AI may be key to solving the most neglected women's health issues
Advances in computational science are delivering insights into how to improve maternal mortality, deliver better therapies for breast cancer patients, and more.

Women may comprise half the world’s population, but research on the major conditions affecting their health have long lagged that of men. One way some scientists are trying to change this is by harnessing the power of artificial intelligence and computational medicine to extract findings that would otherwise be missed. Now this approach is yielding new insights into pregnancy complications, endometriosis, maternal mortality, breast and cervical cancers, and other women’s health concerns that are expected to translate into improved care.
Computational science is helping research in women’s health in two main ways, says Tom Yankeelov, director of the Oden Institute’s Center for Computational Oncology at the University of Texas at Austin. One involves using AI’s machine learning to analyze vast data sets to draw broad conclusions. The other extracts information from individual patients to make assessments or predictions applicable specifically for them.
One reason for this progress is that computer runs are now so inexpensive and so fast that scientists can analyze very large data sets at their institutions. For example, one study of deaths of women linked to childbirth in 200 countries required simulating hundreds of thousands of estimated health parameters that could influence the health of women at this pivotal time, says Zachary Ward, a researcher on this project at Harvard’s T.H. Chan School of Public Health. Such an undertaking would not have been feasible even a decade ago, he says. As it was, high-performance computers worked around the clock for a year to crunch all the numbers, revealing factors that could make the most difference in saving lives.
Greater interest from the growing number of young, female engineers has also been crucial in advancing the field, says Michelle Oyen, the director of the Center for Women’s Health Engineering at Washington University in St. Louis, which draws from both the engineering and medical schools. The idea of using computer simulations to study pregnancy problems, as her lab does, “seems to capture young students’ imaginations,” she says. “In many cases, they say, My mom had this or my friend had this. There’s this personal component.”
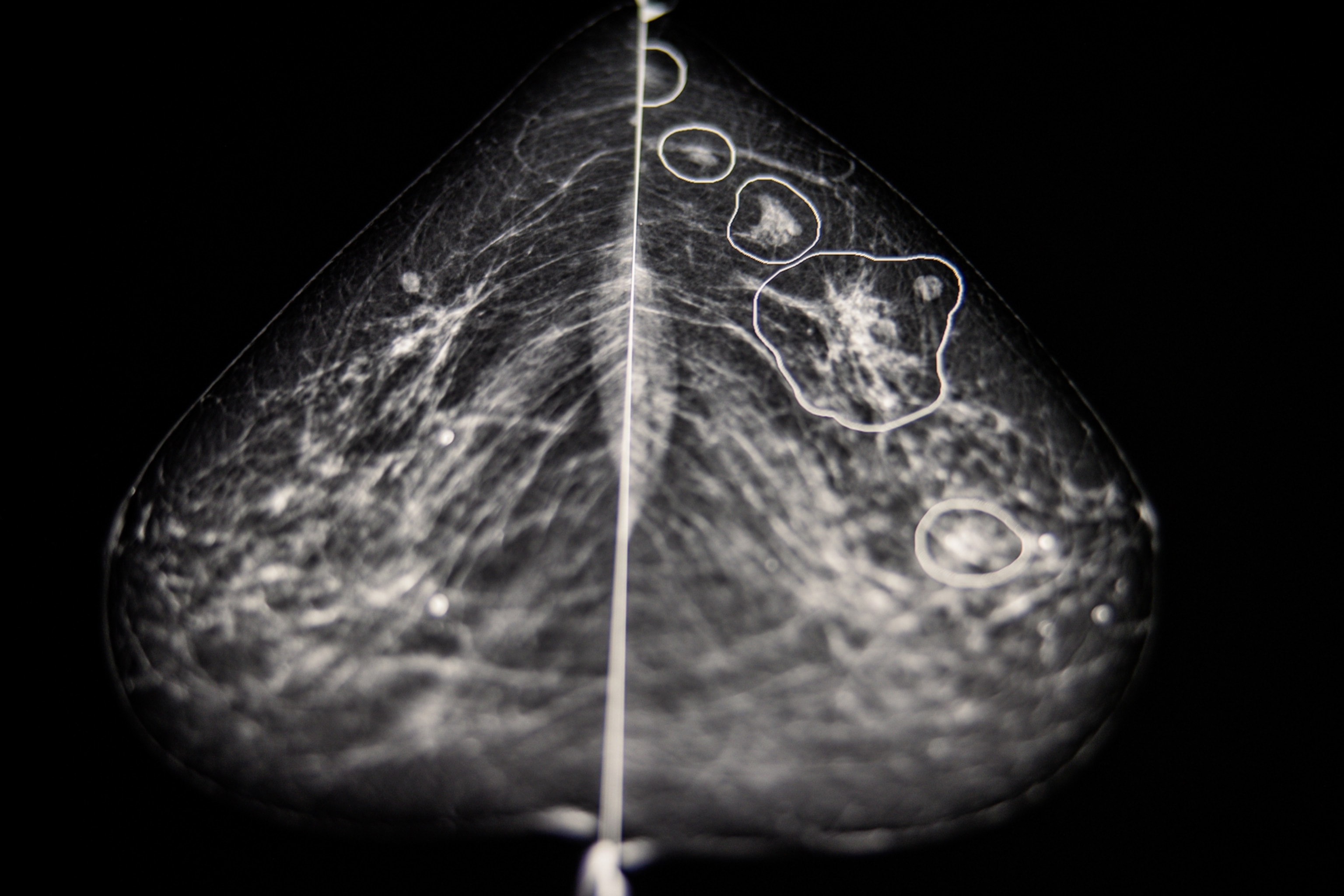
Using math to treat breast cancer
Yankeelov uses the personalized approach in his effort to more effectively treat locally advanced breast cancer (LABC)—where the disease has spread but only to lymph nodes in the armpits. Data are best used from each person, he says, because the many sub-types of breast cancer make each person’s experience and survival prospects unique.
For the most part, medical advances have primarily employed a trial-and-error method in the form of clinical trials. A treatment is deemed successful when it is shown to help the average person, not any one individual. This contrasts with the way other scientific endeavors advance. “When we want to send a satellite into orbit, we don’t launch 100 satellites and hope one of them lands in the right orbit,” he says. A single satellite is sent to its spot by solving mathematical equations physicists and engineers devised.
Yankeelov and his team sought to develop mathematical equations that could be applied to a single LABC patient. They have derived four differential equations that calculate how each tumor grows and responds to treatment. The equations utilize factors known to influence the progression of the disease, like how the tumor cells migrate, proliferate, and interact with the tissue surrounding them, and how they respond to an early course of therapy. Supercomputers then solve these four equations for a specific patient using data culled from magnetic resonance imaging (MRI) of the breast.
Current regimens typically include a standard course of chemotherapy before the tumor is surgically removed. In nearly two-third of cases, however, cancerous cells are left behind, which increases the chances of recurrence. Yankeelov’s equations, currently being tested in an experimental phase, could prove useful for individualizing LABC treatment.
Yankeelov’s study of 56 women with one type of LABC, called triple-negative, found that solving for the equations yielded 89 percent accuracy in determining whether the standard treatment would prove successful. The next step is an upcoming prospective clinical trial using the computerized predictions to personalize treatments, such as giving someone with high odds of failure the option to undergo additional therapies.
Grasping what happens in pregnancy and labor
An individualized approach is also being used to study the uterus of a person in labor. Doctors currently track uterine contractions with a pressure-sensitive device called a tocodynamometer, which detects their length, frequency, and strength. But to better understand what happens in the uterus during preterm labor, or if it stalls during delivery, more detailed information is needed, says Yong Wang, an associate professor in both the engineering and medical schools at Washington University in St. Louis.
Wang and his colleagues have created a unique detection device—called an electromyometrial imaging system—which is placed on the abdomen and contains 250 electrodes that record a half-million bits of data per second. Computers transform the data into real-time, dynamic visual images of the uterus as it experiences each contraction (a representation known as a digital twin).
“For the first time, this is allowing us to noninvasively evaluate human uterine function in three-dimensional space over time,” Wang says.
When the contractions of 55 laboring women were tracked with the device, detailed 3D images documented what happens inside the womb, including clearly portraying how distinct parts of the uterus activate as a contraction progresses.
Wang envisions a future where all patients’ labor is tracked in this way, with the computations quickly yielding real-time visual images for healthcare practitioners to watch on a screen. The device is also being used to study uterine conditions outside of pregnancy, including fertility, painful menstruations, and endometriosis. [Read more in Endometriosis Is Common, Incredibly Painful—and Often Misdiagnosed.]
Michelle Oyen is also working to understand pregnancy; she is focusing on the placenta, which provides nutrients and oxygen to the fetus. For something so vital to human existence, surprisingly little is known, she says. This lack of understanding affords obstetricians few tools—bed rest, for example, or a Cesarean section—when placental problems emerge.
Oyen relies on machine learning to create a dynamic computational model of the placenta. “We take the geometry of the structure and properties of the tissues and put them into the computer, then explore what happens if you vary the properties of the tissues over hundreds of simulations,” she says. This research cannot be done in people for obvious ethical reasons, nor in animals because their placentas are markedly different, she says.
Such modeling studies are expected to help scientists understand the placenta’s role when, say, fetal growth slows abnormally (the subject of an ongoing, multicenter clinical trial), or when a pregnancy complication like preeclampsia—a life-threatening condition in which the placenta is known to play a role—emerges.
Oyen is also digitally probing the fluid-filled sac in which the fetus resides. In approximately three percent of women worldwide, this vast network of collagen membranes that make up the amniotic sac ruptures prematurely, often before the fetus can survive. Subjecting individual fibers to virtual pressure and tears illuminates the cascade of events that may trigger such a rupture, perhaps one day allowing in utero repairs before a minor problem becomes catastrophic.
Using big data for big objectives
Largescale simulations form the backbone of Zachary Ward’s efforts to improve women’s health around the world. Based on globally available data, his team calculates possible factors contributing to maternal mortality—the amount of prenatal care pregnant women in each country receives, for example, or their rates of high blood pressure or access to medical birthing facilities—using over 400,000 medical, social, economic, and other parameters.
Even though it has dropped more than 40 percent in the last 30 years, such mortality remains stubbornly high. Simulating potential interventions across the developing world has allowed Ward’s team to identify those that might have the largest impacts.
The results of these exhaustive computer runs revealed that no single intervention is sufficient on its own. “We’re finding there’s little point to doing one thing at a time. There needs to be comprehensive, integrated strategies specific to each country,” he says. Improving the quality of birthing facilities and encouraging more women to deliver there can keep pregnant women alive in many parts of the world, for instance, but this is insufficient without simultaneously ensuring that enough trained healthcare providers can staff those facilities or that women have access to birth control.
Similar conclusions emerged from simulations on reducing global deaths from cervical cancer. Introducing imaging devices won’t help, for instance, without also increasing chemotherapy agents, trained oncologists, and radiation therapy capabilities, the scientists found.
Although the computer calculations didn’t yield any single, definitive interventions, Ward says gathering such information is crucial. “I would like to see policymakers make data-driven decisions,” he says. As he and other scientists continue to use computational science for women’s health, such a prospect becomes more likely.