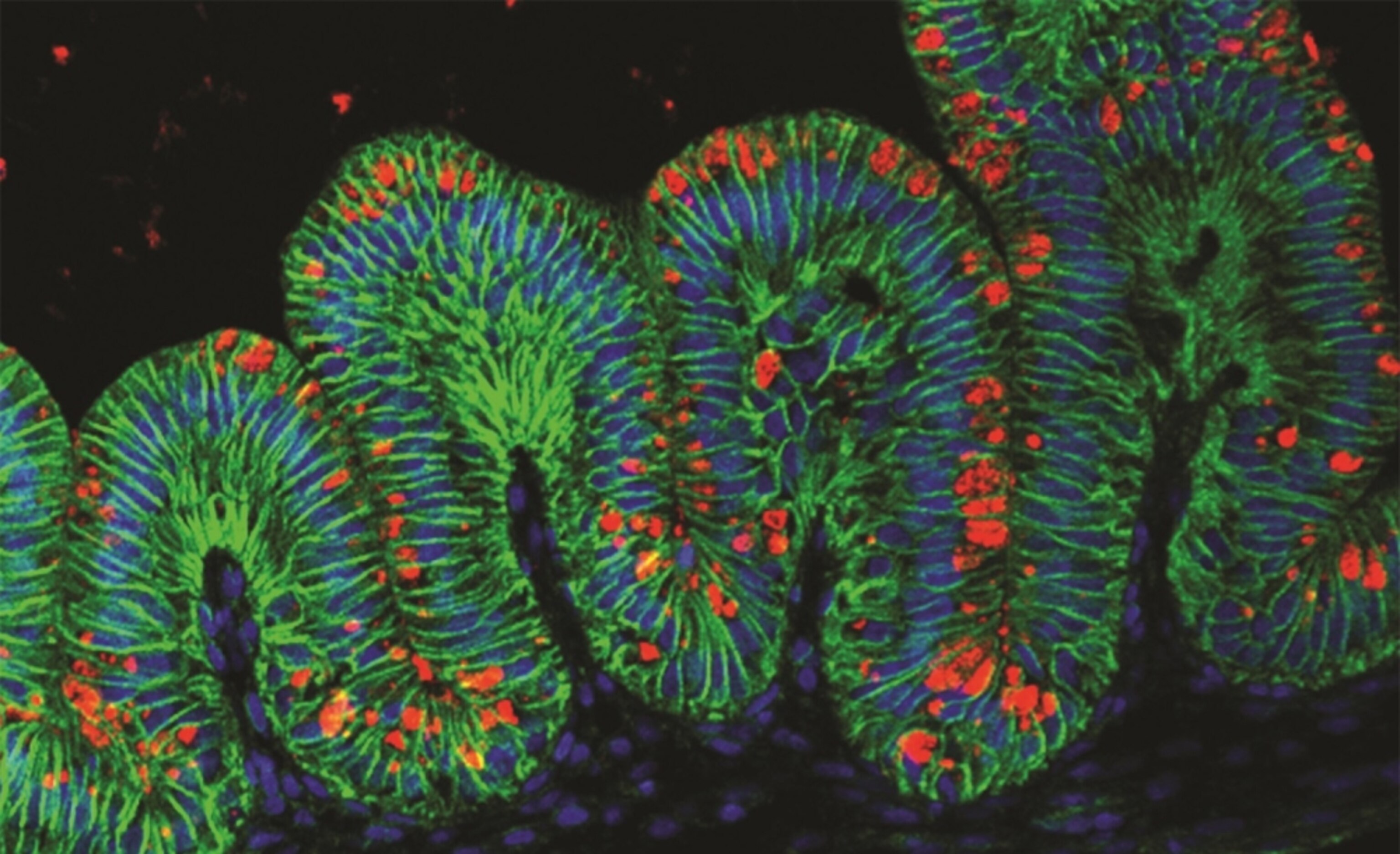
A Personalised Mini-Stomach, Grown in a Dish
In a lab at Cincinnati Children’s Hospital Medical Center, a series of small blobs sit in a Petri dish. They’re white, hollow, and the size of small peas.
They are stomachs.
More precisely, they are lab-grown model stomachs. Graduate student Kyle McCracken worked out how to make them by coaxing stem cells into producing stomach tissue—a feat that no one had yet managed. The results look like simple baubles, but the growing cells somehow organise themselves into the classic architecture of an actual stomach. They make the right layers, folds, and pockets, and they switch on the usual genes. “They’re not mixed bags of cells,” says Jim Wells, who led the study. “They look shockingly like mini-stomachs.”
These creations, known as gastric organoids, are more representative of our actual organs than cultured stomach cells, which lack any three-dimensional structure, or lab mice, which don’t suffer from stomach diseases in the same way as us. They’re not going to help you digest your meals, but they do open the door to experiments that couldn’t be done before.
For example, we know that diseases like ulcers and stomach cancer are mostly caused by a bacterium called Helicobacter pylori. This spiralling microbe has been humanity’s companion since our origins in Africa, and used to infect the majority of people. It colonises us during childhood and stays with us for decades, and even helps us to regulate the acids in our stomachs. But it can also cause disease, typically later in life.
Many scientists have studied H.pylori and how it affects the stomach for decades. Some have even won Nobel prizes for their efforts. But the moments when the microbe colonises a young stomach—those very first handshakes between host and bacterium—are still a mystery, and one that Wells hopes the organoids can solve. “Now we can say: Bacteria, meet stomach,” says Wells. “Then, what happens?”
The gastric organoids are the latest in a growing line of ‘organs-in-a-dish’. Other scientists have used stem cells to grow versions of many other organs, including eyes, guts, kidneys, and even brains. But growing stomachs proved to be exceptionally challenging, because the team didn’t have a clear map to follow.
Through decades of work, researchers have thoroughly charted the genes and molecules that turn stem cells into different organs, and followed these steps to direct the development of the equivalent organoids. But the stomach is the Ringo of viscera—it doesn’t get a lot of attention compared to starrier neighbours like the liver or pancreas. “We just didn’t have a good blueprint for how the stomach forms,” says Wells. They had to work that out for themselves.
For example, McCracken showed that two genes, WNT3A and FGF4, work together to convince a ball of stem cells to create a gut tube—a primitive tube that eventually becomes the entire digestive system. The gut tube divides into three sections and the stomach develops from the first of these—the foregut. To make that, the team had to block a gene called BMP that defines the later sections. In similar ways, McCracken had to identify genes and chemicals that tell the developing organoids to make a complex lining, full of glands that secrete digestive juices and cells that release appetite-controlling hormones.
For the moment, the organoids are still immature. They’re like the stomach of a third-trimester foetus, so they lack some of the features that adult organs have. They also represent just one part of the stomach—the antrum, which connects it to the intestine. The team are now working on developing the other part—the acid-secreting fundus.
But as they stand, the organoids can already be used for experiments. Team member Yana Zavros found that they react to H.pylori much like actual stomachs would. The bacteria stick to their linings and trigger the growth of more cells, but only if they carried a gene called CagA. This gene makes a protein that H.pylori can injects into its host’s cells to exert its influence over them. It’s an interaction gene, and strains with CagA are more likely to cause stomach cancer and to protect against oesophageal cancer. The organoids could help scientists to study both of these effects.
They can also be personalised. Wells’ team can take your cells, revert them to stem cells, and create a miniature version of your stomach in a dish.
There’s a lot of potential there. You could see how different strains of H.pylori affect people from different parts of the world, for example. We know this match between host and microbes is important. In some regions, people have much higher rates of stomach cancer because they carry H.pylori strains that don’t share their ancestrycarry H.pylori strains that don’t share their ancestrycarry H.pylori strains that don’t share their ancestry. With organoids, perhaps scientists can work out why that is, or whether your particular strains are going to cause trouble in your particular stomach.
Reference: McCracken, Cata, Crawford, Sinagoga, Schumacher, Rockich, Tsai, Mayhew, Spence, Zavros & Wells. 2014. Modelling human development and disease in pluripotent stem-cell-derived gastric organoids. Nature http://dx.doi.org/10.1038/nature13863
More on organoids:The Cerebral Organoid, a Lab-Grown Model Brain