
This man gets bitten by deadly snakes in the name of science
A partnership between an immunologist and a snake-keeping ex-truck mechanic is attempting to find a medicinal holy grail: a universal anti-venom. It's a seriously risky business.
Tim Friede has been bitten by venomous snakes more than 200 times. On nearly every occasion, he has positively encouraged it. Lethal cobras, mambas, vipers, taipans, rattlesnakes and kraits—he has willingly offered himself up to the fangs of all, soliciting what could be a potentially fatal bite from some of the most feared animals on the planet.
Nowadays, Friede, a former truck mechanic in his fifties from Wisconsin, is director of herpetology at Californian vaccination research company Centivax—which is attempting to produce a universal anti-venom for all the world’s most lethal snakes. But when he first started his masochistic hobby, he was merely an amateur snake collector. As a high-school kid he would scour the Wisconsin countryside for garter snakes, which are only mildly toxic. This led to keeping far more venomous snakes as pets in vivaria at home. Cobras, mambas, taipans, rattlesnakes—to the chagrin of his parents, his collection grew and grew. (See pictures of some of the world's most extraordinary snakes.)
Constantly at risk of being envenomed, Friede realised he needed somehow to develop an immunity. The theory being that, by stimulating his body to produce antibodies in response to the toxin, he may be physically better-equipped to cope when bitten in future. He started milking his pet snakes for their venom before repeatedly injecting himself with it. He was careful to dilute the venom, just as commercial manufacturers do when they extract anti-bodies from horses or sheep to produce anti-venom. “It was hard because there’s no book on it,” he tells National Geographic (UK.) “So I figured it out by taking lots of notes and lots of photos.”
‘I basically died.’
It was in 2001 that Friede received his first potentially lethal bite—although not intentionally. While at home in Wisconsin, as he was milking his pet Egyptian cobra, the reptile twisted round and bit his finger. Already fortified with a certain immunity, Friede was little affected. But then, just an hour later, he was handling a monocled cobra which lashed out and sank fangs into his right bicep.
“Two cobra bites, back to back, within one hour,” Friede remembers. “I basically flat-lined and died. It wasn’t fun. I had enough immunity for one bite, but not for two. I completely screwed up.”
Rushed to hospital by his wife and neighbour, he spent four days in a coma. After coming round, he realised that self-envenomation was an undertaking he ought either to quit, or perfect. “I chose the latter.”
He certainly did. Over the next 17 years he regularly spliced body fluids with those of a whole range of exotic serpents. As well as the 200 fang bites, another 500 or so doses were administered via hypodermic needle. Among the most toxic venoms were those of coastal taipans, water cobras, Egyptian cobras, diamondbacks, Mojave rattlesnakes, all four species of mamba and various kraits. “I wanted to take the worst snakes on the planet and beat them,” he remembers.
Two cobra bites, back to back, within one hour … I basically flat-lined and died. It wasn’t fun.Tim Friede
Pain for a purpose
In general, when a snake bites, liquid venom is squeezed along grooves in the fangs, or through fangs that are hollow, into the flesh of its victim. It hurts. “Almost every bite is painful,” says Friede, who usually offers up his forearms. “Like a bee sting times a hundred.”
However, he insists he was never motivated by some sort of machismo. Rather, it was all part of a scientific experiment to discover whether he could, by the process of his own immune system, defeat some of nature’s most toxic animals and help fellow humans in the process.
“I never did it to be a tough guy and make YouTube videos,” he says. Nonetheless, social media videos of him allowing snakes to bite him have clocked up hundreds of thousands of views.


The resulting publicity brought him to the attention of immuno-engineer Jacob Glanville, the brains behind Centivax. Glanville, also American, was brought up in the 1990s in a fairly remote village in Guatemala during that country’s civil war, where he witnessed locals, deprived of medicine, suffering needlessly from illness and disease. Later he studied immuno-genetics and computational biology at the University of California, Berkeley, and computational immunology at Stanford University.
Now, through his work with Centivax, he hopes eventually to rid the world of the effects of pathogens altogether. High up on his list is snake venom. Along with Freide —and the precious antibodies in his blood—Glanville is working to produce his universal anti-venom.
Pinpointing precisely which are the world’s most venomous snake species is tricky. According to the Australian Venom Research Unit, in terms of actual venom, the most toxic of all is the inland taipan (Oxyuranus microlepidotus), or fierce snake, which inhabits central east Australia. Its venom contains a witch’s brew of toxins, affecting the blood, the muscles and the nervous system.
The Journal of Herpetology warns that a single bite contains enough toxin to kill at least 100 adult humans. Fortunately, the animal is something of a recluse, and lives in arid regions where humans rarely stumble upon it.
Almost as toxic are several species of sea snake from the Indo-Pacific, such as Dubois’s sea snake, yellow-bellied sea snake and Peron’s sea snake. Again, since they rarely mix with humans, they rarely cause deaths. Other species are less venomous but, for a variety of reasons, they kill more regularly.
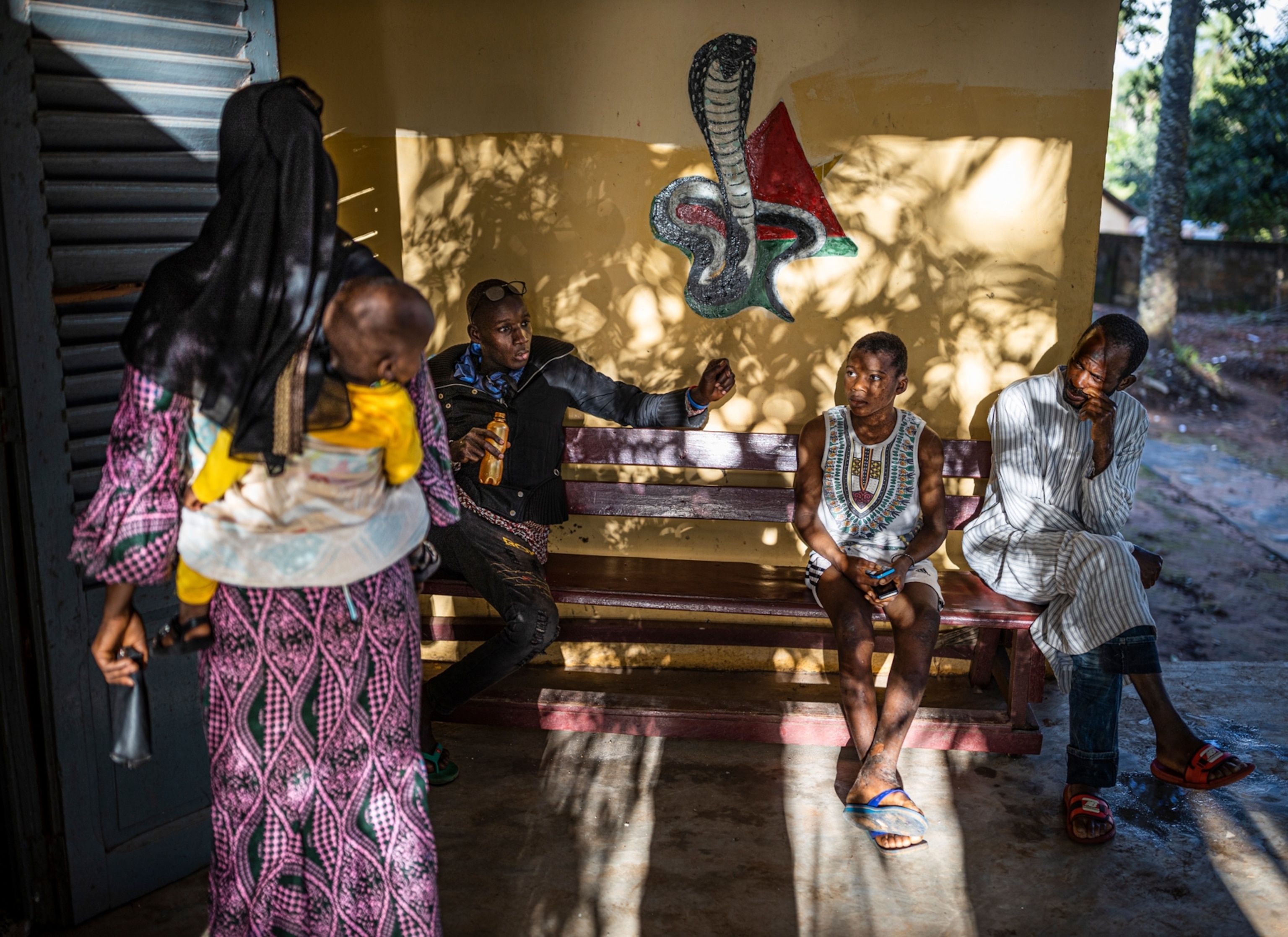
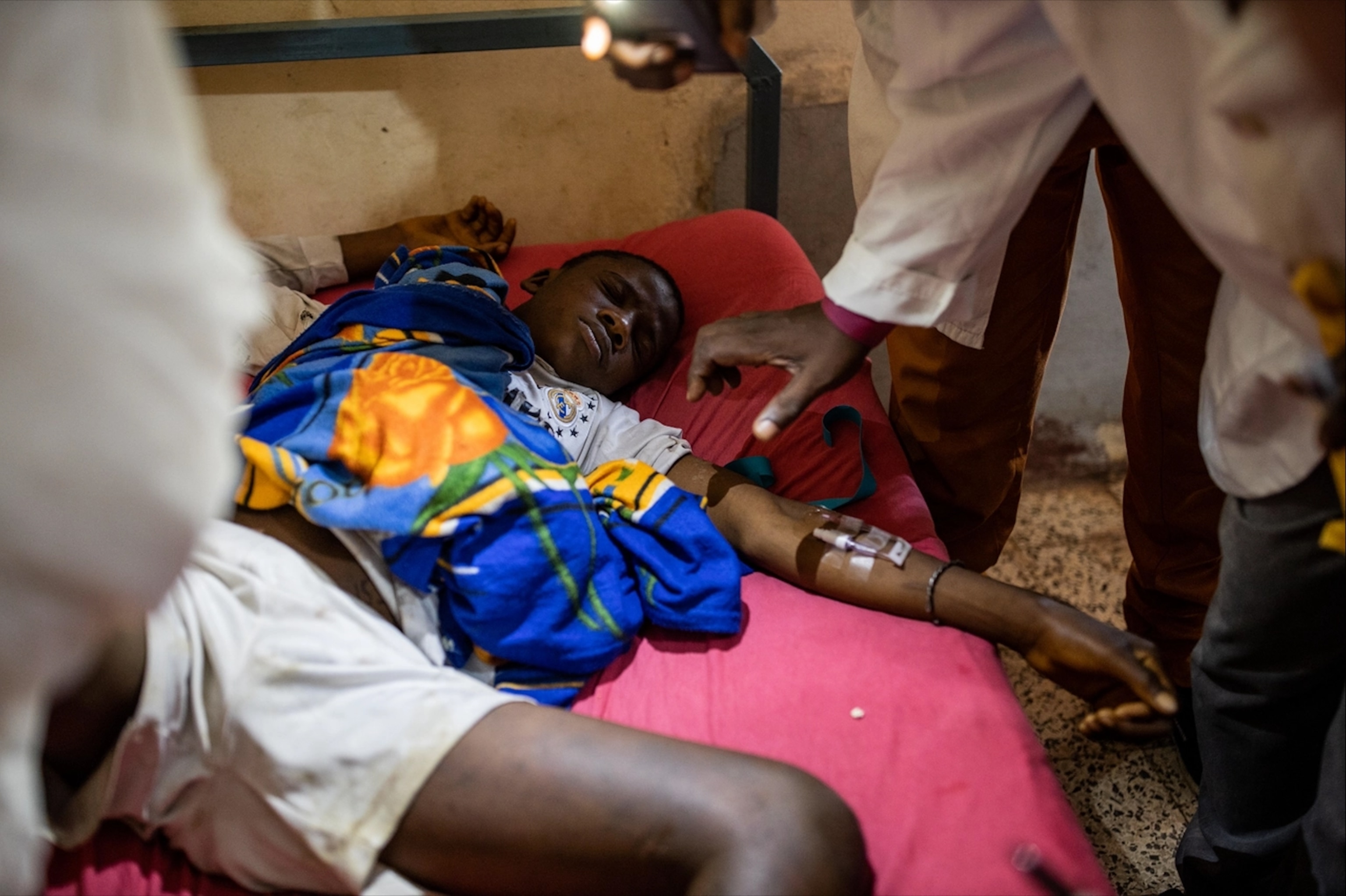
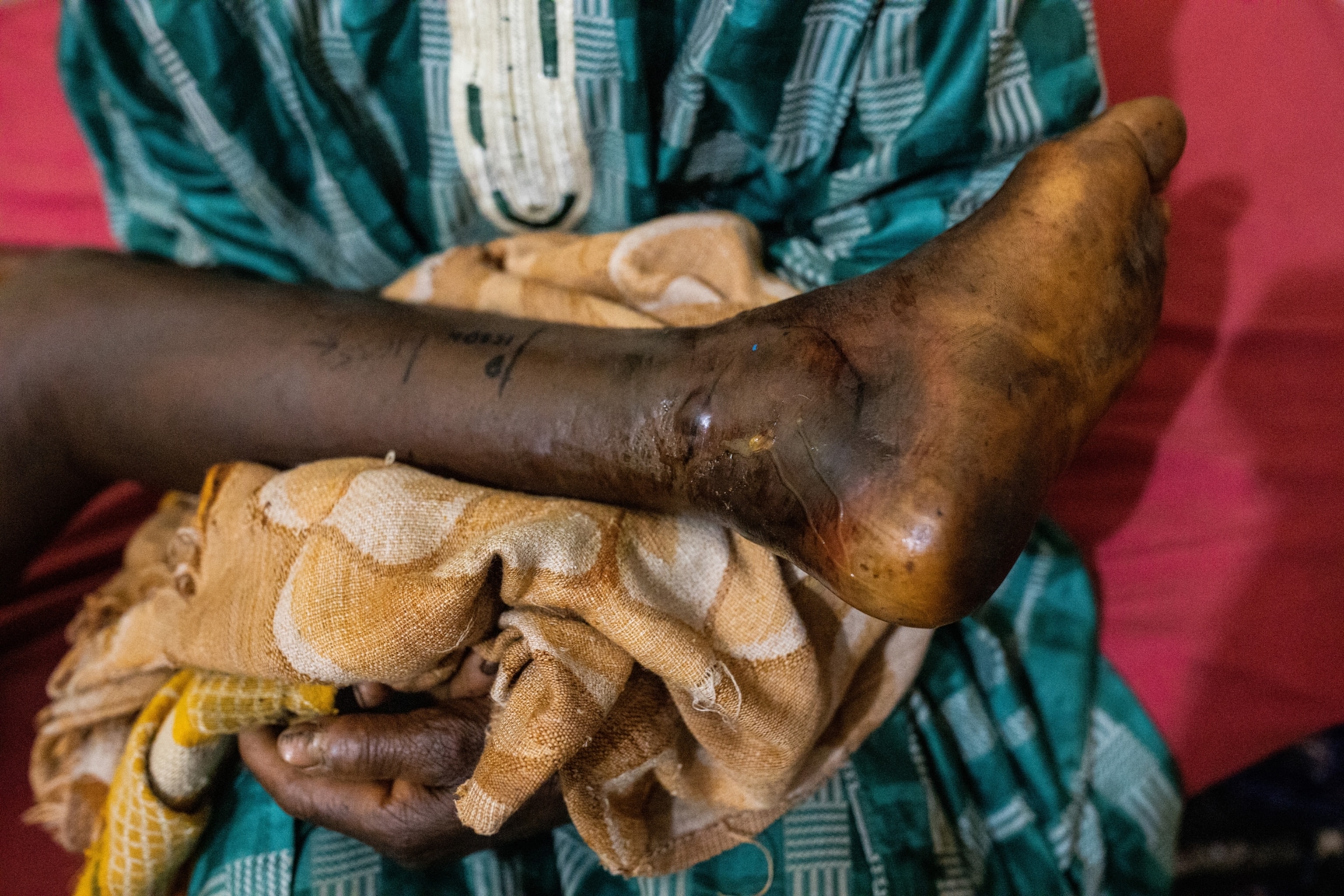
The World Health Organisation (WHO) estimates that 5.4 million people a year are bitten by snakes, and up to 2.7 million of them envenomed. Between 81,000 and 138,000 people die from the bites, while up to 400,000 have limbs amputated or suffer other permanent disabilities. The tropical and sub-tropical regions of Africa, Asia and Latin America are most affected. Most at risk of dying are agricultural workers and, because of their smaller body mass, young children. A lack of footwear makes poor rural workers particularly vulnerable.
(Read: In Africa, snake bites are a neglected health crisis.)
It’s possible many other victims go unreported. The Africa Health Organization explains that this is “because victims seek treatment from non-medical sources or do not have access to health care”.
Deadly serpents by numbers
There are 600 or so species of venomous snakes slithering round the planet. But only around a dozen species groups are responsible for most human deaths and disabilities. As the WHO warns, some are found close to farmers who aren’t wearing adequate footwear. Others are more aggressive, or deliver venom more efficiently, or in amounts large enough to kill humans.
Bearing these factors in mind, statistically, among the deadliest of all are black mamba, coastal taipan, Indian cobra, common krait, Russel’s viper and saw-scaled viper. The latter—scientific name Echis carinatus—which lives across the Middle East and Central Asia, especially in the Indian subcontinent, is considered by many herpetologists the biggest human killer of all. Relatively small, usually no longer than 60cm, it is inconspicuous but extremely aggressive. It rests in a coil, with its head at the center, so that when it strikes, it darts out like a released spring.
A 2020 university study found that, in India alone, 58,000 people die every year from snake bites, and in most cases the saw-scaled viper is the culprit. (Here's why poisonous animals don't poison themselves.)

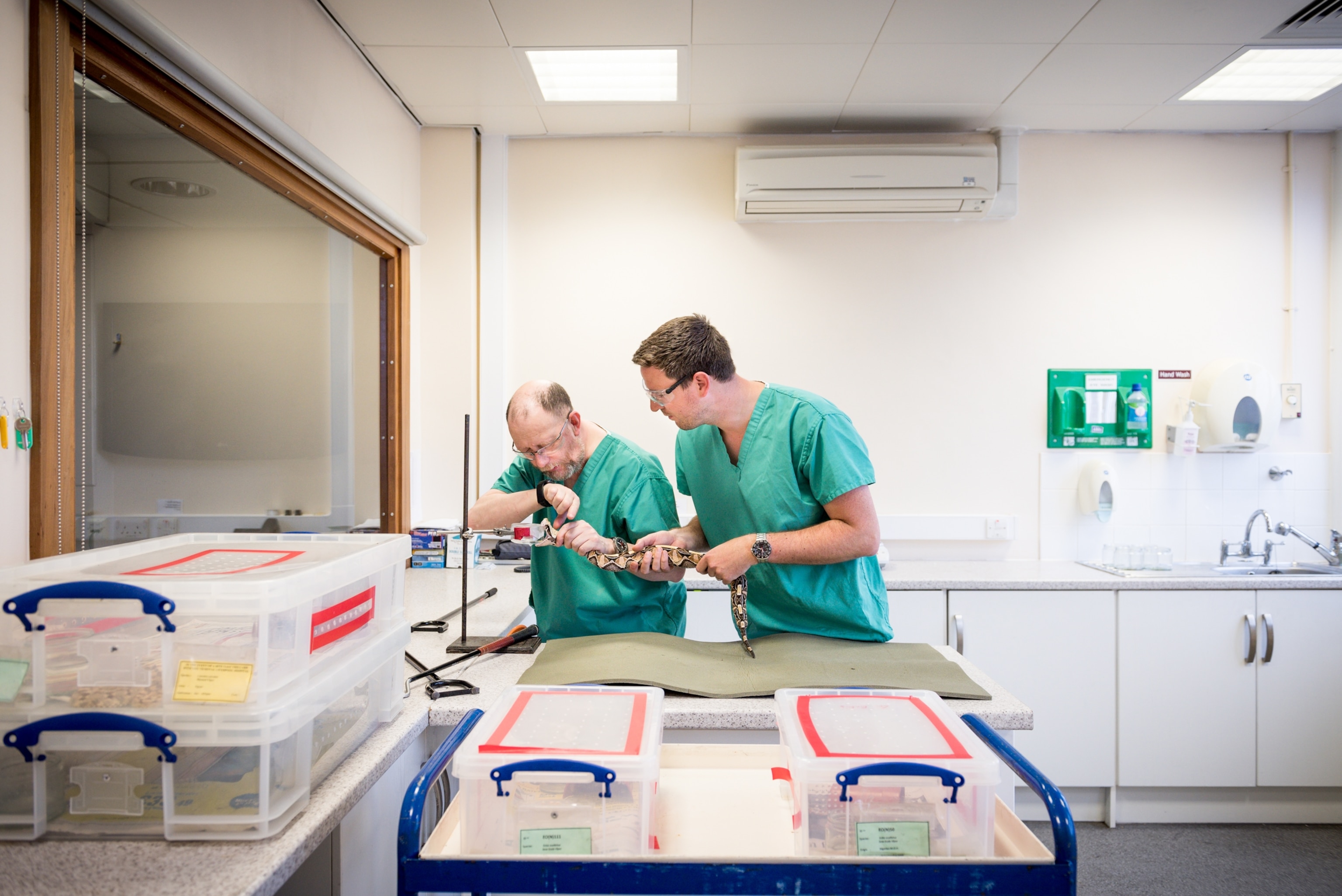

One British herpetologist who knows all about this lethal creature is Professor Nicholas Casewell, director of the Center for Snakebite Research and Interventions at the U.K.’s Liverpool School of Tropical Medicine. Originally set up in the early 1980s, the center now houses 200 venomous snakes from around 50 different species, and is the largest herpetarium in the U.K.
“Saw-scaled vipers are small and look pretty innocuous,” he told National Geographic (UK). “As a group of snakes, they kill more people worldwide than any other group of snakes. It’s not the toxicity of their venom, it’s more of a socio-economic problem because they inhabit regions where people are working agriculturally, typically with no protective footwear or gloves, and they bite a huge number of people.
(Leopards, elephants and cobras: Tea plantation workers in India face poverty—and dangers.)
Because of the delays and challenges in accessing effective healthcare and effective treatment in these parts of the world, a huge number of people die from the bites. Often it can take a victim many hours or many days to get to an appropriate healthcare facility. Sometimes they might seek traditional medicines first. Or they might get passed to another healthcare facility because there aren't staff or medicines to treat them. Often those victims die in transports between hospitals.”
Risk varies between countries, of course. In the U.K. where Casewell works, the only venomous snake is the common European adder, for which anti-venoms are widely available. Whilst possible complications make this still a bite to avoid at all costs, the last Briton to die of an adder bite was a five-year-old boy, back in 1975.
(What's the difference between a poisonous animal and a venomous animal? It's not that simple.)
The world’s first ever snake anti-venom for humans was produced by French physician Albert Calmette in 1895, and the medical science has advanced comparatively little since then. Anti-venoms are still manufactured by immunizing donor animals such as horses, sheep or camels with snake venoms before harvesting and purifying anti-bodies from their plasma to create a serum.
This traditional method isn’t without its flaws. Christiane Berger-Schaffitzel is a professor of biochemistry at the University of Bristol working on snakebite therapy. She told National Geographic (UK) that antibodies from other mammals pose risks of zoonotic disease. And because the snake venom anti-bodies in their blood are so dilute, humans often require huge amounts of serum to be injected, which risks life-threatening side effects. “You develop an immune reaction against these antibodies,” Berger-Schaffitzel adds. “The serum is recognised as a horse antibody. It’s not supposed to be injected into humans.” (Why horseshoe crabs are the silent victims of vaccine rollouts.)
Chemistry in common
Back at Centivax, with their Holy Grail of a universal anti-venom, Glanville and Friede want to revolutionise these outdated systems of treatment. Using Friede’s antibodies, they hope to target the protein-binding sites shared between the deadliest snakes. One of Friede’s antibodies, which they’ve called Centi-LNX-D9, is of particular interest. In experiments with laboratory mice it “provided complete broadly neutralizing protection against whole venom from monocled cobra, black mamba, yellow-lipped sea krait, Egyptian cobra, cape cobra, Indian cobra and king cobra”.
Glanville now estimates he will be conducting human trials on a universal anti-venom in two years’ time. Optimistically, he hopes to bring a product to market three years after that. It may come in the form of ready-to-administer syringes which could be stored at room temperature in medical clinics out on the field.
“Hospitals may be far away from the victim,” he adds. “But each village will have a medical clinic, often just a room in the front of someone’s house. If someone gets bit, you’d have a runner run out and administer the anti-venom.” (Spiders eat snakes around the world, shocking study reveals.)

There are many other research centers around the world with similar goals. One of the main funding organisations in this field is the London-based Wellcome Trust. Leading the snakebite research there is Dr Diogo Martins. He points to two British centers making headway in anti-venom production. The first is the aforementioned Center for Snakebite Research and Interventions in Liverpool, the second a Camarthenshire, Wales-based company called MicroPharm, which is targeting the most dangerous snakes in sub-Saharan Africa and the Middle East.
Other research centers he highlights include the Instituto Clodomiro Picado, part of the University of Costa Rica; the Instituto Butantan, in the Brazilian city of Sao Paulo; Ophirex, in California; and The Queen Saovabha Memorial Institute, in Bangkok.
With current anti-venom technology now over 120 years old, and up to 138,000 people perishing every year, why hasn’t this lethal menace already been dealt with?
“Most of those people are poor,” says Glanville, pointing out how snakebites are predominantly a problem of the developing world. “It's a financial issue. Most of the neglected tropical diseases are viewed as less profitable than other areas such as cancer or neuro-degeneration that lots of rich people die from and would pay lots more money to cure.”
Diogo Martins at the Wellcome Trust concurs. “Snakes will always exist. We cannot, will not, eliminate snakes,” he says. He suggests governments should fund anti-venom treatments more consistently, but realises this is hardly a vote-winning policy. Besides, the rural communities that suffer the most are often the least listened to by politicians.
One group that politicians do listen to are the military. They also happen to operate in regions and situations where dangerous snakes thrive. Glanville believes, once he develops his universal anti-venom, military organisations could be first in line to buy it. This might prove to be an impetus for pharmaceutical companies to manufacture the product at scale, drive down costs—and eventually deliver it cheaply to the people who need it most.
This story was adapted from the National Geographic U.K. website.
—