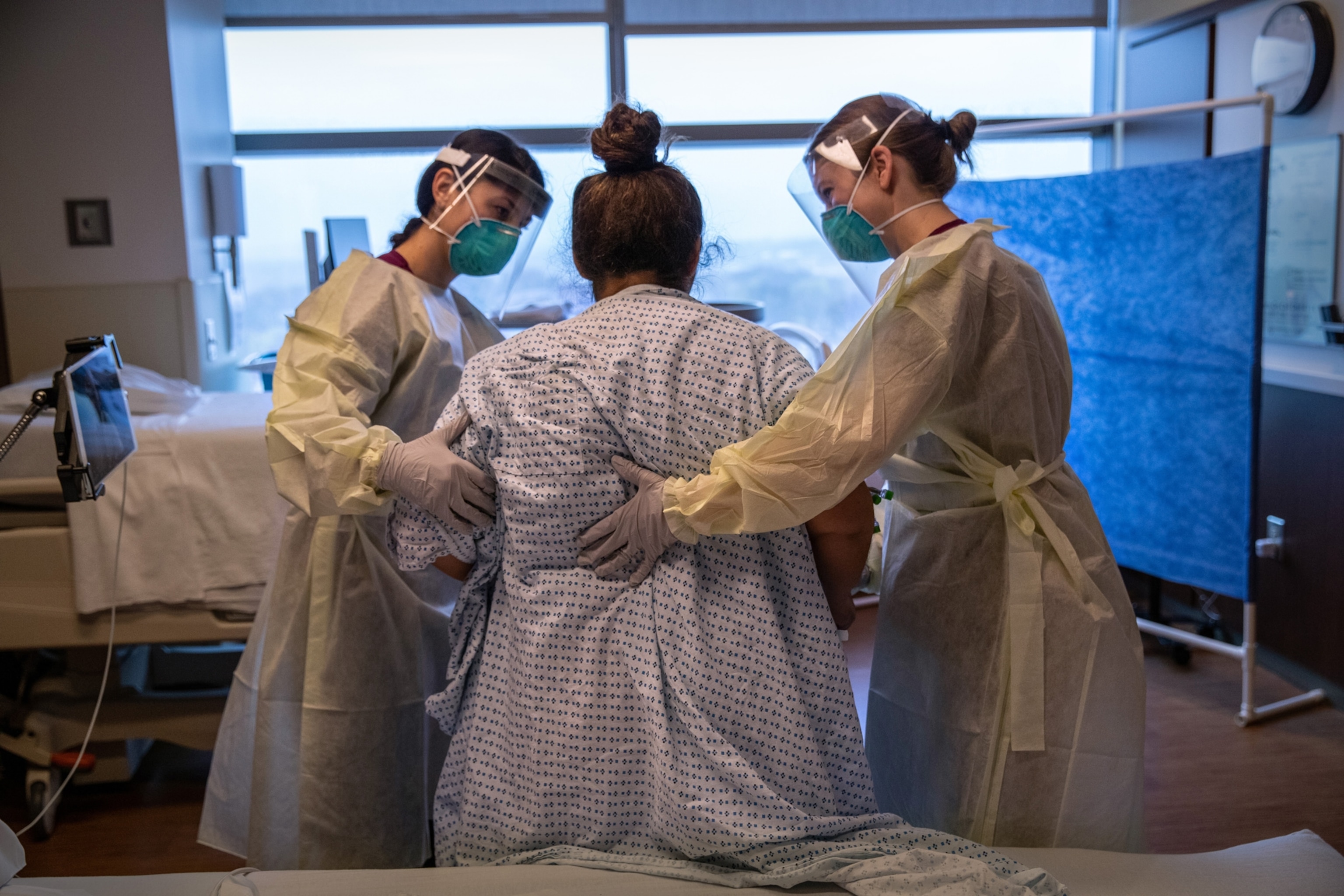
The pandemic highlights why women need better doctors
Many women rely on specialists rather than primary care providers, and now the pandemic is cutting access to those specialists. A new report outlines what’s needed to fix the system in the United States.
“Not applicable.” That’s how Devon Anderson replies on forms asking about her primary care doctor. The 38-year-old dropped her primary care physician four years ago, after she experienced problems getting diagnosed properly and the relationship deteriorated.
“Every single time I saw her, her answer was meds for pain or meds for infection, but I knew something was going on,” says Anderson, who lives in Canton, Ohio. Eventually, her gynecologist referred her to a urogynecologist, where she was diagnosed with interstitial cystitis, a chronic condition that causes bladder pain. Now, she sees her gynecologist for most of her referrals.
Anderson represents a growing trend of adults under the age of 60 without a primary care provider, according to a 2019 study in JAMA Internal Medicine. Like Anderson, many women instead perceive their gynecologists as their primary care providers. Many women only enter the health-care system after having a baby, leaving many more falling through the cracks of a fragmented system—one where maternal health care, women’s health, and primary health care tend to be disconnected.
The COVID-19 pandemic has thrown the system’s flaws into sharper relief. Before the pandemic, 54 percent of all patient visits were with specialists, including cardiologists, oncologists, and gynecologists. Now, access to such specialists may be delayed or limited due to pandemic-related restrictions—a particular concern for women, who rely more on specialists for their broader health-care needs.
A new report by the Commonwealth Fund, which focuses on improving health-care access particularly for society’s most vulnerable people, details how the splintered model of care in the U.S. affects women’s health. The report also describes what a suitable, comprehensive system that responds to women’s needs should look like.
A fundamental flaw, the report says, is how the U.S. health-care system prioritizes intervention over prevention. A primary provider can monitor multiple, ongoing conditions and develop a care relationship with women over time, whereas specialists usually only address particular needs. As a result, about half of American women do not receive the attention to preventive medicine that they need, says Laurie Zephyrin, vice president of Delivery System Reform at the Commonwealth Fund and a co-author of the report.
“It's supposed to be the front door into the health-care system. The primary health-care team should be the one helping address people’s health care, social, and mental health needs,” she says. “Unfortunately, in the United States compared to other similarly wealthy countries, we invest the least in primary health care, and our primary health-care providers aren't reimbursed to the level of specialists.”
Barriers to care
The Commonwealth Fund report outlines a few of the major barriers to improving women’s health care, starting with basic access. According to the American Academy of Family Physicians, an estimated 130,000 deaths in the U.S. could be prevented each year by improving primary health-care access.
“When we look at primary health care—particularly, primary care providers who work in communities of color—there are shortages in many areas whether it's in urban communities or rural communities,” says Zephyrin.
Proper screening for breast cancer and chlamydia could save the lives of 3,700 women and prevent 30,000 cases of pelvic inflammatory disease, a serious condition that can cause infertility or chronic pain.
Areas with fewer primary care providers recorded higher rates of cancer mortality, heart disease, and hospitalizations among all genders, and access to women’s care can face additional setbacks. Research estimates that proper screening for breast cancer and chlamydia could save the lives of 3,700 women and prevent 30,000 cases of pelvic inflammatory disease, a serious condition that can cause infertility or chronic pain.
Often, though, people who provide primary health care don't feel comfortable with treating women’s specialized needs, specifically in regards to sexual well-being, sexual health, menstrual health, says Sirina Keesara, director of Women’s Health at West Oakland Health in Oakland, California. “Women are sent to reproductive health specialists for women’s sex-specific primary health care, like pap smears and mammograms,” says Keesara.
Overall, medical education does not focus on gender-specific needs, the Commonwealth Fund report says, and “there is poor awareness of the sex differences in disease progression and treatment and a lack of awareness of pivotal health experiences that women encounter.”
The social role
Medical training also fails to equip physicians to address the social needs of their patients, even though about 80 percent of doctors believe it's important to do so. “Social factors serve as huge barriers to care. Transportation and childcare are two major barriers that prevent people from coming in to get the care they need,” Keesara says.
Women, in general, are often tasked with the unpaid labor of caregiving and caring for the household. Black women are also more likely than white and Hispanic mothers to be the main source of income for their family, according to analysis from the Center for American Progress. These combined obligations often delay women in seeking care for themselves.
Even when regular, preventive health care is available and accessible, women of color may still be less likely to use it because of cultural reasons. Language barriers, discriminatory experiences, and an overall mistrust of the health-care system among Hispanic, Black, and Native American women are also associated with lower use of preventive health services among these groups.
As a consequence of these various barriers for women of color, combined with institutional racism in health care, Black women are less likely to get earlier-stage breast cancer detection and are more likely to die from the disease; Hispanic women are less likely to get pap smears and mammograms and more likely than white non-Hispanic women to die from cervical cancer; and Black and Native American women are two to three times more likely to die from pregnancy and childbirth-related causes.
“There's definitely been a lot of conversations involving maternity care, and compared to other similar countries, our maternal health and well-being outcomes are worse,” says Zephyrin.
There must be relationships, trust, and an investment in the lives of women beyond the doctor’s office.Barbara Jones, Northside Peachtree Corners Primary Care
A new vision for primary care
A comprehensive primary health-care system is one that “delivers accessible and high-quality services that are prevention-focused, integrated with behavioral health care and social services, equitable, and effective,” Zephyrin and colleagues write in the Commonwealth Fund report. That means access to insurance or affordability shouldn’t determine the quality of care, and preventive medicine should be coordinated among culturally competent providers of physical and behavioral health, as well as social services.
To be truly comprehensive and improve the health of women, Barbara Jones says there must be relationships, trust, and an investment in the lives of women beyond the doctor’s office. Jones, a family medicine physician at Northside Peachtree Corners Primary Care in Peachtree Corners, Georgia, says home dynamics are among the most significant indicators of whether a patient can improve their health. Patients struggle to reverse high blood pressure and diabetes, for example, when they experience chronic stress due to their living situations. The Commonwealth Fund report similarly argues for tailored doctor visits that focus not only on the patient's individual medical history but also on their socioeconomic needs such as housing, food access, and safety from violence.
One way to work toward this is to integrate social workers and community health workers to create a team of providers who can follow up on the needs of patients. At Keesara’s clinic in Oakland, California, they use what are called panel managers. These individuals review patient information and conduct follow-up calls for patients who’ve had gaps in care to connect them, as needed, with social resources such as substance abuse centers and housing information.
Primary health care should also center on disease prevention and not just treatment, the report says. Zephyrin envisions women’s health care as a continuous relationship with a warm handoff during transitions to specialists as needed—a model of care where health does not ignore the community but is integrated into it and co-designed by the women who live there.
Even with these kinds of systemic changes, Devon Anderson says the culture of medicine needs to value women’s voices and make them feel like they’re not alone before she will return to a primary care provider. For now, Anderson says she'll continue utilizing her gynecologist as a primary care physician.
"That won't change for me unless I find a primary care provider that doesn't make me feel like a bother."