
The Secret Lives of Cadavers
How lifeless bodies become life-saving tools.
William and Mary Figel were the kind of American couple that now exists only in black-and-white television shows. They met in the summer of 1952 at Rainbow Beach Park on Chicago’s 75th Street. He asked for her number; she told him it was in the phone book. They married the following January and eventually had four children.
In February 1983, William, then 53, was ready to take early retirement from Science Research Associates, an IBM subsidiary where he worked as a computer programmer. William predicted that computers would become a staple of every American home, with one in every room, like television. He dreamed of running his own neighborhood computer store, one where cigar smoking would be allowed.
But that dream seemed far away the winter day when he and Mary and their son Bill sped around Lake Michigan to Columbus Hospital. An aneurysm in William’s brain had triggered a stroke. The next morning, he couldn’t speak or move the right side of his body.
William came home from the hospital about a year later. He refused help with the porch steps and the stairs to his bedroom, gripping the railings with his working left hand. For the next 30 years he worked hard on physical and speech therapy. He learned 25 words and could say “I love you” in a way others could understand. But he never used a computer again.
The Figels’ son Bill and his wife, Kathy, moved five houses down. During summers their kids would take hamburgers, hot dogs, and chicken legs to their grandparents. Sometimes they’d come back with cookies.

By 2010 William was in hospice care in Peoria, Illinois, and Mary was showing serious signs of dementia. During one terrifying lapse she drove her car through the South Side Irish parade. Miraculously, no one was hurt.
That’s about the time Bill Figel broached the subject of body donation with his father. He’d remembered an article he’d read in college about the brain’s ability to heal itself after a stroke. Perhaps his father’s brain held important clues to the process, he thought. Bill made some calls and consulted his siblings, then presented the idea to his father.
“It wasn’t a tough sell,” Figel recalls. His father decided to donate his body to Loyola University, his alma mater where he’d earned three degrees. His mother followed her husband’s example.
William Figel Sr. died on September 8, 2011. Mary Figel followed the next month. She had cancer, but nobody had known. Stritch School of Medicine at Loyola University took both of their bodies and sent them on a seldom traveled path.
There are more than 120 million registered organ donors in the United States, and an average of 79 people receive transplants each day, according to the U.S. Department of Health and Human Services. The federal government does not monitor whole body donations in the United States, but researchers estimate each year fewer than 20,000 Americans donate their bodies to medical research and training. While organ donation is a point of pride, body donation is often stigmatized.
Most people have only a vague notion of what “body donation” even means. The thought alone frightens, or even disgusts, many people. And scandals involving the illegal sale of body parts, and other snafus, have inspired distrust in body donation programs.
But a closer look reveals the process as both strange and wonderful, clinical and deeply human. A donated organ can save a life, but a body provides the foundation to save many more.
Teaching Doctors to Heal
Cadavers lead all sorts of interesting lives. They allow doctors to practice on patients who don’t feel pain. They help surgeons develop new procedures without risking lives. Dentists dissect their heads and torsos, and physical therapists study their musculoskeletal systems. Pharmaceutical companies test drugs on them, and automakers employ them as crash-test dummies. At the University of Tennessee's Forensic Anthropology Center—nicknamed “the Body Farm”—CSI teams learn how corpses decompose over time. But the majority of cadavers teach.

Nearly all medical students in America begin their education by disassembling a human body. They spend weeks on a task that may disturb or give them nightmares, but most students are mesmerized by the body’s astonishing complexity.
Anatomy class is a rite of passage for all aspiring doctors, and body donors become their first patients. Active learning in the lab is the foundation of every treatment and diagnosis the future physicians will render. A dead body can become a life-saving tool down the road.
“What we’re really trying to do is teach them what’s under the skin,” says Neal Rubinstein, associate professor of cell and developmental biology at Perelman School of Medicine at the University of Pennsylvania. “Most physicians don’t cut into a body when they’re practicing medicine, but they have to know what’s underneath if they stick a needle here or there. Almost every physician needs to have a good three-dimensional picture of the body in their head.”
Trudy Van Houten, director of Clinical Anatomy at Harvard Medical School, says when doctors examine patients, “it’s that mental map that guides their fingers. What dissection gives them is an idea of how deep things are. You can’t get that from a picture.”
Demand Up, Donations Down
Though no dependable national statistics exist, numbers from individual agencies indicate that the body donor pool is shrinking. The Anatomical Gift Association of Illinois, for instance, has seen annual donations fall from 760 in 1984 to 520 last year. Yet the need for cadavers has never been greater.
First-year medical school enrollment is projected to reach 21,304 by 2019-2020, a 29.2 percent increase over enrollment in 2002–03, according to a report from the Association of American Medical Colleges. (For the sake of effective hands-on learning, most medical schools allot one cadaver to every four to six students.) The expansion of physician assistant and nurse practitioner programs further strains supply.
The use of cadavers outside medical schools is also increasing. Michel Anteby, associate professor at Boston University’s Questrom School of Business, published an article in 2009 in the newsletter Economic Sociology analyzing supply and demand for cadavers in the U.S. The report, titled “A Market for Human Cadavers in All but Name?,” found that the appearance of independent ventures such as Science Care and the Anatomy Gifts Registry—nonacademic programs that accept tissue and whole body donations for research—had increased competition for bodies. Like contractors, the programs send bodies where they’re needed and collect on the cost of preservation and transportation.
Human remains cannot be legally bought and sold in the U.S., but independent ventures can provide financial incentives for donors that many schools can’t offer, such as picking up a body for free. Medical schools often ask that families pay for a funeral home to deliver the donated body.
Some schools are hit hard by the lack of cadavers, while others are unaffected. In 2008, Colorado and Wyoming were 20 bodies short of the 158 cadavers requested by the states’ medical schools. Half of Canadian medical schools have cut back on using cadavers, relying instead on new technology to make teaching basic anatomy more efficient. In the Middle East and Caribbean, medical schools routinely ship in cadavers from all over the world.
From Death to Dissection
For donors William and Mary Figel, the road to Loyola University led first to the Anatomical Gift Association of Illinois, which procures, preserves, and distributes donated bodies to most of the state’s medical schools. Tucked in an alleyway in the Illinois Medical District, which encompasses four major hospitals, the innocuous-looking white building is easy to miss.
Inside, director Paul Dudek opens a colossal metal door with a sign reading BIOHAZARD in bright red letters. “These are our embalming areas,” he says. Rigid bodies lie on steel gurneys covered by white sheets. Rubber tubes drip a murky chemical concoction into them from plastic cylinders fastened to the ceiling.
The “waiting room” is down the hall. There, funeral directors from across Illinois deliver bodies through the back door to a refrigerator filled with unembalmed cadavers. The AGA usually gets one or two bodies a day.
In another even larger room, hundreds of cadavers rest on metal shelving units, ready for delivery: 85 to the University of Chicago's Pritzker School of Medicine, 130 to Northwestern University's Feinberg School of Medicine, 150 to Midwestern University's Chicago College of Osteopathic Medicine.
Dudek, a short man with gray hair and sympathetic, intelligent eyes, grew up around medicine. His father was a surgeon at Holy Cross Hospital in Marquette Park on Chicago’s Southwest Side. His mother kept a tarp rolled behind the couch for impromptu surgeries in the living room.
“At 2, 3, 4 o’clock in the morning, people would be crawling up the front stairs—somebody had a heart attack, somebody fell down the stairs, somebody got beat up, somebody got stabbed,” Dudek says.
As a University of Chicago grad student studying the history of medicine, Dudek worked weekends and nights as a research tech in the Department of Surgery.
Dudek says body donation always begins with a call—from people in nursing homes who say they want to give something back, to confused families who’ve found donor documents after a relative dies. A small number call because they don’t have enough money for a funeral.
“I explain the situation, and if they decide they don’t want to donate, I don’t want to push them,” he says. In the U.S., about 130 body donation programs are affiliated with universities, and there are a handful of independent programs. Donor forms are often only a page long and are not legally binding.
Speed is critical after death. The body must be refrigerated before it starts decomposing, usually within 24 hours. In most cases, the family must make arrangements with a funeral director to transport the body and death certificate to the donation facility, where the remains are tested for infectious diseases, such as hepatitis and HIV/AIDS, before embalming.

Funeral director Steve Shimkus stands in a concrete room, shelves lined with plastinated brains and chemicals for embalming. Turning a cadaver’s head to the left, he cuts along the collarbone. The skin splits to reveal a yellow layer of fat, which he snips away with surgical scissors.
“I want to raise the artery, and I want to do it without breaking the vein,” he says. “When you die, blood settles in your veins. If I nicked it, it wouldn’t squirt, but it would ooze and bloody up the field so I couldn’t see what I’m doing.”
Shimkus pulls on the carotid artery and stretches it like a thick white rubber band. He slides a metal hook under it to bring it to the surface. He cuts and inserts a tube into the artery’s reddish inside, securing it with a clamp. Shimkus, a former firefighter and EMT, is strongly built, broad shouldered and shaved bald, with a gray, wispy moustache nested beneath his nose.
The pump hanging from the ceiling sputters. A solution of water and preservatives rushes toward the head in a high-pressure jet. Then, a supernatural transformation begins. Veins leap from the cadaver’s temple, and the stretching skin changes from flesh-toned to purple to patches of ghostly white, bleaching from a chemical called phenol.
“I like to call this embalming for dummies,” he says. Shimkus is a veteran funeral director who can make the victim of a car accident look normal again. He does delicate work; preparing cadavers is quick and dirty.
“You’re not setting features, you’re not gonna’ make ‘em look nice,” he says. “You’re raising your artery, and it’s pretty much you’re plugging ‘em in and walking away, listening for the machine. When the machine kicks up, you know it’s empty, and you go refill it. There’s really nothing to it.”
Shimkus directs the solution’s flow toward the feet. “Now we’re going down,” he says.

Shimkus strains to push the cadaver, now 125 pounds heavier, across the room, where he connects it to a five-gallon drip for the weekend.
A cadaver settles over the three months after embalming, dehydrating to a normal size. By the time it’s finished, it could last up to six years without decay. The face and hands are wrapped in black plastic to prevent them from drying, an eerie sight for medical students on their first day in the lab.
An embalmed person loses his or her identity. Donations are anonymous, and students won’t know who a cadaver was. The face is swollen, the head is shaved, and depending on the cocktail of chemicals and dyes pumped into it, the flesh turns yellow, green, red, or gray. The most important difference is inside.
In the Anatomy Lab
A hush comes over the University of Chicago anatomy lab, a long room with windows at the back and large swinging metal doors at the front. The door goes to the locker rooms where the students change into their scrubs. There are rows of dissection tables in the lab and next to them, stained anatomy books and carts with scalpels and stained anatomy books.
Eighty-eight medical students crowd around the body of an elderly woman. Pathology Professor Tony Montag holds the cadaver’s uterus in his hand. It is as hard as a stone. Montag explains that after a cancerous tumor had killed the uterine tissue, it calcified. The students whisper.
“Could she feel it?” one student says.
“It’s visceral, so not at first,” says a second. “But as it expands, it gets heavier.”
The first nods in agreement.
Callum Ross, a professor in the Department of Organismal Biology and Anatomy, watches and smiles. He’s a lanky, whimsical man with an uncanny ability to pluck a floss-like nerve or blood vessel from some cadaver’s dark crevice without hesitation.
“I try not to organize them too much—I like them to self-organize,” he explains. “The anatomy lab is a place where they can explore and find things out and try different things. It’s a great learning environment, and I like to let that evolve organically.”
Gross anatomy—which deals with structures visible to the naked eye—is daunting. This class runs five days a week, beginning with lectures and ending with three hours in the lab. The students memorize thousands of terms, take 19 exams, and read a 500-page textbook.

Matt Present points to the whiteboard, where the 12 cranial nerves are drawn in blue and red with a Sharpie, labeled by a roman numeral and a letter: S, for afferent sensory nerves, which send signals to the brain; M, for efferent motor nerves, which carry messages from the brain; and B, for nerves that do both. A mnemonic phrase is scrawled at the bottom of the board: “Some say marry money but my brother says big brains matter more.”
The students huddle over a body in groups of four, each taking a quadrant. The teaching assistants roam the lab, stopping to ask students for the function and definition of a bone or muscle. Others squint at grainy CT images, trying to discern one organ slice from another.
“I was here until midnight studying bones,” first-year medical student Herman Luther says. He holds a plastic skull in his hand, quizzing another student, Lauren Glick, for an osteology exam. The skullcap of the cadaver they stand next to was removed, its brain in a container on the floor. Two thick and purple optic nerves snake crossed over the pea-size pituitary gland, a sort of control center for the endocrine system that rests beneath the brain. The gland is the combustion engine of thought and feeling, and the students are technicians studying a beautiful machine.
Glick explains that if a tumor grows on the pituitary gland, it presses against the two nerves, causing headaches and tunnel vision. Same as the woman with a hardened uterus, the students think of their cadaver in terms of a living person.
Bodies of Knowledge
Dissection is costly and time-consuming. At most medical schools, gross anatomy courses last 100 hours, three times the length of most first-year courses. To comply with U.S. Occupational Safety and Health Administration guidelines for formaldehyde levels, which are as low as two parts per million, schools install expensive ventilation systems. Last year, Perelman School of Medicine at the University of Pennsylvania spent $1.5 million updating its ventilation system, Rubinstein says.
Over the past 30 years, tech companies have attempted to replace the cadaver. There’s the Anatomage Table, a stretcher-size screen on wheels displaying a digital body that students can virtually dissect. The biomedical company SynDaver Labs, featured on the ABC show Shark Tank, makes mechanical cadavers that can bleed, scream, stop breathing, and even “die.” Some schools use bodies that are plastinated—preserved using a process where synthetic compounds replace water and fat to prevent decay.
“When you think about it, what’s really important for most physicians is surface anatomy,” says Joel Lanphear, interim senior associate dean of Academic Affairs at Central Michigan University. “We have tremendous simulation devices that will simulate physiological conditions and that will generate the same level of emotion among a group of students who are a team on a mannequin that is beginning to die on them as they work on them. Those experiences can be had.”
Lanphear has been an administrator at medical schools around the world, from Texas to Ontario to Dubai. At his schools, students learn anatomy by looking at prosections, dissections done by skilled anatomists. That way, an entire class can learn with only one body, studying one organ system at a time.
“What was there was a very well dissected, clearly understandable specimen for the students to learn from,” he says. “When bodies are dissected by nonexperts, sometimes what is supposed to be seen or understood is more difficult to do because the site is not as clearly created by a student.”
Ross scoffs when asked if prosections can stand in for dissection. “I don’t think they understand what they’re talking about,” he says. “Do you want to be treated by a doctor who hasn’t dissected somebody?”
In anatomy, students learn to work in groups like doctors do. Each body is both dazzlingly different yet surprisingly similar, and Ross says that it’s very important for them to understand that each person they treat could present a surprise.
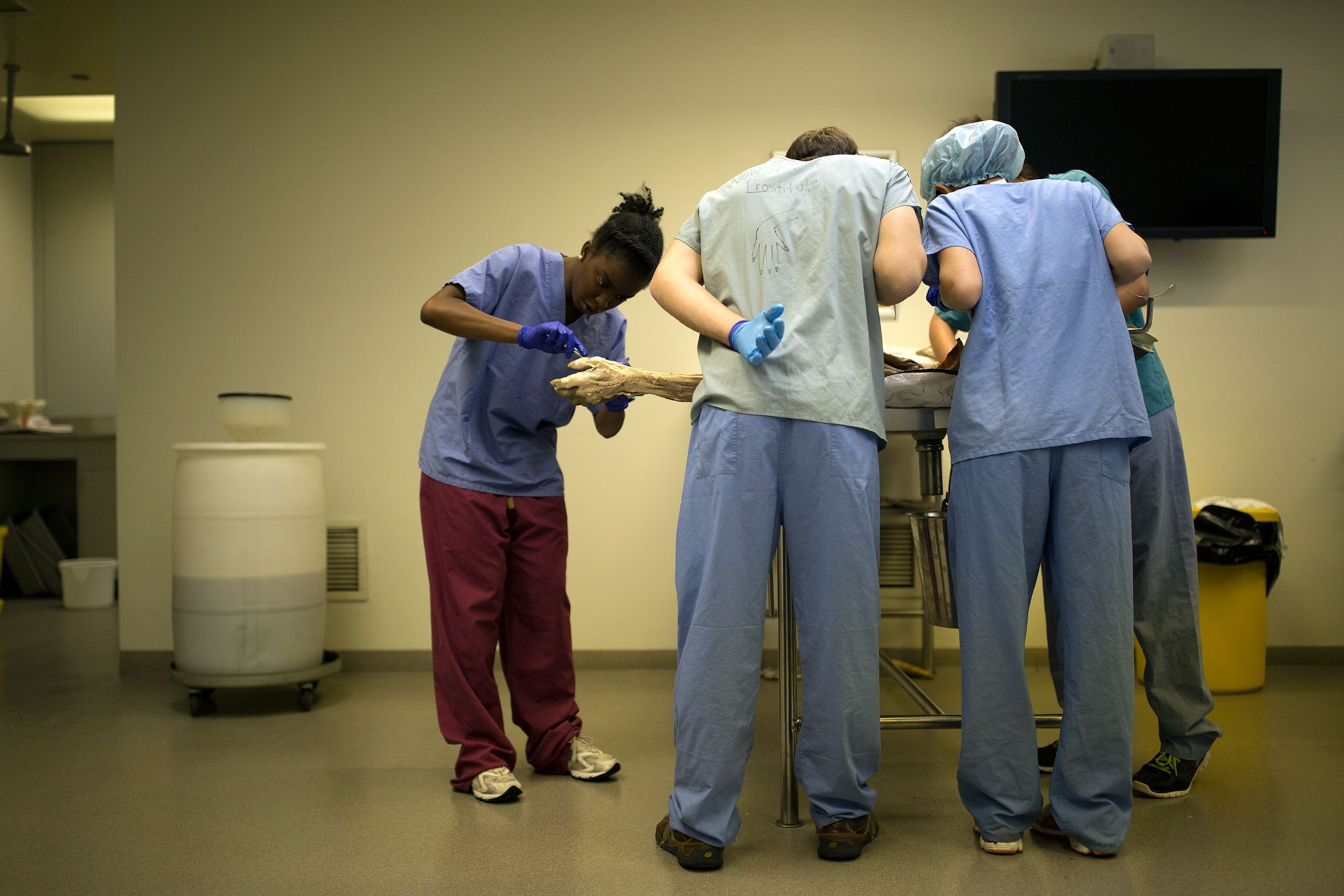
One cadaver’s brain had forced its way into connective tissue in the skull after a massive stroke had killed the person. Another cadaver had a tumor that had spread from the mouth up through the eye and into the brain.
“You could pass a probe through a hole in the side of this person’s face all the way up into their brain,” Ross says. “They had this cancer long enough that it had all scarred over on the outside. They’d been living like this. So the question came up, ‘In what circumstance would a person get into this situation? What was it like?’ You discover things when you dissect people that you can’t discover if it’s 25 bodies on a computer. You don’t find all this randomness, and you can’t ask these questions.”
While some medical imaging programs have variation and pathology built in, Ross says it’s impossible to re-create the actual experience.
“That’s pie in the sky,” he says. “It’s physically interacting with the things. Putting your hands inside them and taking them apart. You learn stuff when you hold the heart in your hand … I think it’s this gee-whiz thing people have with technology. Here’s some old technology: Dead people, dissection tools, and a bunch of great instructors and TAs and a bunch of smart, motivated young people. Put 'em in a room and they’ll learn.”
At Harvard, students begin with virtual anatomy, but that learning is only a prelude to the lab. They put their first IV in a cadaver, a patient who will not hurt. They practice appendectomies—procedures done 280,000 times each year in the U.S.—on cadavers. Then surgical residents are sent back to the lab to study the anatomy again. At the end of the class, students present their cadavers to a pathologist. Unlike in an anatomical drawing, the insides are not color-coded. They are messy and monochrome.
“The human body is still the best three-dimensional model we have,” Van Houten says. “It can look innovative to switch to virtual anatomy teaching, but you can be really innovative teaching in the gross anatomy lab.”
Back at the University of Chicago, medical student Michael Fishman, known as “Fish,” traces a nerve on a skinless arm with his gloved hand. The brachial plexus runs all the way down the arm and dives into the muscles in small branches. Fishman raises it like a grass root from the ground. Without the brachial plexus, movement and feeling in the arms and hands would be impossible.
“As it goes down, the branches innervate the muscle, and then it goes down to the thumb over here,” he says. If you fall asleep with your arm hanging over a chair, the nerve gets compressed against the humerus, and it can die. It’s called Saturday Night Palsy.
“We call it Boat Cruise Palsy because the whole class goes on a boat cruise [at the end of the course] and they all get ...” Ross paused. “Look it up.”
A Meaningful Way to Die
When Bill Figel was a young child, his family rented a cottage on Lake Michigan. His father, the late William Sr., once walked into the water and swam far from view into the sunset. Figel lost sight of him and panicked, but his mother was too far away to hear his cries. He waited.
“Then I think I spot him,” he says. “He gets out of the water like it’s nothing. And that memory was with me while he was dying. I guess my own recognition was how hard he worked to stay alive. He really worked hard to stay alive for my mom and for the rest of us. I always appreciated it.”

Figel drives us to an old cemetery where his parents’ ashes would later be buried side by side in the same burial plot. Until then, their ashes are on a shelf next to his workbench in the basement, where only Figel can find them.
When medical schools are finished with donors, their bodies are cremated and sent back to the families who want them.
At the Anatomical Gift Association of Illinois, the curator of cremains, Tim McGuinness, works the mailroom, a small office of shelving units and rectangular black boxes of ashes with names printed on the sides. He tracks where bodies are and tells families when they will be returned.
“I’m alone in my office every day with 300 people,” he tells me.
The cemetery road is thin and winds between gravestones with Irish and German names: Donahue, Sullivan, Kelly, O’Malley, Figel. When William Sr. was still alive he would ride here on his electric cart while his grandchildren followed on their bikes. It was one of his favorite places to go.
The car stops and we step out. Figel points to the spot where his parents would later be buried, in front of their parents. Donation happens so fast after death that there isn’t time for a funeral. Figel says his father’s brother, a priest, is preparing a eulogy, and his siblings will come for a small ceremony.
In the years since his parents’ deaths, Figel has helped friends do the same for their parents.
Before Greg Carr died in November, his children photographed him wearing a Superman costume, flexing with a goofy expression on his face. His body went to the AGA, and a cardboard cutout of the photo went to the funeral service.
“I’m thrilled they absolutely embraced it and celebrated it,” Figel says. “Anything that can contribute to life, whether it’s for science or pure love, usher along mankind. That may sound lofty, but it’s how I feel.”