The World Health Organization on Wednesday declared the Ebola outbreak in the Democratic Republic of the Congo a public health emergency of international concern.
“It is time for the world to take notice and redouble our efforts,” said WHO Director-General Dr. Tedros Adhanom Ghebreyesus. “We need to work together in solidarity with the DRC to end this outbreak and build a better health system. Extraordinary work has been done for almost a year under the most difficult circumstances. We all owe it to these responders—coming from not just WHO but also government, partners and communities—to shoulder more of the burden.”

The declaration followed a meeting in Geneva of the international health regulations emergency committee for Ebola in the DRC. The committee, which has met four times since the outbreak was declared in August 2018, cited the first confirmed Ebola case in Goma, a city of nearly 2 million people near the Rwandan border.
The emergency committee expressed frustration with funding delays that have negatively impacted the Ebola response. They also stressed the importance of keeping transportation routes and borders open. Since it was declared almost a year ago the Ebola outbreak has been classified as a level 3 emergency, the most serious, by WHO. (See how new technology, treatment, and education aid the fight against the deadly disease.)
“It is important that the world follows these recommendations. It is also crucial that states do not use the PHEIC as an excuse to impose trade or travel restrictions, which would have a negative impact on the response and on the lives and livelihoods of people in the region,” said University of Zurich Professor Robert Steffen, chair of the Emergency Committee.



An Ebola epidemic thundering through heavily populated provinces in the northeastern Democratic Republic of the Congo has sickened 2,512 people and killed 1,676 since the outbreak was declared last August, according to WHO—despite the efforts of specialist medical teams, an effective vaccine, and new treatments that are being tested in the region.
The outbreak already is the second-largest on record, behind the epidemic that burned through West Africa from 2014 to 2016, killing more than 11,300 people. In its most extreme form, the viral hemorrhagic fever leads to uncontrollable bleeding and death.
In this outbreak, the virus appears to be infecting an unusually high number of children and killing a large percentage of people before they’ve sought or received treatment in Ebola centers staffed by local and international aid workers. Now, teams trying to track the spread of the disease are finding fresh cases with no obvious connection to previous patients, leading some health specialists to worry that the end of this epidemic is nowhere in sight.
Efforts to contain the virus also have been hindered by the path of the outbreak, which is spreading through areas marked by a deep distrust of foreigners, and therefore more hesitance to seek treatment. As well, ongoing political strife and violence are tearing through the region—including assaults aimed specifically at Ebola responders—and making it difficult for aid workers to corral the spread of the outbreak.
“I’m not at all optimistic that the epidemic will be brought under control in the near to medium term. All the data point in the direction of an extended epidemic,” says Lawrence Gostin of Georgetown University, director of the WHO Collaborating Center on Global Health Law. “With ongoing community distrust and explosive violence, and no concrete plan to overcome these obstacles, cases will increase with potential regional or global transmission.”


Any delay in treatment makes the virus more dangerous by giving it more chances to kill and spread, says Natalie Roberts, emergency operations coordinator for Médecins Sans Frontières (MSF), also known as Doctors Without Borders.
“You have a window of time in which treatment is effective. Wait too long, the patient dies anyway, and people lose confidence” in treatment, Roberts says. “Like any disease, the more severe it gets, the less likely any treatment is going to have an impact.”
Violence and viruses
The first embers of this outbreak began to smolder last summer, when cases started appearing in northeast Congo. This is the tenth time Ebola has emerged in the country, and as before, the virus crept out of a still-unidentified natural reservoir. Named after a river in Congo where it first appeared in 1976, the virus under a microscope resembles a kinked strand of spaghetti. It works its ways into cells, creates countless copies of itself, and destroys the connections between tissues, causing organ failure and leaky blood vessels, and essentially dismantling bodies from the inside out.
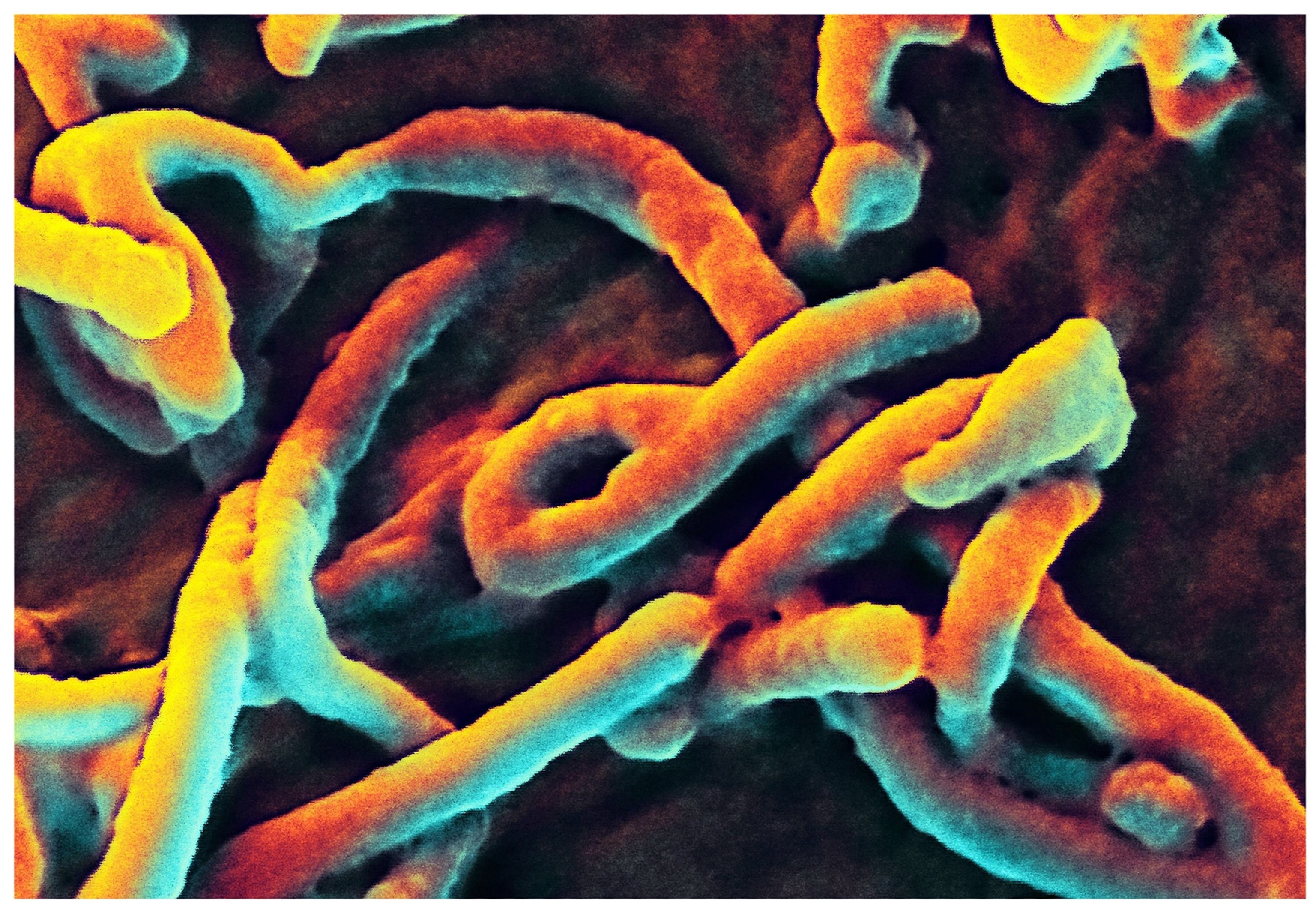
But transmitting Ebola is not exactly simple: The virus travels between humans through infected bodily fluids and tissues, but infiltrating a second host requires going in through broken skin or a mucous membrane, such as the eyes or nose.
“Ebola is not the most infectious disease in the world,” Roberts says. “It’s a very lethal disease, and it’s got a high mortality rate, but it’s not that infectious.”
Yet during the past 10 months, those first embers have ignited a viral fire. Because of the outbreak, the DRC delayed a presidential electionin three affected areas and agencies including MSF, the WHO and the U.S. Centers for Disease Control and Prevention (CDC) moved response teams into North Kivu and Ituri provinces.
Efforts to contain the epidemic have been stymied by local reluctance to seek or accept aid from foreigners, a partial reflection of the long-held mistrust of authority in a region torn by civil conflict. In some cities, residents even launched targeted attacks on Ebola diagnostic and treatment facilities, recently burning one MSF center largely to the ground, and prompting the temporary evacuation of various response teams. Now, aid workers are trickling back in.

“We have increased the footprint of CDC staff in-country over the past month,” says the CDC’s Inger Damon, co-lead of the Ebola response. “What we’re really trying to focus on, since we haven’t been able to get into some of the heavily affected areas, is working with teams on the ground to look carefully at the data that’s been collected and find the gaps where we can help to focus additional efforts.”
Vaccine shows promise


Health workers aren’t fighting the epidemic empty-handed. Besides four different treatments currently being field-tested, teams have a powerful weapon in their arsenal: the rVSV-ZEBOV vaccine, developed by Canadian scientists in the early 2000s and tested in Guinea in 2015. It’s made of an animal virus engineered to wear a non-lethal Ebola virus protein, which provokes the human immune system into mounting a pre-emptive defense.
Still officially unlicensed by the U.S. Food and Drug Administration, the vaccine is being donated by its manufacturer, Merck, and distributed under compassionate use protocols.
As of May 7, more than 111,000 people have been vaccinated. Most of those, according to the WHO, are primary or secondary contacts of Ebola patients—people such as health care providers or family members with a high likelihood of being infected. Those folks are identified through contact-tracing, a process used to track disease transmission and, ideally, halt its spread. The idea, Roberts says, is to create a ring of vaccinated individuals around a patient, and then create yet another ring around those primary contacts.
“You’re not necessarily protecting the contacts because they might have already contracted Ebola by the time you’ve confirmed the case,” she says. “But if you then vaccinate their contacts, you should be able to prevent them from getting Ebola – and therefore stop the epidemic.”
The WHO reports that so far, rVSV-ZEBOV-GP is proving highly effective, especially when administered early enough. No deaths have been reported among people who developed Ebola symptoms more than 10 days post-vaccination. As well, the overall fatality rate is lower among all vaccinated individuals, regardless of when they develop the disease.
So, with an extremely effective vaccine in hand, and more supplies on the way, why is the epidemic still out of control?
“The strategy looks fine on paper and theoretically we understand why it should work, but in practice we’re just questioning how feasible it is,” Roberts says. “We do have a good vaccine but it’s not managing to control the epidemic.”
Pinpointing the virus
Roberts and Damon both point to the same few reasons preventing the epidemic’s end.
For starters, people in the northeastern DRC are highly mobile and the region has hundreds of health care providers, ranging from private clinics to traditional healers to pharmacies. Many common diseases, such as measles or malaria, share initial symptoms with Ebola—meaning that identifying Ebola in its early stages is not necessarily easy. As of right now, the disease can be diagnosed only at specialized centers, which makes it tricky to quickly isolate patients and begin treatment.

“We’re seeing that many of the cases subsequently identified as Ebola cases will transit through one or two health care facilities prior to be identified,” Damon says.
Along the way, those patients come into contact with multiple caregivers and other patients—and then, by close contact with doctors, nurses and others, often unknowingly spread the virus. This type of disease transmission in health care facilities, termed nosocomial, is especially prevalent among children, Roberts says.
“They get admitted to a health facility with another medical problem and end up sharing a bed or may even equipment,” she says. “There’s actually more children getting sick with Ebola than we’d expect.”
By the time Ebola has been diagnosed, it’s sometimes too late for treatment to help. Perhaps most alarmingly, Damon reports that lots of people are dying at home rather than in Ebola treatment centers, suggesting that they aren’t seeking or accepting treatment early enough, if at all. These community deaths make it even harder to isolate cases, trace contacts, and effectively deploy vaccines.
“Over the past couple of weeks, it has been very disheartening that over 30 percent of the cases have been identified as deaths in the community,” Damon says. “There’s a longer period of time when there’s potential additional transmission to others who cared for these individuals before their death.”
New strategies
Quelling the rising numbers of Ebola victims will require some shifts in how teams work in the region.
Damon says that paying more attention to how teams interact with communities is crucial, and that CDC behavioral scientists are studying how information can be shared most effectively with local communities. The goal, she says, is to promote understanding and trust.
“It’s difficult to understand who can be the most effective messengers and identify them and train them, and have them better understand the disease and response effort,” she says.
In areas of the DRC where response efforts have successfully meshed with existing community structures and expectations, “we have seen outbreaks end,” says Tarik Jasarevic, WHO spokesperson. WHO teams work daily to engage communities in the disease response, gathering information about concerns, criticisms, beliefs and observations, and working to gain access to hostile areas. As a result, Jasarevic says, the vast majority of people eligible for vaccinations accept the vaccine, and a large percentage of families are conducting safe and dignified burials in areas where funerals are normally hotspots for disease transmission.
But Roberts points to another, perhaps more systemic factor that could be changed: the centralized Ebola facilities. She suspects that if it were possible for local health care providers to diagnose Ebola, outcomes would be better. Patients would receive treatment more quickly, they wouldn’t need to travel as far, and teams could vaccinate contacts before the disease spreads further.
“I really think if we could test people closer to home, then that would change an awful lot,” she says. “We could deploy the vaccine in a more simple manner. We could get much more quickly on top of the epidemic…. Right now, we can’t follow the chains of transmission, we don’t really know where the next case is going to appear.”