
The Secrets of Sleep
From birth, we spend a third of our lives asleep. After decades of research, we’re still not sure why.
Cheryl Dinges is a 29-year-old Army sergeant from St. Louis. Her job is to train soldiers in hand-to-hand combat. Specializing in Brazilian jujitsu, Dinges says she is one of the few women in the Army certified at level 2 combat. Level 2 involves a lot of training with two attackers on one, she explains, with the hope of “you being the one guy getting out alive.”

Dinges may face an even harder fight in the years ahead. She belongs to a family carrying the gene for fatal familial insomnia. The main symptom of FFI, as the disease is often called, is the inability to sleep. First the ability to nap disappears, then the ability to get a full night’s sleep, until the patient cannot sleep at all. The syndrome usually strikes when the sufferer is in his or her 50s, ordinarily lasts about a year, and, as the name indicates, always ends in death. Dinges has declined to be tested for the gene. “I was afraid that if I knew that this was something I had, I would not try as hard in life. I would allow myself to give up.”
FFI is an awful disease, made even worse by the fact that we know so little about how it works. After years of study, researchers have figured out that in a patient with FFI, malformed proteins called prions attack the sufferer’s thalamus, a structure deep in the brain, and that a damaged thalamus interferes with sleep. But they don’t know why this happens, or how to stop it, or ease its brutal symptoms. Before FFI was investigated, most researchers didn’t even know the thalamus had anything to do with sleep. FFI is exceedingly rare, known in only 40 families worldwide. But in one respect, it’s a lot like the less serious kinds of insomnia plaguing millions of people today: It’s pretty much a mystery.
If we don’t know why we can’t sleep, it’s in part because we don’t really know why we need to sleep in the first place. We know we miss it if we don’t have it. And we know that no matter how much we try to resist it, sleep conquers us in the end. We know that seven to nine hours after giving in to sleep, most of us are ready to get up again, and 15 to 17 hours after that we are tired once more. We have known for 50 years that we divide our slumber between periods of deep-wave sleep and what is called rapid eye movement (REM) sleep, when the brain is as active as when we’re awake, but our voluntary muscles are paralyzed. We know that all mammals and birds sleep. A dolphin sleeps with half its brain awake so it can remain aware of its underwater environment. When mallard ducks sleep in a line, the two outermost birds are able to keep half of their brains alert and one eye open to guard against predators. Fish, reptiles, and insects all experience some kind of repose too.
All this downtime comes at a price. An animal must lie still for a great stretch of time, during which it is easy prey for predators. What can possibly be the payback for such risk? “If sleep doesn’t serve an absolutely vital function,” the renowned sleep researcher Allan Rechtschaffen once said, “it is the greatest mistake evolution ever made.”
The predominant theory of sleep is that the brain demands it. This idea derives in part from common sense—whose head doesn’t feel clearer after a good night’s sleep? But the trick is to confirm this assumption with real data. How does sleeping help the brain? The answer may depend on what kind of sleep you are talking about. Recently, researchers at Harvard led by Robert Stickgold tested undergraduates on various aptitude tests, allowed them to nap, then tested them again. They found that those who had engaged in REM sleep subsequently performed better in pattern recognition tasks, such as grammar, while those who slept deeply were better at memorization. Other researchers have found that the sleeping brain appears to repeat a pattern of neuron firing that occurred while the subject was recently awake, as if in sleep the brain were trying to commit to long-term memory what it had learned that day.

Such studies suggest that memory consolidation may be one function of sleep. Giulio Tononi, a noted sleep researcher at the University of Wisconsin, Madison, published an interesting twist on this theory a few years ago: His study showed that the sleeping brain seems to weed out redundant or unnecessary synapses or connections. So the purpose of sleep may be to help us remember what’s important, by letting us forget what’s not.
Sleep is likely to have physiological purposes too: That patients with FFI never live long is likely significant. A lot of interest has focused on what exactly kills them, but we still don’t know. Do they literally die from lack of sleep? And if not, to what extent does sleeplessness contribute to the conditions that kill them? Some researchers have found that sleep deprivation impedes wound healing in rats, and others have suggested that sleep helps boost the immune system and control infection. But these studies are not conclusive.
In the most famous attempt to figure out why we sleep, in the 1980s, Rechtschaffen forced rats to stay awake in his University of Chicago lab by placing them on a disk suspended on a spindle over a tank of water. If the rats fell asleep, the disk would turn and throw them in the water; when they fell into the water, they immediately woke up. After about two weeks of this strict enforcement of sleeplessness, all the rats were dead. But when Rechtschaffen performed necropsies on the animals, he could not find anything significantly wrong with them. Their organs were not damaged; they appeared to have died from exhaustion—that is, from not sleeping. A follow-up experiment in 2002, with more sophisticated instruments, again failed to find “an unambiguous cause of death” in the rats.
At Stanford University I visited William Dement, the retired dean of sleep studies, a co-discoverer of REM sleep, and co-founder of the Stanford Sleep Medicine Center. I asked him to tell me what he knew, after 50 years of research, about the reason we sleep. “As far as I know,” he answered, “the only reason we need to sleep that is really, really solid is because we get sleepy.”
Unfortunately, the reverse is not always true; we don’t always get sleepy when we need to sleep. Insomnia is at epidemic levels in the developed world. Fifty to 75 million Americans, roughly a fifth of the population, complain about problems sleeping. Fifty-six million prescriptions for sleeping pills were written in 2008, up 54 percent over the previous four years. The revenue for sleep centers is expected to approach four and a half billion dollars by 2011. Yet remarkably little is being done to understand the root causes of insomnia. Most medical school students get no more than four hours of training on sleep disorders; some get none. Family doctors’ health questionnaires often don't even ask about sleep.
The social and economic costs from the undertreatment of sleeplessness are huge. The Institute of Medicine, an independent national scientific advisory group, estimates nearly 20 percent of all serious motor vehicle accidents are associated with driver sleepiness. It places the direct medical cost of our collective sleep debt at tens of billions of dollars. The loss in terms of work productivity are even higher. Then there are the softer costs—the damaged or lost relationships, the jobs tired people don't have the energy to apply for, the muting of enjoyment in life’s pleasures.
If a medical problem in some less private, less mysterious bodily function were causing such widespread harm, governments would declare war on it. But the National Institutes of Health contributes only about $230 million a year to sleep research—comparable to the amount that the manufacturers of the popular sleeping pills Lunesta and Ambien spent in one season on television advertising in 2008. The military also spends money investigating sleep, but its primary mission is keeping soldiers up and ready to fight, not ensuring they get a good night’s rest. As a result the fight against insomnia is largely left to drug companies and commercial sleep centers.
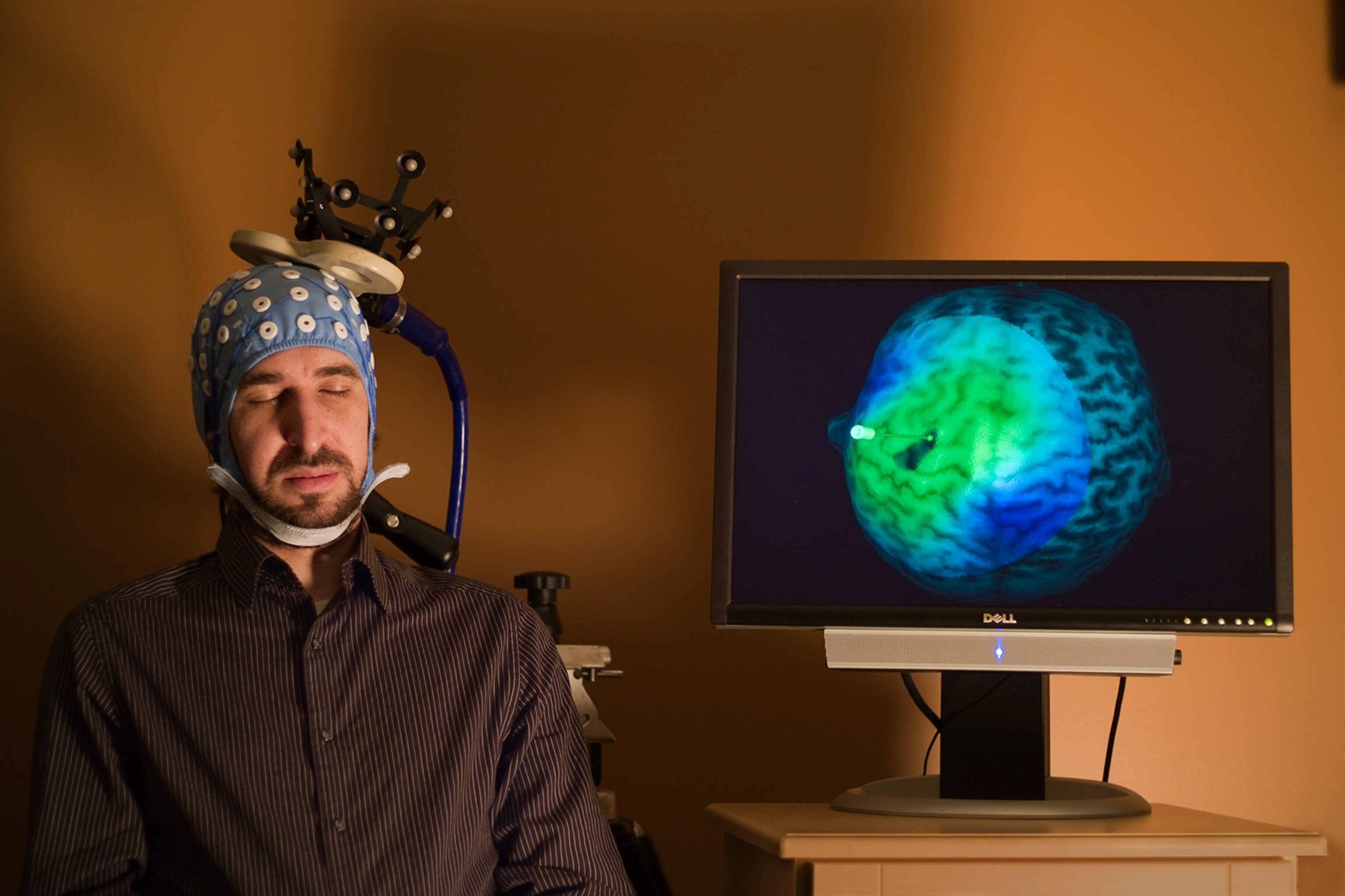
“Sleep has been the Rodney Dangerfield of medicine,” says John Winkelman, medical director of the Brigham and Women’s Hospital’s Sleep Health Center in Brighton, Massachusetts. “It just gets no respect.”
One early afternoon last year I paid a visit to the Sleep Medicine Center at Stanford. The clinic, founded in 1970, was the first in the country devoted to the problem of insomnia, and it remains among the most important. The sleep center sees over 10,000 patients a year and does more than 3,000 overnight sleep studies. The 18 bedrooms that patients occupy looked comfortable, the beds soft and cozy. The monitoring equipment was hidden in the furniture.
The main diagnostic tool at the clinic is the polysomnogram, the main element of which is the electroencephalograph (EEG), which captures the electrical output from a sleeping patient’s brain. As you fall asleep, your brain slows down, and its electrical signature changes from short jagged waves to longer rolling ones, much the way the movement of the sea smooths out the farther you get from shore. In the brain these gentle undulations are interrupted periodically by a renewal of the sudden agitated mental activity of REM sleep. For unknown reasons, REM is the time during sleep when we do nearly all our dreaming.
As the EEG records this fitful voyage, the polysomnogram technicians also measure body temperature, muscle activity, eye movement, heart rhythms, and breathing. Then they look over the data for signs of abnormal sleep or frequent wake-ups. When a person has narcolepsy, for instance, he or she plunges from wakefulness into REM sleep without any intermediate steps. In fatal familial insomnia, the sufferer can never get past the first stages of sleep; body temperature soars and crashes.
FFI and narcolepsy cannot be diagnosed without EEGs and other monitoring devices. But Clete Kushida, the clinic director, told me he can spot most people’s sleep problems right at the intake interview: There are those who cannot keep their eyes open, and those who just speak of their exhaustion but don’t actually nod off. The former often have sleep apnea. The latter have what Kushida calls “true insomnia.”
In obstructive sleep apnea sufferers, the muscle relaxation that comes with sleep allows the soft tissue of the throat and esophagus to close, shutting off the sleeper’s air passage. When the brain realizes it is not getting oxygen, it sends an emergency signal to the body to wake up. The sleeper awakes, takes a breath, the brain is replenished, and sleep returns. A night’s sleep for an apnea sufferer turns out to really be a hundred micro-naps. Sleep apnea is the behemoth of the sleep center business. Brigham and Women’s John Winkelman says that at his sleep center, two-thirds of those examined are diagnosed with the condition.
Apnea is a serious problem, implicated in increased risk for heart attacks and stroke. But it is only indirectly a sleep disease. True insomniacs—people diagnosed with what some sleep doctors call psychophysiological insomnia—are people who either can’t get to sleep or can’t stay asleep for no evident reason. They wake up and don’t feel rested. They lie down and their brains whir. This group makes up about 25 percent of those seen in sleep clinics, according to Winkelman. The Institute of Medicine estimates that over all, there are 30 million people with this condition in the United States.
While apnea can be treated with a device that forces air down the sleeper’s throat to keep the airways open, the treatment of classic insomnia is not so clear-cut. Acupuncture may help—it has long had this role in Asian medicine and is being studied at the University of Pittsburgh sleep center now.
Typically, psychophysiological insomnia is treated with a two-part approach. First come the sleeping pills, most of which work by enhancing the activity of GABA, a neurotransmitter that regulates overall anxiety and alertness in the body. Though safer than they once were, sleeping pills can lead to psychological addiction. Many users complain that their sleeping-pill sleep seems different, and they feel hungover when they wake up. “Sleeping pills are not a natural way to sleep,” points out Charles Czeisler, director of the Harvard Work Hours, Health and Safety Group. Pills can make future insomnia worse, too, a drawback called rebound insomnia.
The second step in treating true insomniacs is usually cognitive behavioral therapy (CBT). In CBT, a specialized psychologist teaches the insomniac to think about his or her sleep problems as manageable, even solvable—that’s the cognitive part—and to practice good “sleep hygiene.” Good sleep hygiene mostly amounts to tried-and-true advice: Sleep in a dark room, go to bed only when you are sleepy, don’t exercise before bed. Studies have shown that CBT is more effective than sleeping pills at treating long-term insomnia, but many sufferers aren’t convinced. “Some people continue in my experience to struggle,” says Winkelman. “They’re not super-satisfied with their sleep.”
Winkelman thinks CBT is better at helping some kinds of insomniacs than others. Insomnia covers a multitude of conditions. Between FFI, which is extremely rare, and apnea, which is very common, there are almost 90 recognized sleep disorders and a host of harder to codify reasons people can't sleep. Some insomniacs suffer from restless legs syndrome (RLS), an intense discomfort in their limbs that prevents falling asleep, or periodic limb movement disorder (PLMD), which produces involuntary kicking during sleep. Narcoleptics often have difficulty both staying asleep and staying awake. Then there are people who can’t sleep because of depression, and people who are depressed because they can’t sleep. Others have problems sleeping because of dementia or Alzheimer’s disease. Some women sleep badly during their periods (women are twice as likely to have insomnia as men) and many during menopause. Older people in general sleep less well than young. Some insomniacs can’t sleep because they are on medications that keep them awake. Others are worrying about work or soon having no work; one-third of Americans report they have lost sleep in the recent economic crisis. Of all these non-sleepers, patients with insomnia derived from physical internal causes—probably excesses or scarcities of various neurotransmitters—are likely the ones least able to respond to the treatment.
Yet for most of these conditions, CBT is offered as a potential cure. Perhaps this is because the problem of insomnia was for a long time the purview mainly of psychologists. In their eyes, insomnia is generally caused by something treatable through their tool kit, usually anxiety or depression. By extension, cognitive behavioral therapy asks the sleeper to think about what he or she is doing wrong, not what is wrong with his or her body. Winkelman wishes that the two aspects of sleep—the physical and the mental—were more often considered jointly. “Sleep is extraordinarily complicated,” he says. “Why would we think that there couldn’t be something in the wiring that goes awry too?”

If we can’t sleep, perhaps it’s because we’ve forgotten how. In premodern times people slept differently, going to bed at sunset and rising with the dawn. In winter months, with so long to rest, our ancestors may have broken sleep up into chunks. In developing countries people still often sleep this way. They bed down in groups and get up from time to time during the night. Some sleep outside, where it is cooler and the effect of sunlight on our circadian rhythm is more direct. In 2002, Carol Worthman and Melissa Melby of Emory University published a comparative survey of how people sleep in a variety of cultures. They found that among foraging groups such as the !Kung and Efe, “the boundaries of sleep and waking are very fluid.” There is no fixed bedtime, and no one tells anyone else to go to sleep. Sleepers get up when a conversation or musical performance intrudes on their rest and intrigues them. They might join in, then nod off again.
No one in developed nations sleeps this way today, at least not on purpose. We go to bed near a fixed time, sleep alone or with our partner, on soft cushions covered with sheets and blankets. We sleep on average about an hour and a half less a night than we did just a century ago. Some of our epidemic of insomnia or sleeplessness is probably just our refusal to pay attention to our biology. The natural sleep rhythms of teenagers would call for a late morning wake-up—but there they are, starting high school at 8 a.m. The night shift worker sleeping in the morning is fighting ancient rhythms in his or her body that order him or her awake to hunt or forage when the sky is flooded with light. Yet he or she has no choice.
We fight these forces at our peril. In February 2009 a commuter jet en route from Newark to Buffalo crashed, killing all 49 aboard and one on the ground. The copilot, and probably the pilot, had only sporadic amounts of sleep the day leading up to the crash, leading the National Transportation Safety Board to conclude that their performance “was likely impaired because of fatigue.” This sort of news enrages Harvard’s Charles Czeisler. He notes that going without sleep for 24 hours or getting only five hours of sleep a night for a week is the equivalent of a blood alcohol level of 0.1 percent. Yet modern business ethic celebrates such feats. “We would never say, ‘This person is a great worker! He’s drunk all the time!’” Czeisler wrote in a 2006 Harvard Business Review article.
Starting in 2004, Czeisler published a series of reports in medical journals based on a study his group had conducted of 2,700 first-year medical residents. These young men and women work shifts that are as long as 30 hours twice a week. Czeisler’s research revealed the remarkable public health risk that this sleep debt entailed. “We know that one out of five first-year residents admits to making a fatigue-related mistake that resulted in injury to a patient,” he told me in the spring of 2009. “One in 20 admits to making a fatigue-related mistake that resulted in the death of a patient.” When Czeisler came out with this information, he expected hospitals to thank him. Instead many “circled the wagons.” He despairs of anything being done until U.S. employers get serious about insomnia and sleepiness. “My conviction is that one day people will look back on what will be viewed as a barbarous practice.”

Now consider the siesta. The timing of the traditional siesta corresponds to a natural post-lunch dip in our circadian rhythms, and studies have shown that people who catnap are generally more productive and may even enjoy lower risk of death from heart disease. It is the Spanish who have made the siesta famous. Unfortunately, Spaniards no longer live close enough to work to go home and nap. Instead some use the afternoon break to go out for long lunches with friends and colleagues. Having spent two hours at lunch, Spanish workers then cannot finish work until seven or eight. But even then they don’t always go home. They go out for drinks or dinner instead. (Go to a Spanish disco at midnight and you’re likely to be dancing alone; their prime-time TV shows are just ending.)
Lately the Spanish have begun to take the problem of sleep deprivation seriously. The police now question drivers in serious accidents about how long they slept the night before, and the government has recently mandated shorter hours for its employees to try to get them home earlier.
What has motivated the Spanish to take action against sleepiness is not so much their accident rate—historically among the highest in western Europe—as their flat productivity. The Spanish spend more time at work and their productivity is less than most of their European neighbors. “It’s one thing to log hours, another to get something done,” Ignacio Buqueras y Bach, a 68-year-old businessman who has spearheaded the attempt to get Spaniards to bed earlier, lectured his countrymen in a Madrid newspaper recently.
“Every once in a while we have to close our eyes,” Buqueras told me. “We’re not machines.”
In 2006 a commission formed by Buqueras to change things became part of the Spanish government. Two years later I had occasion to go to one of the commission’s meetings in the annex to the Congreso de los Diputados, the lower house of Spain’s legislative branch. An assortment of modern Spanish grandees testified to the problem. They spoke of accidents by tired workers, Spanish women doubly exhausted by long work hours and household duties, and small children deprived of their proper ten to twelve hours of sleep. Members were urged to contact the television networks to see if they would consider moving prime time earlier.
Buqueras kept the meeting moving, exhorting the speakers to adhere to a “telegraphic brevity.” But the lights were low and the room warm. In the audience a few participants’ heads began to slump to their chests, then pop back up as they resisted, then their eyes closed more fully, their programs lowering to their laps, as they began to pay back their nation’s sleep debt.


