
To save lives, midwives mix Mayan heritage with Western medicine
The fight to reduce maternal and infant deaths in Guatemala and Mexico doesn’t usually take place in fully staffed hospitals but in bare-boned rooms hours away.
Nuevo San Antonio, Guatemala — In a dimly lit green bedroom in Guatemala’s western highlands, the 66-year-old midwife chants the words like a prayer, mixing Spanish and her K’iche' Indigenous language as she cradles the woman giving birth on the ground before her.
“Breathe. Breathe, mija,” says Epifanía Elías. “You have to breathe. Be strong.”
Her patient, 25-year-old Leidy Chavez, writhes in pain, gripping the thick wool picnic blanket she has laid on the floor of her family’s home. None of Chavez’s family members are present, but Elías and her sister-in-law provide some comfort by gently stroking her hair.
In this tiny mountain village of stretching corn fields, where access to running water is scarce and basic healthcare services limited, pregnancies tend to be high-risk, according to the region’s health official. Indigenous midwives like Elías are the frontline soldiers in the battle to reduce maternal and infant death—not just in Guatemala but across other parts of Central America and southern Mexico.

“They’re the women improving access to healthcare, because often women can’t go to places like health centers to give birth,” says Edgar Kestler, director of Guatemala’s Epidemiological Research Center in Sexual and Reproductive Health.
Guatemala has the highest maternal death rate in Latin America, according to a 2017 report from the World Bank (the most recent data available). In this country, 115 mothers die in childbirth, compared to the regional average of 87 per every 100,000 births. Infant mortality rates are even higher with two of every 100 children dying in birth.
“Such alarming figures can be attributed to the extremely low levels of formal prenatal and delivery care, especially in rural areas,” the World Bank report states. “Almost three-quarters of maternal deaths are among women of Indigenous ancestry.”
The fight to save mothers and newborns doesn’t usually take place in hospitals with well-staffed, well-equipped medical teams. It happens in bare-boned rooms like this one where Chavez is giving birth, hours from a hospital. As the sun sets over the distant mountains, the room gets quiet except for Elías softly whispering to the birthing mother, “ya está llegando”— here she comes. Seconds later, an eruption of cries comes from the newborn who gets swaddled in a sea blue blanket.


With mother and daughter now out of danger, Elías soon shifts her attention to other expectant mothers. She sometimes walks hours to reach patients, her simple medical bag slung over her shoulders in a red woven Mayan cloth.
The work done by midwives has become even more essential during the COVID-19 pandemic. Hospitals have struggled to stay afloat, and patients have been turned away from health facilities. Women like Elías fill in the cracks.
“We're doing what the health system doesn't,” she says. “We work more than the doctors, and we’re the ones helping women. Midnight. 1 a.m., 2 a.m., at any hour. When they call, ... you have to go to the patient.”

Evolution of midwives
Here, in the remnants of the Mayan empire, a region spanning from southern Mexico to northern Central America, Indigenous women have been passing on the tradition for centuries. Known as parteras or comadronas, midwives were some of the region’s first healthcare providers.
The practice is believed to be a talent bestowed upon women, often handed down generation-to-generation. Mother to daughter, daughter to granddaughter.
As a young woman, Elías would watch her mother care for pregnant women, going house-to-house to do prenatal checkups, working with herbal medicines, delivering babies, and doing traditional steam baths called “temazcal” after the births.
Elías herself didn’t begin the work until she delivered her own baby, alone, on the floor of her kitchen. Her mother was off treating another patient when Elías, then 35, went into labor.
“I felt the baby was about to be born, so I woke my husband up and told him ‘Get up, the baby is coming.’ He told me ‘no, no, no. I don’t want to do it. Ay, I’m scared!’” she remembers.
“But I didn’t feel scared. I felt strong.”
She went on to become one of at least 22,000 traditional midwives working across Guatemala and 15,000 in Mexico, according to government figures. In Guatemala alone, comadronas deliver half of the country’s births.

Over three decades, Eiías has become the most active and trusted midwife in her area, taking daily treks to see patients.
“Those women (patients) fall under the care of the comadrona, who go to their homes and shorten the massive distances between these communities (and healthcare),” Kestler says.

Maternal and infant mortality are preventable crises defined by global health inequalities.
Health providers across the globe have been able to slash death rates among women and infants over the past two decades, especially in higher-income nations, says Aboubacar Kampo, health program director for UNICEF. Midwives, says Kampo, are crucial to that progress.
“We’ve halved the number of (global maternal and infant) deaths, and that’s definitely a success,” he says. “I don’t think the global community has wasted its time.”
Yet the danger is still high in parts of Latin America, sub-Saharan Africa, and Southeast Asia.
The toll of COVID-19
In the broader Mayan region, Indigenous and rural women are more vulnerable to high-risk pregnancies. In Guatemala, they’re twice as likely to die during birth than the average woman, United Nations data shows. Those women are also fighting a range of uphill battles, including a growing hunger crisis.
In this farming town of Nuevo San Antonio, the closest thing residents have to a health center is a small building, perpetually understaffed with broken medical equipment, where the first thing nurses ask is: “Is your child malnourished?”


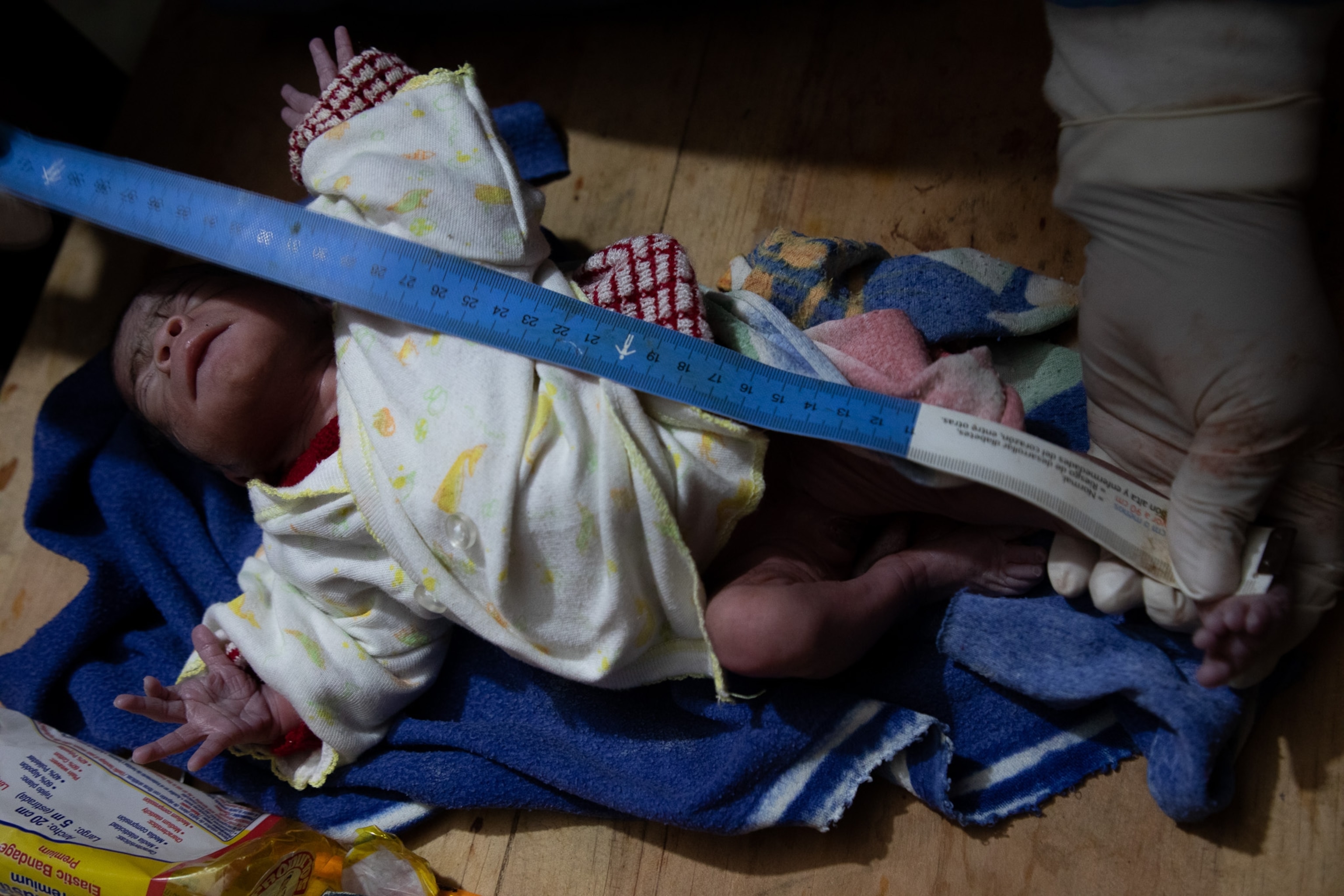
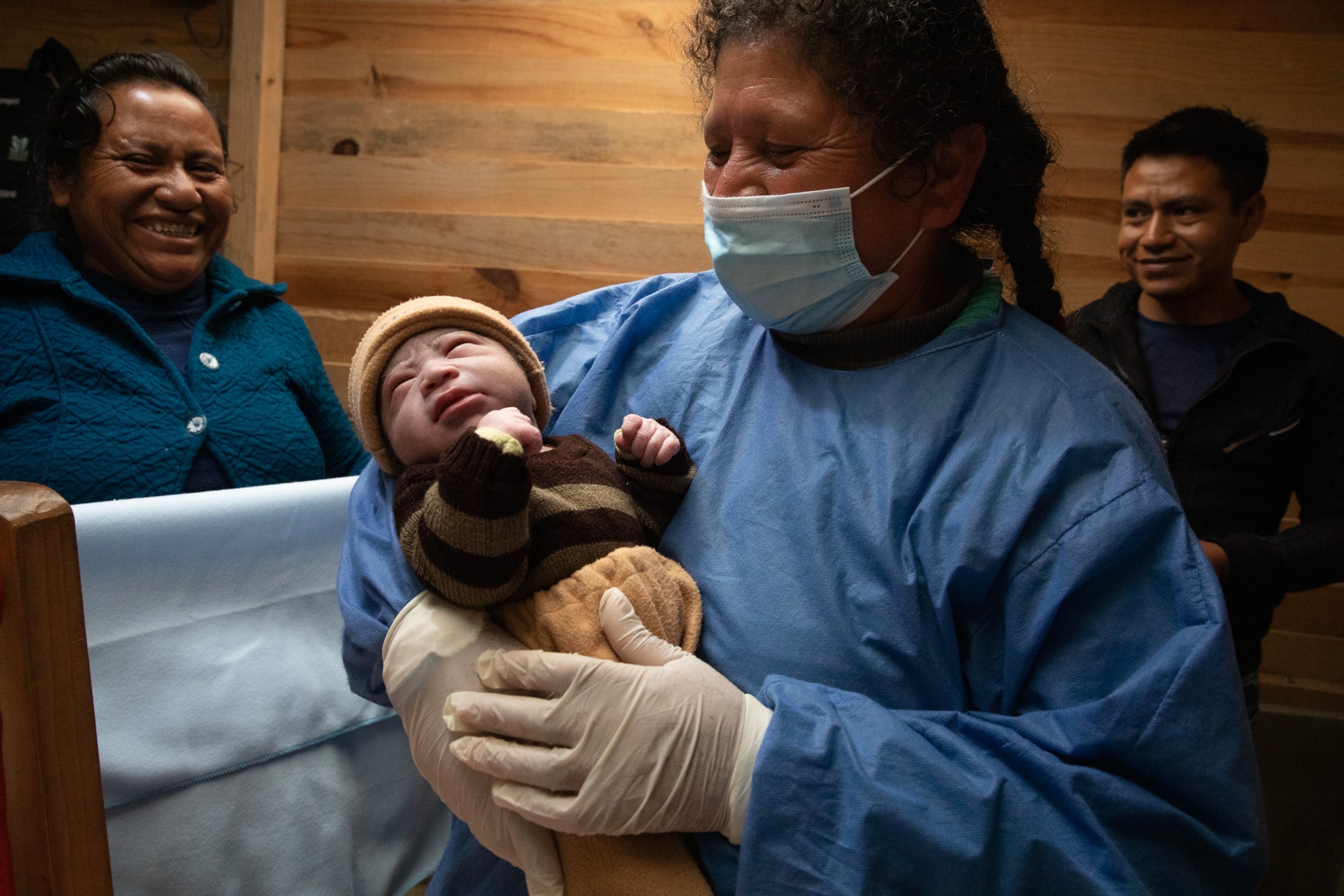
Lack of state presence in such zones has spurred accusations by experts, doctors, women, and midwives, who say that regional governments have failed women in rural areas.
While Guatemala’s Health Ministry declined to comment on criticisms, Ana Luz de León Barrios, of the country’s National Program of Reproductive Health, attributed the lack of health services to logistics.
“We’re a country … that has many problems with its infrastructure, with very far-off communities, so it impedes health services from reaching many people,” León Barrios says.

Without advanced medical care or the resources to pay a private clinic, women seek out midwives. But comandronas like Elías often earn little more than 400 quetzales ($52) for weeks of work that includes prenatal care through childbirth. Because of it, midwives, too, often lack basic resources including stethoscopes, oximeters, and ultrasound machines, essential tools in detecting complications early on.
Over the past two years, access to healthcare has diminished, just as endemic fear of mistreatment or exposure to the coronavirus festered. For many midwives work has more than doubled.
“Women don’t want to go to the hospital, even if the pregnancy complicates, because they can get infected [with COVID], so they think it's better to do it at home,” Elías says. “They say: ‘If I die, I'm going to die here, not in the hospital.’”
That was the choice made by Elías’s patient, Chavez, who smiled as she cuddled her newborn daughter under a pile of blankets.


This pregnancy had been marked by difficulties. With the region’s economy still ravaged by COVID-19, Chavez has struggled to put food on the table and she could not afford to buy prenatal pills before the birth. She managed to pay for an ultrasound at a private clinic about 30 minutes away, but it cost her two days of work in the cornfields.
To make ends meet, her husband migrated to the United States to work, leaving her alone, just a year after a previous pregnancy ended in miscarriage. She worried the same would happen with her recent pregnancy.

“I was scared that I would lose my baby,” she said. “But thank God, everything was fine.”
While aid providers like UNICEF say it’s still difficult to pinpoint exactly how much progress on infant and maternal mortality has been lost during the pandemic in Guatemala and elsewhere, Kampo says the backslide will be felt for decades.
“We’ve lost (progress). Now, is it 10 years, or 20 years? It’s difficult to say because we haven’t seen the full fallout of COVID-19,” Kampo says. “But it’ll take us a long time to recover, especially in poorer countries.”
A cultural chasm
The fear of a potential uptick in infant and mortality rates, coupled with patients seeking a higher level of medical care as a last resort has resurfaced old tensions between health officials and midwives.

Both fight for the same thing—reducing maternal and infant deaths—but simultaneously exist on two sides of a chasm that has divided the region for decades.
Midwives accuse medical staff of discriminating against them, mistreating their patients, and blocking them from entering medical facilities. Health officials, meanwhile, are quick to note the important role midwives play across the region, but some also blame the comadronas for maternal deaths. They accuse comadronas of bringing birthing mothers to the hospitals after it's too late.
“You feel frustrated because you know you could’ve done more, but in the end, it just wasn't possible,” Alvaro Recinos, who works at a hospital in Guatemala’s second biggest city, says of the patients he’s lost.
Some health authorities also say many midwives are not qualified to deliver births and accuse some of using unauthorized drugs on patients. While there is no hard evidence to back those claims, physicians say they often see patients come to the hospital in grave condition with symptoms from the drug, oxytocin, used to induce labor.
Frenzied hospital care
At the hospital in Quetzaltenango, Recinos rushes with a pack of other doctors and nurses to wheel in a young woman who is in labor. The hospital is the only source of higher-level care in western Guatemala, and women sometimes travel half a day to get here.
While the workload for midwives like Elías has skyrocketed, the number of expectant mothers doctors treat has decreased. But when women do arrive to the hospital during childbirth, they often come on their deathbeds, Recinos says.
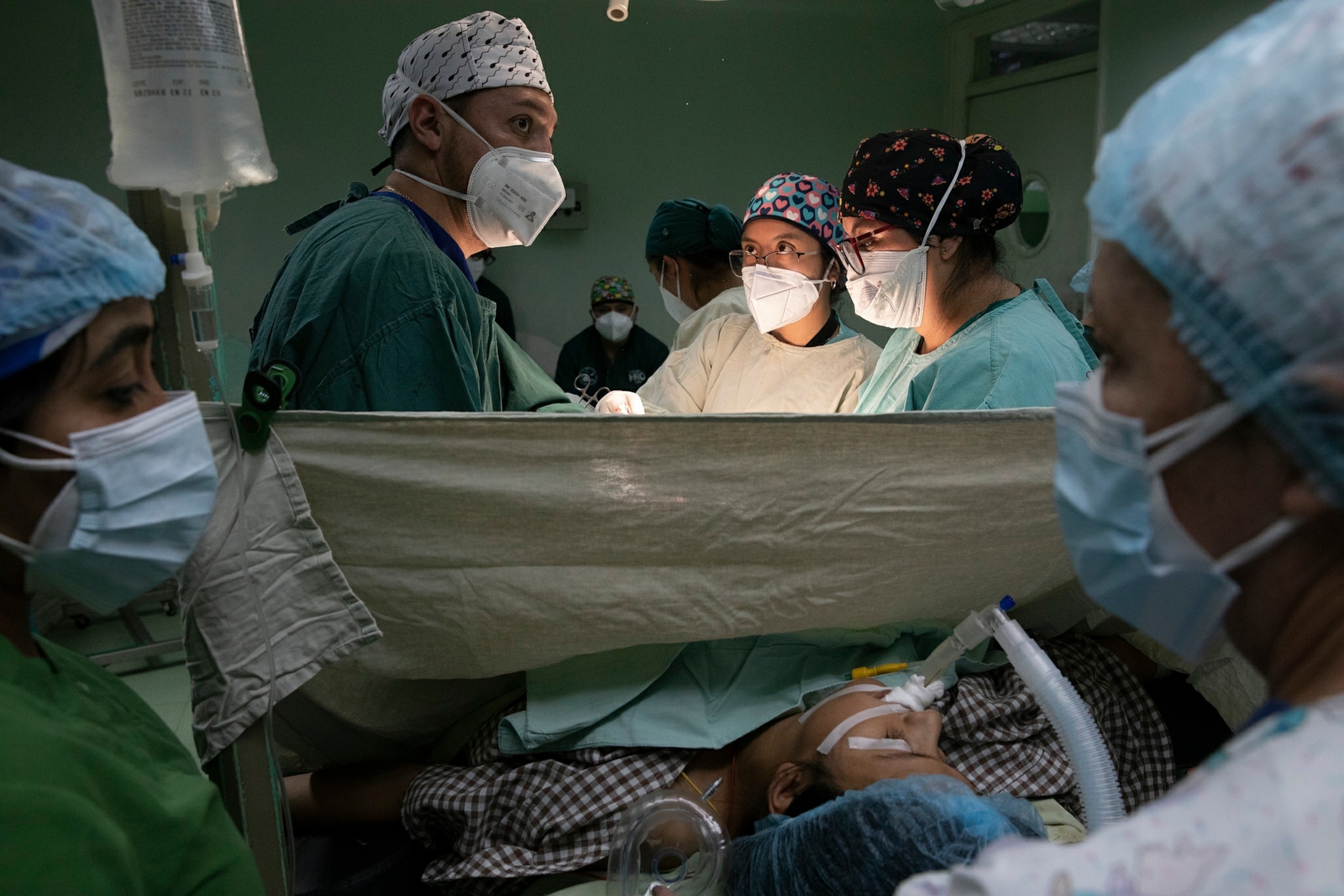
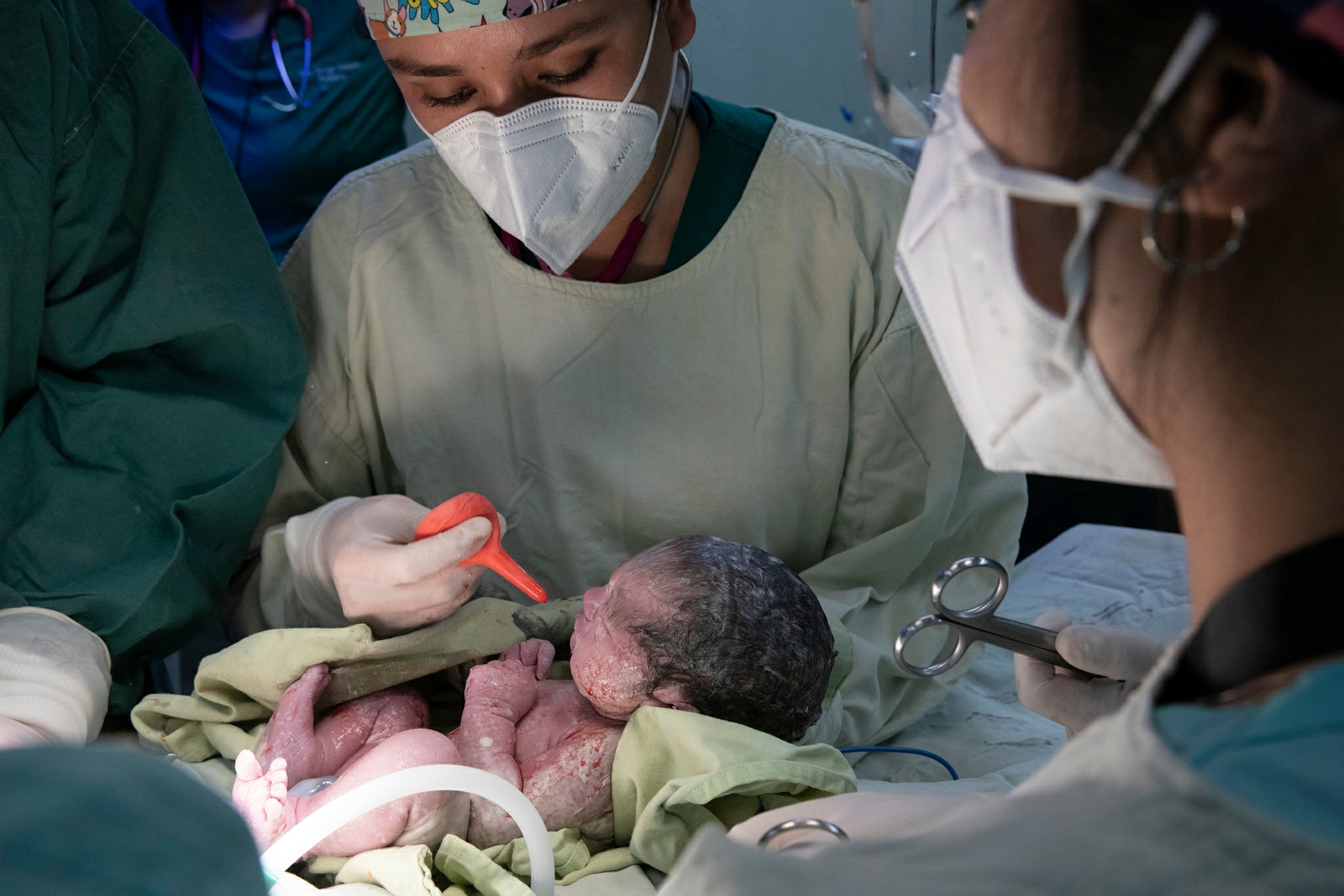
On this day, the hospital staff is frantically tending to a patient with a heart condition that went undiagnosed because she had no health center in her rural community. Now, she’s giving birth during cardiac arrest.
Nurses line up sets of towels and scissors, preparing for the Cesarean surgery as if they were going to war. Recinos, wearing a Garfield scrub cap and a N95 mask wrapped around his face, snaps on a pair of gloves.
Recinos tells the woman—half conscious, scared, and alone—“you’re going to feel a little cold,” as a group of doctors operate. After two hours in a tense surgical room, the stress slowly melts away as the patient's vital signs stabilize with the steady “beep, beep, beep” of the heart monitor.
“If she had decided to have her birth with a comadrona, she would have died,” Recinos says.
Yet it’s those very midwives who often convince women to seek healthcare in hospitals in high-risk situations like this one.
‘Keeping this tradition alive’
In the high hills above Quetzaltenango’s hospital, Emelda López Sánchez stands in the single room of an adobe home in the heart of Concepción Chiquirichapa, a tiny 17,000-person town marked by dirt roads and potato farms.
The 40-year-old comadrona carefully wraps a blood pressure monitor around one of the woman’s arms as a dozen of midwives around her watch intently. The midwives peer over as López Sánchez explains in her native language, Mam, how to take a blood pressure reading.

She leads the Association of Comadronas in the Mam Area (ACAM), a collective of 71 midwives surrounding the small town of Concepcion Chiquirichapa. The collective is just one of hundreds of grassroots groups across the region working to train midwives based in far-off communities.
Midwives in the Mayan region have fought a decades-long battle to be recognized by their governments and to bridge the divide with the public health system.
Guatemala and Mexico’s governments have launched programs to help train midwives, and provide some resources. But critics say those efforts have fallen flat.
“Traditional midwives here are incredibly important, and will be incredibly important in the next 50 years. But not because there’s a health policy recognizing that,” Kestler says. “Rather, it’s the exact opposite. The health system is so fragmented, with such little focus on primary care, and that’s where comadronas get their importance.”
ACAM travels by bus out to remote communities to provide ultrasounds and prenatal kits. The organization also constructed a birthing clinic, staffed with a handful of medically trained traditional midwives and a doctor who assists in more complex cases.

“While the government doesn’t recognize us, we’re at least doing something important in our community,” she said. “We’ve mixed traditional medicine with Western medicine, and it’s helped a lot.”
In Mexico, such movements have gained even more traction, becoming a voice pushing for international recognition. In southern Chiapas, the grassroots movement Nich Ixim was created in 2014 to pressure authorities into recognizing midwives’ work.
“We’ve learned it’s much better to be united than all alone,” says Ofelia Pérez, a leader of the movement.
For Pérez and López Sánchez, the work also serves another purpose: to pass on a dying tradition.
ACAM was formed 17 years ago to train a new generation, the children of current comadronas. But today, leaders say younger women have turned away from the practice, causing scarcity at a time when UNICEF’s Kampo highlights a need for more midwives.
It’s an existential threat, not just for midwives, but to the very women they serve, says López Sánchez.
“If comadronas were to go extinct, the consequences would be the deaths of many women,” she says. “And hospitals could collapse from the number of patients.”

But in the pandemic, their small building has gained increasing importance in their small community, bringing new hope that their work won’t die out.
“It's about preserving the culture. Keeping this tradition alive,” she says, wrapping her hand around the fabric of her deep green and blue Mayan skirt as her team drives down a rugged roadway, returning from a training. “We have to continue passing it on to the next generation.”

Janet Jarman is a documentary photographer and filmmaker based in Mexico City. Follow her on Instagram.