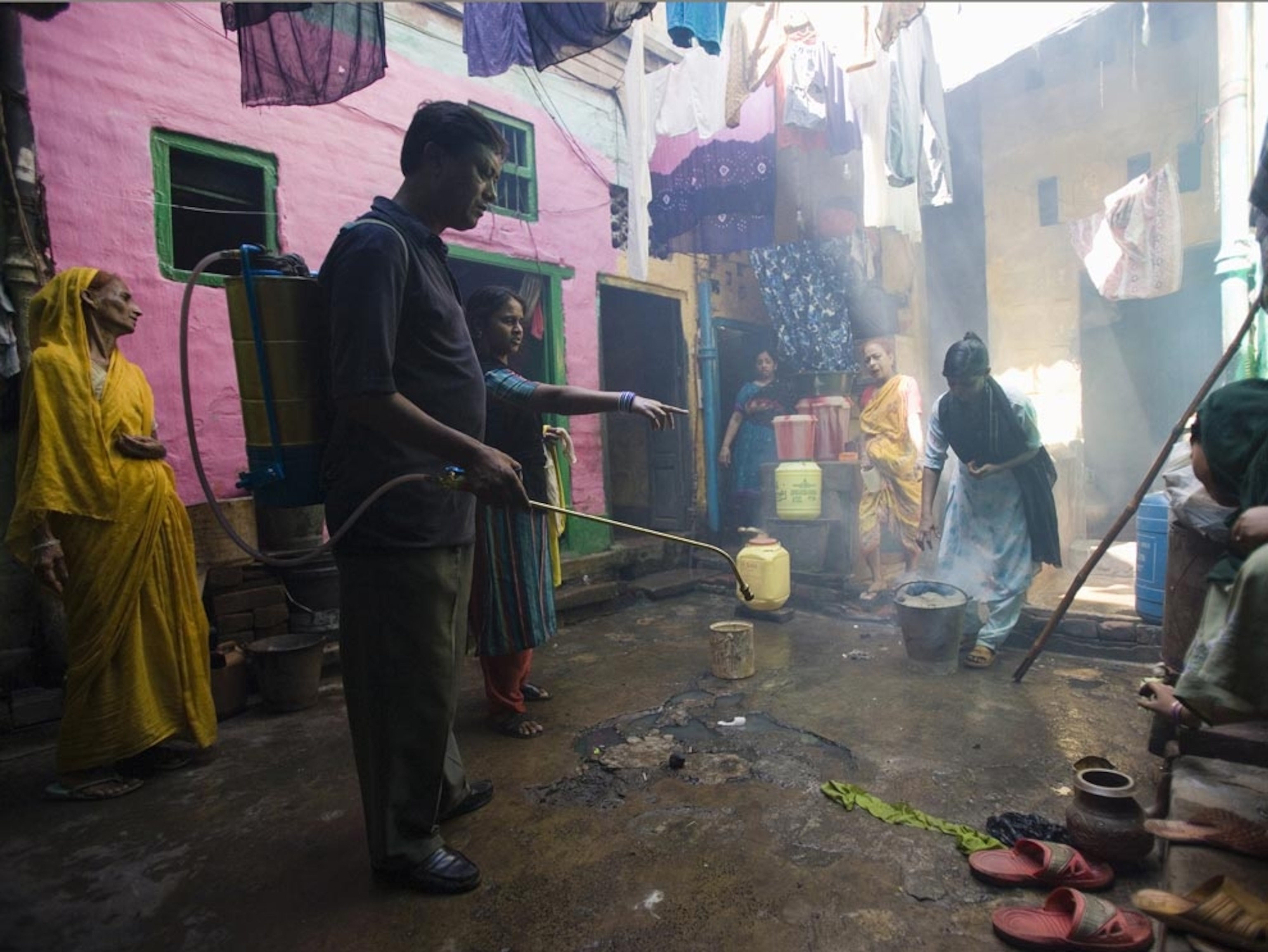The disease chiefly affects lowland tropical regions, where conditions favor Anopheles mosquitoes, which carry the malaria parasite plasmodium. It's the blood-seeking females that inject these microscopic invaders, each bite acting like an infected hypodermic needle.
Of the four kinds of plasmodia, Plasmodium falciparum is by far the most dangerous, responsible for about half of all malaria cases and 95 percent of deaths.
Parasite
The parasite has a complicated life cycle, which begins in the mosquito's gut before moving to the salivary glands, where it awaits transfer to the next host. Once in a human's bloodstream, the parasite lodges in the liver, burrowing into cells where it feasts and multiplies. After a week or two the plasmodia burst out—around 40,000 replications for each parasite that entered the body. Next they target red blood cells, this time repeatedly, until there are billions of parasites in circulation. If this cycle isn't checked, the body starts to fail, because with so many oxygen-carrying red cells being destroyed there are too few left to sustain vital organs. Meanwhile, all it takes for the parasite to pass on its grim legacy is for another mosquito to stop off for a meal.
No Vaccine
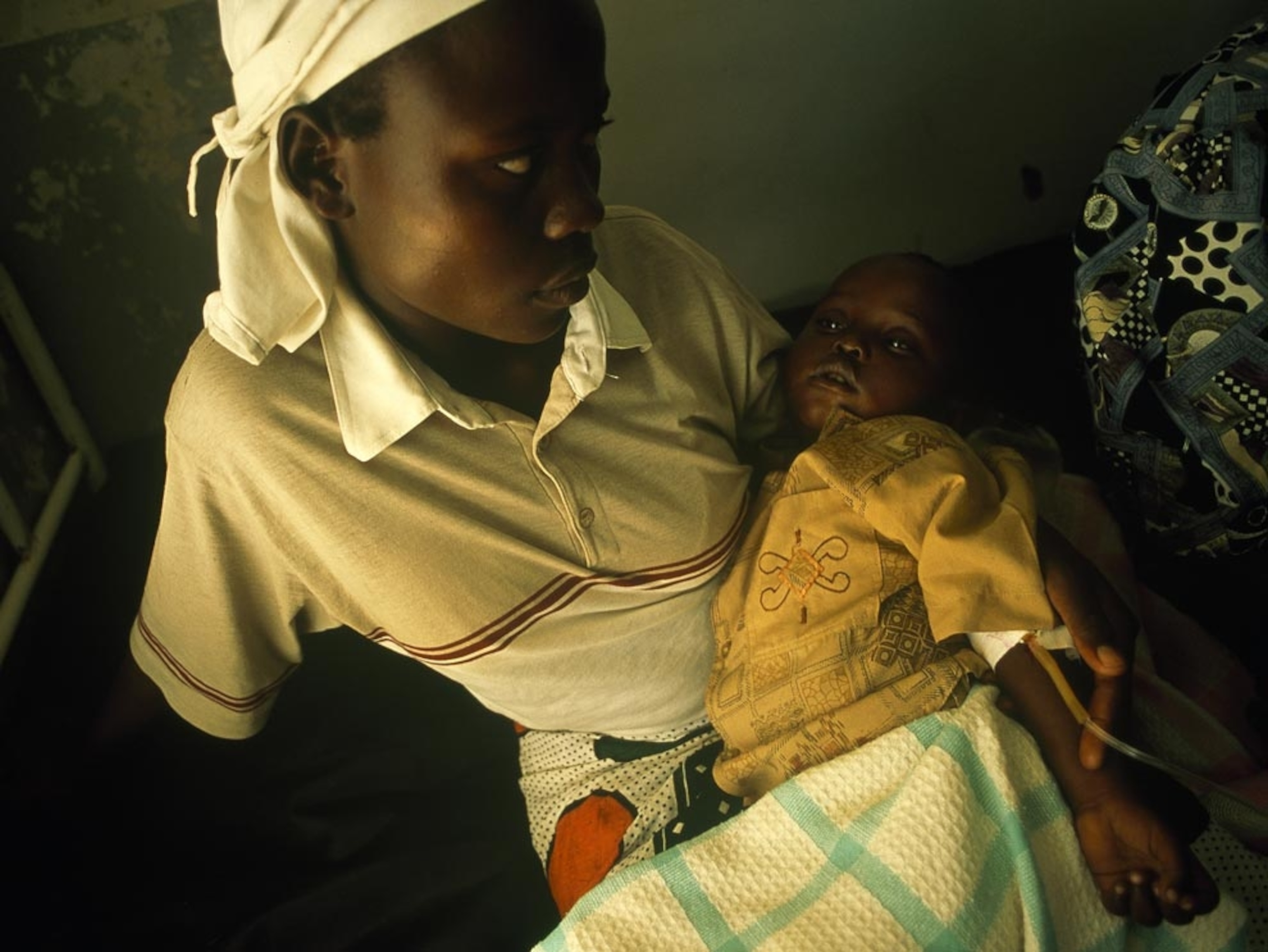
Almost two-thirds of humans infected live in sub-Saharan Africa, which also bears around 90 percent of the global malaria death toll. A child there dies from the disease about every 30 seconds. Elsewhere, countries worst affected are in southern Asia and Latin America.
Those most vulnerable are young children, who have yet to develop any resistance to the disease, and pregnant women who have reduced immunity. Signs of infection include flu-like symptoms such as fever, shivering, headache, and muscle ache. The P. falciparum parasite can lead to life-threatening conditions such as brain damage (cerebral malaria), severe anemia, and kidney failure. Survivors are often left with permanent neurological damage.
For centuries the only widely known malaria remedy was quinine, which came from the bark of the cinchona tree of Peru and Ecuador. Then, in the 1940s, a synthetic drug was created using the compound chloroquine. Around the same time, the insecticide known as DDT was developed. These twin weapons led to a worldwide assault on malaria, eradicating the disease in many areas, including the United States and southern Europe.
But malaria has made a major comeback since the 1970s, partly because DDT use was severely restricted after it was found to be harmful to certain wildlife, and because the plasmodium parasite started becoming resistant to anti-malaria drugs.
With more people now falling sick from malaria than ever before, the need to tackle it has never been so urgent. The top priority, health experts say, is finding a vaccine—seen as the only surefire way of beating the disease.