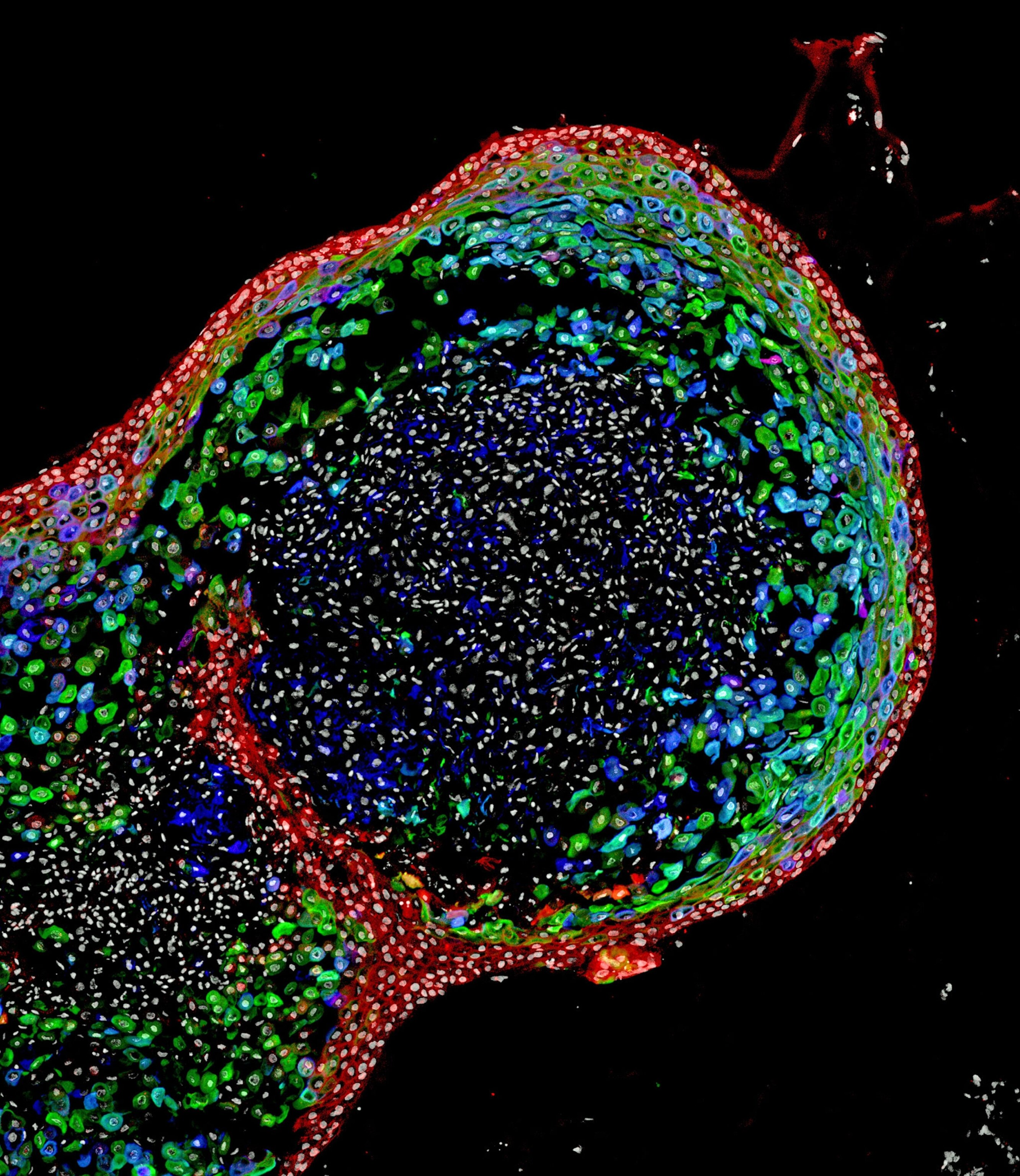
Here’s something to digest: Scientists in Cincinnati have grown miniature versions of an esophagus, the organ responsible for guiding your food to your stomach. And in a first, they did it entirely using human stem cells.
Called organoids, these tiny balls of lab-grown tissue resemble a real human esophagus, the researchers report today in the journal Cell Stem Cell. Previously, scientists succeeded in growing all sorts of organoids—stomachs, kidneys, brains, and even an esophagus made using mature patient tissue as the starting material. (Here’s how one team used a spinach leaf to create a mini beating heart.)
These tiny organs-in-a-dish help scientists study how organs develop normally, and they’re used to figure out how these body parts go wrong, giving rise to cancer and other disorders.
“Three-dimensional laboratory models of human esophagus are badly needed, especially since the mouse anatomy is fundamentally different to a human’s,” says Rebecca Fitzgerald, an esophageal cancer researcher at the University of Cambridge who wasn’t involved in the study.
And since organoids act as a kind of stand-in for the real thing, they can also be used to test drugs to better predict how patients might respond to different treatments. (For instance, artificial wombs may help with premature births.)
“Because they grow in a petri dish, we can poke and prod them all we want,” says James Wells, senior author on the new study and chief scientific officer of the Cincinnati Children's Center for Stem Cell and Organoid Medicine.
Follow the Recipe
Wells and his colleagues started with induced pluripotent stem cells, a kind of “master” cell that has the ability to become any other cell in the body. To make them turn into specialized esophagus cells, investigators added a mixture of chemicals and proteins to the stem cells.
“These act as cues or signals that help to guide those pluripotent stem cells into specifically forming esophageal tissues,” Wells says. “It’s like following a recipe.”
One key step in this recipe was the gene Sox2 and its associated protein, which have been linked to esophageal conditions. The team found that this gene plays a central role in helping the esophagus develop in a human embryo. It took about two months to grow the tiny blobs—each about a millimeter wide—in the lab. (Other researchers have used human stem cells to grow sheep-human hybrids to help with organ regeneration.)
Wells and his Cincinnati team are already growing a few organoids to help diagnose patients who have medical conditions that affect the esophagus, like congenital birth defects. It’s part of the hospital’s bigger effort to create personalized mini-organs from pediatric patients with gastrointestinal disorders.
“So let’s just say, in the clinic they’ve done everything they can to figure out what’s wrong with the patient using all the standard clinical tests,” Wells explains.
The patient gets put into a custom-made MRI machine, which renders a 3-D image of the child’s organs. That image is sent to a team of surgeons, who will try to figure out if the organs can be surgically repaired. Meanwhile, doctors take a tiny piece of tissue from the patient and send it off to Wells’ lab, which makes stem cells from the tissue sample and then grows the organoids. Being able to examine these mini-organs up close, outside of a patient, can lead to a diagnosis.
Opening Up Possibilities
In the future, Wells hopes to be able to grow organoids that could be transplanted back into patients born with unhealthy or missing esophagus tissue. He says this could also work in adults who have had parts of their esophagus removed due to cancer.
“In the long term, we want to make tissue to help the surgeons reconstruct the esophagus in cases where there’s too much missing for the surgeon to correct,” Well says. But that’s likely several years away.
Using stem cells as a starting material “may be a major plus, since some patients may lack healthy esophageal tissue from which to try to engineer a new esophagus,” says Paul Knoepfler, a stem cell biologist at the University of California, Davis, School of Medicine.
It’s also possible that esophageal organoids made from stem cells rather than patient tissue may grow bigger or produce more types of cells that occur naturally in the esophagus, he says. One thing that was missing from the esophagus-in-a-dish, for instance: The open space where food and liquids would go, called the lumen.