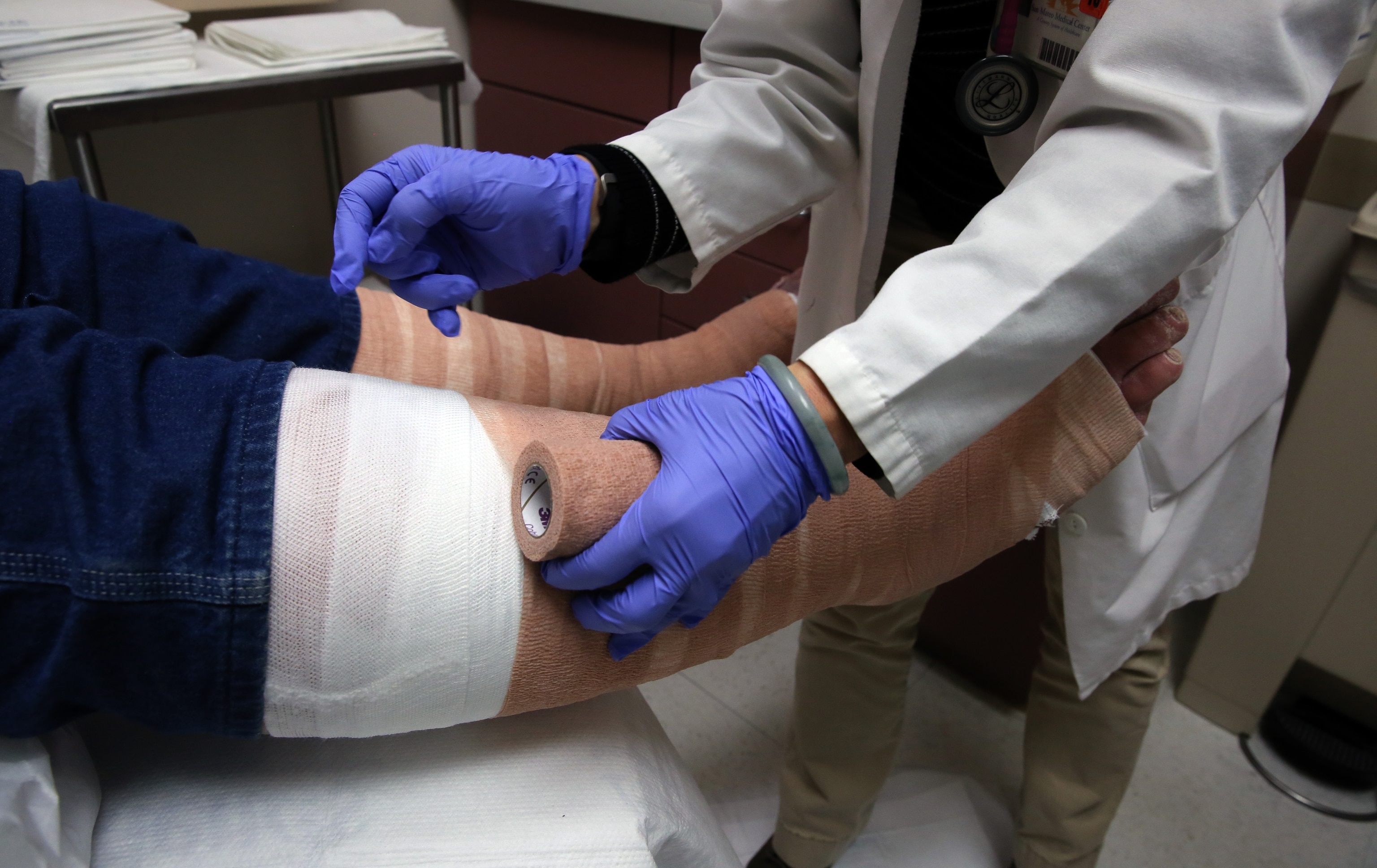
This underdiagnosed vein disorder affects 4 in 10 Americans
From tingly legs to bulging veins, these warning signs may point to chronic venous insufficiency—a widespread circulatory issue doctors say is on the rise.
Swelling, aching calves, tingling, or bulging veins might seem like everyday discomforts, but they could point to a hidden problem in your circulatory system. A surprisingly common yet underrecognized condition called chronic venous insufficiency is behind a growing number of cases—and scientists say it’s far more widespread than most people realize.
Here are five things to know about this painful and underdiagnosed vascular disorder.
What is chronic venous insufficiency?
Chronic venous insufficiency (CVI) occurs when the valves in your leg veins become weak or damaged and begin leaking. “Because veins carry blood back to the heart, these leaky valves can allow blood to flow backward or pool in the leg,” says Raul Guzman, division chief of vascular surgery and endovascular therapy at Yale School of Medicine, New Haven Hospital.
Over time, this backward flow and pooling increases pressure within the veins, leading to inflammation and damage to surrounding tissues. Left unchecked, the condition can trigger a chain reaction that affects both the skin’s surface and the deeper structures of the leg.
Early signs and symptoms of CVI
Early signs of CVI can be as subtle as a tight feeling in your calves, cramping, or especially heavy or tired legs after a long day. But as the condition progresses, symptoms often intensify and include “pain or discomfort in the leg, swelling, and skin damage,” explains Guzman. The skin may take on a discolored or leathery appearance, become itchy or cracked, and develop slow-healing wounds or ulcers.
(Scientists are unraveling the mysteries of pain.)
Due to the pooling blood, varicose and bulging veins are another hallmark sign, though not everyone with CVI has them. Left untreated, CVI can lead to increased venous pressure, more serious conditions, and even blood clots.
Who is most at risk for CVI?
Despite its low profile, chronic venous insufficiency affects an estimated 40 percent of Americans, according to the Society for Vascular Surgery. It’s especially common in women over 50 and those who are pregnant. But men aren’t immune, particularly if they lead a sedentary lifestyle or are living with obesity. It’s also prevalent in individuals with a history of deep vein thrombosis or other venous diseases. “We know that there is a hereditary component to CVI,” says Guzman.
(Why heart attacks are rising in young adults—and what to watch out for.)
Smoking and high blood pressure can also contribute to the condition. So can jobs that require prolonged standing or sitting because they “may cause blood to pool in the legs, increasing pressure on your veins,” says Marie Robert, a surgical pathologist at Yale School of Medicine, New Haven Hospital.
Why CVI is often misdiagnosed
One of the biggest challenges with CVI is that its symptoms are frequently misinterpreted. Swollen legs may be attributed to aging or fluid retention. Varicose veins are often seen as purely cosmetic, and skin changes may be mistaken for eczema or unrelated irritation.
But ignoring these signs can allow the condition to worsen, Guzman says—sometimes even resulting in irreversible damage. That’s why it’s essential to consult a healthcare provider, such as a vascular specialist, if even minor symptoms persist or worsen.
Robert says that a simple physical exam and either an magnetic resonance angiogram (MRA) or ultrasound are usually all that are needed to determine whether CVI is present and what treatment may be required.
How is CVI treated
The good news is that CVI is highly treatable, especially when caught early. Doctors often begin with conservative approaches, such as suggestions to elevate your legs above your heart during the day and using compression garments to improve blood flow. “The first method of treatment involves the use of elastic compression stockings,” says Guzman.
(The ability to reverse damage to your lungs and heart is tantalizingly close.)
Lifestyle changes, such as weight loss, improving diet, regular exercise, and avoiding prolonged periods of sitting or standing, are also frequently recommended. All such recommendations “help ease swelling, improve circulation, and relieve symptoms,” says Robert.
Medications such as blood thinners or diuretics may also be prescribed to reduce swelling or improve blood flow. “And there are several surgical procedures and more advanced medical interventions that can be performed,” adds Guzman.
These include sclerotherapy (an injected solution that causes the affected veins to collapse and fade), vein stripping, angioplasty and stents, endovenous ablation (a minimally invasive procedure using heat or laser to close off the affected veins), or surgical removal of malfunctioning veins. “Use of these treatments depends on the location of the involved veins and the degree of the problem,” says Guzman.
As awareness of chronic venous insufficiency grows, so do opportunities for earlier detection and more effective management. “For many people, CVI is annoying and uncomfortable—but not usually life-threatening,” says Robert. “It’s a condition that can be helped by a variety of lifestyle changes and mild interventions.”