Antibiotics Can’t Cure ‘Super-Gonorrhea’—Here's What That Means
The sexually transmitted infection has been steadily becoming more resistant to antibiotics.
A man in the U.K. has contracted what is being called the "worst-ever" case of "super-gonorrhea." This venereal disease appears to be the first instance in which the infection can't be treated with common antibiotics, according to public health officials.
The man, who has not been named, likely picked up the STI after having sexual contact with a woman in Southeast Asia last year. He apparently began showing symptoms one month later and attended sexual health services in England in early 2018.
Health officials have tried targeting the man's disease with the antibiotics azithromycin and ceftriaxone, but with no success. They've turned to a different drug called ertapenem, which has also been used to prevent infections after colon and rectal surgery. Ertapenem appears to be effective now, and the man will be tested again in April to see if it's still working.
The man has one regular female partner in the U.K., and she has tested negative for the superbug. Health officials are tracing back the man's past partners to see if any of them has been infected, but no other cases have currently been discovered.
"This is the first time a case has displayed such high-level resistance to both of these drugs and to most other commonly used antibiotics," Gwenda Hughes, head of Public Health England's STI section, tells media. "We are following up this case to ensure that the infection was effectively treated with other options and the risk of any onward transmission is minimized."
Although this may be the first time a case of gonorrhea has been reported "incurable," the disease has steadily become more drug-resistant over the years. At the same time in 2016 when the United Nations declared antibiotic resistance "the greatest and most urgent global risk," the CDC announced gonorrhea was going down an untreatable path. (Related: "Scary New Superbug Is Popping Up in More Places")
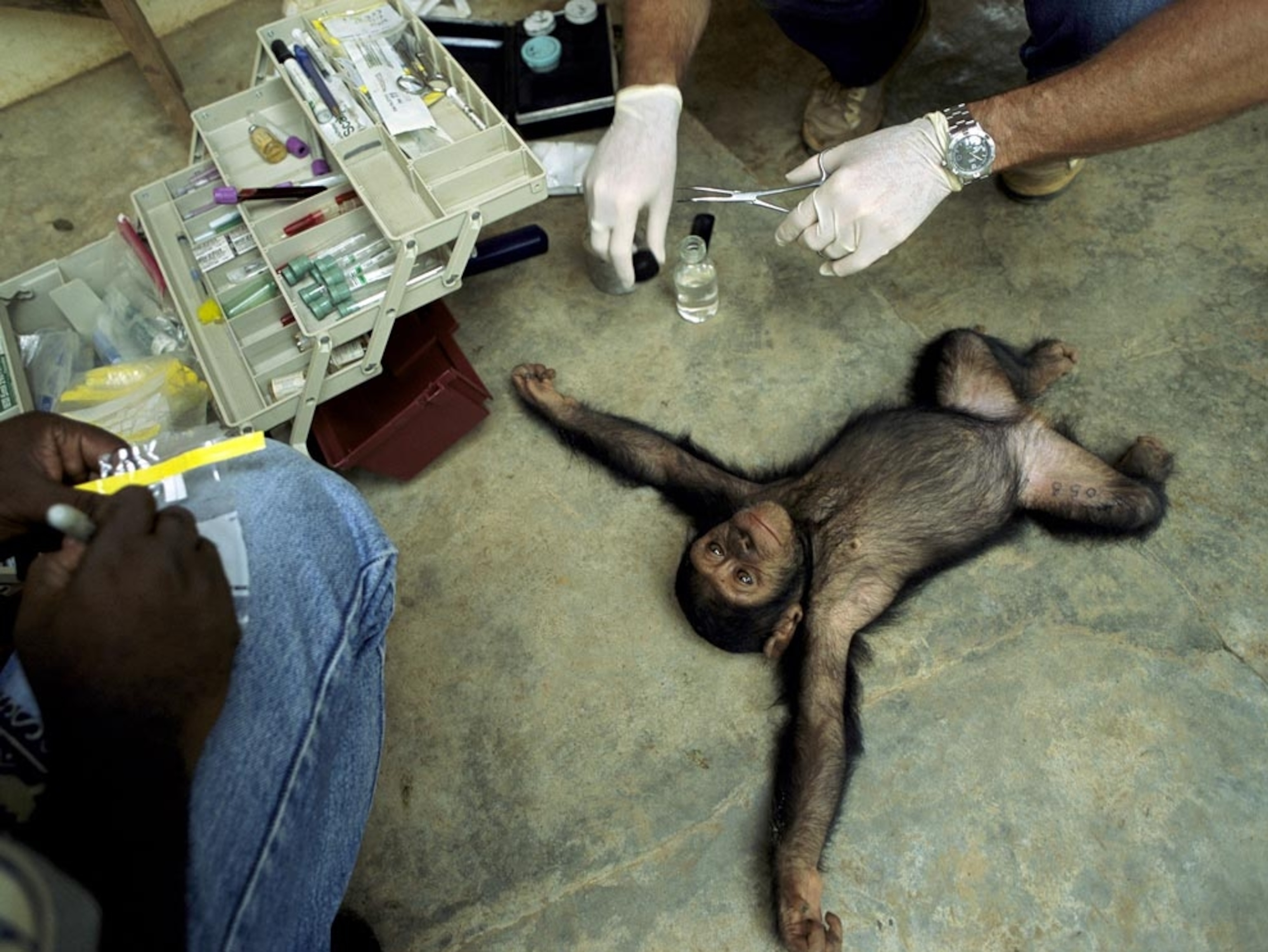
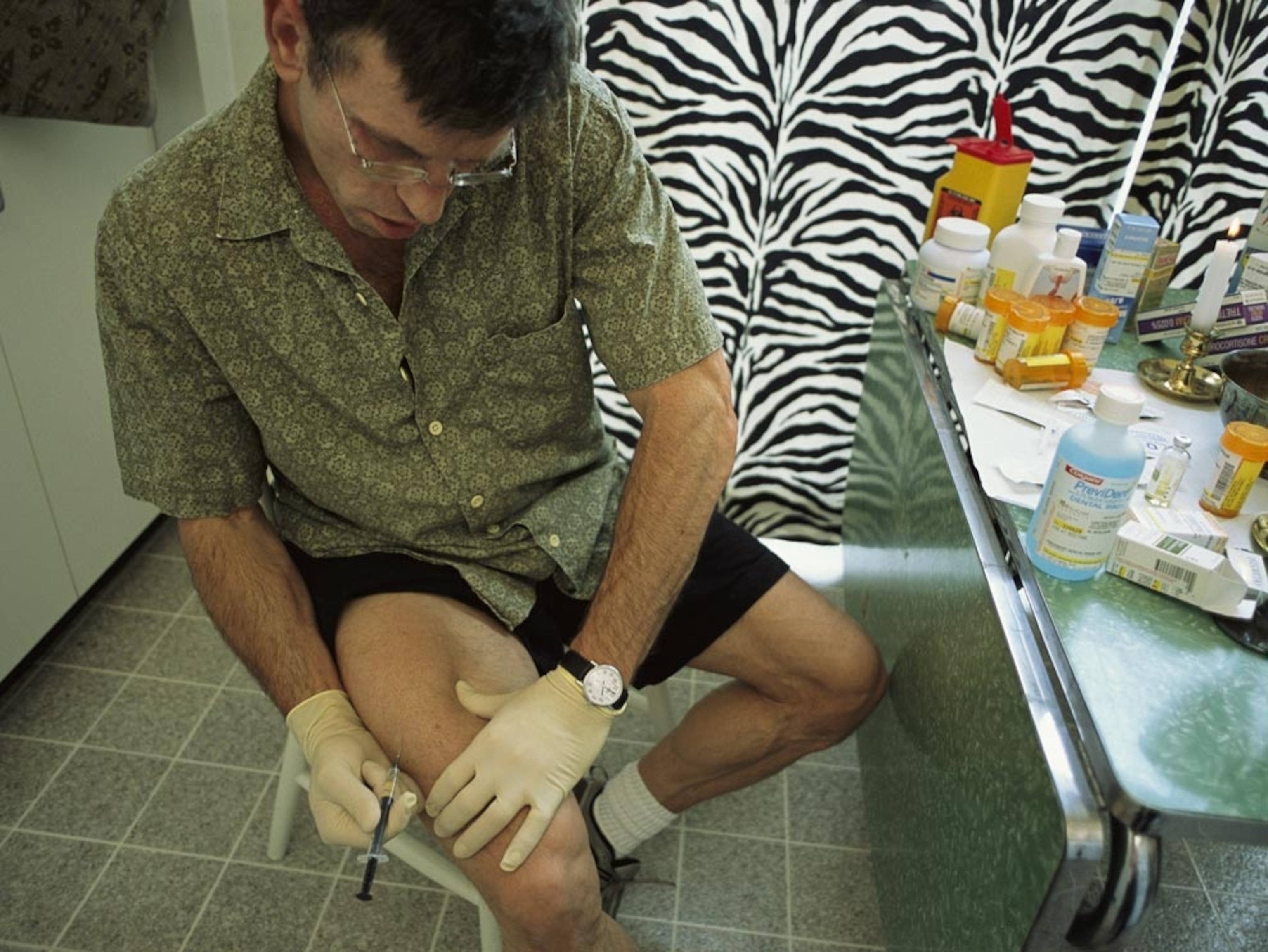
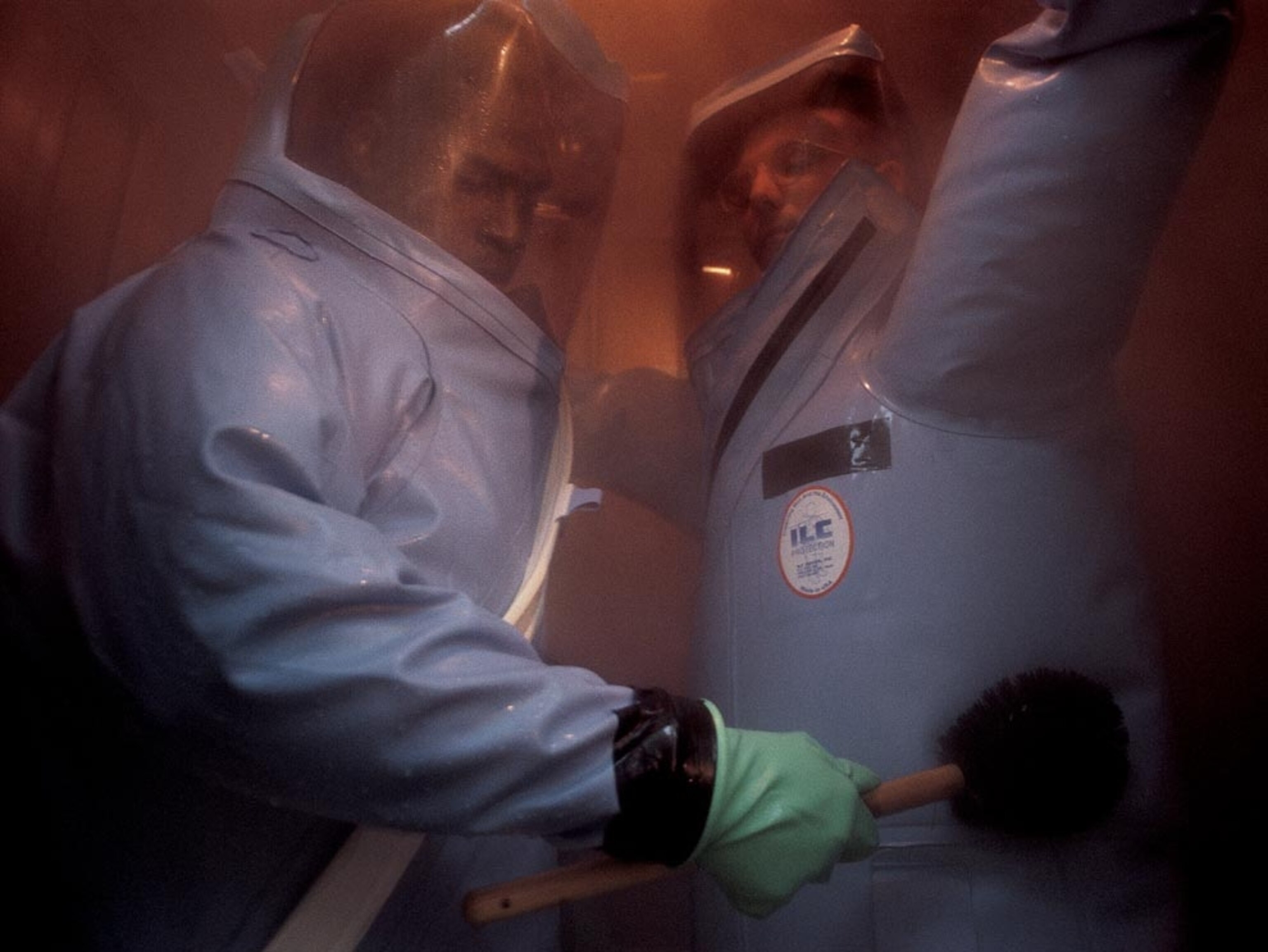
Related: Photos of the AIDS Crisis
Undiagnosed Cases
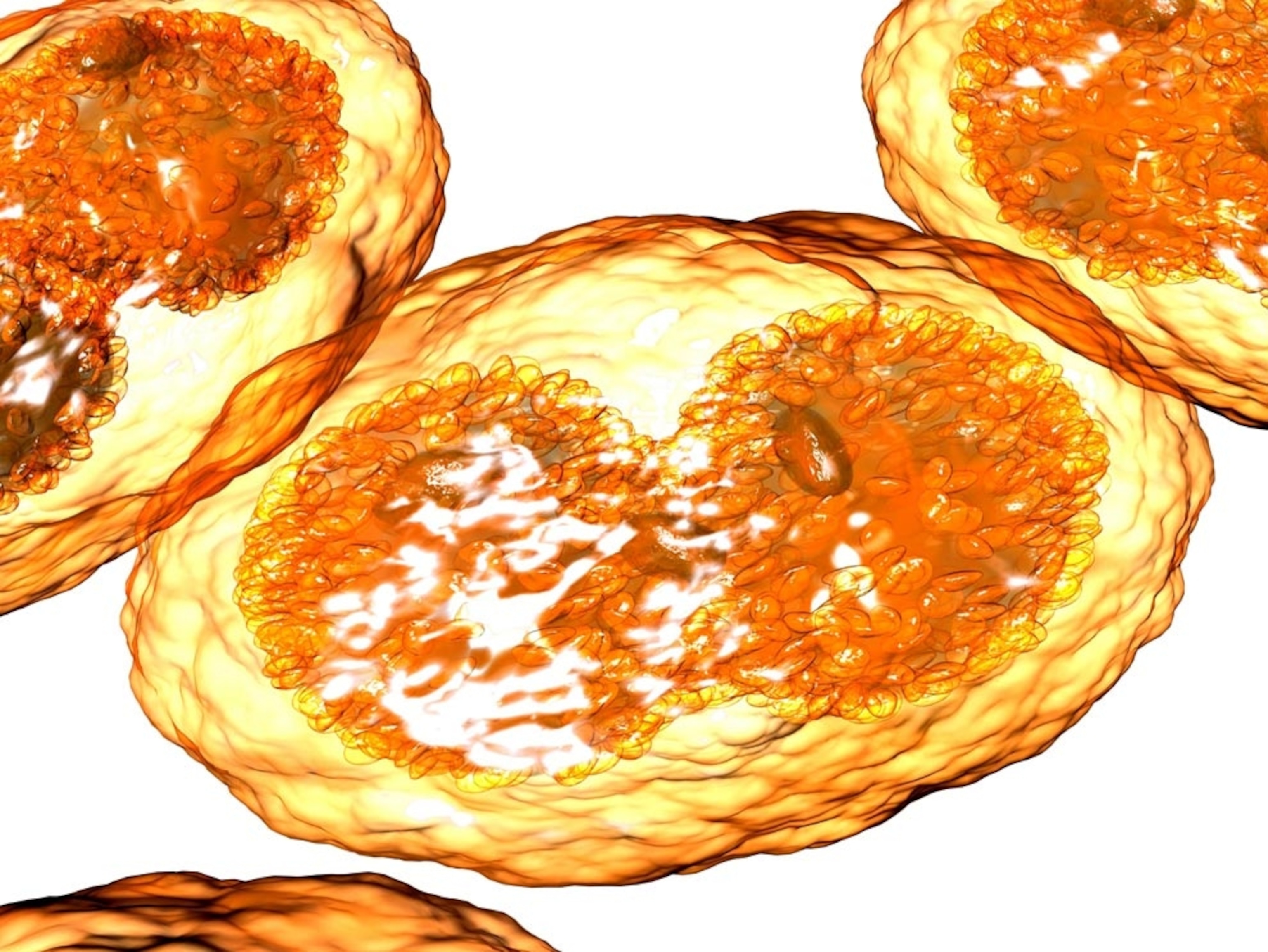
Gonorrhea, a venereal disease caused by Neisseria gonorrhoeae bacteria, is an infection that can be spread by sexual contact. During childbirth, it can also be transferred from mothers to babies, where it most commonly effects the eyes.
Most people who contract gonorrhea are asymptomatic, but those who exhibit symptoms experience painful urination, abnormal discharge from sexual organs, or pain around these areas. If left untreated, gonorrhea can lead to infertility or pelvic inflammatory disease. Once a patient has cured their infection, it's possible to become reinfected.
The CDC estimates that about 820,000 people in the United States contract gonorrhea each year, and more than half of these cases are reported. Although many patients go undiagnosed because they may not have obvious symptoms, the disease is becoming more difficult to treat. Cheaper, older antibiotics that have been misused and overused are now failing. Of the three most common STIs—the others being chlamydia and syphilis—gonorrhea is the most antibiotic resistant. (Related: "Superbugs, Meet Your Worst Nightmare: This Pepper Tree")
Fast Clap
There are concerns that gonorrhea is developing into a superbug that can't be treated with antibiotics. Of the two million people in the United States who are infected with antibiotic-resistant bacteria each year, 23,000 of them die as a result. (Related: "Teaching People How to Stay Healthy Has Come a Long Way")
"We're continuing to use antibiotics in a bad way. They're supposed to be used to combat bacteria, not viruses," Stuart Levy, director of Tufts Medical Center's Center for Adaptation Genetics and Drug Resistance, told National Geographic in 2014. "Any time you use an antibiotic when it's not needed, you're pushing antibiotic resistance ahead."
In 2011, National Geographic reported that the disease is picking up human DNA. After the onset of infection, the bacteria invade human cells, where they copy themselves, and some research suggests the bacteria may even advance into deeper tissue. (Related: "New Human 'Organ' Was Hiding in Plain Sight")
"The bacteria have acquired the ability to destroy the antibiotic in order to protect themselves," Levy continued. "A genetic mutation might enable a bacteria to produce enzymes that inactivate antibiotics. Or [a mutation] might eliminate the target that the antibiotic is supposed to attack."
Margaret Chan, former director-general of the World Health Organization, put it well at the UN meeting in 2016: "We are running out of time."
(Related: "How We'll Tackle Diseases That Are Becoming Untreatable")