what they feel comfortable with. Without uniformity in the form of rules and regulations, some funeral directors felt abandoned to fend for themselves. Now, nearly four months into the pandemic, almost all deceased are treated as if they have COVID-19 in order to protect staff.
“We are an unregulated industry. There is no ministry of death [in the U.K.],” says undertaker Simon Albin Dyer, who, at one point during the height of the pandemic, had 280 bodies at his funeral home, most of which were COVID-19 victims. “We were left with very little guidance and help from the beginning. We were left, I felt, just to get on with it, and I am sure a lot of funeral directors would agree.”
View from the hospitals
At the end of May, as the lockdown started to ease, I was finally invited to document COVID-19 in four hospitals across England, from London through the midlands and up to the northwest.
By that time, the deluge of patients had slowed. Most had recovered or passed away. In hospitals, the wards that had been appropriated for COVID-19 were being disinfected and reverted back for cancer treatment or surgical theaters.

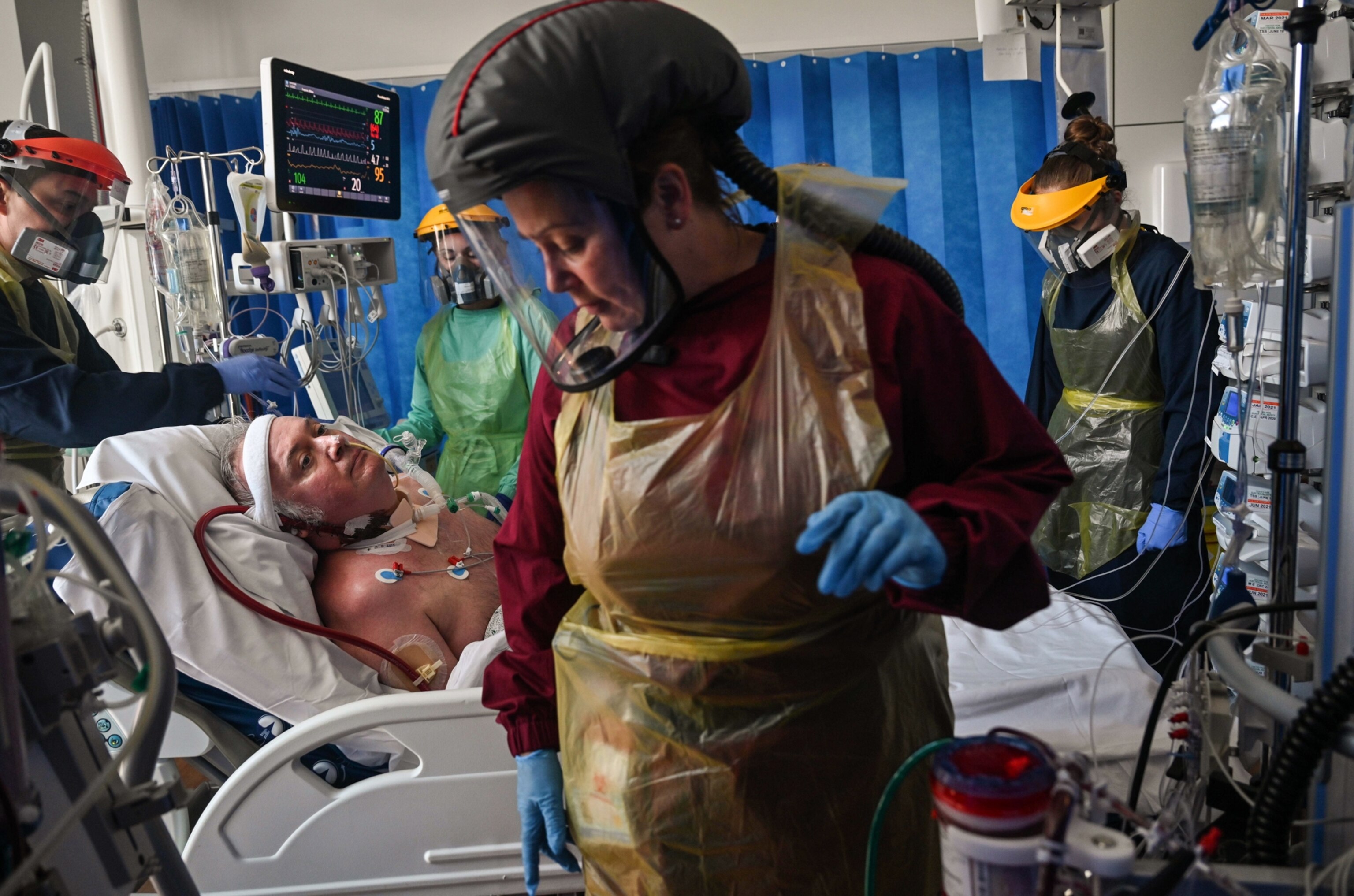
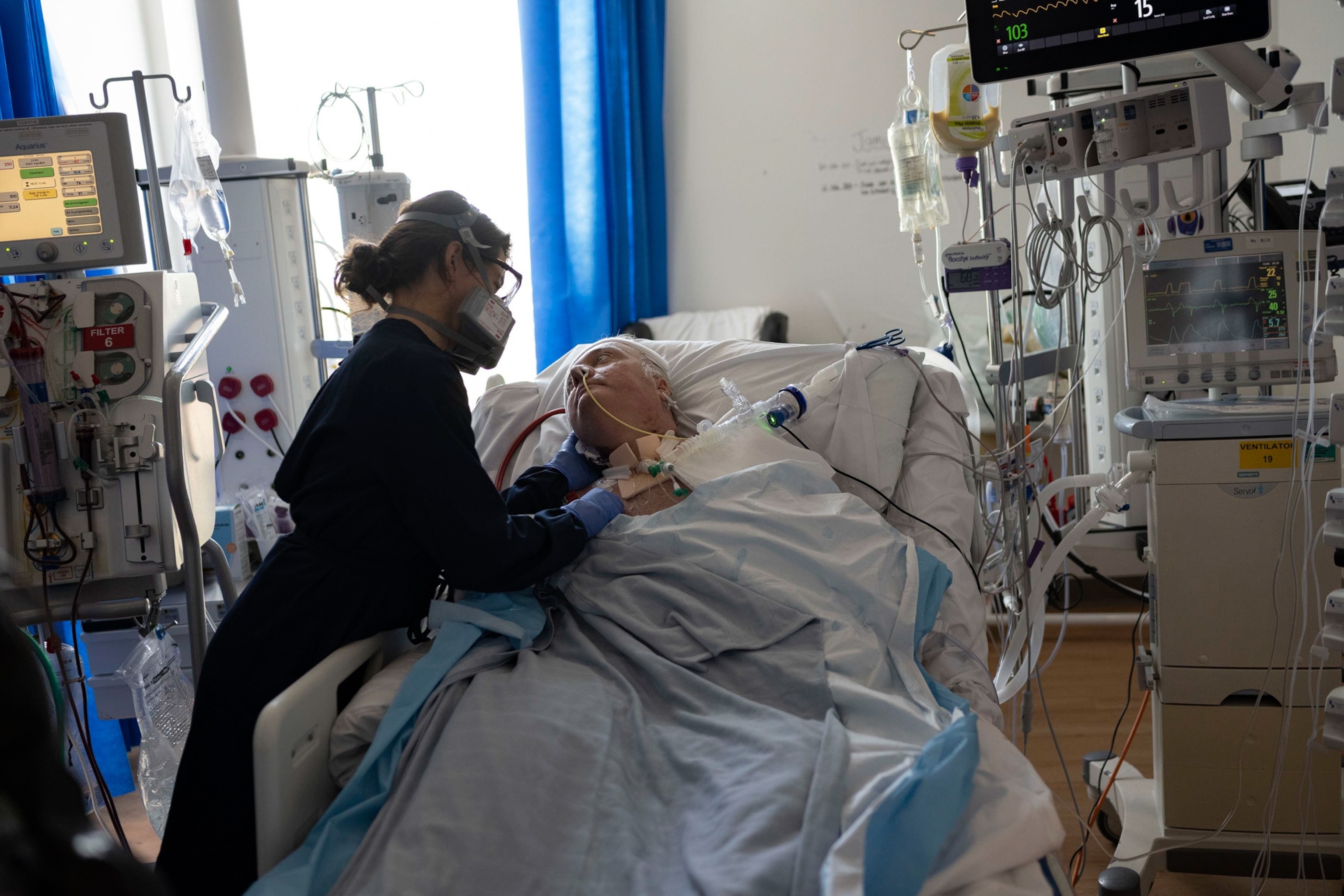
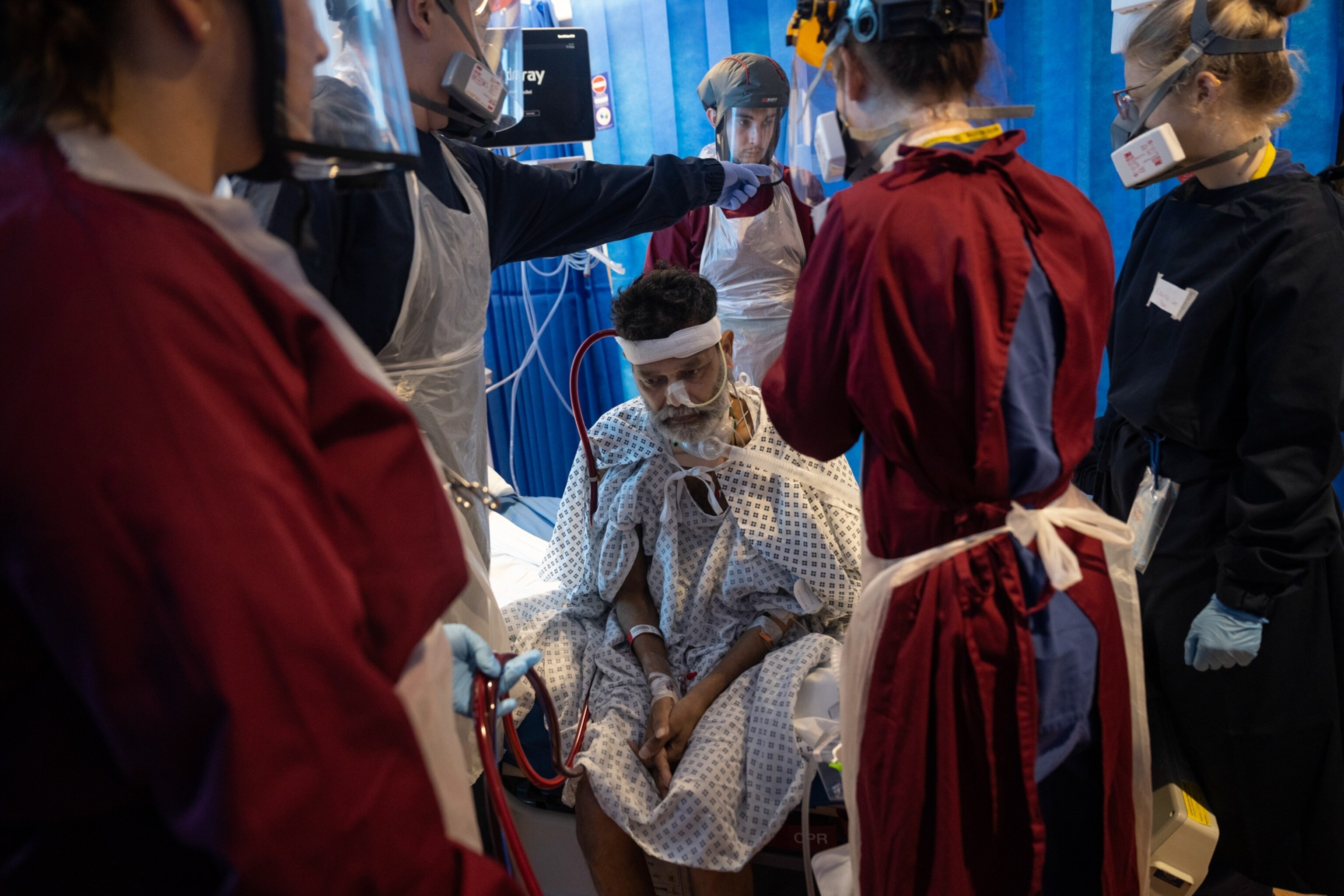
But intensive care units were still filled with patients kept alive by a labyrinth of tubes and cables and machines emitting a cacophony of ominous beeps. The medical staff had mastered the tedious process of donning and doffing PPE—full-body apron, two sets of gloves, hair net, mask, face shield, and clogs—each time they went into a COVID-designated area. The system was well oiled by now, but health care workers still tended to each coronavirus patient with incredible intimacy. Through their masks and face shields and hoods with motor-operated ventilation systems, nurses on their rounds spoke to patients reassuringly (even if most were unconscious) and doctors made daily phone calls to family members to update them on their loved ones’ status.
One of those patients is William Ferguson, a 50 year old who still lies hooked up to life-saving machinery at Royal Papworth Hospital in Cambridge.
On the evening of Wednesday, March 18, Ferguson made a dinner of steak and potatoes with a peppercorn sauce for his wife and 10-year-old daughter. He was the chef of the family, but something didn’t taste right. That night, Ferguson felt hot and clammy, and developed a fever. On Thursday morning, still feverish, Ferguson emailed his team at work to say he wouldn’t make it in. On Friday, he was short of breath. On Monday, only bottled water was palatable and he had developed a cough. His wife called an ambulance. That day, Prime Minister Boris Johnson announced a nationwide lockdown.
When asked for Ferguson’s medical records at the hospital, his wife laughed. They didn’t have any—he rarely even caught a common cold. On April 3, he was transferred to Royal Papworth Hospital, where he was connected to an ECMO machine, which functions as an external set of lungs, and gives a patient with acute respiratory failure the chance to rest and recover. The therapy is reserved for the sickest COVID-19 patients with the best chance of survival. One hundred days in, Ferguson is still hooked up to the ECMO. He’s one of the longest running patients in critical care in the country.
Saying goodbye
Between the time Ferguson entered the ICU and today, much has happened in the U.K. and globally. Stores have re-opened; supermarket lines have dwindled; and toilet paper, hand sanitizer, and face masks are readily available once again. Those who passed away in March, April, and May are almost all buried or cremated now, but there remains a collective sense of solitude—for those who died alone, and for the loved ones who never got a chance to say goodbye.

Some are only now getting their chance.
Esther Akinsanya, 55, and her elder sister, Mary Idowu, 62, were originally from Nigeria. For over 20 years, they had worked side by side as National Health Service (NHS) health care assistants at the Queen Elizabeth Hospital in London. Esther’s colleagues called her “Matron”, because she always went above and beyond to care for others. When coronavirus struck, Esther took on extra shifts. In early April, both sisters fell ill with COVID-19, and after trying to look after each other, they ended up in separate ambulances to the same hospital. Mary was immediately put on a ventilator. Esther was given oxygen.
Four days later, on the morning of April 15, Esther FaceTimed her son, Samuel, from her hospital bed. She told him she was about to go on a ventilator, she loved him, and instructed him to look after his sister. He assumed he would speak with her again when she came off the ventilator. When he looked at his phone a few hours later, he had seven missed calls from the hospital. His mother had passed away. Mary Is still recovering in the hospital.
On June 22, two months after her death, I attended Esther’s funeral.
Her casket wove its way around the perimeter of the Queen Elizabeth Hospital in a horse-drawn carriage. Hundreds of doctors, nurses, health care assistants, relatives, and those who were simply grateful for her service came to see her off. Some were silent in their grief, some wailed, some fell to the ground in despair. They wept for Esther, for what they had seen, for the 218 NHS workers who died in the pandemic, and for what was still ahead in their fight against coronavirus.