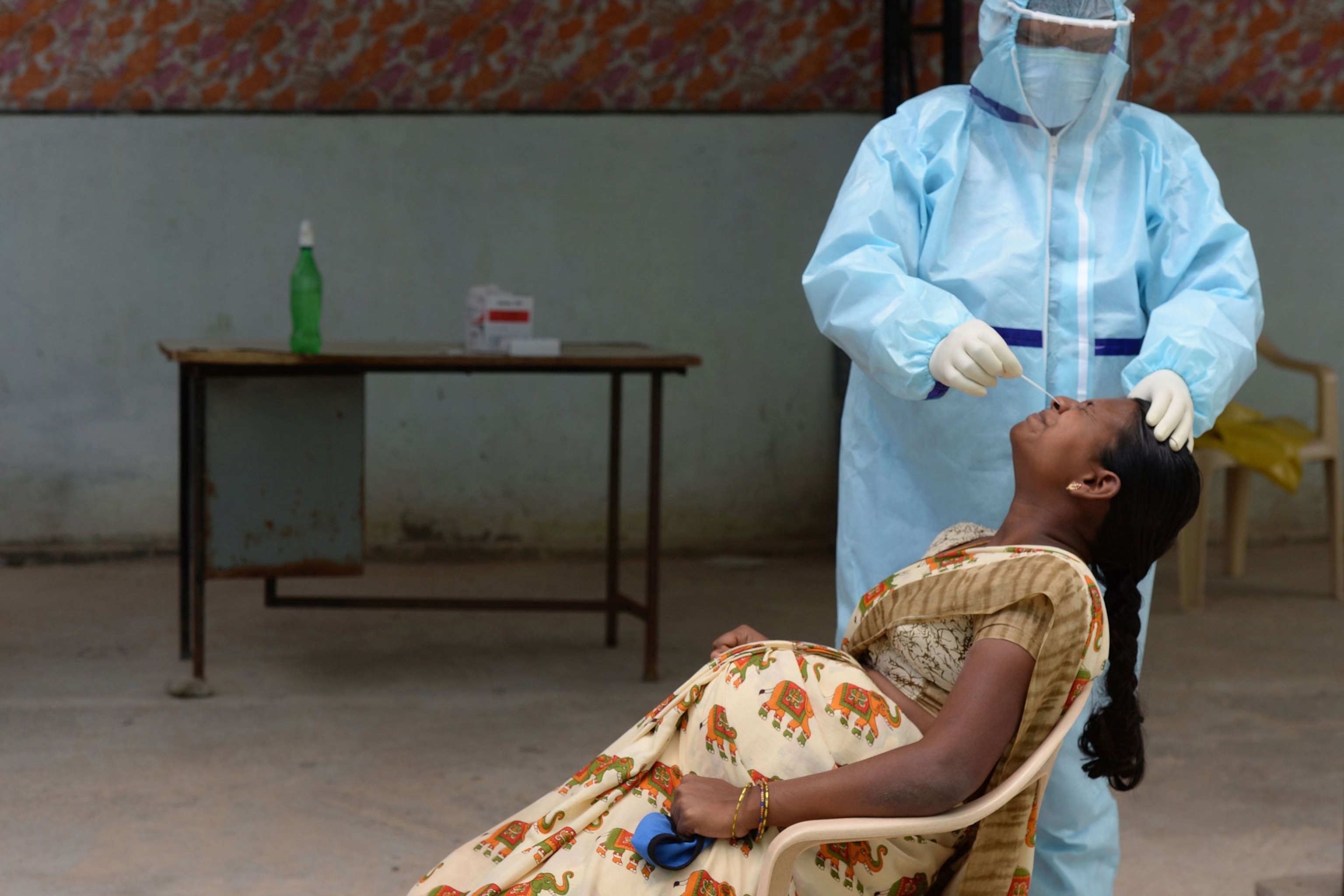
Why pregnant women in India still are not eligible for COVID-19 vaccines
Government concerns about safety mean expecting mothers can't get shots. But some doctors are raising alarms about pregnant women's increased risk of severe disease and death.
On June 21, most people in India 18 years and older became eligible to receive a COVID-19 vaccine for free—but that still doesn’t include women who are pregnant.
India’s second wave has caused one of the worst COVID-19 outbreaks in the world, with the virus killing more than 390,000 Indians to date, according to official estimates. While there’s no government data on how many pregnant women in the country have had COVID-19, anecdotal reports suggest the number is at least in the thousands, with the situation being far worse in rural areas due to poor testing and a lack of treatment. (See how COVID-19 is ravaging rural India.)
The government recently approved vaccines for lactating mothers. But in an official statement, Vinod Kumar Paul from the National Institute of Transforming India (NITI) Aayog, a government think tank, said officials couldn’t extend access to pregnant women because of the lack of available safety data. The government hopes to “clarify the situation in a few days based on new scientific inputs,” he added. (National Geographic reached out to Paul, who is also a spokesperson for India's COVID-19 task force, but he did not respond to requests for comment.)
Pregnant and lactating women were initially excluded from mass vaccination drives in most countries because they were not part of any clinical trials for COVID-19 vaccines. Since then, Pfizer and Moderna’s mRNA vaccines have been tested on pregnant animals and their babies and showed no additional health risks. A recent study published in the American Journal of Obstetrics & Gynecology showed similar results for pregnant and lactating women who received an mRNA vaccine. Based on these and other studies, the U.S., along with the United Kingdom and Belgium, have given pregnant women priority status for vaccination.
In India, however, there’s little safety data available for pregnant women receiving Covishield or Covaxin, two vaccines authorized for use in the nation. Still, many experts believe the benefits of vaccinating pregnant women and their babies likely outweigh the risks.
A report from the U. S. Centers for Disease Control and Prevention found that pregnant women infected with SARS-CoV-2, the virus that causes COVID-19, faced a 70 percent greater risk of dying compared to non-pregnant women. They were also more likely to require hospitalization in the ICU, ventilation, and life support due to their weaker immune systems. These findings are backed by a recent study published in JAMA Pediatrics, which surveyed 2,100 pregnant women across 18 countries, including India, and found that both pregnant women and newborns faced a higher risk of dying if mothers caught the virus while pregnant.
With less than 5 percent of India’s adult population fully vaccinated, experts argue that vaccinating pregnant women should be a priority to contain the number and severity of such cases. The Indian federation of gynecologists, also known as FOGSI, publicly urged the Indian government to change its COVID-19 vaccine policy. It argued women should consult with their physicians and have the power to decide if they want to get the jab.
“From a public health perspective, we know it’s needed,” says Neerja Bhatla, head of the gynecology ward at A.I.I.M.S. Hospital in Delhi, India’s premier research hospital. “We are just hoping it happens soon as we don’t want the same dilemma in case there’s a third wave.”
Anxiety and loss
Early this year, 26-year-old Priyanka Chand and her husband Jayasurjya Bhanja asked their gynecologist if she could get the jab. Although India’s vaccination drive wasn’t open to all adults, Chand was pregnant and wanted to stay clear of the virus. “We wanted to be safe,” Bhanja says. “But the doctor told us it wasn’t allowed.”
Chand tested positive for COVID-19 in late April, during her sixth month of pregnancy. She had barely left the house, but after experiencing headaches and a bout of fever, she tested positive for the virus. When her oxygen saturation levels plunged to 30 percent, her gynecologist urged her to go to a hospital immediately.
But this timing coincided with the beginning of India’s second wave, and for three days the couple struggled to find a vacant hospital bed. At 1 a.m. local time on April 28, Chand was finally admitted to Max Super Specialty Hospital in South Delhi. By then, her condition was critical and she was put on a ventilator to help her breathe. She survived after ICU treatment—but she lost the baby. As Chand now recovers at home, still on oxygen support and steroids, the couple wonders if a vaccine could have prevented this tragedy.
“Who knows, maybe our baby might have survived,” says Bhanja. Their harrowing experience has made one thing clear, he adds: “Pregnant women are very vulnerable, we really need to focus on how to strengthen their immunity.”
At A.I.I.M.S. Hospital in Delhi, head gynecologist Bhatla says she saw a clear spike in cases of pregnant women with COVID-19 experiencing premature labor or having stillbirths. There is no one reason why, says Bhatla. While immunity is generally compromised during pregnancy, the increased abdominal pressure can also compress the lungs and aggravate shortness of breath, a common symptom triggered by the new Delta variant of COVID-19 that has been sweeping through India. (This is why the Delta variant is so scary.)
Hema Divakar, a physician and former president of FOGSI, says that in her network, obstetricians and gynecologists have also seen “frightening numbers” of pregnant women dying. The physician believes many of the deaths could have been prevented, but patients were either too late in consulting their doctor, or doctors failed to recognize the COVID-19 symptoms.
“Because each case is so different, the treatment of pregnant women with COVID-19 cannot be standardized,” she says.
Medical system in crisis
The Indian Council of Medical Research does have a standard protocol for how to manage pregnant women during the pandemic: Potential or mild COVID-19 cases should be tested, isolated, and monitored at home, while those with more severe symptoms should be hospitalized. But in practice, within an overwhelmed healthcare system, most doctors are left to find their own solutions.
Many hospitals across the country refused to admit pregnant women because they either ran out of empty hospital beds or didn’t have the special facilities like maternity wards and neonatal ICUs to treat mother and child. Other hospitals weren’t designated for the treatment of COVID-19 patients. Local reports are filled with such stories: In Karnataka, one woman was discharged from the hospital after she tested positive for COVID-19 despite being in labor; in Kerala, another woman who recovered from COVID-19 was still turned away by private and government hospitals, and lost her unborn twins shortly afterward.
The lack of specialized prenatal care during the second wave has also impacted pregnant women who didn’t contract COVID-19. Many women have been unable to go for routine screenings and clinical check-ups due to lockdowns. As a result, “we have seen lots of cases develop anemia, preeclampsia, and other serious morbidities because of the delays,” Bhatla says.
Bhatla and Divakar are among many doctors who feel that vaccination will at least prevent or drastically reduce the number of COVID-19 cases and mortalities among pregnant women. In a yet-to-be published study led by Yamini Sarwal, the chief medical officer at New Delhi’s Safdarjung Hospital, evidence of the safety and efficacy of COVID-19 vaccines from studies worldwide revealed that many pregnant women responded well to whichever type of vaccine they received and produced a “robust immune response.” The report even recommends making vaccination part of routine antenatal protocols, given the fact that shots also protected the fetus through the transfer of antibodies.
But until the Indian vaccines are backed by data and approval for use on pregnant women, doctors are left feeling lost on how to best advise their patients: “It’s a dicey decision-making process,” said Divakar. She adds that all her patients want “utmost certainty” that the vaccine won’t harm them and their babies, something she cannot guarantee.
Nupur Kaushik, a 35-year-old mother who is currently six months pregnant with her second child, wants to get vaccinated, but she doesn't have confidence in Covishield, which uses a modified cold virus to deliver genetic material from SARS-CoV-2, or Covaxin, which uses an inactivated coronavirus to trigger a protective immune response. Kaushik feels that the government rushed approval of these vaccines.
“There’s just been so much politics with the vaccination drive here,” she says. In January, Covaxin’s approval was fast-tracked before it had gone through phase three trials, while Covishield had not completed local clinical trials in India before approval. Kaushik would rather wait to get the Pfizer or Moderna vaccines. “When it comes to my children, I want to take zero percent risk,” she says.
Until then, Kaushik will continue to isolate in her home in Noida, a satellite city 30 miles from the national capital of Delhi. She stays in a separate room from her husband, a lawyer who leaves the house every day for work, and her five-year-old son.
“We were so happy that I was pregnant again, but now I feel anxious and lonely all the time,” she says. “This virus has changed everything.”
When will pregnant women get their shots?
Although the government hopes to approve vaccines for pregnant women based on new information, doctors are skeptical this will happen soon. Collecting safety data will take time, since the Indian-administered vaccines are different from the ones approved for pregnant women overseas. In India, the authority to approve vaccine eligibility rests with the Ministry of Health and Family Welfare, which reviews the data collected by a national technical advisory group on immunization before granting permission for use.
There are ways to collect and review data on pregnant women more efficiently, Divakar says. Some pregnant women are willing to participate in clinical trials, while others may have had unintended pregnancies after taking their doses. So far, though, the advisory group has not adopted these suggestions, and its process for collecting data remains unclear.
In addition, prioritizing pregnant women will be difficult during the nation’s current vaccine shortages. In January, the government ordered just 15.5 million doses for its population of 1.4 billion. When cases shot up in March, it placed another order for 110 million doses, but vaccine makers in India struggled to keep up with the demand. Against this backdrop, lactating women are already struggling to get shots, and once pregnant women are approved, they will have to become the main priority for vaccination centers.
“It will be a nightmare for the government if those women are denied a dose,” Divakar says.