Scientists are unraveling the mysteries of pain
With the opioid crisis, the quest to understand the biology of pain and explore new ways to treat it has taken on fresh urgency.

More than three decades ago, when Tom Norris was fighting cancer, he underwent radiation therapy on his groin and his left hip. His cancer disappeared and hasn’t come back. But Norris was left with a piercing ache that burned from his hip up his spine to his neck.
Since then, Norris, now 70, has never had a single day free from pain. It cut short his career as an aircraft maintenance officer in the U.S. Air Force. It’s been his constant companion, like the cane he uses to walk. On bad days, the pain is so excruciating, he’s bedridden. Even on the best days, it severely limits his ability to move about, preventing him from doing the simplest chores, like taking out the garbage. Sometimes the pain is so overpowering, Norris says, that his breathing becomes labored. “It’s like I’m drowning.”
Norris, who lives in a Los Angeles suburb, spoke to me from a long, cushioned bench, which allowed him to go from sitting to lying flat on his back. A tall and genial man, he’s become adept at wearing a mask of serenity to hide his pain. I never saw him wince. When his agony is especially intense, his wife of 31 years, Marianne, says she can tell by a certain stillness she sees in his eyes.


When the pain began to take over his life, Norris sought solace in speaking out. He became an advocate for chronic pain sufferers and started a support group. And for 30 years he has searched for relief. For many of those years he was on fentanyl, a powerful opioid that he says covered his pain “like a thick blanket” but kept him “basically horizontal and zoned out.” He has tried acupuncture, which was somewhat helpful, as well as bee stings, magnet therapy, and faith healing, which weren’t. Norris now manages his pain with physical therapy, which improves his mobility, and steroids injected into his spine, which quiet his inflamed nerves.
Like Norris, nearly 50 million people in the United States and millions more around the world live with chronic pain. The causes are diverse, from cancer to diabetes to neurological illnesses and other ailments. But they share a common source of suffering: physical agony that disrupts their lives, intermittently or all the time. It’s not uncommon for cancer patients experiencing severe, unrelenting pain after chemotherapy to opt out of treatment in favor of the ultimate salve of dying.
The toll exacted by chronic pain has become increasingly visible in recent years. After doctors in the late 1990s began prescribing opioid medications such as oxycodone to alleviate persistent pain, hundreds of thousands of Americans developed an addiction to these drugs, which sometimes produce feelings of pleasure in addition to easing pain. Even after the risks became evident, the reliance on opioids continued, in part because there were few alternatives. No novel blockbuster painkillers have been developed in the past couple of decades. (Read how science is unlocking the secrets of addiction.)
The misuse of opioid pain relievers—which are ideally suited for short-term management of acute pain—has become rampant across the United States. In 2017, an estimated 1.7 million Americans had a substance abuse disorder stemming from having been prescribed opioids, according to the National Survey on Drug Use and Health. Every day in the U.S., about 130 people die from opioid overdoses—a grim statistic that includes deaths from prescription painkillers as well as narcotics like heroin. (See the toll of the opioid crisis on one Philadelphia street.)

The quest to understand the biology of pain and find more effective ways to manage chronic pain has taken on fresh urgency. Researchers are making significant strides in detailing how pain signals are communicated from sensory nerves to the brain and how the brain perceives the sensation of pain. Scientists also are uncovering the roles that specific genes play in regulating pain, which is helping to explain why the perception and tolerance of pain vary so widely.
These advances are radically altering how clinicians and scientists view pain—specifically chronic pain, defined as pain that lasts more than three months. Medical science traditionally regarded pain as a consequence of injury or disease, secondary to its root cause. In many patients, it turns out, pain originating from an injury or ailment persists long after the underlying cause has been resolved. Pain—in such cases—becomes the disease.
The hope is that this insight, coupled with the steadily advancing understanding of pain, will lead to new therapies for chronic pain, including nonaddictive alternatives to opioids. Norris and other patients are keen to see those breakthroughs happen. Researchers, meanwhile, are testing promising alternative strategies, such as stimulating the brain with mild electric shocks to alter its pain perception and harnessing the body’s intrinsic capacity to soothe its own pain.
Clifford Woolf, a neurobiologist at Children’s Hospital in Boston who’s studied pain for more than four decades, says it’s tragic it has taken a “societal catastrophe” for pain to get the attention it deserves from scientists and physicians, but the impetus this has given to pain research is a silver lining. “I think we have the potential in the next few years of really making an enormous impact in our understanding of pain,” he says, “and that will definitely contribute to new treatment options.”
The capacity to feel pain is one of nature’s gifts to humankind and the rest of the animal kingdom. Without it, we wouldn’t reflexively recoil our hand upon touching a hot stove or know to avoid walking barefoot over broken glass. Those actions, motivated by an immediate or remembered experience of pain, help us minimize the risk of bodily injury. We evolved to feel pain because the sensation serves as an alarm system that is key to self-preservation.





The sentries in this system are a special class of sensory neurons called nociceptors, which sit close to the spine, with their fibers extending into the skin, the lungs, the gut, and other parts of the body. They’re equipped to sense different kinds of harmful stimuli: a knife’s cut, the heat of molten wax, the burn of acid. When nociceptors detect any of these threats, they send electrical signals to the spinal cord, which transmits them via other neurons to the brain. Higher order neurons in the cortex—the final destination of this ascending pain pathway—translate this input into the perception of pain.
Upon registering the pain, the brain attempts to counteract it. Neural networks in the brain send electrical signals down the spinal cord along what’s known as the descending pain pathway, triggering the release of endorphins and other natural opioids. These biochemicals inhibit ascending pain signals, effectively reducing the amount of pain perceived.
Scientists had sketched out this basic schematic of ascending and descending pain pathways when Woolf began working in the field in the 1980s. A soft-spoken man with eyes that seem to brim with kindness, Woolf was struck by the plight of patients he saw in the surgery ward when he was pursuing his medical degree.
“It was clear that all were suffering from severe pain,” he says. Woolf felt the senior resident surgeon seemed almost resentful that they were complaining. “I said to the surgeon, ‘Why aren’t you doing anything?’ ” Woolf recalls. “And the surgeon said, ‘Well, what do you expect? They just had an operation. They’ll get better.’ ”

“Pain was a problem the medical profession downplayed—to a substantial extent because there were no safe and effective interventions,” Woolf says. This realization kindled his desire to understand the nature of pain.

Using rats as a model, he set out to learn more about how pain is transmitted. In his experiments, Woolf recorded the activity of neurons in the animals’ spinal cords in response to a brief application of heat to their skin. As he expected, he observed these neurons firing excitedly when signals arrived from the nociceptive neurons. But Woolf made an unexpected finding. After a patch of skin subjected to heat a few times became inflamed, the neurons in the spinal cord attained a heightened state of sensitivity. Merely stroking the area surrounding the previously injured patch caused them to fire.
This showed that the injury to the skin had sensitized the central nervous system, causing neurons in the spinal cord to transmit pain signals to the brain even when the input from peripheral nerves was innocuous. Other researchers have since demonstrated this phenomenon—called central sensitization—in humans and shown that it drives various types of pain, such as when the area around a cut or a burn hurts at the slightest touch.
A startling conclusion from Woolf’s work and subsequent research was that pain could be generated in the absence of a triggering injury. This challenged the view held by some doctors that patients who complained of pain that couldn’t be explained by any obvious pathology were likely lying for one reason or another—to get painkillers they didn’t need, perhaps, or to gain sympathy. The pain transmission system can become hypersensitive in the wake of an injury—which is what happened in the rats—but it also can go haywire on its own or stay in a sensitized state well after an injury has healed. This is what happens in patients with neuropathic pain, fibromyalgia, irritable bowel syndrome, and certain other conditions. Their pain is not a symptom; it’s a disease—one caused by a malfunctioning nervous system.
With advances in growing human stem cells in the lab, Woolf and his colleagues are now creating different types of human neurons, including nociceptors. This breakthrough is allowing them to study neurons in greater detail than was previously possible to determine the circumstances where they become “pathologically excitable,” Woolf says, and fire spontaneously.
Woolf and his colleagues have used lab-grown nociceptors to investigate why chemotherapy drugs cause neuropathic pain. When the nociceptors are exposed to these drugs, they become more easily triggered and begin to degenerate. This likely contributes to the neuropathies that 40 percent of chemotherapy patients endure.
While scientists like Woolf are advancing the understanding of how pain is transmitted, other scientists have discovered that these signals are just one factor in how the brain perceives pain. Pain, it turns out, is a complex, subjective phenomenon that is shaped by the particular brain that’s experiencing it. How pain signals are ultimately translated into painful sensations can be influenced by a person’s emotional state. The context in which the pain is being perceived also can alter how it feels, as evidenced by the pleasantness of the aches that follow a strenuous workout or the desire for a second helping of a spicy dish despite the punishing sting it delivers to the tongue.
“You’ve got this incredible capability of altering how those signals are processed when they do arrive,” says Irene Tracey, a neuroscientist at the University of Oxford.
A skilled communicator who speaks in rapid-fire sentences, Tracey has spent much of her career trying to bridge the mysterious link between injury and pain. “This is a highly nonlinear relationship, and many things can make it worse or can make it better or could make it very different,” she says.
In experiments, Tracey and her colleagues have imaged the brains of human volunteers while subjecting their skin to pinpricks or bursts of heat or smears of cream laced with capsaicin, the chemical compound that makes chili peppers spicy. What the researchers have found has led them to discover a much more complex picture of pain perception than had been previously envisioned. There’s no single pain center in the brain. Instead, multiple regions are activated in response to painful stimuli, including networks that also are involved in emotion, cognition, memory, and decision-making.
They also learned that the same stimulus doesn’t produce the same activation pattern every time, indicating that a person’s experience of pain can vary even when the injuries are similar. This flexibility serves us well, raising our pain tolerance in situations that demand it—for instance, when carrying a scorching bowl of soup from the microwave to the kitchen counter. The mind knows that dropping the bowl midway would result in greater misery than the brief anguish caused by holding the bowl, so it tolerates the momentary suffering.
Tracey and her colleagues have shown that fear, anxiety, and sadness can make pain feel worse. In one of their experiments, healthy student volunteers listened to Prokofiev’s deeply melancholic “Russia Under the Mongolian Yoke,” slowed to half speed, and read negative statements such as “My life is a failure.” At the same time, they received a burst of heat on a patch on their left forearm, which had been rubbed with capsaicin. Later the students received the same stimulus as they listened to happier music and read neutral statements such as “Cherries are fruits.” In the sad condition, they reported finding the pain “more unpleasant.”
Comparing scans of the students’ brains in the two moods, the researchers found that sadness influenced more than just the emotion-regulation circuitry. It led to increased activation in other brain regions, indicating that sadness was physiologically dialing up the pain. “We’ve made people anxious and threatened and fearful,” Tracey says, “and we’ve shown that that makes the actual processing of those signals amplified.”
Strong medication would be needed to dull the pain after surgery for arthritis in her hand, Jo Cameron was informed by her anesthesiologist. But the 66-year-old Scottish woman doubted it. “I bet you any money I will not take any painkillers,” she told him.
The anesthesiologist looked at her as if she were not fully sane. He knew from experience that the postoperative pain was excruciating. When he came by to check on her after surgery, he was astonished to find that she hadn’t requested so much as the mild analgesic he’d prescribed. “You haven’t even taken paracetamol, have you?” he asked.
“No,” Cameron recalls having replied cheerfully. “I told you I wouldn’t.”
Growing up, Cameron says, she was frequently surprised to discover bruises whose origins were a mystery. When she was nine, she broke her arm in a roller-skating accident, but three days passed before her mother noticed that it was swollen and discolored. Years later, Cameron gave birth to her two children without any pain during delivery.
“I don’t really know what pain is,” she says. “I see people in pain, and I see the grimace, the strain on their faces, and the stress, and I have none of that.”
Cameron’s inability to sense physical hurt may be unremarkable to her, but it places her in a rarefied group of individuals who are helping scientists unravel the genetics underlying our ability to feel pain. Her amazed anesthesiologist put her in touch with James Cox, a geneticist at University College London. Cox and his colleagues studied her DNA and found she had two mutations in two neighboring genes, called FAAH and FAAH-OUT. They determined that the mutations reduce the breakdown of a neurotransmitter called anandamide, which helps provide pain relief. Cameron has an excess of the biochemical, insulating her against pain.
Cox has been studying people like Cameron since he was a postdoc at Cambridge in the mid-2000s, when his supervisor, Geoffrey Woods, learned about a 10-year-old street performer in Pakistan who could walk barefoot over hot coals and stick daggers into his arms without so much as a whimper. The boy would earn money from these stunts and then go to the hospital to be treated for his wounds. He was never the subject of a study—he died from head injuries after falling off a roof while playing with friends—but Cox and his colleagues were able to analyze the DNA of six children from the same clan, who showed similar insensitivity to pain. The children each had a mutation in a gene called SCN9A, known to be involved in pain signaling.
The gene makes a protein that is instrumental in the transmission of pain messages from nociceptive neurons to the spinal cord. The protein, christened Nav1.7, sits on the surface of the neuron and serves as a channel for sodium ions to pass into the cell, which enables electrical impulses constituting the pain signal to propagate along the threadlike axon that connects to another neuron in the spinal cord.
The mutations the researchers discovered in the SCN9A gene yield malformed versions of the Nav1.7 protein that don’t allow sodium ions to pass into nociceptive neurons. With their nociceptors incapable of conducting pain signals, the children were oblivious when they chewed their tongues or scalded themselves. “The beauty of working with these extremely rare families is that you can identify single genes which have the mutation and essentially are human-validated analgesic drug targets,” Cox says.
Mutations in the SCN9A gene are also linked to a rare condition called inherited erythromelalgia, or man-on-fire syndrome. Patients who have it face the extreme opposite of insensitivity to pain: a burning sensation on their hands, feet, and face. In warm surroundings, or with slight exertion, the sensation gets unbearably intense, akin to holding one’s hand over a flame.
Pamela Costa, a 53-year-old clinical psychologist from Tacoma, Washington, who suffers from the syndrome, describes the pain as “inescapable.” To cope, she has her office temperature set at a chilly 60 degrees. She can sleep only with a complement of four fans around her bed and the air-conditioning on at full blast. In an ironic similarity to individuals with pain insensitivity, the constant burning sometimes makes it hard for Costa to discern hot surfaces, which is how she burned her arm a year ago while ironing.
“I didn’t realize until I heard a hissing sound from my skin getting seared,” she says. “It was the same sensation as I was already having.”
Stephen Waxman, a neurologist at Yale University School of Medicine and one of the world’s foremost experts on nerve conduction, has studied Costa and others like her in his lab at the Veterans Affairs Medical Center in New Haven, Connecticut. Gracious and affable, Waxman speaks animatedly and possesses a cheery disposition despite having made pain his life’s work. He and his colleagues found, as another group had, that man-on-fire patients had mutations in their SCN9A gene. Those mutations have the opposite effect of the one in the pain-free kids from Pakistan, creating Nav1.7 channels that open too easily, allowing sodium ions to flood in even when they shouldn’t.
Through lab experiments conducted on neurons in petri dishes, Waxman and his colleagues proved that this was the mechanism by which the SCN9A mutations caused the syndrome in patients like Costa. “We were able to put the channel into pain-signaling neurons and cause them to go BRRRP! when they should be going bop-bop,” says Waxman, referring to the hyperactivity that results from the unabated inflow of sodium ions. In patients with the syndrome, this defect causes nociceptors to bombard the brain with pain messages constantly.

The discovery that Nav1.7 can open or close the floodgates to nociceptive pain signals has made the channel an attractive target for researchers looking to develop new pain medications that don’t pose the risk of addiction that opioids do. Opioids work by binding to a protein on the surface of nerve cells called the mu-opioid receptor, causing the receptor to communicate with proteins inside the cell. While the action of some of these proteins alleviates pain, the receptor’s communication with other proteins results in pleasurable feelings. The body develops a tolerance to these drugs, meaning that higher and higher doses are required to trigger the sense of euphoria, which can cause addiction.
Because Nav1.7 is present only in damage-sensing neurons, a drug that selectively turns off the channel promises to be an effective pain reliever. The sole known side effect is the loss of the sense of smell. Likewise, individuals with the mutation also can’t smell. Existing local anesthetic drugs such as lidocaine indiscriminately block nine sodium channels in the body, including ones that are key to an array of brain functions, which is why doctors must limit their use to numbing patients temporarily. Drug companies are searching for compounds that might be able to block Nav1.7 without disabling other sodium channels, but success has been elusive.
Even so, Waxman is optimistic that the research eventually will lead to better drugs. “I’m confident there will be a new and more effective class of medicines for pain that are not addictive,” he says, his eyes brightening. Then he pauses for a moment and tempers his enthusiasm. “But I can’t begin to attach a time line.”
While the search for new drugs continues, clinicians and researchers are investigating ways to deploy the brain’s intrinsic abilities to modulate pain and lessen the suffering associated with it. And those abilities are impressive. After all, our minds and bodies have been coping with pain for a lot longer than we’ve been studying it.
Take, for example, a recent British study of more than 300 patients with a type of shoulder pain thought to be caused by a bone spur. To relieve the pain, the spur is often removed in surgery. Researchers randomly divided the participants into three groups. One group underwent the surgery. A second group was led to believe it had, but it hadn’t. A third group was asked to return in three months to see a shoulder specialist. The group that had the operation and the one that thought it did reported similar relief from their shoulder pain.
“What it showed is that it’s just a placebo. The surgery is not mechanistically doing anything for the pain,” says Oxford’s Irene Tracey, one of the study’s authors. “The pain relief the patients are getting is just driven by a placebo effect.”
But to Tracey, the outcome isn’t any less important because it shows the placebo effect worked. On the contrary, she says, the study reveals the force of a patient’s belief in the treatment. “What it’s powerfully saying is expectations shape pain,” Tracey says.
Other studies have uncovered how a patient’s expectation of reduced pain can translate into actual relief. It seems to activate the brain’s descending pain pathway, leading to the release of opioids synthesized inside the brain that impede the incoming pain signals from the body.
“This is not just pretend,” Tracey says. “The placebo mechanism hijacks this very powerful system in the brain.”
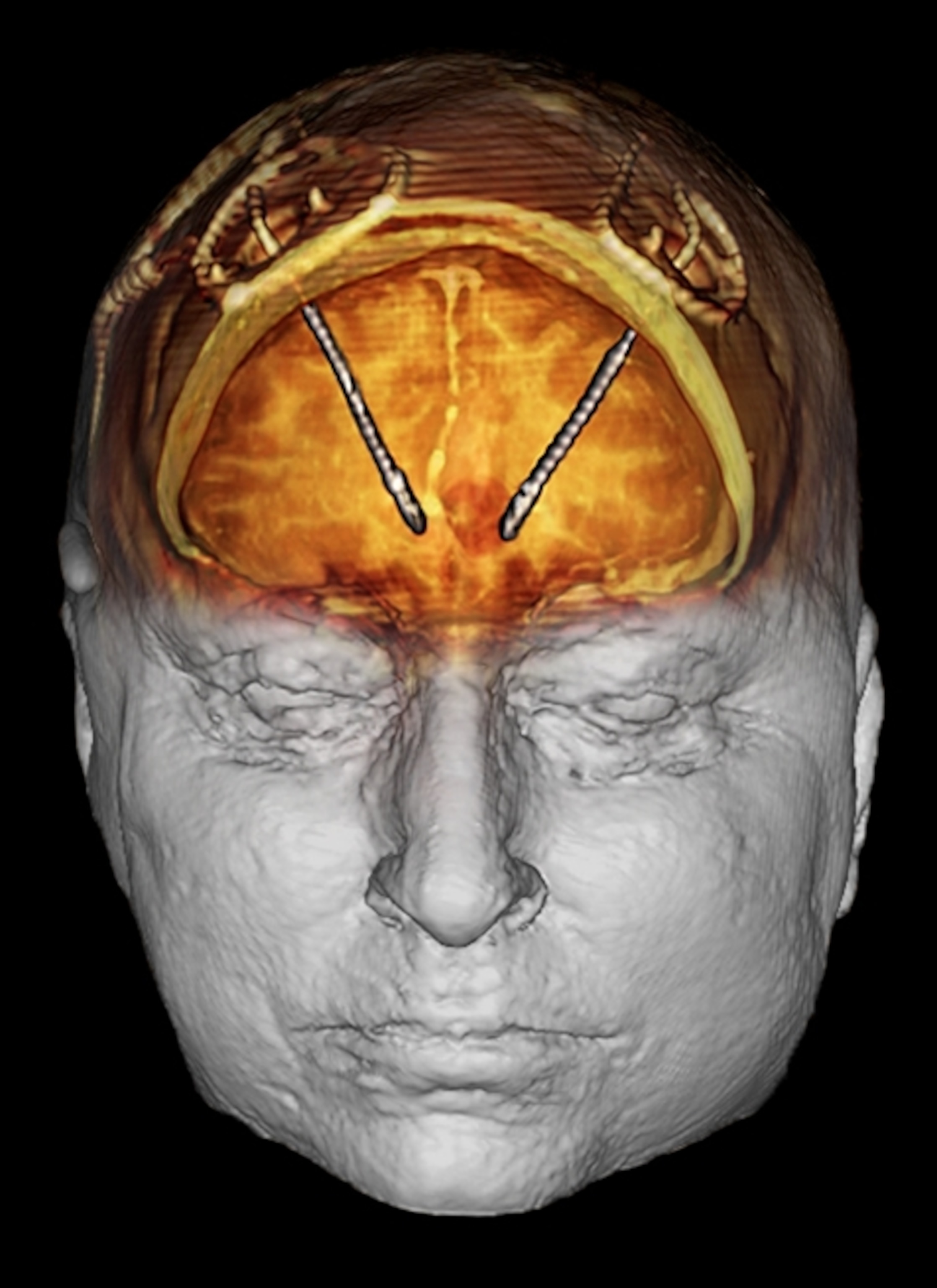
Our perception of pain isn’t limited to merely sensing it. The feelings of unpleasantness, fear, and anxiety that accompany the sensation are an integral part of experiencing pain. In a trial at the Cleveland Clinic, researchers led by neurosurgeon Andre Machado used deep brain stimulation (DBS) to target this emotional component of pain in 10 patients who had chronic neuropathic pain after suffering a stroke. The researchers implanted tiny electrodes in a part of the brain involved in processing emotions. Wired to an electronic device inserted in the chest, the electrodes delivered mild shocks to the implantation site at a rate of nearly 200 a second.
“In several patients, we saw an improvement in their quality of life, in their sensation of well-being, in their independence—without improving the amount of pain,” Machado says.
Patients who had scored their pain as a nine on a 10-point scale, for example, continued to give it the same score but reported being able to function better. One of the study subjects, Linda Grubb, describes the treatment as transformative. “It made all the difference in the world as far as being able to go places,” she says, adding that her post-stroke pain had compelled her to spend her days on the couch. “I have so much more energy. My husband says I seem so much happier. It really changed my life completely.”
A subsequent part of the study involving both healthy subjects and chronic pain patients gave Machado and his colleagues some insight into why deep brain stimulation appeared to have benefited patients like Grubb. The researchers recorded electrical activity from the brains of participants as they watched a screen while they had two devices strapped to their arms. One device delivered a flash of heat to the skin; the other delivered a harmless buzz. From the visual cue that appeared on the screen, the participants could tell which of the two stimuli they were about to get or if they were going to get nothing at all.

The researchers compared the brain activity of participants as they received heat pulses and buzzes or nothing. They found that the brains of chronic pain patients responded similarly when anticipating a painful stimulus and a harmless one, whereas the brains of healthy volunteers showed increased activity in certain regions only when anticipating the heat. When chronic pain patients repeated the experiment while receiving DBS, their brain activity was more similar to that in healthy participants.
To Machado and his colleagues, these findings suggest that the brains of chronic pain patients are conditioned by constant exposure to pain to react as if every stimulus is potentially painful, causing the patients to live in distress. The DBS treatment seems to restore a degree of normalcy, enabling the brain “to again distinguish painful from nonpainful, which is what you need in order to be able to function,” Machado says.
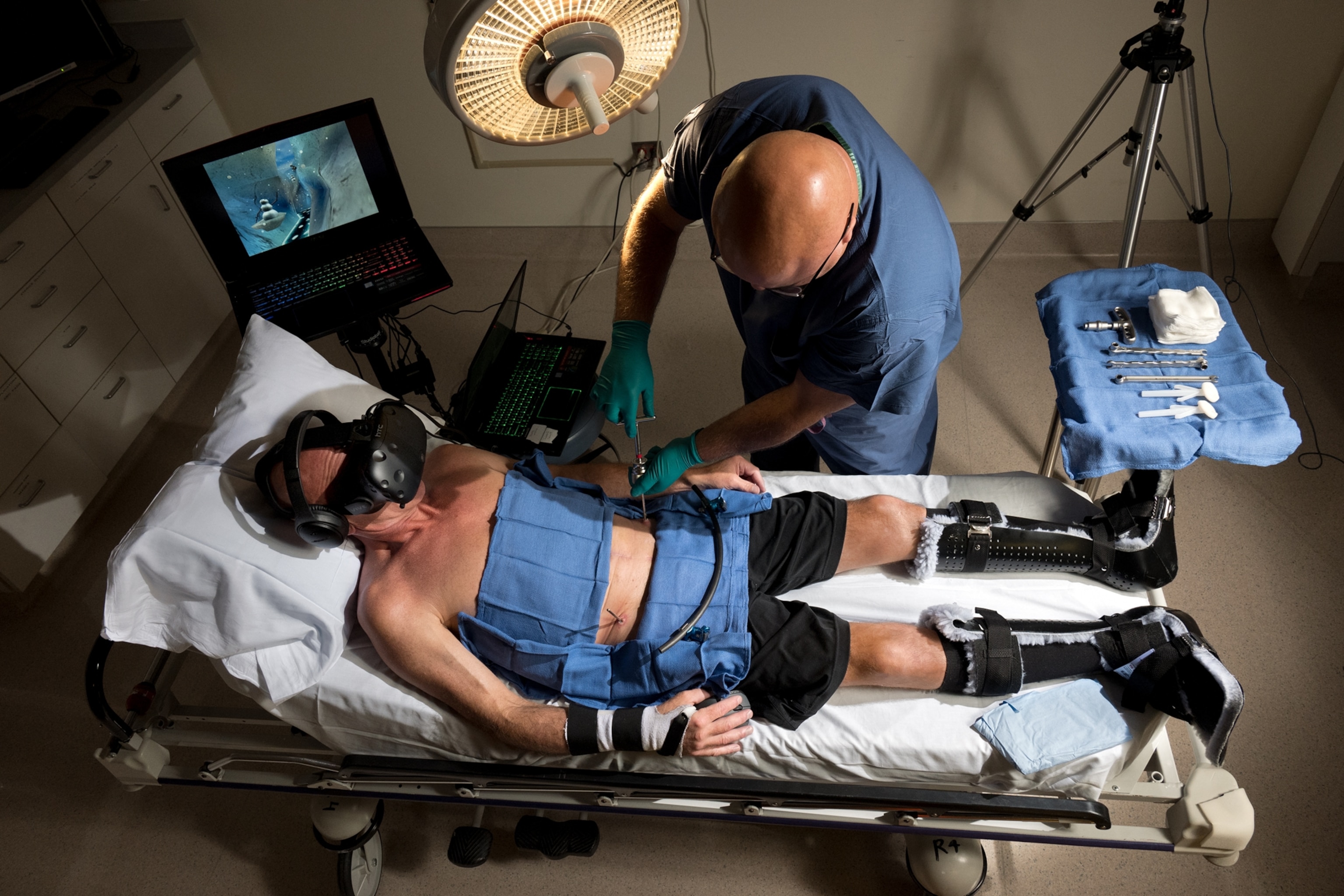
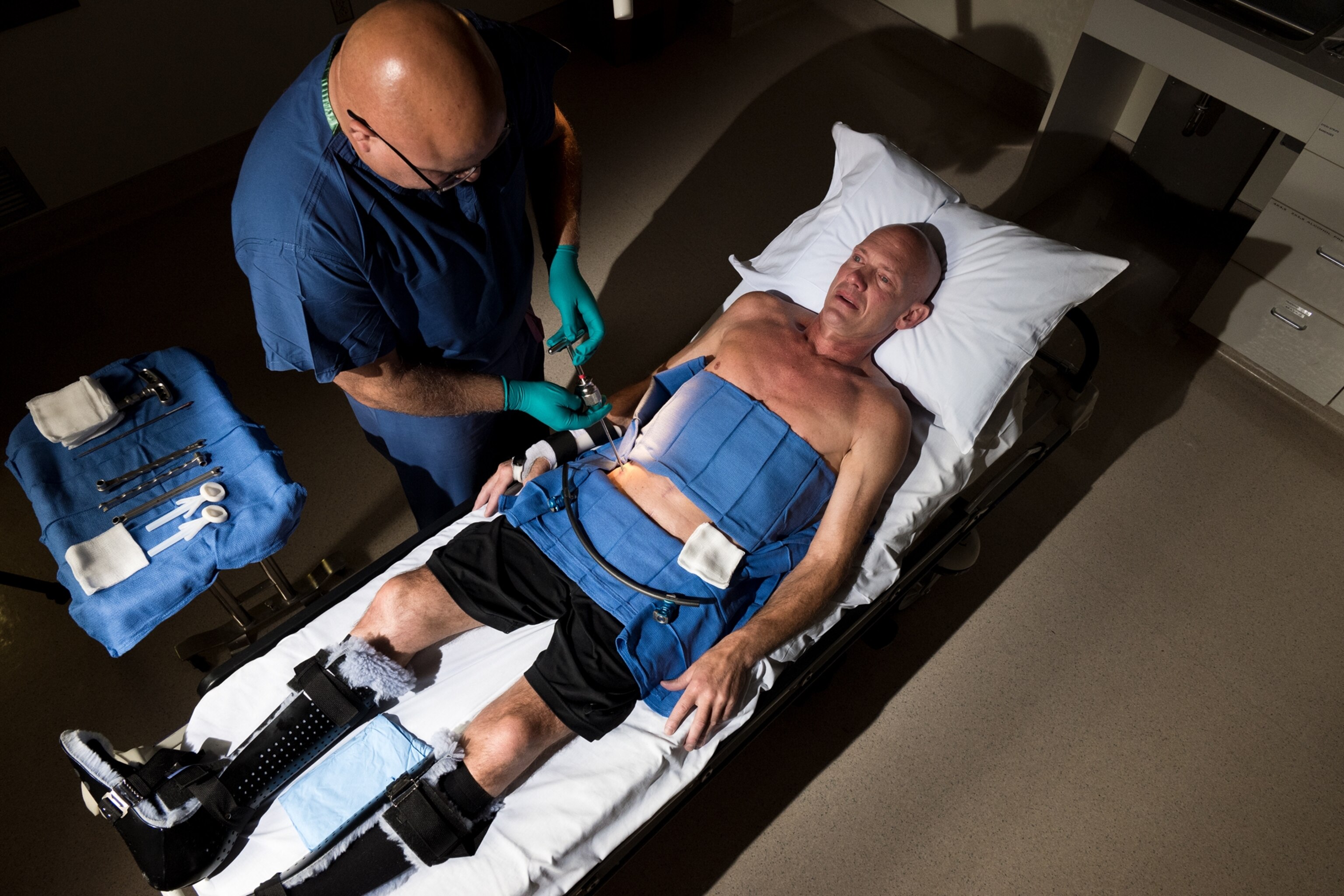
Virtual reality may prove to be another way of reducing pain. I experienced the power of the technique firsthand at the lab of Luana Colloca, a neuroscientist at the University of Maryland. One of Colloca’s assistants strapped a little box onto my left forearm as I sank into a comfortable recliner. The device was similar to the one that Machado’s group had used: Connected to a computer by a cable, it was capable of heating up and cooling down rapidly. In my right hand, I held a controller with a button that I could press to stop the heating on my arm. “Don’t worry; you won’t get burned,” the assistant reassured me.
In the first few trials, Colloca asked me to press the button as soon as I felt the device getting warm. In the next few rounds, I had to wait a little longer until the device felt uncomfortably hot; in the final series of trials, I had to switch it off only when it felt too hot to bear.
Colloca then led me through the same sequence while wearing virtual reality goggles, which immersed me in an oceanic environment. Soothing music played in my ears as I watched dazzlingly colored fish flitting through the water, which was lit up by sunlight filtering down from above. Large iridescent jellyfish floated past. Periodically I felt the device heating up the skin on my forearm, reminding me that I hadn’t gone scuba diving.
When the experiment ended, Colloca showed me the temperatures I had allowed the device to reach in all the trials. The readings for what I felt to be “warm,” “hot,” and “unbearably hot” were all higher during the immersive experience. Specifically, the hottest temperature I could handle without flinching had gone up by 2.7 degrees Fahrenheit, to 118 degrees Fahrenheit, which in Colloca’s view was “huge.”
“That means you were tolerating a much, much higher level of pain when you were immersed in this environment along with calming music,” she says.

Scientists don’t yet know for sure why virtual reality has this positive effect on pain tolerance. Some hypothesize it works through distraction: by engaging networks that would otherwise be involved in signaling and perceiving pain. Others speculate that it works by regulating emotions and altering mood. Colloca has shown that the key driver of the benefit is the entertainment provided by the experience, which helps relax patients and reduce their anxiety. Whatever the mechanisms underlying its effectiveness, doctors already are using virtual reality to help patients in acute pain, such as those with severe burns. Colloca believes the strategy also could prove useful in treating chronic pain.
Every month, Norris leads a meeting of a support group that he helped found a few years ago through the American Chronic Pain Association. The goal is to provide members with informal group therapy, applying the emerging scientific insight that our thoughts and feelings can alter our experience of pain.
I joined Norris at a recent gathering at a Los Angeles church, and he introduced me to the members as they trickled in. (To respect their privacy, I decided not to ask for their last names.) One of them, a slender young man named Brian, shook my hand. When I explained to him, as I did with the others, that I’d come to listen, not to participate, he joked: “Maybe we should punch you in the face so you can relate.”
There were 10 of us in all—five men and five women. We arranged our chairs in a circle and sat down. Resting his cane against a table, Norris settled into his seat and asked the members to share how things had been going for them.
Brian, who suffers from severe abdominal pain that doctors haven’t been able to diagnose, was the first to speak. He described going to a jujitsu class, which he said helped him temporarily forget his pain. “It’s sad that I have to cause myself other pain to forget this one,” he laughed. “I thought of all you guys throughout the week. It made me feel better.”
The members are familiar with each other’s stories. But they seemed bound by an unspoken contract to listen to everyone with full attention, even if they’d heard the same words before. “I called a suicide hot line today,” a woman named Jane said. She suffers from fibromyalgia and complex regional pain syndrome, among other issues. “I’ve complained to my friends so much that I don’t want to call them anymore.”
Norris told her and the rest of the group that he’s just a phone call away. “Sometimes you just need to scream,” he said. Turning to another woman in the group who’d admitted earlier to being reluctant to reach out for support, he said, “So please, yell.”
When the meeting was over, Norris waited for everybody to file out of the room before turning out the lights. I asked what inspired him to organize the monthly meeting. “I find that my experiences are often helpful to others,” he said. But this was just as much about helping himself, he added. “These meetings help me feel like I am still a contributing member of society, and I am not alone in dealing with chronic pain.”