
Why giving birth in the U.S. is surprisingly deadly
Black mothers are particularly at risk. Better basic care could help.


There are times when flip-flops and sweatpants seem appropriate. At a Saturday afternoon picnic in the park. Or at the county fair. Or when you’re a couple preparing for the arrival of Baby Number Two. Comfort is key.
But something made Kira Johnson, 39, change her mind on the evening of April 11, 2016.
“Babe, I want to look really pretty for Langston,” she told her husband, Charles Johnson IV, as she sat before her bedroom mirror brushing her hair. The next afternoon they would head to Los Angeles’s Cedars-Sinai Medical Center for the birth of their second son.
They were committed to raising “men that would leave a mark on the world and who have a sense of purpose and responsibility far beyond themselves,” Charles explains.
Baby Number One, born in 2014 by emergency cesarean section, was named Charles Spurgeon Johnson V, after his great-great-grandfather, the famed sociologist and first black president of Fisk University in Nashville, Tennessee. His little brother would be named after the legendary Harlem Renaissance poet Langston Hughes. Kira packed jewelry and a dress so she could bring him home in style. Charles decided he needed to dress the part too. “You never know when you need to look like you have a little bit of sense and a little bit of money,” Johnson recalls thinking, as he scrapped the basketball shorts and T-shirt for a button-down shirt, slacks, and loafers.
The choice was as mindful as the selection of Cedars-Sinai, consistently ranked among the best hospitals in the United States. When you have all the other bases covered—a healthy mom, a healthy baby, the best prenatal care available—why not put the icing on the cake by having your baby at a world-class facility?
Langston Emile Johnson was born at 2:33 p.m. on April 12, 2016. The scheduled C-section seemed routine, and Kira was able to breastfeed just after giving birth. She helped introduce Langston to his 18-month-old brother before drifting off to sleep.
Charles was sitting beside his wife’s bed when he noticed blood in her catheter. It was after 4 p.m. when he first told a nurse about it, according to a complaint Charles filed in 2017 with a lawsuit he brought against Cedars-Sinai. Also included in the complaint are details about the care Kira received: The catheter was changed at about 5:30 p.m. and was followed by an ultrasound and blood work. The ultrasound showed signs of internal bleeding. Pain medication and intravenous fluids were administered. A CT scan was ordered at 6:44 p.m. Ultrasounds and blood work were repeated. A blood transfusion was given. Another four hours and still no CT scan. Another blood transfusion was given, according to the complaint. Kira was “pale and groggy,” Charles says, adding that she was “shivering uncontrollably.” Her abdomen was painful to the touch. Charles says he repeatedly asked hospital staff what was being done to identify the source of her bleeding.
“As a father and a husband, there’s a fine line between trying to advocate for your wife and crossing a line, particularly as a black man,” he recalls. Charles says he did not want to do anything that would be detrimental to his wife’s care.
Especially, Charles says, after one staff member answered his anxious query by saying, “Sir, your wife’s just not a priority right now.”
The CT scan never happened, according to the complaint. Kira was taken into surgery around 12:30 a.m., 10 hours after the C-section. Her abdomen was full of blood. Her last words to her husband, he says, were, “Baby, I’m scared.”
His wife’s fear rattled Charles, because bravery defined her: Kira had lived in China, spoke five languages, had a pilot’s license, and had driven race cars. But he assured her everything would be OK.
Kira died at 2:22 a.m. on April 13.
“‘We did everything we could to save your wife, but we couldn’t save her,’” Charles recalls the doctor telling him. It was “like watching my whole world crumble around me. It was like a bomb went off, and I see her mother fall on the floor, her aunt screaming, her brother just breaking.”

“We were so prepared. We had this. We had the best of everything. We did everything right. And they’re standing there telling me they lost her?” Charles says.
According to the complaint, the autopsy determined that Kira died of internal bleeding after her C-section. Racial bias is not part of the complaint. A trial is scheduled for January. In October, the Medical Board of California found Arjang Naim, the attending physician who oversaw Kira’s care, to be grossly negligent. Naim said Kira Johnson’s death was unfortunate, adding that he did not expect her to pass away on the operating table during surgery. “I did as much as possible to take the best care of the patient,” he said. Naim was put on probation for four years.
A hospital spokesperson would not comment on the specifics of the case but said in a statement that “Kira Johnson’s death was a tragedy. We thoroughly investigate any situation where there are concerns about a patient’s medical care. Based on our findings, we make any changes that are needed so that we can continue to provide the highest quality care to our patients. This includes reviewing hospital procedures as well as the competency of health care providers.”
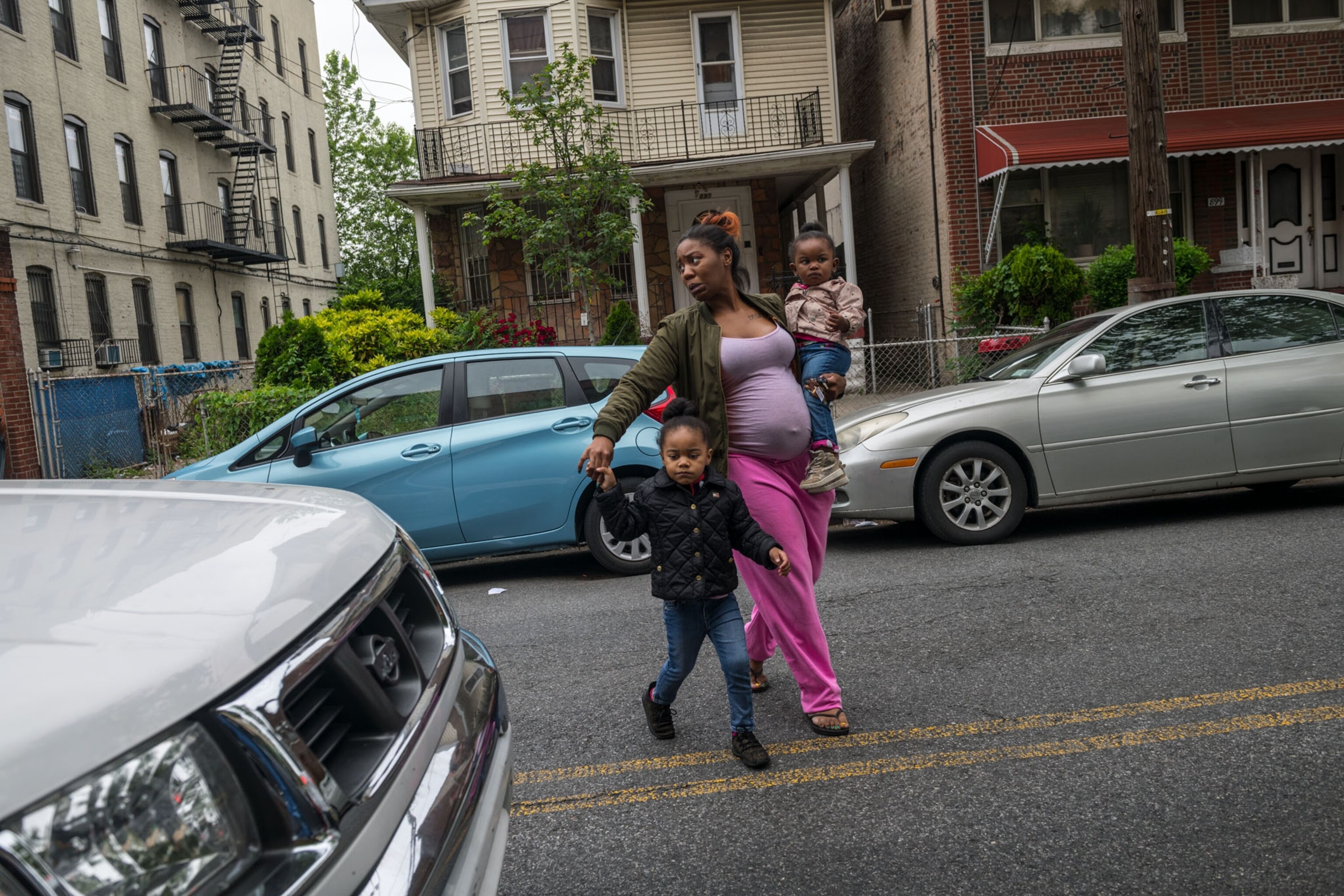
Kira’s death was shocking but underscores a harsh reality: At a time when the pace of medical advances can be breathtaking—from genetic testing that can predict the likelihood of conditions to treatments that have never been more effective in targeting cancer and other diseases—the rate of maternal deaths remains stubbornly high in the United States: about 14 deaths for every 100,000 live births. Among 46 developed nations, the World Health Organization says, only Serbia and the United States had maternal death rates that worsened between 1990 and 2015. This rate includes mothers who die of complications within six weeks of the end of the pregnancy.
In the United States the problem is marked by two particularly alarming statistics: African-American women are about three times as likely to die of pregnancy-related causes as white women, and more than 60 percent of maternal deaths are preventable, according to the Centers for Disease Control and Prevention (CDC).
“We have higher maternal mortality than much of the rest of the developed world; we are capable of doing the best in the world,” says William Callaghan, the CDC’s chief of maternal and infant health. The CDC defines a pregnancy-related death as a woman who dies while pregnant or within one year of the end of her pregnancy.
“When deaths are reviewed and we see what the contributing factors were, there are so many instances where communication was not carried out correctly, where people didn’t recognize urgency, or when the patient wasn’t listened to, or the delay in reaction.”

The maternal mortality rate for the United States remains far below those of developing nations in Africa, where 20 countries have maternal death rates of at least 500 deaths for every 100,000 live births. But even in those countries, where medical facilities and access to basic care often are lacking, maternal mortality rates have declined since 1990 by an average of almost 40 percent, thanks in part to low-tech solutions such as midwives and improvements in prenatal and postpartum care.
All women are vulnerable to the same pregnancy-related health conditions that can lead to death: postpartum hemorrhage, or excessive bleeding; preeclampsia, or dangerously high blood pressure; and sepsis stemming from an infection. So why are the maternal mortality rates for African-American women so high?


Researchers say the toxic stress that racial and ethnic minorities, including African Americans, Latinos, and Native Americans, experience—regardless of economic or social success—can erode their physical health. It’s known as “weathering,” a concept developed by University of Michigan professor of public health Arline Geronimus that suggests the health of African Americans deteriorates earlier than that of whites because of the cumulative effects of racism and bias. It may help explain why even black mothers with the highest levels of education are dying at higher rates than white women with the least education.
Valerie Montgomery Rice, president and dean of the Morehouse School of Medicine in Atlanta, Georgia, believes that not only do bias and racism build up to affect the health of black women over time, but that stress from racism and poverty may have adverse effects as early as in utero or soon after a baby is born.
She also points out that unconscious bias from medical providers can affect the care black mothers receive. While training at Grady Memorial Hospital, she saw that providers would occasionally withhold epidurals and local anesthetics from African-American women. “You have people who believe that black women don’t experience pain the same way because they have higher muscle mass, that their pain fibers don’t fire as much. ‘That woman can push that baby out—she’s a big girl.’” Summing up, Montgomery Rice says, “They didn’t see the person in their totality.”
In developing countries, maternal deaths are vastly more prevalent and an accepted fact of life. Health care infrastructure is often sparse or nonexistent. Quality prenatal care and pregnancy information can be limited. More than 9,000 miles from Los Angeles, the dusty highway between Somaliland’s capital, Hargeisa, and its third largest city, Borama, pierces the horizon like an arrow. The landscape is dotted sparsely with thorny acacia trees, and the sun beats down like a drum.

Venture off the paved surface, and the only roads are rocky and perilous, sure to scar the undercarriage of all but the sturdiest utility vehicle. It’s hard to imagine a woman in labor surviving the journey, in a vehicle or on foot, from a remote rural area to a health facility. Somaliland is a self-declared nation in the Horn of Africa, though it is widely viewed internationally as an autonomous region within Somalia.
The main causes of maternal deaths in Somaliland are eclampsia (seizures or convulsions due to high blood pressure), hemorrhage, infection, and ruptured uterus. Other reasons include early or too many pregnancies, unassisted deliveries, and complications from female genital mutilation (FGM), a practice of removing external genitalia of girls and women in order to make them “pure” and suitable for marriage. The scarred tissue can narrow the birth canal, complicating childbirth.
In Somaliland, consent for C-sections or any kind of lifesaving procedure, including a blood transfusion or surgery, has to be obtained from a male relative financially responsible for a woman’s health, such as her husband or a man from her husband’s side of the family.
That is the landscape into which Edna Adan Ismail, the eldest of three children in a wealthy family, was born.
Her father, Adan Ismail, was the most senior Somaliland health professional in the former British protectorate, which declared its independence in 1960. Of her mother’s five deliveries, one girl died during a forceps delivery in a hospital, a procedure that had almost killed Adan. Another died after being dropped on his head by a midwife.

Education traditionally was considered useless for girls, but Ismail encouraged it for all his children. He was furious upon returning home from a business trip when Adan was about eight years old to learn that her mother and grandmother had arranged for her to undergo FGM.
In 1954, at 17, Adan left Hargeisa to train as a nurse and midwife in London, England. Adan wanted to prevent girls and women from experiencing the trauma she endured during and after receiving “the cut,” as she calls FGM.
Now 81, Adan will tell you that her greatest achievement was not when she was Somaliland’s first female cabinet member. Her ultimate fulfillment comes from living at the Edna Adan University Hospital in Hargeisa as its on-site administrator. She rises every day before dawn and will not refuse a 9 p.m. meeting if it’s in service of her maternity hospital.
Adan says she begged, borrowed, and used her savings and pension to build the hospital.

“The two main killers of pregnant women are poverty and ignorance,” Adan says, striking a regal pose from behind her desk. “A combination of those two kill more women than eclampsia or postpartum hemorrhage. So when you have a woman who’s illiterate, who’s poor—in Somaliland she’s also likely to be a nomad—she’s also lived a life where she’s never had any social justice. Superimpose on that a pregnancy that may have arrived when her body was not fully ready to receive a pregnancy. We delivered a woman here who was having baby number 21.”
Or she may be like the mother of the midwife and chief anesthetist at Edna Adan University Hospital, 27-year-old Hamda Omar Mohammed.
Omar’s mother, Samsam Mohammed, cooked for the construction crew as the hospital was being built in 2002, and Adan struck up an acquaintance. When Mohammed was not at her usual spot one day, Adan wondered why.
Mohammed was at home, bleeding nearly to death. A neighbor who had come to help had pulled on the umbilical cord when trying to deliver the placenta. The cord became detached, and Mohammed began to bleed. Mohammed’s husband ran to get help. Omar, then 11 and the eldest child of four, stayed behind to clean up the blood and look after her siblings. Adan arranged transportation to a government hospital, even donating her own blood to help save Mohammed.
Omar’s mother survived. Years later Adan persuaded that traumatized girl to become a midwife, one of the 938 she has helped train in Somaliland so far. “If I can help train a million midwives on the African continent, it will change the experience of childbirth. It will end the suffering for so many women and families.”


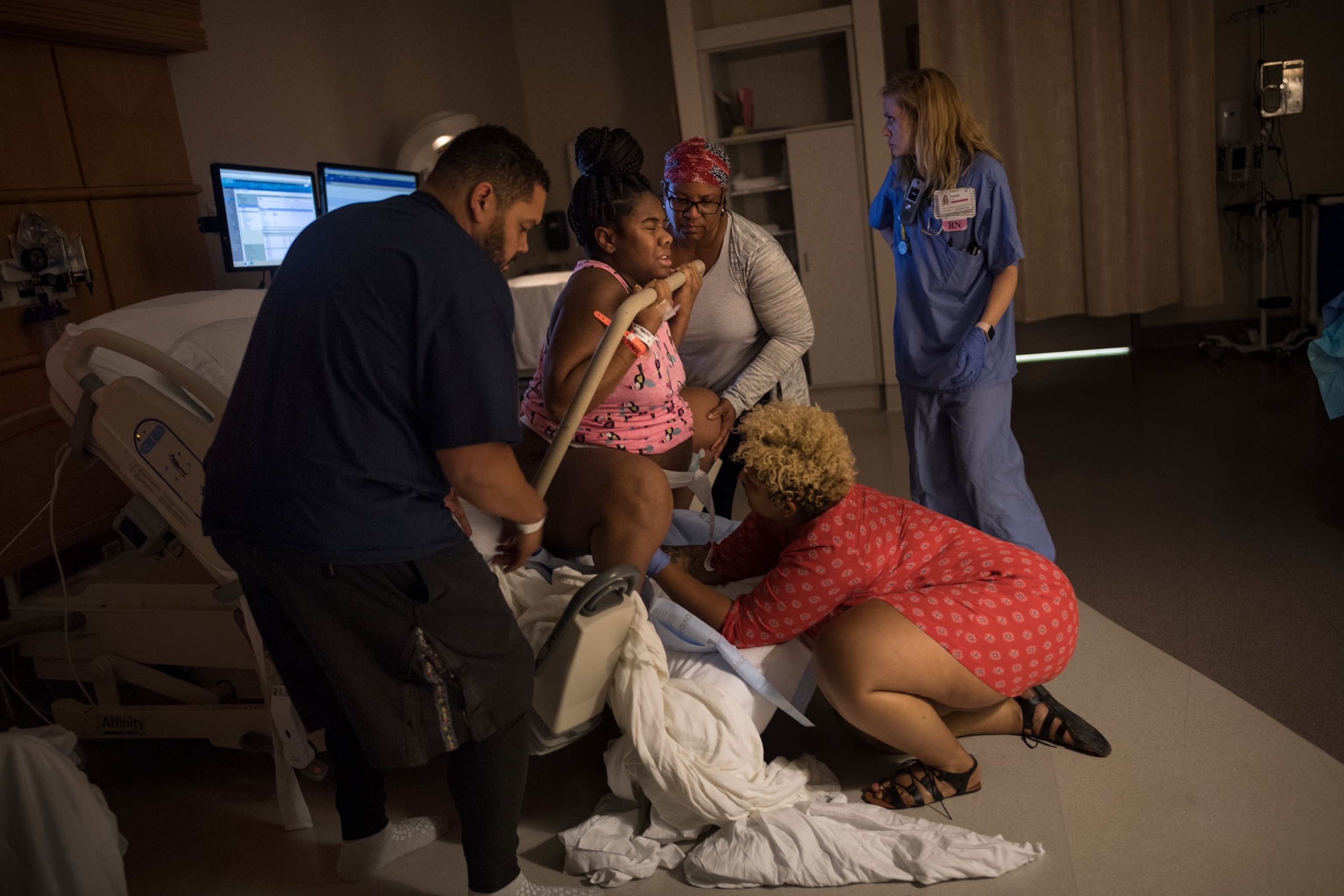
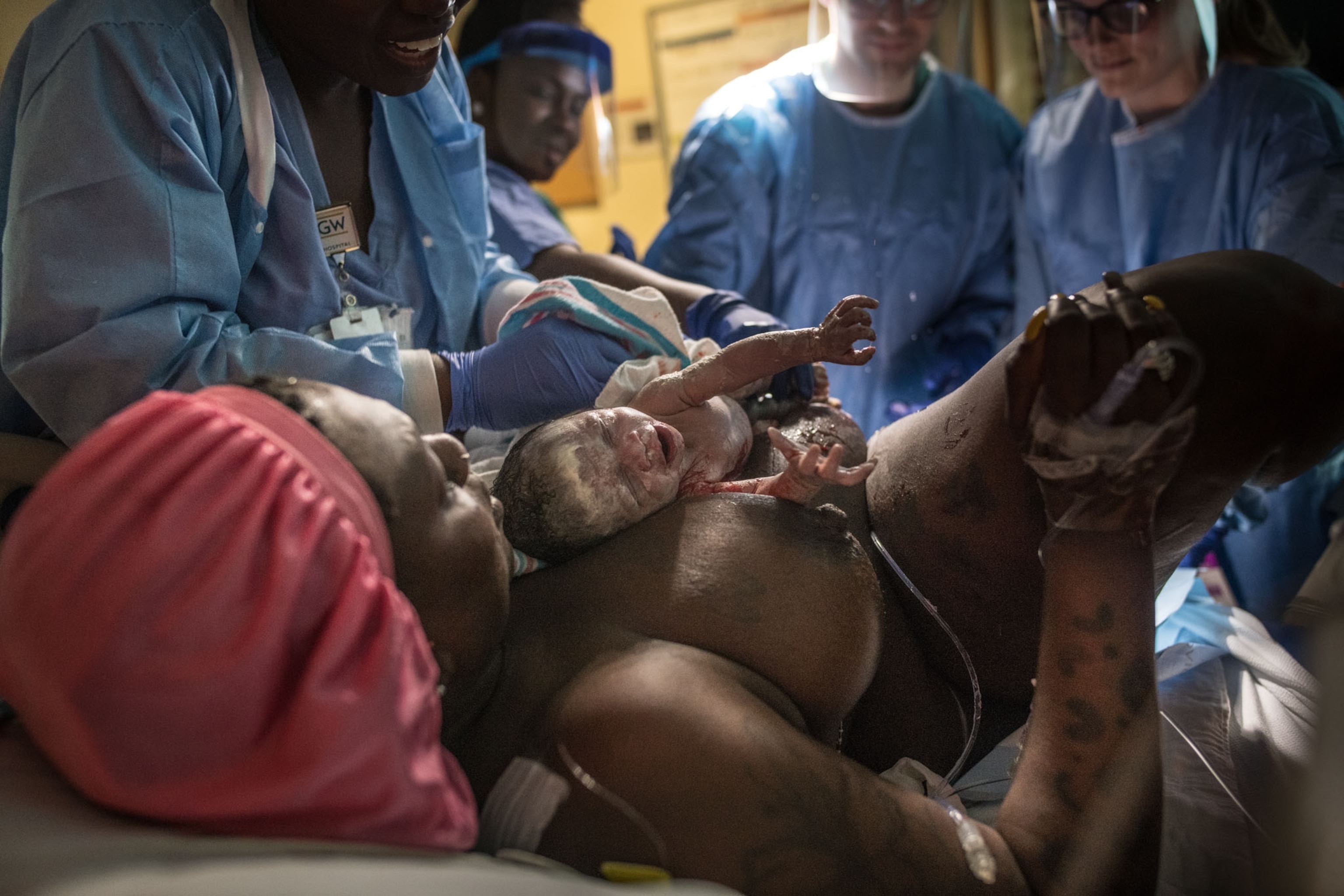
Over the swoosh, swoosh sound of a fetal monitor, Jontelle Gallman’s voice is surprisingly calm. The Washington, D.C., native checked into the George Washington University Hospital on a cloudy Tuesday morning in May, three days after heavy rains flooded her two-bedroom home. Gallman, 39, spent the weekend before her scheduled induced delivery searching for a new place to live.
The mother of three had maintained steady employment as a retail clerk and manager in the two decades since high school, often working 50-hour weeks and providing a good life for her family until 2015. Soon after, doctors diagnosed her with polycystic kidney and liver disease, a chronic genetic condition that causes cysts to grow in those organs.
Too sick to work and relying on Medicaid, the U.S. assistance program that provides health coverage to those with low incomes, Gallman was in the late stages of pregnancy with her fourth child when doctors identified a problem she’d faced previously: dangerously high blood pressure. Without a car and with meager finances, she depended on public transportation and support from friends and family to get to medical appointments and care for her children.
“I just felt like as hard as I had worked to keep things together, life was trying to defeat me,” she says. “But I wasn’t going to let that happen.”
Standing in Gallman’s hospital room through most of the 12 hours of her labor and delivery, I couldn’t help thinking about my own mother, Eloise Blocker Jones. I am the ninth of her 10 children and one of the only three born in a hospital. We all had been born in poverty in Cairo, Illinois, a small town where the Ohio and Mississippi Rivers meet that is known for its tumultuous racial history.
When Mama died in 2005, it never occurred to me that I would one day want to ask her about her pregnancy and childbirth experiences. After all, she had done her best to drum independence and self-sufficiency into each of her five daughters. Pregnancy before marriage was unthinkable, but to hear Mama tell it, it wasn’t exactly a picnic afterward either. I long to ask my mother how she felt as a 19-year-old about to deliver my eldest brother in 1947, far away from her family and friends in Philadelphia. Now I wonder how she endured as a poor woman with no family planning advice, no parenting education, no health insurance.
When Gallman’s Medicaid case manager recommended that she contact the Mamatoto Village maternity-support organization in Washington, D.C., she thought she might be able to get some nutritional advice that could improve her diet and boost her energy.
What Gallman got was a lifeline in the form of a perinatal community health worker named Briana Green.
The 39-year-old former corporate lawyer with a waist-length ponytail and a ballet dancer’s stride now enters Labor and Delivery Room 8 and heads straight for Gallman’s belly, rubbing it gently while also reaching for her hand.
“How are you holding up?” she asks, peering intently at her client through eyelids strained from lack of sleep. At any given time, Green works with about 50 pregnant or postpartum women, making home visits and offering counseling, education, and support. She accompanies them to doctor’s visits and is present during delivery.
Green may have been destined for this life: Her great-grandmother Nancy Gayles Burton had 17 children and was a revered granny midwife in Mecklenburg County, Virginia, in the 1920s and 1930s.
Green says she gave up a six-figure income in law and later selling real estate to train as a perinatal-support worker because of her own birth experiences. She says she was denied the opportunity to try for a vaginal delivery after a cesarean section, even after following guidelines to ensure she was physically prepared.
“I realized that if I, as an educated African-American woman with some financial security, couldn’t be seen or heard or respected, what about women who didn’t have a voice, who were probably being dismissed and mistreated from the minute they entered a health care setting?”
Jessica Flowers is only seven years old, but she’s strong, her grandmother Nicole Black says. Black will never forget how calm the little girl was when she called at 1:46 a.m. on July 4, 2018.
“She said, ‘Mommy’s fallen over in the tub, and she has foam coming out of her mouth,’” recalls Black, who’s 53 and lives in Tampa, Florida. A week earlier, Black’s daughter, Crystle Galloway, had delivered her third child, a healthy six-pound, four-ounce boy named Jacob Flowers, by cesarean section at St. Joseph’s Hospital.
Black scrambled out of bed and over the short distance to Galloway’s apartment, where the 30-year-old mother was slumped over the bathtub.
Just a few hours earlier, Galloway had been sitting on the couch watching a movie and talking about the Fourth of July menu. She’d had a bit of pain from the C-section incision, but otherwise Galloway had been so happy, so proud to complete her family of two girls by adding a son.
Exactly what happened in the minutes between when fire medics, dispatched for a possible stroke victim, according to a Hillsborough County, Florida, official statement, arrived at Galloway’s home and when she was evaluated at an emergency room three blocks away was the focus of an investigation by Hillsborough County officials.
Black says that instead of checking Galloway’s vital signs and transporting her to a hospital, the medics asked whether her family could afford to pay the $600 ambulance fee. Black says that she begged medics to take her daughter in the ambulance.
At a press conference, Hillsborough County Administrator Mike Merrill said that there was confusion about transport and that a conversation about cost was between Black and sheriff’s deputies who arrived first on the scene and not with medics, according to the medics’ and deputies’ statements. Merrill also noted that fire medics admitted that Galloway nodded yes when they asked her directly if she wanted to be transported to the hospital. Merrill said the medics should have obtained an informed refusal document for them not to take her in the ambulance, and that did not happen. Black wound up driving her daughter to the emergency room. Galloway then was taken by helicopter to Tampa General Hospital, where she slipped into a coma. She died five days later.
Hillsborough County announced in September that it had taken disciplinary action against the four medics for violating standard operating procedure by failing to check Galloway’s vital signs, for falsifying documents, and for not having Black sign an informed refusal document for declining the ambulance ride for her daughter.
One medic was terminated; two were demoted. The three medics still on staff were suspended without pay for 30 days.

Better and sustained health care support during mothers’ pregnancies and after they give birth seems a logical solution to help lower U.S. maternal mortality rates, but it’s not that simple. Doulas and midwives can charge upwards of $1,500 for their services, and many low-income mothers simply can’t afford that. California has made progress reducing the number of maternal deaths in the state by adding routine protocols at participating hospitals for common pregnancy complications such as hemorrhage and preeclampsia. Procedures such as measuring blood loss or administering high-blood-pressure medication when needed to prevent preeclampsia are part of a set of practices that medical facilities sometimes ignore or delay.
And as Charles Johnson says, simply listening to mothers and families is also important.
Every day Charles spends time reading, dancing, or playing with his sons in a light-filled room adorned with poster-size photos of Kira posing with family and friends, her smile beaming brighter than the sun’s rays. The boys often ask whether Mommy would have liked this song or whether she would have liked playing with their race cars.
Now raising his young sons alone, Charles devotes most of his time to telling Kira’s story to health officials, advocacy groups, and even the U.S. Congress.
“More than anything I want people to understand that these women we’re losing are more than statistics,” he says.
“They’re mothers, they’re daughters, they’re sisters, they’re friends,” he says. “And they’re leaving behind these precious children, and there’s no statistic that can quantify what it’s like to tell an 18-month-old that Mommy’s not coming home. Or to tell a two-year-old, who never will know his mom, how amazing she is.”