Inside the swift, deadly history of the Spanish Flu pandemic
Before SARS and coronavirus, Spanish flu infected a third of the world’s population and killed as many as 50 million in the waning years of World War I.

Scientist Johan Hultin traveled to Brevig Mission, Alaska, a town of a few hundred souls in the summer of 1997. He was searching for buried bodies, and Alaska’s frozen ground was the perfect place to find them. Digging through the permafrost—with permission from the town’s authorities—he eventually uncovered a woman who died almost 80 years previously and was in a state of excellent preservation. Hultin then extracted samples of the woman’s lung before reinterring her. He intended to use this to decode the genetic sequence of the virus that had killed this Inuit woman along with 90 percent of the town’s population.
Brevig Mission was just one place that was part of a global tragedy, one of the worst ever to befall humanity: the influenza pandemic of 1918-19. The outbreak of this influenza virus, also known as Spanish flu, spread with astonishing speed around the world, overwhelming India, and reaching Australia and the remote Pacific islands. In just 18 months at least a third of the world’s population was infected. Estimates on the exact number of fatalities vary wildly, from 20 million to 50 million to 100 million deaths. If the upper end of that estimate is accurate, the 1918 pandemic killed more people than both World Wars put together. (Get the facts on influenza.)
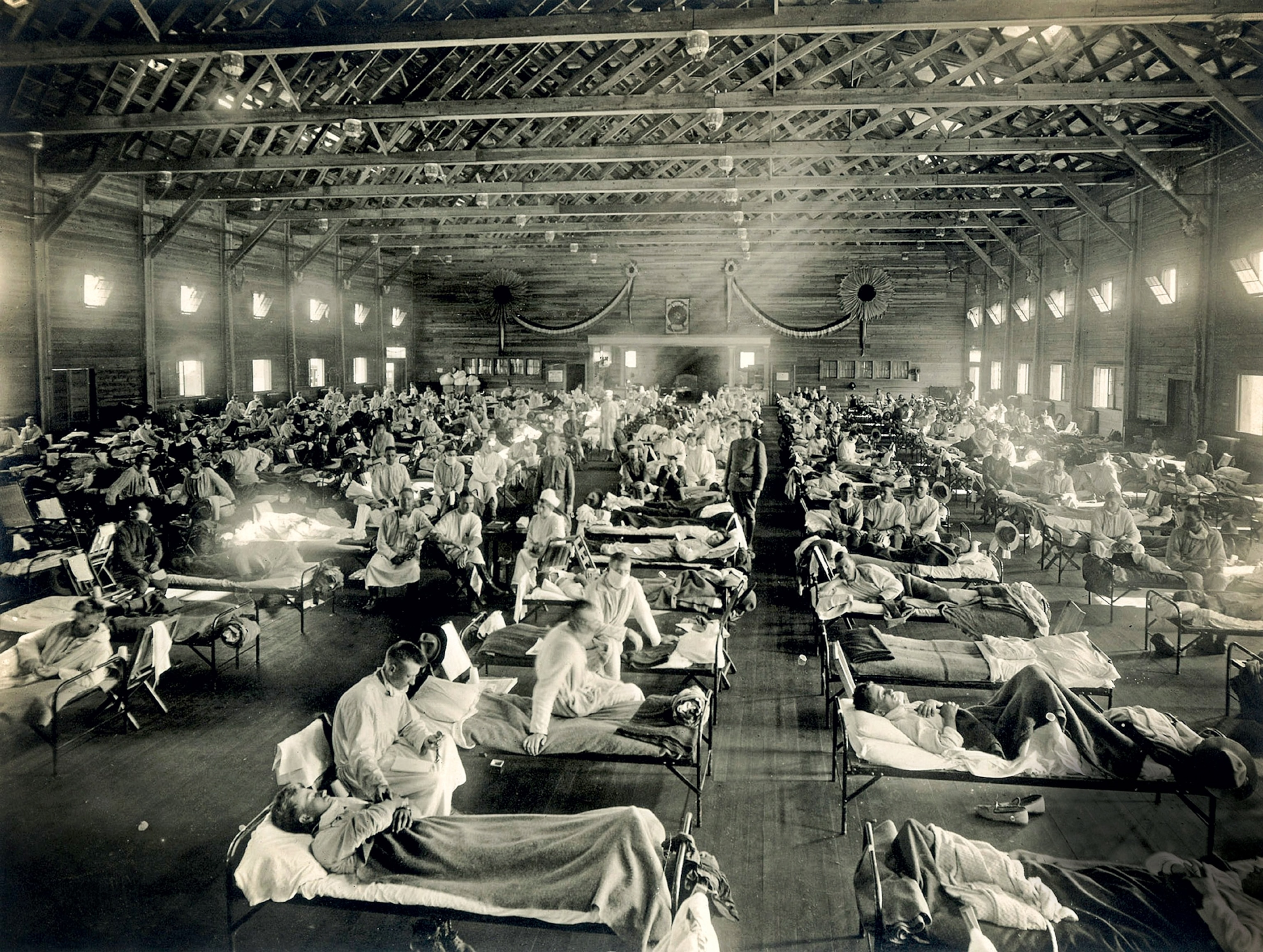
War and pestilence
Several closely related viruses cause influenza, but one strain (type A) is linked to deadly epidemics. The 1918-19 pandemic was caused by an influenza A virus known as H1N1. Despite becoming known as the Spanish flu, the first recorded cases were in the United States in the final year of World War I. (Explore the memorials of World War I.)
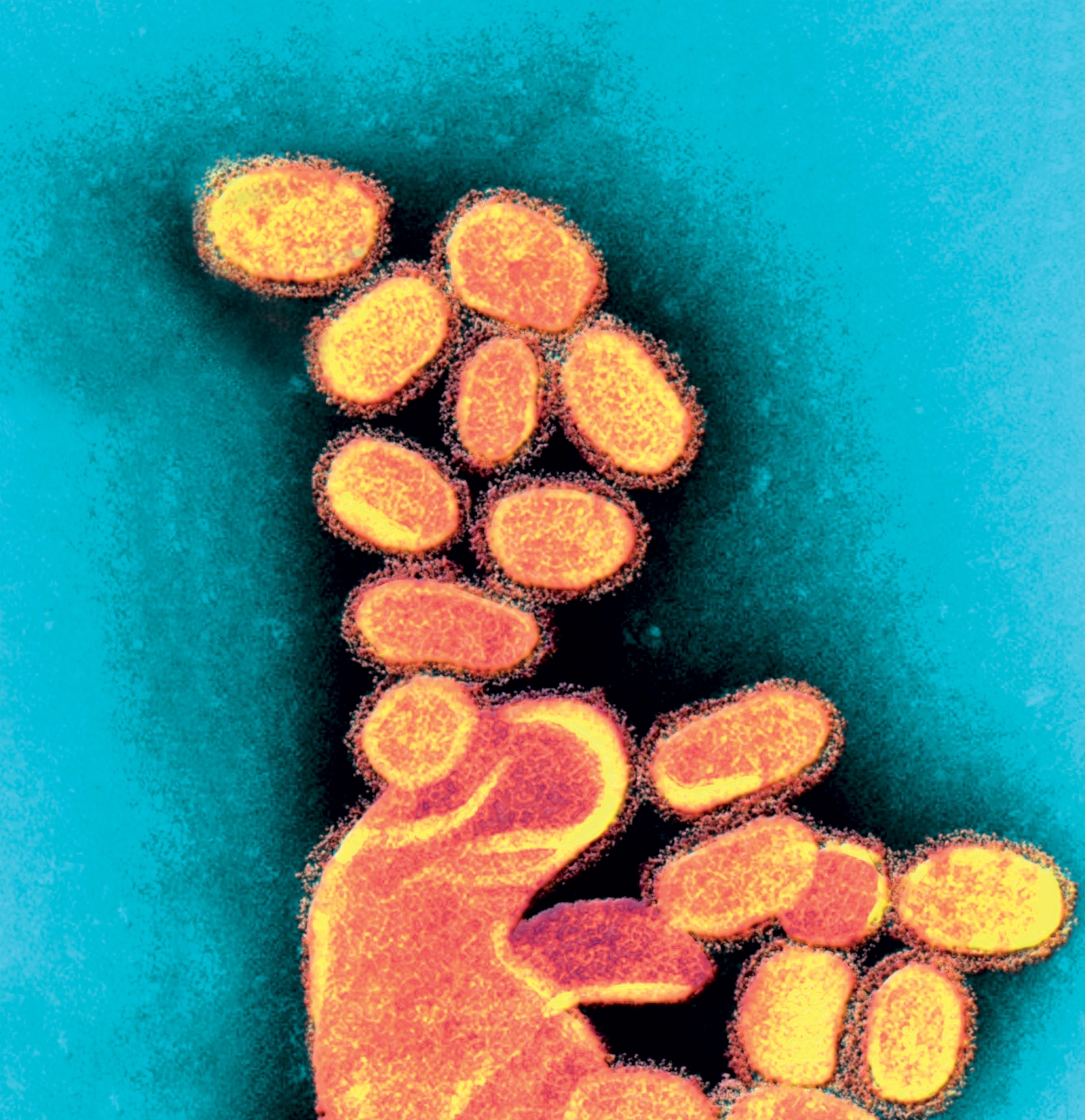
By March 1918 the United States had been at war with Germany and the Central Powers for 11 months. During that time America’s small, prewar army had grown into a vast fighting force that would eventually send more than two million men to Europe. (How the United States entered World War I.)
American forts experienced a massive expansion as the entire nation mobilized for war. One of these was Fort Riley, Kansas, where a new training facility, Camp Funston, was built to house some of the 50,000 men who would be inducted into the Army. It was here in early March that a feverish soldier reported to the infirmary. Within a few hours more than a hundred other soldiers had come down with a similar condition, and more would fall ill over the following weeks. In April more American troops arrived in Europe and brought the virus with them. The first wave of the pandemic had arrived. (What is the difference between an epidemic and a pandemic?)
Deadly speed
The Spanish flu strain killed its victims with a swiftness never seen before. In the United States stories abounded of people waking up sick and dying on their way to work. The symptoms were gruesome: Sufferers would develop a fever and become short of breath. Lack of oxygen meant their faces appeared tinged with blue. Hemorrhages filled the lungs with blood and caused catastrophic vomiting and nosebleeds, with victims drowning in their own fluids. Unlike so many strains of influenza before it, Spanish flu attacked not only the very young and the very old, but also healthy adults between the ages of 20 and 40.

The principal factor in the virus’s spread was, of course, the international conflict then in its last phase. Epidemiologists still dispute the exact origins of the virus, but there is some consensus it was the result of a genetic mutation that perhaps took place in China. But what is clear is that the new strain went global thanks to the massive and rapid movement of troops around the world.
The drama of the war also served to obscure the unusually high mortality rates of the new virus. At this early stage, the illness was not well understood and deaths were often attributed to pneumonia. Strict wartime censorship meant that the European and North American press were unable to report outbreaks. Only in neutral Spain could the press speak freely about what was happening, and it was from this media coverage that the disease took its nickname.
Deadly Contact

Epidemics are as old as civilization: Signs of smallpox appear on 12th-century B.C. Egyptian mummies. Increased contact led to the spread of disease. In the sixth century A.D. the Plague of Justinian moved along trade routes, killing 25 million people across Asia, Africa, Arabia, and Europe. Eight centuries later, the Black Death wiped out 60 percent of Europe’s population. When Europeans settled in the Americas in the 16th and 17th centuries, they introduced smallpox, influenza, and measles to the native peoples, killing an estimated 90 percent of the population. Here, Native Americans treat patients infected by European diseases in a 1591 engraving by Theodor de Bry.
The second wave
The overcrowded trenches and encampments of the First World War became the perfect hosts for the disease. As troops moved, so the infection traveled with them. The wave that had first appeared in Kansas abated after a few weeks, but this was only a temporary reprieve. By September 1918 the epidemic was ready to enter its most lethal phase.
It has been calculated that the 13 weeks between September and December 1918 constituted the most intense period, taking the greatest number of lives. At least 195,000 Americans died in October alone. In comparison, total American military casualties for the whole of World War I came in at just over 116,000. Once again, it was the crowded military encampments where the second wave initially gained a hold. In September an outbreak of 6,674 cases was reported at Camp Devens, a military base in Massachusetts.
As the crisis reached its zenith, the medical services began to be overwhelmed. Morticians and gravediggers struggled, and conducting individual funerals became impossible. Many of the dead ended up in mass graves. The end of 1918 brought a hiatus in the spread of the illness and January 1919 saw the beginning of the third and final phase. By then the disease was a much diminished force. The ferocity of the autumn and winter of the previous year was not repeated and mortality rates fell.
Although the final wave was much less lethal than its predecessors, it was still able to wreak considerable damage. Australia, which had quickly enacted quarantine restrictions, managed to escape the worst of the flu until the beginning of 1919, when the disease finally arrived and took the lives of several thousand Australians.

The general trend of mortality, however, was downward. There were cases of deaths from influenza—possibly a different strain—as late as 1920, but by the summer of 1919 health care policies and the natural genetic mutation of the virus brought the epidemic to a close. Even so, its effects, for those left bereaved or suffering long-term health complications, were to last decades.
Lasting impact
The pandemic left almost no part of the world untouched. In Great Britain 228,000 people died. The United States lost as many as 675,000 people, Japan some 400,000. The south Pacific island of Western Samoa (modern-day Samoa) lost one-fifth of its population. Researchers estimate that in India alone, fatalities totaled between 12 and 17 million. Exact data in the number of deaths is elusive, but global mortality figures are estimated to have been between 10 and 20 percent of those who were infected.
In 1997 the samples taken by Johan Hultin from the woman found in the frozen mass grave in Brevig Mission added to scientists’ knowledge as to how flu viruses mutate and spread. Drugs and improved public hygiene—in conjunction with international institutions such as the World Health Organization and national bodies such as the Centers for Disease Control and Prevention in the United States—put the international community in a much better position to meet the challenges of a new outbreak. However, scientists know a lethal mutation could occur at any time, and a century on from the mother of all pandemics, its effects on a crowded, interconnected world would be devastating.