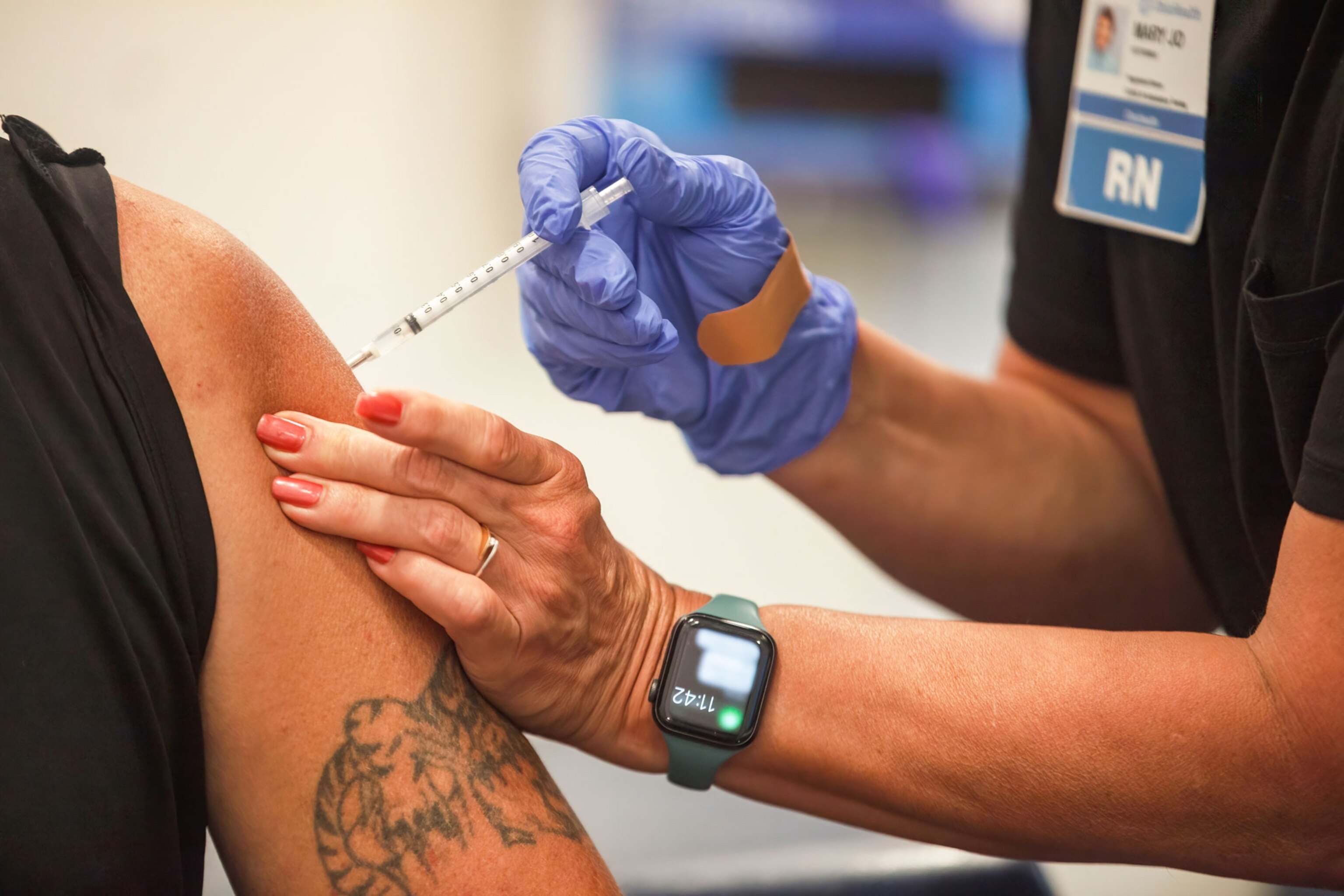
Vaccine mandates have worked in the past. Can they overcome modern hurdles?
The public health directives are older than the U.S. itself. But it's unclear whether they will be effective at driving up COVID-19 vaccination among the nation's 80 million resistant adults.
As vaccinations lag across the U.S. and COVID-19 cases continue to rise, new federal mandates will attempt to stymie the spread of the virus by requiring millions of workers to be vaccinated or face weekly testing.
President Joe Biden on September 9 announced the new mandates, which apply to workers at companies with more than 100 employees, federal workers and contractors, and health-care workers at institutions that receive federal funding. Together, the various orders affect about 100 million American workers.
These mandates, although sweeping, follow a precedent of U.S. vaccine directives that date to the days of the Revolutionary War. “Mandates are American, and resistance to them is American,” says Elena Conis, a historian of medicine at the University of California, Berkeley.
Some companies have already mandated COVID-19 vaccines—including Disney, Uber, Facebook, Google, Netflix and Delta Air Lines—and many celebrated those announcements, but the backlash against the new requirements has been thunderous: Several Republican governors declared them unconstitutional, and the Republican National Committee threatened to sue.
Experts say that this opposition, along with other hurdles, makes it tough to predict how much the mandates will contribute to slowing the spread of the virus, and ultimately, bringing the pandemic to an end.
While history is on the side of the vaccine mandates, “no one knows how effective this will be,” says Eric Toner, a senior scholar and emergency medicine expert with the Johns Hopkins Center for Health Security. “[But] I think more people will be vaccinated with these measures than would be vaccinated otherwise.”
The historical precedent for vaccine mandates
While some politicians have touted the new mandates as “un-American,” vaccine mandates are older than the United States itself. “General [George] Washington mandated smallpox inoculation—the precursor to the vaccine, and a more dangerous procedure—for the Revolutionary Army,” says Dorit Reiss, a law professor who specializes in vaccine policy at the University of California, Hastings College of the Law. “And I don't think it’s fair to describe Washington as un-American.”
In 1809, Massachusetts enacted a law that gave the state’s municipal boards of health the authority to require smallpox vaccinations for people older than 21. “Throughout the 19th century, individual employers would sometimes insist on proof of smallpox vaccination or infection before hiring someone who might work in their shop or home,” Conis says. That proof was usually just the bodily scar that remained on the arm or leg after vaccination.
The Supreme Court upheld the law when it was challenged, setting a precedent that such mandates are constitutional. In 1922, the court again backed vaccine mandates, supporting the authority of states to make them a condition of school attendance.
Today, armed services personnel face a long list of vaccine mandates, and health-care workers may be required to have certain vaccines—such as those for influenza, as well as measles, mumps, and rubella—as a condition of employment. But most vaccine mandates affect school children: All 50 states have vaccination requirements as a condition for admittance. (And some states, such as Mississippi and Maine, do not allow religious or philosophical exemptions.)
Vaccine mandates must work in two ways to be most effective, says Reiss: They must increase vaccination rates and prevent outbreaks. Multiple studies show that school mandates have increased childhood vaccination rates across all 50 states and tamped down the spread of preventable diseases.
In one example, measles outbreaks in 1976 and 1977 led Alaskan health officials to more strictly enforce the state’s measles, mumps, and rubella vaccine mandate. According to the Centers for Disease Control and Prevention, 7,418 of the state’s 89,109 students were unable to provide proof of vaccination on the day of the announced enforcement. They were forced to leave school. One month later, however, fewer than 51 students were still excluded, the CDC reported, and no further cases of measles occurred.
Hospitals with mandatory influenza vaccinations have achieved higher vaccination coverage than those that make it voluntary. And the agencies that mandated COVID-19 vaccines before Biden’s announcement have already seen some success: For example, the number of active-duty military personnel who are vaccinated increased from 76 percent to 83 percent in the weeks after the Pentagon issued its mandate.
The mandates still face hurdles
But the new mandates are not an instantaneous fix to the pandemic, nor are they guaranteed to work. The mandates will face legal challenges from Republicans and employers. It’s also unclear how many of the 100 million American workers affected by the mandates are already vaccinated, leaving some experts to question how many new inoculations will occur.
“Undoubtedly, [the vaccine mandates] are very effective tools if fully implemented and properly enforced, but that is fraught with challenges,” says Rossi Hassad, an epidemiologist at Mercy College in New York. “So, there will be many cracks in the system that unfortunately may prolong this pandemic.”
What’s more, getting a COVID-19 vaccine does not offer instantaneous protection; it takes time for immunity to build, and with the highly transmissible Delta variant now the dominant strain in the U.S., non-medical measures—like hand washing, mask wearing, and social distancing—will continue to be important tools to stop the spread of COVID-19, Hassad says.
And while an August AP-NORC poll showed that more than half of Americans support employer vaccine mandates, 87 percent of unvaccinated respondents to a later CNBC poll said they would not get a COVID-19 vaccine even if their employers required them to do so.
“Polls are really important to get a temperature” for how people are feeling and as guidance for policy efforts, says Angela Shen, vaccine policy expert and visiting research scientist at the Vaccine Education Center at Children’s Hospital of Philadelphia. But people don’t always stick with their decision not to get vaccinated when faced with the consequences of their choices, she adds.
“We know that while people don’t like mandates, when [people] comply, they’re highly effective,” Shen says.
In the case of the new mandates, the Biden administration will allow employees to opt out of shots by testing weekly for the virus. Because of that option, “what we’re calling a vaccine mandate is basically just a testing program with a vaccine exemption,” says Zoe McLaren, a professor of public policy at the University of Maryland, Baltimore County. Even that measure should help to curb the virus’ transmission by catching cases before they spread, she says.
Of course, some employees could choose to quit their jobs, changing companies or opting out of the labor force, rather than submit to regular COVID-19 testing. “There may be places that see something of a hiring crunch,” McLaren says, but adds that effect should be somewhat limited.
Prior to last week, if people didn’t want to get vaccinated, they could leave their jobs at companies that required them for ones at companies without a mandate.
But the Biden administration’s policy applies “across the board, nationally,” she says, “which means that it’s much harder for anybody who wants to avoid the mandate to find a job.”
The new mandates also leave out large segments of the population: Those who are retired or unemployed, homemakers, or those who work at companies with fewer than 100 employees.
But McLaren says that everyone still stands to benefit from the mandates, if they are effective: “Vaccination doesn’t only protect the person who gets vaccinated,” she says. “It protects everybody around them too. Even people who are unaffected by the mandates will benefit from the ripple effects of higher vaccination rates.”