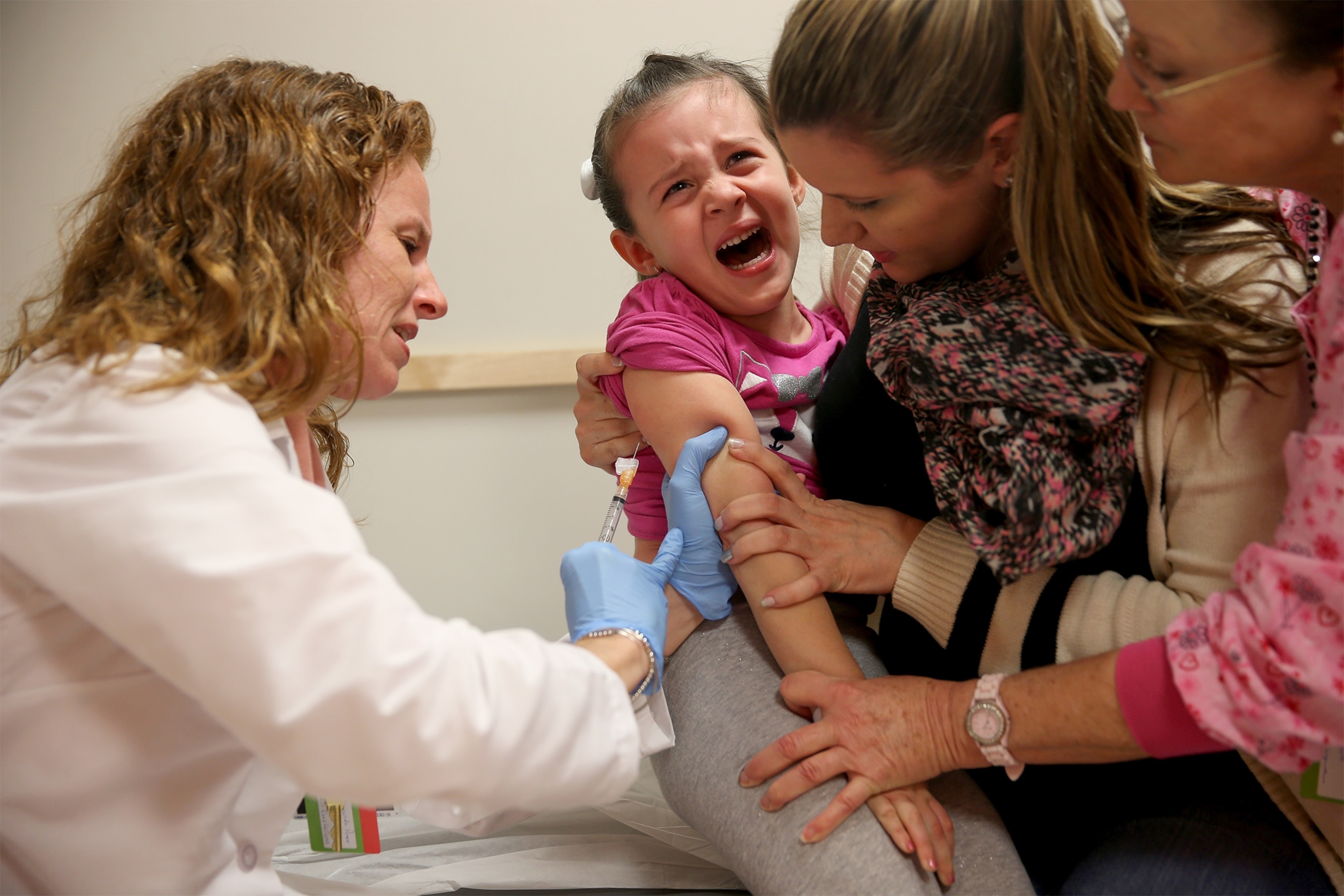
The Anti-Vaccine Generation: How Movement Against Shots Got Its Start
Mistrust and misinformation give a shot in the arm to measles vaccine naysayers.
You could call New Jersey Governor Chris Christie and Kentucky Senator Rand Paul members of the "vax generation."
Born in 1962 and 1963, respectively, they were in grade school when the newly developed measles vaccine became the life-saving advance that protected millions from a highly contagious childhood disease. Though not as scary as polio, it was potent enough to strike four million kids, hospitalize 48,000 of them with complications, and kill more than 400 every year.
That both men stoked an anti-vax movement this week by suggesting in the middle of a national measles outbreak that parents should be allowed to choose whether to vaccinate their children speaks to a generational shift in thinking about science and politics. Parents should have "some measure of choice" in vaccinating their children, Christie told a reporter, while Paul called the decision not to vaccinate "an issue of freedom."
This is a dangerous game to play.
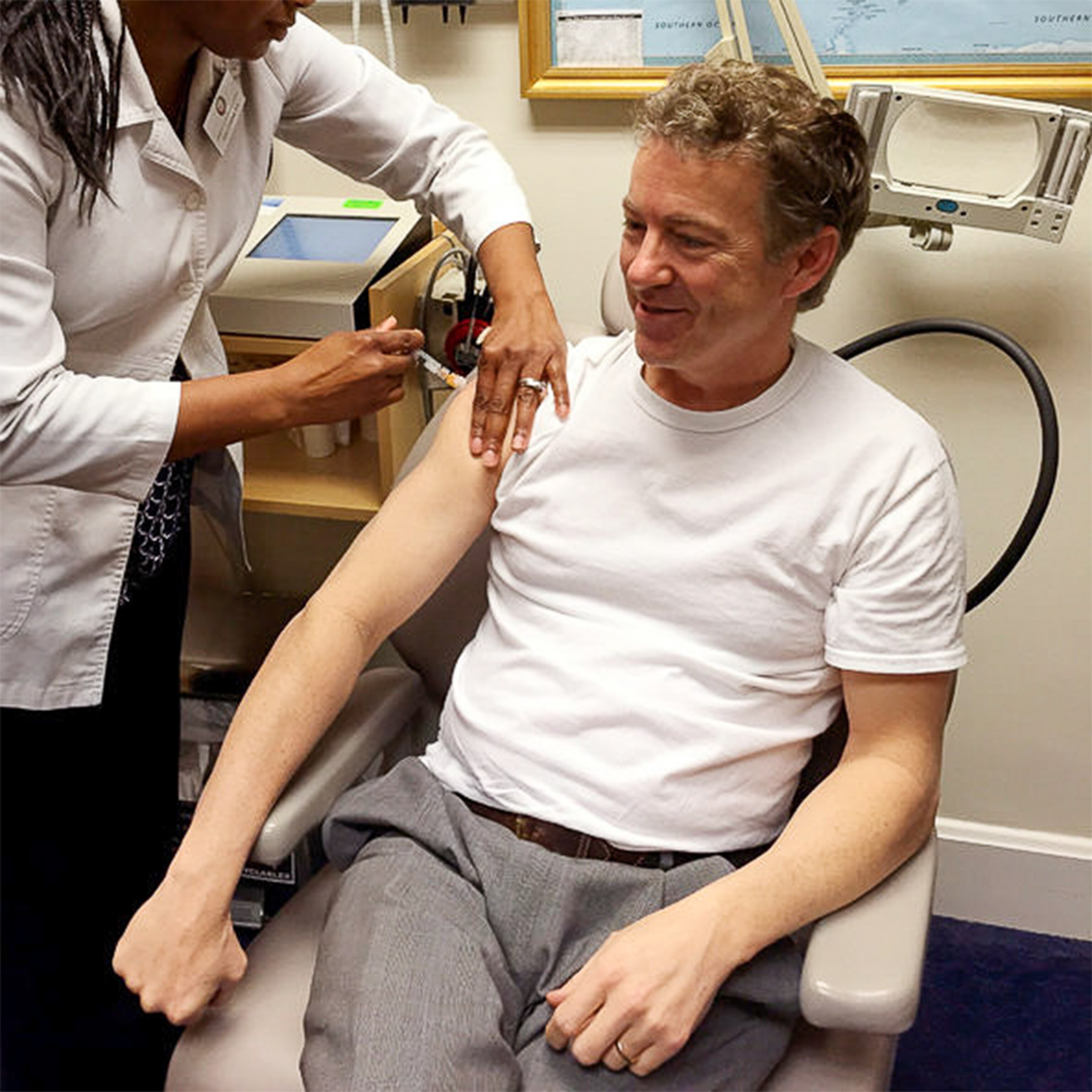
Even though both men quickly revised their remarks in the uproar that followed—and Paul was photographed getting vaccinated for hepatitis A—their comments moved the topic of vaccine safety out of the fringes and firmly into the arena of presidential politics. Both men are considering running for the Republican nomination in 2016.
Their remarks—and the broader vaccination debate that's followed the measles outbreak that began in California in December—have been a wake-up call for many doctors and scientists who work on the front lines of infectious disease outbreaks. They have watched with growing unease as the anti-vaccination movement has gained voice.
"Chris Christie has a state law requiring car seats for children," says Paul Offit, a University of Pennsylvania pediatrics professor and director of the Vaccine Education Center at Children's Hospital of Philadelphia. "Why isn't that a matter of parental choice? This is a dangerous game to play."
Misinformation and Mistrust
How childhood immunization—once a given—crossed the divide from breakthrough science to public policy debate in the space of 50 years is a complicated picture. But it is rooted in distrust of government and science.
Stir together an even more intense distrust of Big Pharma—the multinational pharmaceutical companies that manufacture vaccines—the Internet as an incubator for misinformation like the now-discredited theories linking vaccines to autism, and celebrity activism that turns small causes into bigger ones.
Then add the rise of citizen science-which has activists doing their own research-and grassroots movements focused on holistic lifestyles, and you are left with the distilled essence of parents who are skeptical and politicians who see opportunity.
We have become prisoners of our own success. Nobody knows what measles is.
But it's unlikely these elements would have come together and flourished if Americans had not become so utterly unfamiliar with the diseases of Christie's and Paul's childhoods. (Get answers to your questions about measles and vaccinations.)
"We have become prisoners of our own success," says William Schaffner, who chairs the department of preventive medicine at Vanderbilt University in Nashville, Tennessee. "Nobody knows what measles is.
"We now have two generations who haven't seen measles," he says. "The mothers were vaccinated. They never saw measles. Their mothers—the grandmothers—barely saw measles themselves. So the grandmother has no influence. The mother is clueless and so the child goes unvaccinated."
A few years ago, Schaffner was invited to speak to a group of 20 young mothers who had reservations about vaccine safety. His task was to educate, not argue, so he began by talking about polio and the vaccine developed in 1954 that practically eradicated it. He had barely begun speaking when one mother, looking confused, blurted out: "Why are you now talking about shirts?"
"She was bright, college educated, computer savvy, and she'd never encountered the concept of polio. She instead mixed it up with Ralph Lauren," Schaffner says. "It's a bit humorous, a bit tragic, and illustrative of the problem today."
A Natural History of Measles
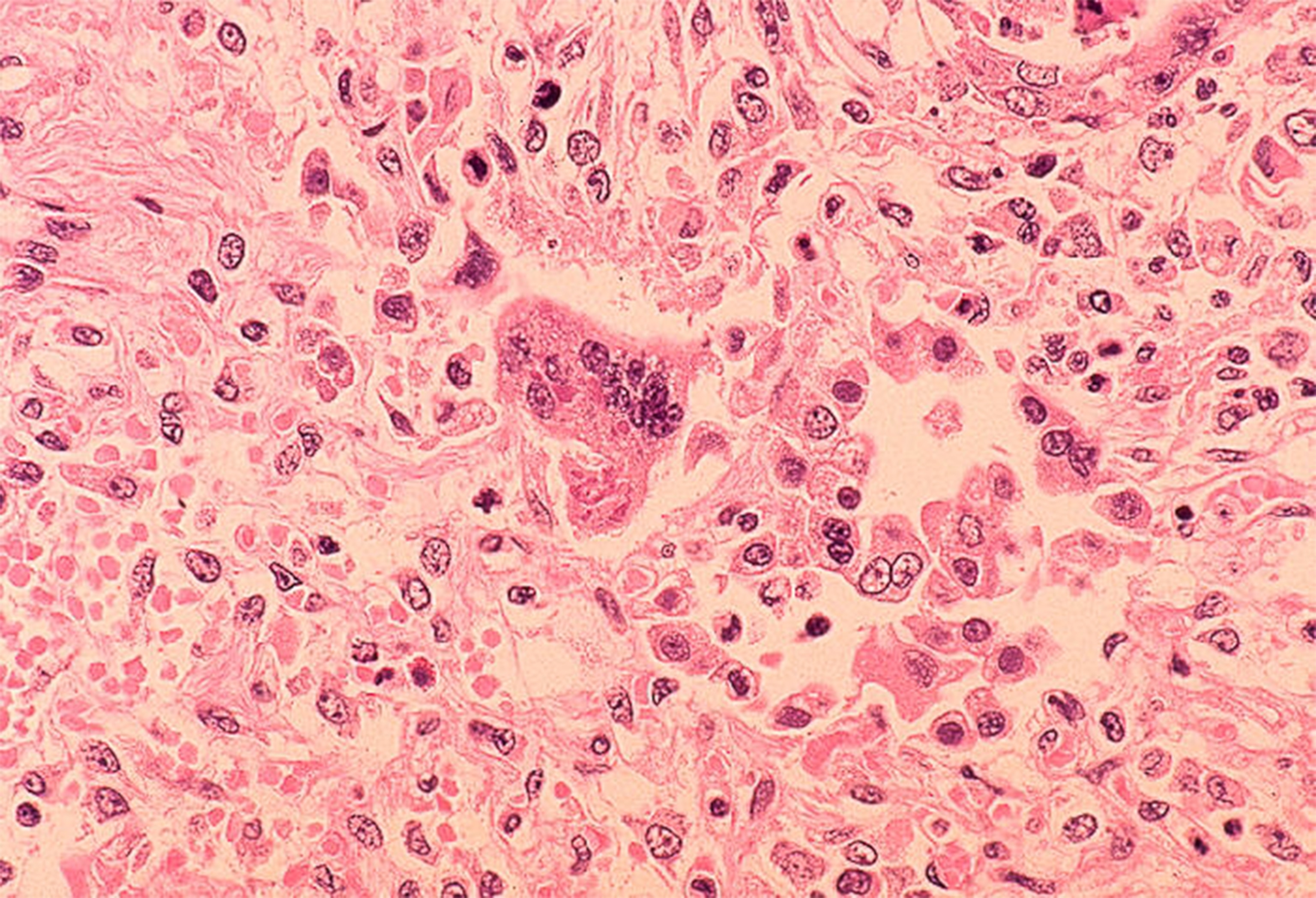
Schaffner calls measles "the most infectious disease doctors know." It's an airborne illness, transmitted with stunning efficiency when an infected person exhales. Unlike the flu, which requires close proximity for transmission, measles can be spread over time and distance.

"An infected person can walk into a room and leave the room, and a susceptible person can walk into the same room an hour or two hours later and breathe in the residual air in the room and become infected," Schaffner says. (Learn more about how measles spread.)
In the early part of the 20th century, measles was so common it was considered a rite of childhood. But it was not innocuous. Not only could it be fatal, complications included encephalitis. After the vaccine was licensed in 1963, some 19 million children were immunized over the next dozen years, according to the Centers for Disease Control and Prevention in Atlanta.
The only country that now has measles transmission in the Western Hemisphere is the U.S.
By 2000, the CDC declared measles eradicated in the United States. By 2011, the Pan American Health Organization announced that measles had been eliminated from Latin America.
"Talk about stunning," Schaffner says. "We have no measles upriver on the Amazon. None in Chile, Nicaragua, Mexico. The only country that now has measles transmission in the Western Hemisphere is the U.S.
"You see on the Internet [people] worrying about illegal immigrants causing the outbreak we're seeing now," he says. "Hey, they're doing a better job than we are. We have these upper-middle-class parents of means in the U.S. who have decided they don't want to vaccinate their kids."
Turning Points
Although the conquest of polio became the turning point in the battle against infectious diseases, the measles vaccine provided the foundation for the national immunization program that exists today.
"Polio is far less contagious, so victory was achieved pretty quickly," says Walter Orenstein, associate director at Emory University's vaccine center in Atlanta. "With measles, it took a while, because of the immunity levels we needed to achieve to stop transmission of it and the problems with getting access to the vaccine for poor children."

Because measles was so infectious, controlling its spread meant vaccinating huge numbers of children, which before the late 1960s had never been done on such a vast scale. The big breakthroughs came in the 1960s and 1970s, when public health officials in Rhode Island first tested the effectiveness of "herd immunization." Schaffner, then working for the CDC, documented the effort in a study that proved conclusively that measles could be eliminated by comprehensively immunizing children.
Next came the "no shots, no school" policy that eventually became law in all 50 states. An outbreak in Los Angeles prompted officials to send unvaccinated children home, with instructions to not return until they'd had their shots.
Public health officials took note. "They said, 'Why wait for an outbreak? Why not just insist that every kid who comes to school be vaccinated?'" Schaffner says.
It took about a decade, but today, all 50 states have laws requiring vaccination for school children. All 50 states also allow medical exemptions for children with diseases whose health could be compromised by vaccinations.
Religious exemptions are allowed in every state except Mississippi and West Virginia, according to the National Conference of State Legislatures. Among states allowing religious exemptions, 20 also allow exemptions for personal or moral beliefs.
Applications for exemptions are on the rise, as are proposals by legislators to ease restrictions. Even in Mississippi, a poor state with the toughest restrictions, lawmakers are considering a proposal to allow exemptions for "conscientious beliefs."
As the investigation of the outbreak that began in December at Disneyland spread from California to 13 additional states, Orenstein, the Emory physician, cautioned against the false notion that outbreaks affect only the unvaccinated.
"One thing that has not been made clear to the public is that an outbreak of a vaccine-preventable disease doesn't only affect the people who are unvaccinated," he says. "There are also costs to taxpayers involved in controlling an outbreak."
A Rash of Misinformation
The defining moment that gave momentum to the anti-vax movement came in 1998, when a British gastroenterologist named Andrew Wakefield held a press conference in London and linked the measles vaccine to rise of autism.
Wakefield's research, published that year in the respected British medical journal the Lancet, has since been discredited and retracted by the journal. Wakefield subsequently lost his medical license.

Even so, in the aftermath of the episode, vaccination rates dropped in Britain and Western Europe, and his theory lived on in Internet chat rooms and among believers of the anti-vax movement. Many are highly educated professionals, who trust their own shared research over the findings of mainstream medicine.
Their distrust of vaccines is informed not by political ideology—they come from both sides of the aisle—but more often by a sense that conventional medicine has failed them. Some want to pick and choose which vaccines their children will receive; others object to the schedule many school districts have set for immunizations.
In the United States, vaccination rates have not declined, even as requests for exemptions increase. Because of this, the chance of getting measles in the United States is still infinitesimally small, even for those not immunized. So, what's the risk?
The danger, scientists say, lies beneath the broad national statistics in pockets around the country where like-minded anti-vax parents are clustered.
In 1991, a measles outbreak in Philadelphia that spread to more than 1,500 children and killed nine, began in private schools run by two fundamentalist churches whose 350 students had never been immunized.
"You see today the rights of the individual trump the good of society," the Vaccine Education Center's Offit says. "We crossed that line in Philadelphia in 1991. This city was in a panic."

Today, pockets of unvaccinated children are scattered across the nation, especially, Schaffner says, in California, Washington, Oregon, and Utah. This week, for example, the Los Angeles Times reported a 51 percent rate of unvaccinated children in a preschool in Santa Monica.
Washington State has the highest rates of school vaccine exemptions in the country; some elementary schools there have an exemption rate of 43 percent. Paul Throne, a spokesperson for the Washington State Health Department's immunization office, says the state's overall vaccination rate remains high.
In 2011, the state tightened the rules regarding exemptions. Parents seeking an exemption are required to confer with a physician to learn about the benefits of vaccinations and risks of forgoing them. Now, instead of merely signing a form, parents must invest as much effort to obtain an exemption as they invest in vaccinating their children. "I do think we've seen some headway," Throne says.
The state is also training a network of parents to educate their friends about immunization. "Health care providers don't carry as much weight now as friends and family do," he says. "The millennials have a lot of confidence in their ability to interpret information. So we're training them to take these conversations to their peer networks. That's the place where people make decisions."
Follow Laura Parker on Twitter.