
Can We Stop Mosquitoes From Infecting the World?
Mosquitoes carrying dangerous viruses like Zika are spreading worldwide. Some even hide underground. Scientists struggle to find new weapons to control them.
Update: The World Health Organization declared Zika a global emergency on Monday. The declaration by the UN agency likely will increase funding and research efforts to control the outbreak.
Somewhere beneath the mounds of snow covering Washington, D.C.’s Capitol Hill district, just steps from the Library of Congress, a cluster of tropical mosquitoes capable of carrying Zika and other viruses is holed up, waiting for spring.
Washington, D.C. is well beyond the comfort zone for these mosquitoes—this species can’t survive winters north of Alabama and South Carolina. But this colony has somehow hung on for four years, genetic evidence shows, making it the northernmost permanent outpost for the disease-transmitters Aedes aegypti known to date.
This particular colony is small, virus-free, and poses no health threat, say the scientists who’ve been monitoring it. But its existence shows the species is adapting to cold climates and conquering new territory: another sign of the growing threat that insect-borne diseases pose in a rapidly changing world.
“It’s still amazing to me,” says entomologist David Severson, a Notre Dame University professor and member of the research team that last week released news of the underground mosquitoes. “Clearly the climate of Washington D.C. is not hospitable enough for them to survive above ground.”
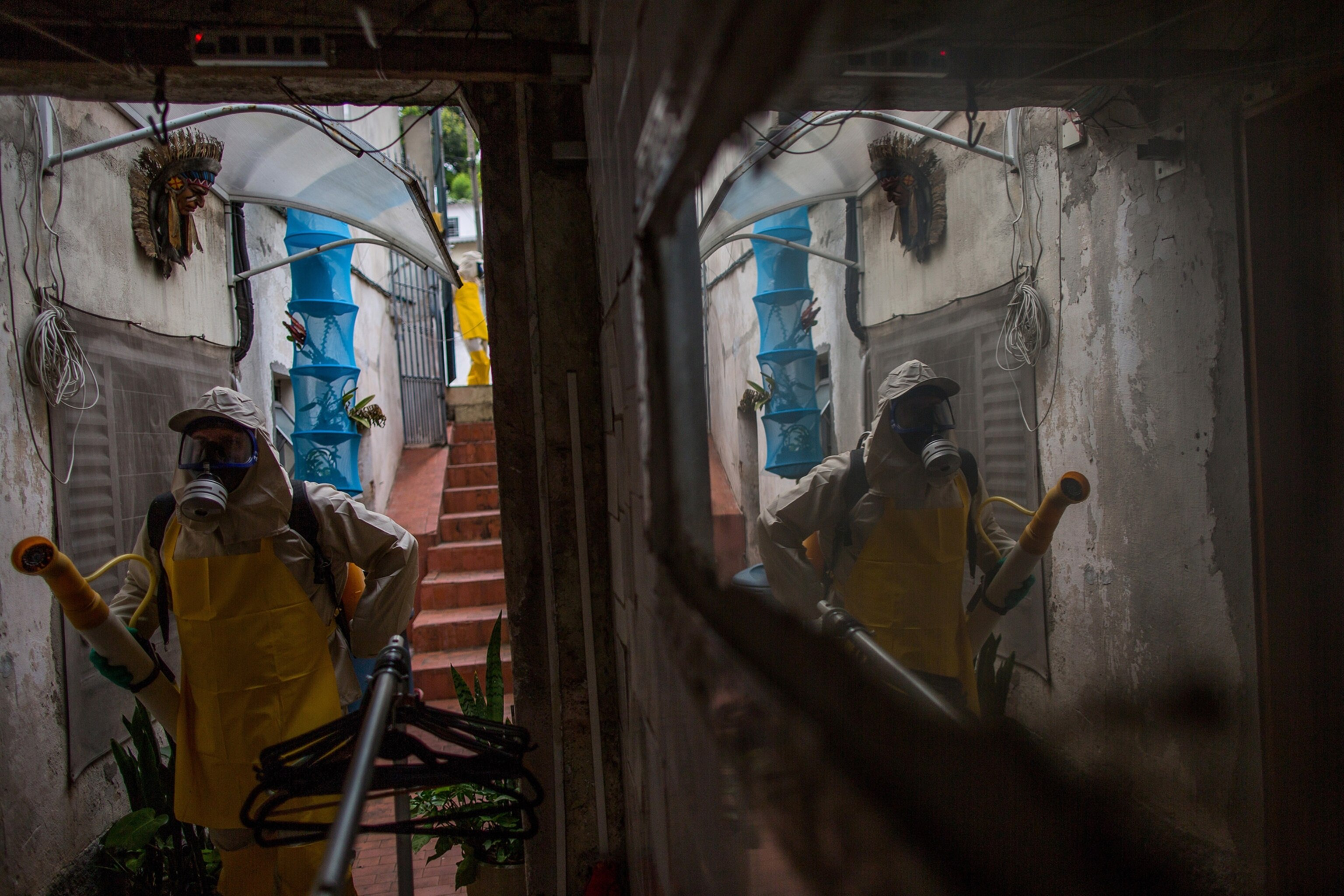
These mosquitoes may be sheltering somewhere like a metro tunnel or storm sewer, Severson says. This enterprising behavior could put them one step closer to dense northern populations. Aedes aegypti mosquitoes have been found this far north in summers before, but were likely imported by travelers, and none have become established year-round. Severson thinks it’s likely that other colonies are in the area but just haven’t been found yet.
Disease outbreaks hitchhiking in the innards of mosquitoes, like the Zika virus currently racing across South and Central America, are likely to become increasingly frequent and far-reaching, public health experts say. Climate change, along with growing urbanization and the rise of international shipping and travel, will stretch the insects’ range and access to large human populations.
“Looking forward, climate change is a clear risk for burden of a variety of infectious diseases,” says Kristie Ebi, an epidemiologist at the University of Washington’s Department of Global Health, who studies the disease impacts of climate change. “The question is, will public health agencies be up to handling the risk?” she asks. “And the second part is, will those efforts be sustained?”
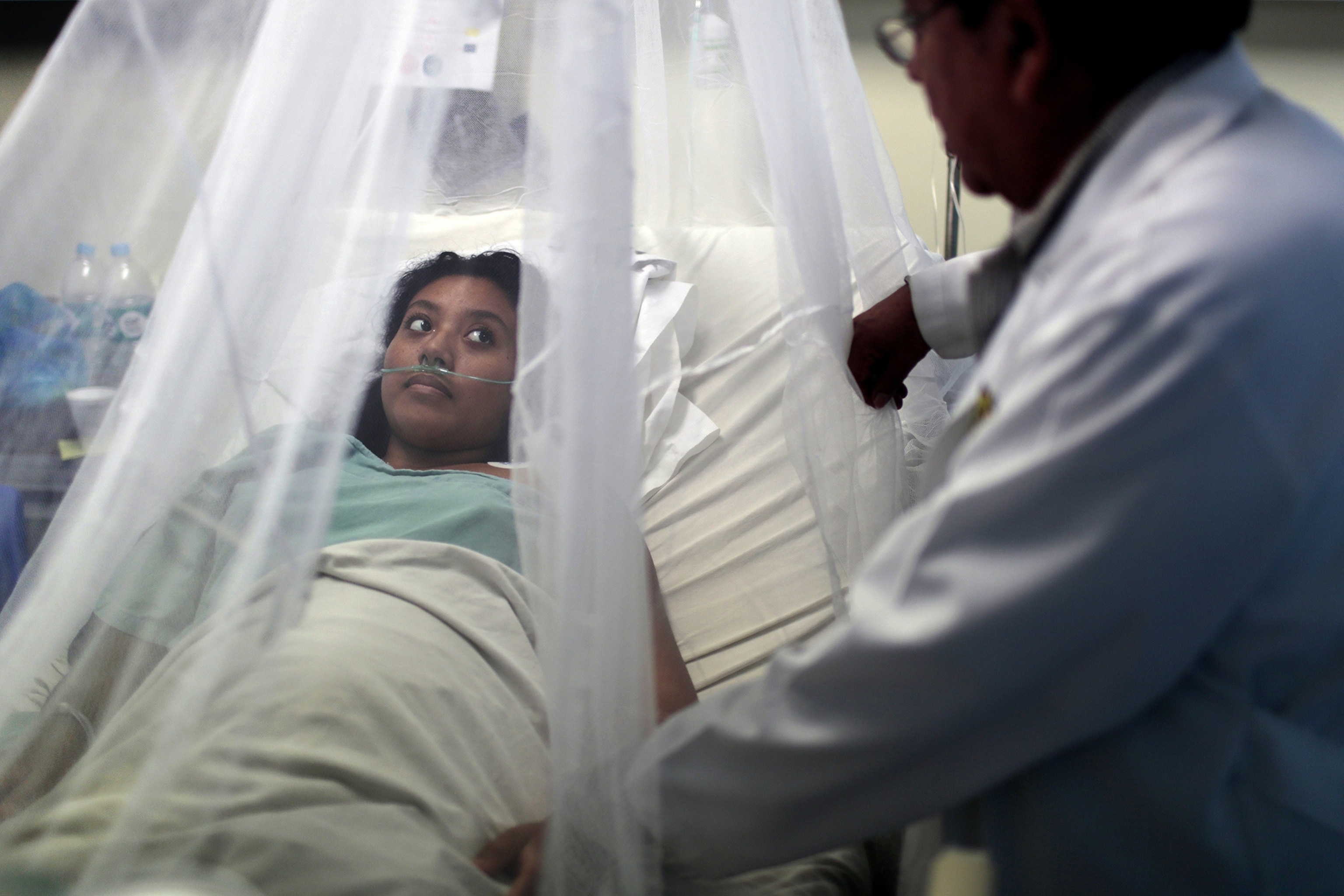
Climate models predict many parts of the planet will become hotter and wetter due to the buildup of greenhouse gases in the atmosphere, and these conditions are ideal for increasing the range of viruses and the insects that transport them. Precise forecasts are difficult because of the multiple factors that enable mosquitoes to spread. But scientists expect mosquitoes like the ones transmitting Zika to move farther north and south as the climate warms.
Zika, which the World Health Organization on Thursday announced was “spreading explosively” in the Americas, is now being actively transmitted in at least 20 nations between Mexico and Brazil, and is projected to reach as far north as Texas and Florida. As many as 4 million could become infected this year. Disease experts are worried that college students on spring break next month will bring the virus back from the Caribbean and Mexico. And the summer Olympics in Brazil are on everyone’s mind.
Although the disease is mild in most cases, Zika is suspected in a spate of microcephaly, a rare and disabling condition in which babies are born with abnormally small heads. Health officials for Brazil, the outbreak’s epicenter, say the number of new microcephaly cases there has topped 4,000 since October—many times more than the annual average. The virus also may be linked to Guillain-Barré syndrome, which attacks the nervous system and can cause paralysis.

The Zika eruption caught the world unprepared. Public health officials are now struggling to cope with the sudden virulence of a virus that had been fairly docile, while researchers test new ways to control mosquitoes and try to develop a human vaccine.
But Zika is only one of many rising insect-borne disease threats, scientists say.
Dengue, which can cause internal bleeding and circulatory failure, infects as many as 400 million people worldwide every year, according to the U.S. Centers for Disease Control and Prevention. Chikungunya, which can lead to chronic joint pain, infected around 1 million people in the Americas alone last year. Both viruses are carried by the same A. aegypti spreading Zika, and both are also poised to take off as the mosquito’s range spreads.
“Aegypti is really adapted to living with people in an urban environment,” Severson says. “They can breed in just about any container that holds water…They can use pop cans or any kind of trash lying around.”
What’s more, dengue and chikungunya viruses can also replicate inside A. albopictus, the Asian tiger mosquito, a hardier species that’s rapidly staking out new territory in the United States and Europe.
“Dengue is still by far the most important of the human pathogens…Half of the world is at risk,” says Scott Weaver, director of the Institute for Human Infections and Immunity at the University of Texas Medical Branch in Galveston. “Even though Zika is in the news, just to keep it in perspective, dengue is still the big player.”
Behind dengue, Weaver says, are mosquito-borne menaces like Japanese encephalitis, which infects tens of thousands in Asia every year; West Nile, which has sparked several recent flare-ups throughout the U.S.; and yellow fever, which still sickens around 200,000 people in Africa and South America every year even though a vaccine is available. “New World” viruses like mayaro, which is similar to chikungunya but so far has stayed mainly in South America, and Everglades virus, now contained to South Florida, could be just a couple mutations away from becoming more infectious.
And limited surveillance efforts mean other emerging diseases may be going undetected.

“Probably there are other pathogenic viruses, bacteria, maybe parasites out there that we either don’t have a diagnostic test for,” says Weaver, “or maybe we don’t even know they exist.”
The world needs to prepare for multiple new insect-borne disease threats emerging in new ecological niches, National Institute of Allergy and Infectious Diseases director Anthony Fauci wrote in a recent New England Journal of Medicine perspective.
“One has to be very concerned,” says Stephen Higgs, president of the American Society of Tropical Hygiene, and director of the Biosecurity Research Institute at Kansas State University. “The impact on human health just can’t be overestimated at the moment.”
Researchers are working on a number of new weapons for combatting insect-borne disease. One potential is a common bacterium, wolbachia. Mosquitoes infected with it in laboratory studies are unable to transmit dengue, chikungunya, and yellow fever. Wolbachia-infected mosquitoes are being introduced in Medellin, Colombia, part of a project aimed at eliminating dengue. Matthew Aliota, a research scientist at the University of Wisconsin, Madison School of Veterinary Medicine, will be studying the method’s prospect for controlling Zika and other mosquito-borne diseases.
“It’s certainly promising,” Aliota says. “But like with most of this stuff, there are so many questions that remain.”
A Zika vaccine is also being developed, but is likely many months away. And a British company is planning to release genetically modified mosquitoes with a trait causing offspring to die before they can mate, in hopes of sterilizing native mosquitoes.
But it doesn’t take a magic bullet to protect people from insect-borne diseases, Ebi says. Cleaning up places where mosquitoes can breed and draining puddles can go a long way toward keeping the numbers down.
“We’ve got the tools out there to make sure that we control the habitat for a variety of vectors,” Ebi says. “Sure we could use better tools, but we can do it.”