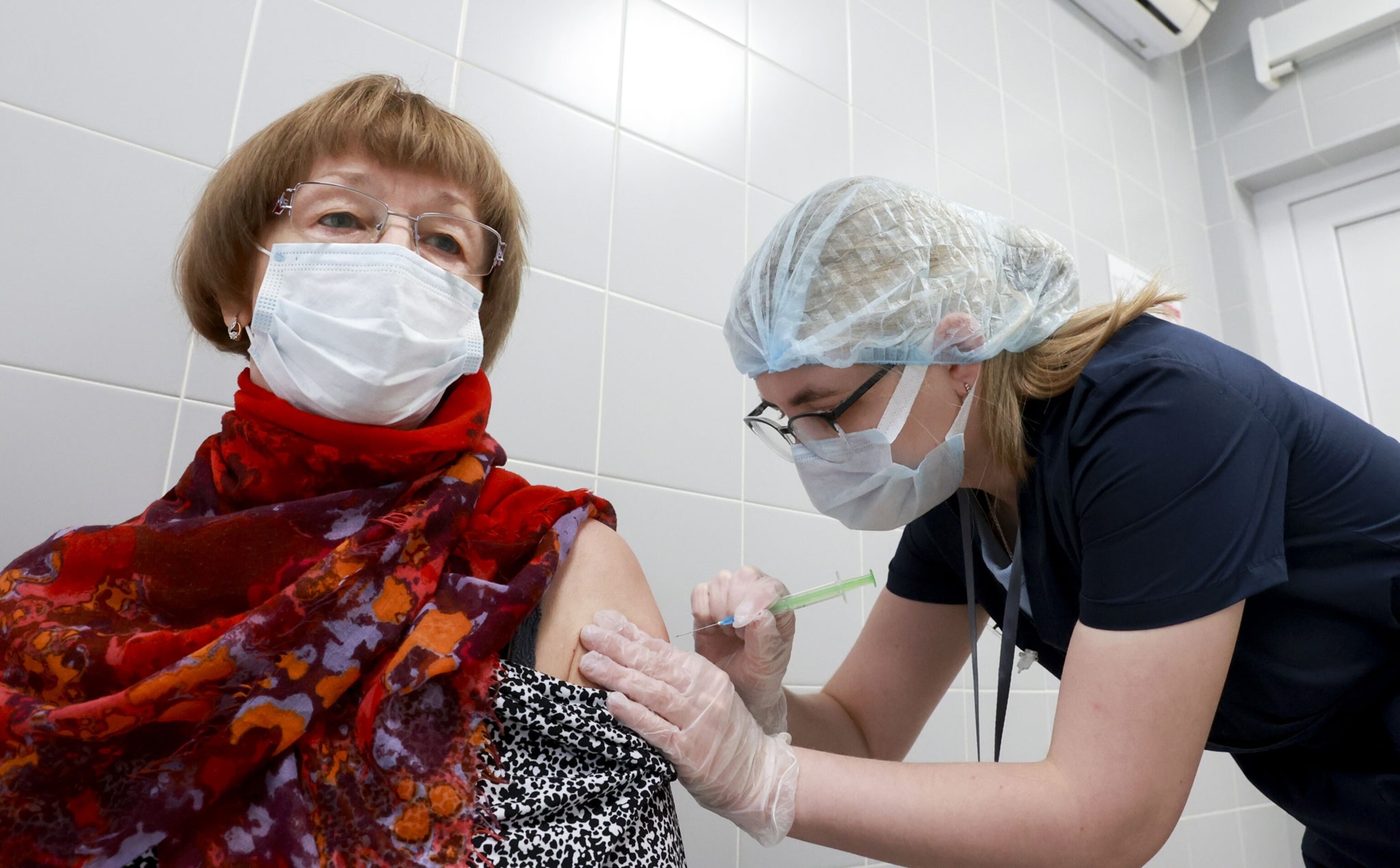
Is a 'twindemic' of flu and COVID-19 about to hit the U.S.?
Experts warn that the U.S. is ripe for a severe influenza outbreak in the coming months, making vaccination against both diseases more important than ever.
As cooler autumn days arrive in the U.S., experts are once again warning that the ongoing COVID-19 pandemic is about to collide with cold and flu season. And this year, the flu season may be worse than average in part because last year’s was shockingly mild.
Experts believe that a combination of social distancing, wearing masks, travel restrictions, hand washing, remote work, and shuttered schools played key roles in dramatically reducing the number of flu cases during the 2020-21 season. Last year there were only a little over 2,000 lab-confirmed cases in the U.S., compared to the 200,000 that occur during a typical flu season. Flu-related hospitalizations in 2020-21 were also the lowest ever recorded.
One influenza strain even seems to have died out during COVID-19’s deadly winter surge. However, scientists remain puzzled at the mild outbreaks in other countries that didn’t implement strict lockdowns and follow mitigation rules.
“Essentially, there was no flu anywhere,” says Richard Webby, director of the World Health Organization Collaborating Center for Studies on the Ecology of Influenza in Animals and Birds. “It suggests that all of these activities reduced circulation and affected the way flu travels even in countries that did nothing to mitigate COVID. But we still don’t know the entire story.”
So far, the evidence is mixed regarding the likelihood of a “twindemic” of COVID-19 and influenza this year, but predictions suggest the situation could be severe. And with many businesses, restaurants, schools, and other public places opening back up, fewer people are embracing social distancing and masks. In addition, last year’s mild flu season is complicating the annual task of deciding which strains to include in this year’s flu shot.
Scott Gottlieb, former head of the Food and Drug Administration, has warned that the confluence of the two respiratory diseases could overwhelm hospitals’ critical care capacity—which is already stretched thin in many regions of the country. According to estimates from the Centers for Disease Control and Prevention, an especially severe flu season could send more than 700,000 people to the hospital and claim as many as 52,000 lives.
“It’s a little mysterious as to what’s going to happen,” says Monica Gandhi, an infectious disease specialist at the University of California, San Francisco. “We don’t have influenza immunity from last year and we’re going to be mingling more. We need to be prepared for both [viruses] coming up at once.”
Gauging the next flu season
To get a preview of the upcoming flu season for the U.S., experts look at cases in the Southern Hemisphere that occur from May to October—the winter months in New Zealand, Australia, and parts of Asia. “So far, they’ve had another historically light flu season,” says Webby.
Flu activity in the U.S. is also currently low, according to the CDC, although it’s still early in the season. And unfortunately, a combination of other factors suggest that influenza may yet come roaring back.
For starters, cases of other illnesses such as respiratory syncytial virus (RSV) have been edging back up, which indicates more respiratory germs are in circulation. Plus, last year’s mild flu season left the population with less natural immunity—the part of our immune system that remembers foreign invaders and activates our defenses when their presence is detected once again.
What’s more, fewer people are social distancing or wearing masks, some Americans are still flu vaccine holdouts, and kids are back in school, all of which boosts the chances of a severe influenza outbreak.
“School-age children are the engines of influenza transmission in the community,” says Hana El Sahly, a virologist and infectious disease specialist at the Baylor College of Medicine in Houston. “And the social and behavioral changes that mitigated the spread of COVID are not in full force this season.”
The results of a pair of University of Pittsburgh mathematical studies, which were published online in August, paint an especially alarming picture. Researchers analyzed factors that included lower natural immunity to influenza and more social mixing in work, school, and social gatherings, then they calculated the possible outcomes when the influenza strain was either highly transmissible or a completely new strain.
One analysis found that the 2021-22 flu season could have around 20 percent more flu cases than normal. Depending on how contagious or unusual the flu strains were, those numbers could climb as high as double the typical caseload, which varies between nine and 45 million cases per year in the U.S.
Using a slightly different methodology, the other mathematical model suggested the incoming flu season could be responsible for 600,000 hospitalizations, which is at least 100,000 more than an average season. That number could spike as high as 400,000 additional hospitalizations if vaccination rates are low.
“Both studies said pretty much the same thing: The potential for a really large outbreak this year is high,” says Mark Roberts, director of the Public Health Dynamics Laboratory at Pitt Public Health and senior author on both studies.
“The way to combat that is to maintain social distancing and vaccinating, which decreases the possibility of an epidemic this year,” he says. The predictions are especially troubling for regions that are still experiencing COVID-19 surges because of resistance to preventive measures and vaccinations.
“It could be extremely variable across the country with pockets of outbreaks,” Roberts says. “Places that are not being careful about COVID could have a profound pandemic of influenza and COVID.”
Finding the right strains
With worries about such a severe season looming, Roberts and other experts urge more people in the U.S. to get vaccinated against the flu this year.
Typically flu shots are quadrivalent, which means they contain four inactivated strains from the main influenza virus families. That includes strains of H1N1 and H3N2—two sub-types that are part of the influenza-A family—as well as B/Victoria and B/Yamagata, which are the two “lineages” belonging to the influenza-B family.
Surveillance centers around the world monitor which flu viruses are circulating by looking at the genetics of samples from reported cases. This information is then used to select the most likely strains to include in the following year’s shot.
Sometimes scientists make the wrong choice, which is what happened in the 2017-18 flu season; that flu shot didn’t protect three-quarters of vaccinated people in the U.S. against the H3N2 strain that ended up being dominant. And because there were so few infections last year, only a fraction of the samples were gathered, making it harder to identify which strains will be making the most mischief this season.
The current shot contains two updates from last year’s version, and experts are hopeful they’ve chosen the right players. And in a potentially positive twist, the monitoring revealed that one branch of B viruses belonging to the Yamagata lineage seems to have died out during the 2020-21 season.
“It’s possible we haven’t looked carefully enough and it’s lurking somewhere,” says Peter Palese, chair of the microbiology department at the Icahn School of Medicine at Mount Sinai in New York. “But it would be extraordinary if that branch died out, because we’d be back to a trivalent vaccine that’s cheaper to make.”
It’s not yet clear why a particular virus would become extinct, but experts have some hypotheses.
“We have four influenza viral types, and usually only one dominates at any one time,” says Webby, who’s also a virologist at St. Jude Children’s Research Hospital in Memphis. “Periods of low flow activity, when we’re wearing masks and social distancing, make it harder for viruses to find another host to infect, so they may die out.”
Mixing shots
The other good news on the prevention front is that you can safely get a dose of the COVID-19 vaccine at the same time as your flu shot, according to the results of a British clinical trial published online in the Lancet in September.
The study encompassed 679 people across Britain who had already received their first dose of a COVID-19 vaccine. When researchers administered the second dose, half the volunteers also received a flu shot while the other half got a placebo. Getting both vaccines at the same time didn’t increase the side effects, which were mild to moderate in both groups, and the vaccines didn’t lose their potency.
Even if it’s your first COVID-19 vaccination, experts don’t think it’s a problem getting both shots at the same time. And while COVID-19 vaccines are not yet authorized for kids under 12, toddlers as young as six months are eligible for the flu shot. Kids younger than two are especially vulnerable because they haven’t had any previous exposure to the influenza virus.
“Get the flu shot, and get your kids vaccinated,” says Gandhi of UCSF, “especially if they didn’t get the flu vaccine last year, because they’re at higher risk.”