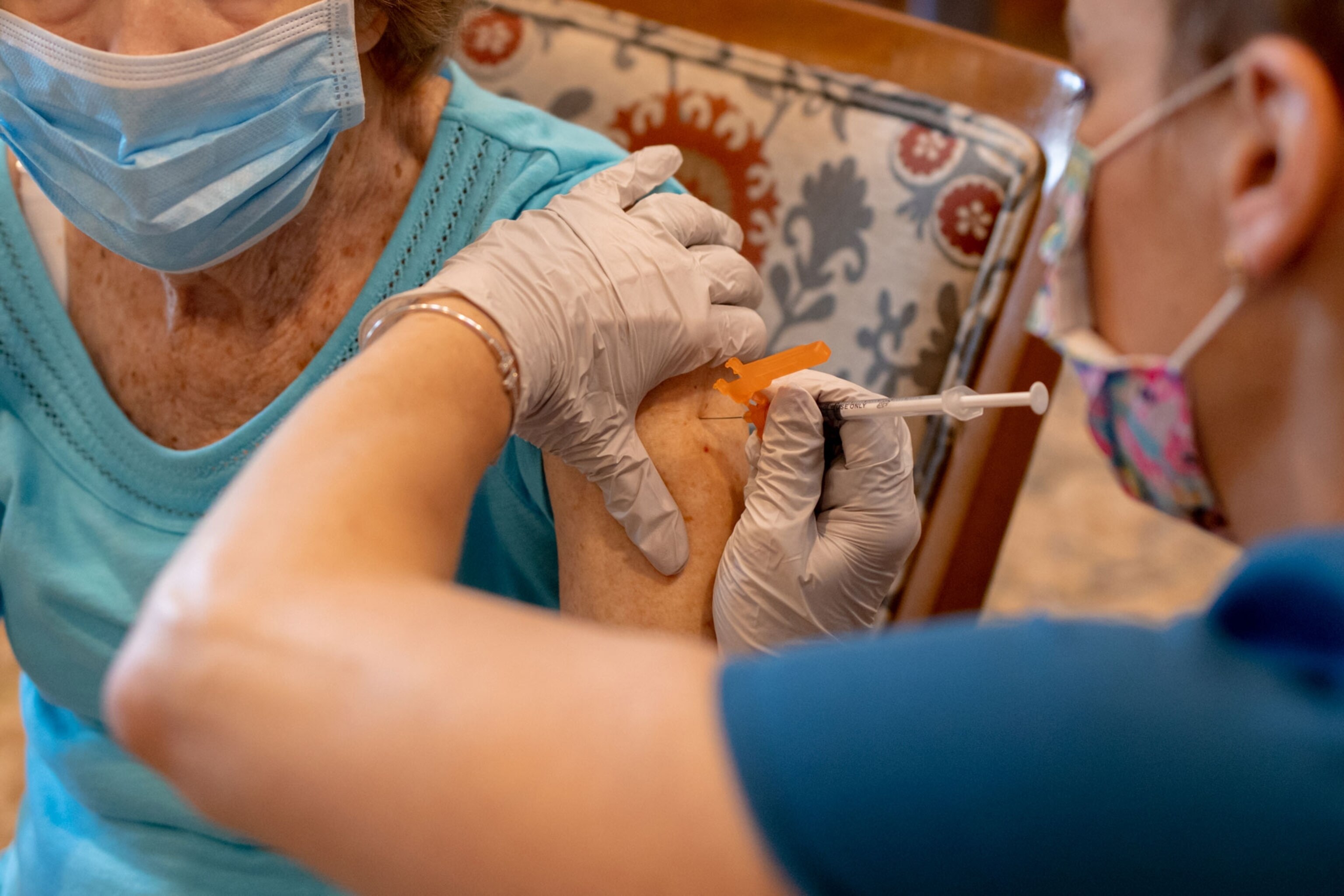
Why the CDC and FDA only approved booster shots for some Americans
Given what we know about breakthrough infections, most experts remain unconvinced there’s enough data to justify an extra dose for most Americans.
In a blow to President Joe Biden’s plan to begin rolling out COVID-19 booster shots this month, the U.S. Food and Drug Administration granted emergency use authorization of a third dose of the Pfizer vaccine only to certain subgroups of the national population. That includes people age 65 and older and people at risk of severe disease, such as adults with underlying conditions or in high-risk jobs. The Centers for Disease Control and Prevention later gave their ruling to start administering boosters to older adults, residents of long-term care facilities, and people ages 50 to 64 with conditions that leave them vulnerable to severe disease.
But in an unusual move that highlights how complicated the decision-making on boosters has been, CDC director Rochelle Walensky overruled her agency’s advisory panel and also endorsed extra doses for younger people whose jobs put them at high risk, such as health-care workers and teachers. Walensky otherwise agreed with the advisers’ recommendation that people ages 18 to 49 with underlying conditions should only receive a booster dose if their personal benefit outweighs the risks.
This is a far different plan for boosters than what was announced in August, when President Biden said that his administration planned to offer third doses of the Pfizer and Moderna vaccines to all eligible Americans. His team advised people to get the boosters eight months after their second doses, and they set a September target for clinics to start giving people third jabs. “It will make you safer, and for longer. And it will help us end the pandemic faster,” Biden said at the time.
The FDA departed from that plan because the evidence is much stronger that boosters will benefit people age 65 and older than it is for benefits to the general population, says Anna Durbin, a vaccine researcher at Johns Hopkins University.
“To their credit, they’re following the process that they always follow,” she says of the FDA ruling. “These decisions need to be based on data. It’s really important to maintain the integrity of the science.”
Conflicting data on breakthrough infections
The data trickling in so far does seem to suggest that the two-dose Pfizer-BioNTech vaccines are less able to prevent infection after six to eight months, but experts point out there are wide discrepancies.
In July, Israel said data from its highly vaccinated population shows that Pfizer’s vaccine is now only 64 percent effective against preventing infection. Then there were the alarming reports that month of a large COVID-19 outbreak in Cape Cod, Massachusetts. Out of hundreds who had been infected, about three-quarters were fully vaccinated. By contrast, a United Kingdom study in August found that the Pfizer vaccine is 88 percent effective against the Delta variant. Weeks later, a study of New York State residents showed a combined vaccine effectiveness of 79.8 percent among those who had received the Pfizer, Moderna, and Johnson & Johnson jabs.
One thing that’s perfectly clear to scientists is that the COVID-19 vaccines are still performing admirably where it matters most: protecting against severe disease and death.
In the aftermath of the Cape Cod outbreak, scientists pointed out that only four of the people who got breakthrough cases had to be hospitalized. And according to a September 10 report from the CDC, the vaccines are more than 90 percent effective against hospitalization and death. Unvaccinated people are 10 times more likely to be hospitalized than vaccinated people and 11 times more likely to die.
In interviews conducted before the FDA announced its decision, experts emphasized that the data will be much clearer if regulators can take more time before weighing the science behind booster shots, since breakthrough infections remain overwhelmingly mild in the general population.
“Your protection does not fall off a cliff at six months or eight months,” Durbin said at the time.
Protection against severe disease
To understand why breakthrough infections happen, it helps to recall how the immune response works. Antibodies are the first line of defense against infection, and people can develop antibodies that target the SARS-CoV-2 virus both through natural infection and vaccination. When the virus enters the body through the nose or throat, the antibodies that reside there fight off the virus before it can take hold.
But your body can’t maintain high levels of antibodies against every pathogen it has ever encountered all the time. People also tend to have relatively low levels of antibodies in their noses and throats because they have to travel there from your bloodstream. So sometimes a virus—particularly one as potent as the Delta variant—can slip past them to cause a breakthrough infection.
As the virus penetrates the cells in the nose and throat, it begins to replicate. At that point, a person may exhibit symptoms characteristic of an upper respiratory infection, including stuffiness, cough, fever, and fatigue.
“It’s a nuisance but it’s not life-threatening,” says Deepta Bhattacharya, an immunobiologist at the University of Arizona College of Medicine.
That’s when the rest of the immune system kicks in to keep the infection from escalating to the lungs, where it can cause severe harm resulting in hospitalization or death. Having been trained by the COVID-19 vaccines to recognize the virus, the immune system ramps up production of new antibodies, as well as memory B and T cells that join the fight.
It takes time for an infection to travel to the lungs, giving your immune system plenty of opportunity to mount a robust defense. Bhattacharya says severe disease is low among the vaccinated because they can clear the virus from their systems more quickly. This both reduces the severity of their symptoms and reduces the window in which they can infect others. “I think we’re fairly confident in that,” he says.
Assessing the evidence
Booster shots are additional doses of the original vaccine that increase antibodies in the nose and throat, so they would decrease the chance of getting an infection in the first place. And researchers say that the data on breakthroughs is an early signal that the vaccines’ ability to prevent infection is waning, particularly among people with compromised immune systems and older populations.
These are groups that you would expect might not have a robust response to the standard dose of the vaccine, says Jack O’Horo, an infectious disease specialist at the Mayo Clinic who is based in Rochester, Minnesota. People who have had solid organ transplants, for example, take medication that suppresses the response of their memory cells. They rely on antibodies alone to fight off infection—and studies have shown that they have a poor antibody response to the vaccine.
In August, this evidence prompted the FDA to approve use of a booster dose for certain immunocompromised populations. “To the extent that a third shot gets them a little bit closer to what we see in healthy people after their second shot, I think that’s worth doing,” Bhattacharya says. “That’s the easy one.”
The next group that scientists suggested might benefit from booster shots were older Americans. According to a September CDC study, people over 65 account for about 70 percent of hospitalizations from breakthrough infections. But scientists note that there may be specific age groups or other factors in play, such as whether someone lives in a nursing home. Still, the FDA agreed that there’s enough evidence to suggest that people over 65 should be eligible for boosters.
It’s a little trickier to parse the data for other populations. Recently, a September 7 preprint echoed the findings of previous studies when it showed that the odds of vaccinated people testing positive for COVID-19 are higher 120 days after the date they reached full vaccination. Yet O’Horo, co-author of the study, stresses that “this was from a very small risk to a small risk.” He says follow-up research is needed to break down the populations whose risk of a breakthrough infection—while still small—is most concerning.
Ultimately, O’Horo says the findings of his study provide “a very early signal” to federal regulators that it’s time to carefully assess how the vaccines are working. He also points out that the FDA and CDC have access to more and better data than what has been released publicly about the vaccines’ real-world effectiveness.
“If I had to boil it down to a single phrase, it would be, Walk, don’t run,” he says. “We have information suggesting that this is a good time to have a scientific discussion about boosters, but it is emphatically not a time to hit a panic button.”
Complicating factors
There are other factors to consider when it comes to administering booster shots to the general population. For one, the three vaccines approved or authorized for use in the U.S. aren’t all the same.
Recent studies suggest that people who received Moderna’s vaccine are better protected from severe breakthrough infections because it elicits higher and more durable antibody levels than Pfizer’s vaccine. And a recent CDC report showed that the Moderna two-dose shot remains 95 percent effective in preventing hospitalizations compared to 80 percent for Pfizer and 60 percent for Johnson & Johnson.
But it will take more in-depth investigation to tease out what that means for who needs booster shots: Scientists point out that the Moderna vaccine is administered at a higher dose than Pfizer’s vaccine and with a longer interval between doses. It also rolled out after Pfizer’s vaccine, so the data are slightly lagging.
“People shouldn’t be running out and saying, I want a Moderna vaccine now,” Durbin says, adding that Moderna’s effectiveness is likely to drop off over time as well.
It’s also possible that another dose might not be a booster at all, but rather the proper dosage. Vaccines typically take years to develop because researchers take time to study many different dosing options. For the COVID-19 vaccines, they didn’t have that luxury of time to test whether three full doses might be better than two, says Francesca Torriani, an infectious disease specialist at University of California, San Diego Health.
And that could end up being the case. Anthony Fauci, head of the National Institute of Allergy and Infectious Diseases, said in an earlier White House press briefing that he “would not at all be surprised that the adequate full regimen for vaccination will likely be three doses.”
The bottom line for boosters
Ultimately, the decision on boosters came down to what regulators are trying to achieve: to reduce all symptomatic infections among Americans, or to slow transmission of the virus. Bhattacharya says there just isn’t evidence yet to show that a booster would provide much extra protection to most people.
He points to the discrepancies among global studies of vaccine effectiveness. Most show only a slight drop, but a handful of countries see a more significant change. The Biden administration has cited Israel’s reports that the Pfizer vaccine is now only 64 percent effective in its plan to roll out boosters. If that’s true, Bhattacharya says, it suggests boosters would offer a large benefit to the general population. But he cautions against putting too much weight in any one study.
“Most scientists believe that both in the short term and in the long term we have so much more to gain by getting the rest of the world vaccinated,” Bhattacharya says. He argues that the pockets of unvaccinated people around the world are far more dangerous than breakthroughs, because they create potential for even more dangerous variants that might evade the vaccines entirely.
Durbin agrees that global vaccine distribution should be the focus, and she adds that experts need to manage expectations about the purpose of vaccines.
“We are so privileged to be able to have these vaccines that are so highly effective,” she says. “Unfortunately, because of that people now think that they shouldn’t have any symptoms, there shouldn’t be breakthrough infections. And that’s just not a reasonable expectation,” she says.
Torriani points out that there might be an even easier and more effective way to prevent breakthrough infections in the U.S.: wearing a mask. Earlier this month, she was part of a team of researchers that examined breakthrough infections among health-care workers in San Diego. They noted that the drop in vaccine effectiveness from June to July was likely caused by waning immunity and the emergence of the Delta variant. Yet the study also coincided with the end of masking requirements in San Diego, which Torriani says likely increased the risk of breakthrough infections. It’s yet another factor that public health officials need to keep in mind when making policy.
“We still need to mask,” Durbin says. “It’s going to help prevent COVID, it’s going to help prevent you from getting influenza, it’s going to prevent you from getting other colds and respiratory illnesses. It just makes good sense. Wear a mask.”
Editor's note: This story originally published on September 16, 2021. It has been updated with details of the FDA's decision to grant emergency use authorization for some Americans and the subsequent ruling from the CDC refining who should receive boosters.