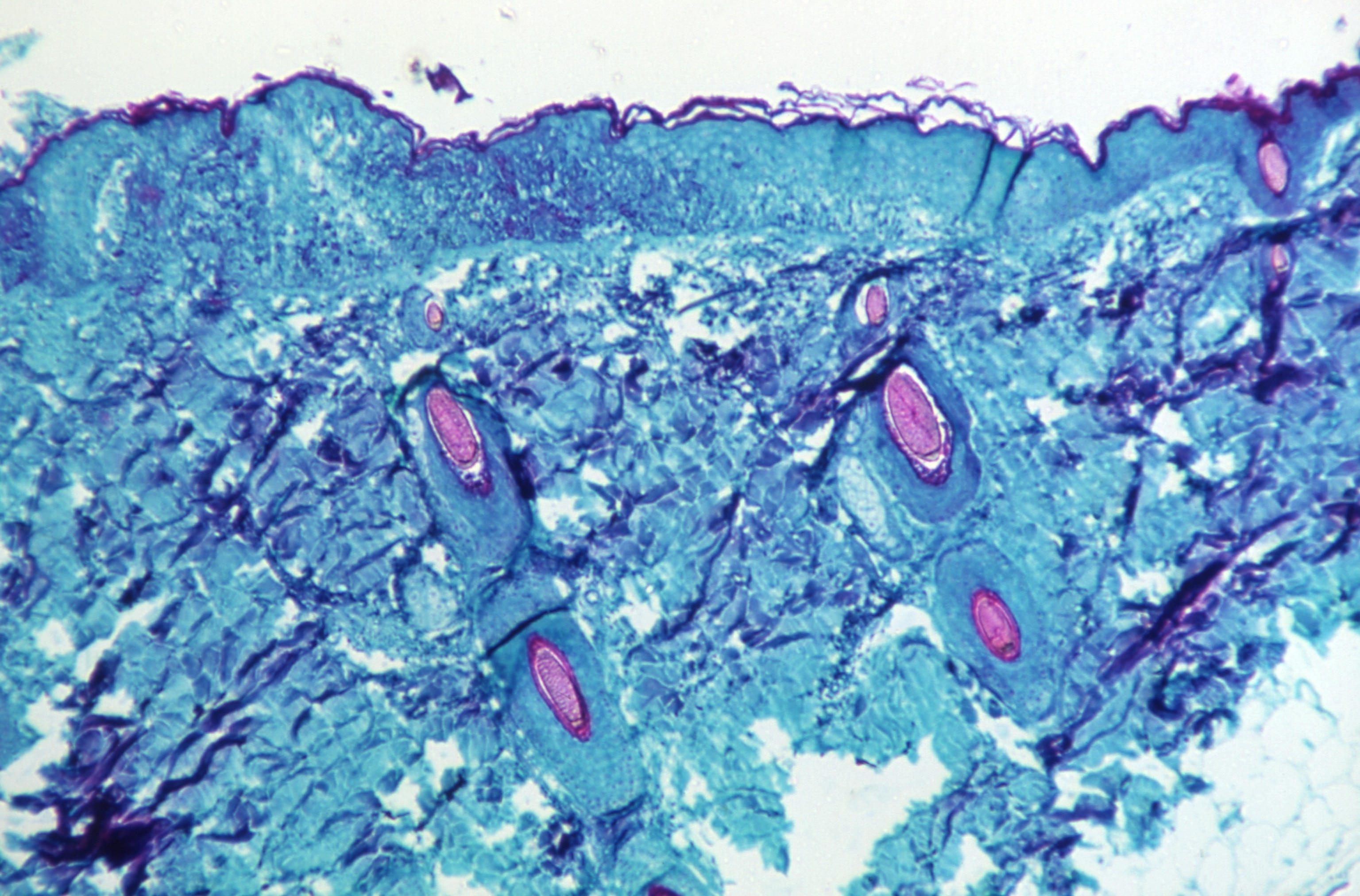
Why monkeypox cases are still rising at such an alarming rate
The U.S. had tools to contain this virus, which is far less contagious than COVID-19. So what went wrong?
Unlike COVID-19, the monkeypox virus requires intimate, often skin-to-skin contact with an infected individual’s rashes, scabs, bodily fluids, or contaminated linens to spread. So with at least some known transmission routes, available diagnostic tests, and two vaccines on offer, monkeypox should have been easy to manage in the United States.
And yet cases—most among men who have sex with other men—are still rising at such an alarming rate that the federal government has now declared monkeypox a public health emergency, leaving many people baffled about what went wrong.
Since May more than 80 countries where monkeypox is not endemic have reported nearly 28,000 cases, including about 7,500 in the U.S. All states except Montana and Wyoming have confirmed cases, but more than half have been recorded in New York, California, Illinois, Florida, and Texas.
Part of the problem is that “by the time we were aware of this [in May], there was already probably substantial transmission in the community,” says Wafaa El-Sadr, an infectious disease physician and epidemiologist at Columbia University in New York City. And according to public health experts, the ongoing crisis has been exacerbated by inadequate access to testing, misdiagnosis, limited availability of the vaccine, and—until very recently—a cumbersome prescription process for the only available antiviral drug.

“When you have an infectious disease that’s spread through contact and appears in a community where it circulates through social and sexual networks, and the main tool to prevent the spread—the vaccine—isn’t easily available, it’s not surprising we’re seeing the situation we’re seeing right now,” says El-Sadr.
Other contributing factors include poor understanding of suspected routes—such as sexual transmission via semen or vaginal fluids—and a lack of financial support for people who cannot afford to miss work. Infected individuals must isolate for 21 days; that can be a huge challenge, especially for low-income communities of color, undocumented immigrants, and transgender people who may already be struggling to access healthcare, says Jason Cianciotto, vice president of communications and public policy at the New York City nonprofit Gay Men’s Health Crisis.
It’s also possible asymptomatic or mild cases are going unnoticed, which might make current case counts a gross underestimate.
“We’re seeing cases that more likely have classic symptoms, but I suspect that there may be many more where the disease may be mild and the person gets better on their own or their case is misdiagnosed,” El-Sadr says. “I fear what we’re counting is likely the tip of the iceberg.”
But while the federal response has been slow, declaring monkeypox a public health emergency could help mobilize resources, streamline data collection, and cut through red tape so that states and local governments can better respond, according to some public health experts.
Where is the monkeypox vaccine?
A two-dose vaccine called Jynneos can be given to people exposed to the virus or at risk of getting infected. A single-dose vaccine called ACAM2000 is approved for smallpox and can be given for monkeypox, but the Centers for Disease Control and Prevention caution that the jab produces more adverse side effects, especially in immunocompromised people like those with HIV. Surveillance data from the U.S., England, and the European Union, indicated that in monkeypox cases in which HIV status was known, between 28 and 51 percent had HIV infections.
For the severely ill, some medical professionals are prescribing a smallpox antiviral called tecovirimat, or Tpoxx, that can be used to treat monkeypox.
Currently, though, the vaccine supply is nowhere close to meeting demand among the eligible population, which includes men who have sex with men, sex workers, and healthcare staff exposed to the virus.
San Francisco has been running through its allotted vaccines at a rapid clip, says the city’s health officer Susan Philip. At the Zuckerberg San Francisco General Hospital, the city’s only drop-in monkeypox vaccination site, “there are lines that stretch for several blocks when vaccines are available,” Philip says.
The situation is similar in New York City. “Amongst my friends, we jokingly consider it like a Hunger Games activity to try to get a vaccination slot,” says 28-year-old New Yorker William McChriston, who got his first monkeypox vaccine dose on July 24. The FDA has stressed administering the second dose 28 days after the first, but it’s unclear when McChriston will get his second dose because the city is prioritizing the first jab to get more people at least partially protected.
The supply problems create extra hurdles for people who aren’t digitally savvy and those who don’t readily have access to the internet or are working at 6 p.m., which is when appointments in New York go live and then get booked up within minutes.
“The virus is taking advantage of the runway that it’s been given, and I think we’ll continue to see a lot more cases,” says Anne Rimoin, an infectious disease epidemiologist at the University of California, Los Angeles, given the highly interconnected social and sexual network within which the virus is quickly spreading (although the virus can infect anyone who comes in close contact with an infected patient) and no prior immunity.
How does declaring a public health emergency help?
Although monkeypox doesn’t spread as easily as SARS-CoV-2, the virus that causes COVID-19, the emergency declaration “enables people to pay attention to it,” says El-Sadr. It could also allow for governments at different levels to work together, share information, and potentially tap into additional resources.
For now the emergency announcement doesn’t legally bind state or federal agencies to provide certain cities or jurisdictions with more vaccines, Philip says, but “we’re making the case for it.”
On July 28 the U.S. Department of Health and Human Services announced plans to allocate 786,000 doses of the Jynneos vaccine in addition to the 340,000 that had already been distributed. Their plan is to prioritize areas that have large at-risk populations and high numbers of new cases. “The strategy ensures that jurisdictions have the doses needed to complete the second dose,” according to an HHS press release.
In New York, the emergency declaration extends the pool of personnel who can administer the monkeypox vaccines to include emergency medical service workers, pharmacists, and midwives. Similar to California, it will also mandate that healthcare providers send vaccination data and potentially antiviral prescription data to the state health department.
These data would help public health managers understand how many courses of antiviral medication are being given, where vaccine demand is high, who is getting vaccinated, and how many people come seeking evaluation and testing, Philip says.
So far, the majority of infected individuals are men who have sex with other men, and many are people of color. A recent CDC report revealed that 58 percent of the nearly 1,300 U.S. monkeypox patients who provided data on their race and ethnicity were either Hispanic or Black.
As more people get tested, vaccinated, and use the antiviral Tpoxx, there’s an opportunity to understand even more about this monkeypox strain, which is endemic to West Africa, and how well the treatments currently in use work against it.
Until now, the effectiveness of the Jynneos vaccine and the Tpoxx antiviral have only been formally tested in animals because human trials were either unfeasible or unethical. Real-world data will allow scientists to study how well these therapeutics work, how much immunity a single dose imparts compared to two doses, and the extent to which Tpoxx limits the virus’s spread in the body and contains symptoms, says Amesh Adalja, an infectious disease expert at Johns Hopkins Center for Health Security. “That data collection is happening to some degree,” Adalja says.
The National Institutes of Health will also be testing another injection strategy to stretch the limited vaccine supply by administering smaller doses of Jynneos into the skin rather than under the skin, which is current practice.
There’s also an opportunity to fill in gaps in our understanding about how the virus spreads. A recent study found monkeypox DNA in the semen, saliva, urine, and feces, of some infected individuals. Whether the virus remains infectious in bodily fluids is unclear, although a study published on August 2 suggests that the semen of monkeypox patients could be a source of infection spread.
“Same goes for the risk of transmission from surfaces and respiratory droplets,” El-Sadr says. “We have an endless list of the questions, and this is the moment to mobilize research funding to answer these questions as quickly as possible.”