Scientists are trying to resurrect mostly dead organs—here’s why
Jaw-dropping studies in pigs have given hope that new preservation strategies could end a deadly shortage of transplant organs.

When Yale University neuroscientist Nenad Sestan used a brew of nutrients, proteins, and drugs to resuscitate a pig’s brain hours after its death, he discovered the line between life and death wasn’t as clear as he’d once thought. His goal hadn’t been to reanimate the brain but rather to study its wiring. As soon as he published the sensational results in 2019, interest in his lab’s activities flooded in from around the world.
“A lot of colleagues at Yale and elsewhere came knocking on our door, saying, ‘We need to try this in kidneys, we need to try that,’” Sestan says. All this interest led him and his team to concoct a solution, which they dubbed OrganEx, that when pumped through the circulatory system can restore function to multiple organs in an animal that has been dead for more than an hour. “I’m a neuroscientist,” Sestan laughs. “In my wildest imagination, I never thought I’d be working on a kidney, heart, or another organ. But the unmet needs of organ transplantation really motivated us.”
In the United States alone, more than 6,000 patients perish waiting for an organ transplant and every year 700,000 people die due to end-stage organ disease. The World Health Organization estimates that only 10 percent of people worldwide who need an organ transplant are able to get one; yet thousands of donated organs end up in the trash every year because they aren’t preserved immediately. In 2012, for example, while 2,421 hearts and 1,634 lungs were transplanted in the U.S., 5,723 donor hearts and 6,510 donor lungs were wasted.
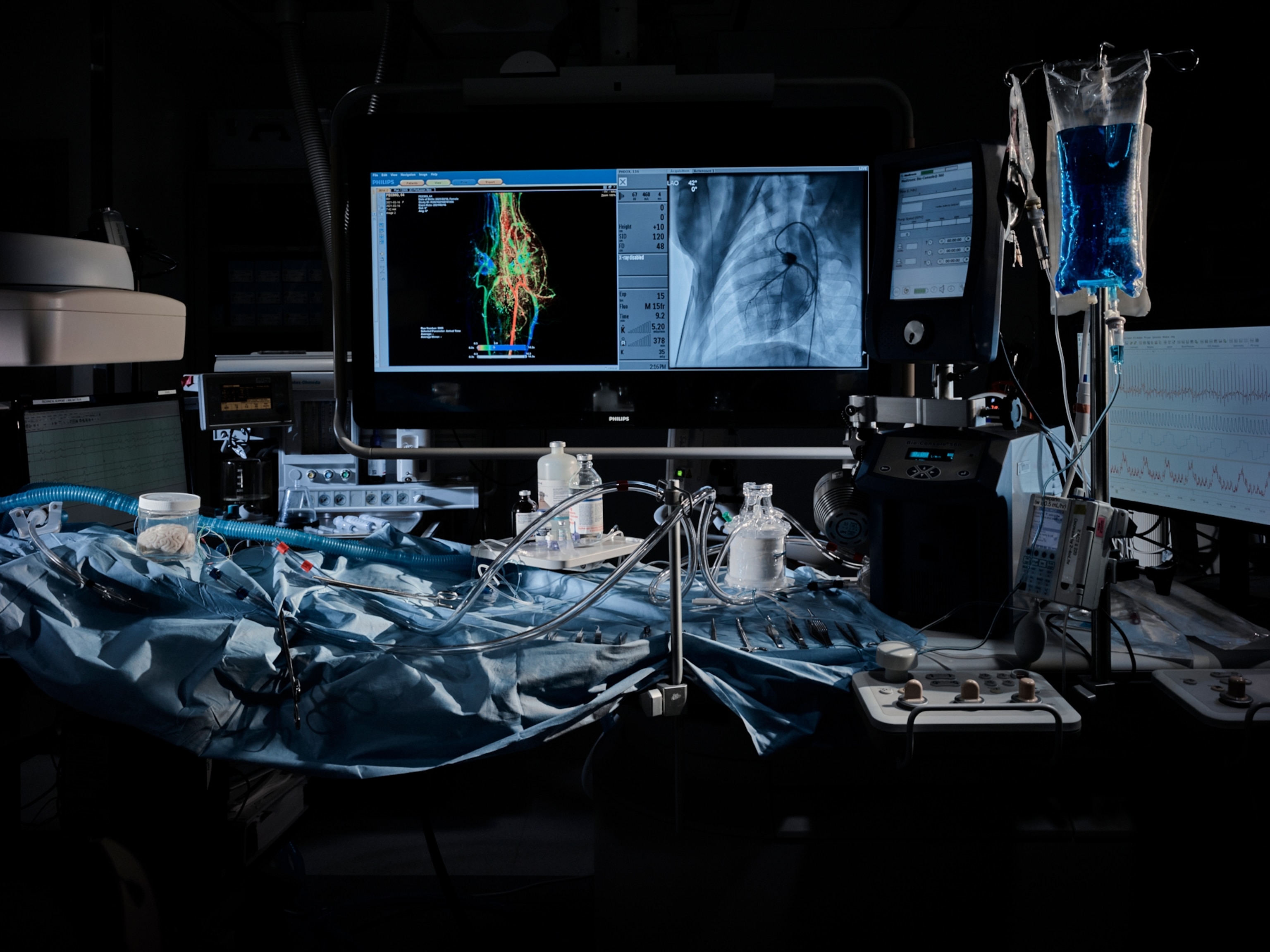
After the heart stops pumping, organs must be harvested immediately to be viable for transplant. For this reason, most come from brain-dead organ donors already on life support. Once this support is removed, the organs are preserved—typically, by placing them on ice, which slows metabolism and cellular death. But Sestan’s work could one day push the boundaries of this restriction. “What Sestan’s team did is gain time prior to organ recovery—which is important when we talk about expanding the donor pool,” says Gerald Brandacher, a transplant surgeon at the Johns Hopkins Reconstructive Transplantation Program, who is intimately familiar with these challenges. “Everything in transplant medicine is a race against time—it’s our most precious resource.”
Their work, which was done in pigs and published this August, marks the first-time multiple organs—the heart, liver, brain, and kidneys—can be rescued and made to function even if the animal hasn’t been cooled and has been dead an hour.
Recovering multiple organs with one intervention would increase the organ supply by including those that would normally be discarded—such as those of patients who die at home and whose bodies can’t be retrieved immediately, says David Andrijevic, a physician-neuroscientist at Yale and a member of Sestan’s team.

“For me, it was really surprising to see that we were able to restore circulation and cells throughout the body, because as soon as you die, there are biochemical cascades that begin to destroy cells and block the flow of blood,” says Sestan. “You can’t just take blood that’s treated with anticoagulants and perfuse it, which is why this has never been done before—it just doesn’t work.”
This research and other similar developments have upended the field—transforming our understanding of how and when cells and tissues die, as well as uncovering alternative ways to keep them viable.
“The Yale group proved that cells in a cadaver do not become irreversibly damaged for [at least one hour] post-mortem,” says Sam Parnia, a critical care physician at NYU Langone. “And so instead of having this accepted idea of death as the end, we recognize that you can die, but the potential for developing treatments to bring you back exists.”
Why cells die
Unlike the depiction in countless medical dramas, the brain (and other organs) don’t die immediately when the heart stops pumping blood laden with oxygen and nutrients through the body. “Instead, it’s a more protracted series of events, which opens up a window where we can intervene, stop the process, and even initiate the recovery of cells,” Andrijevic says.

Our organs thrive because of thousands of little power stations inside every cell, called mitochondria, which transform food into energy that fuels essential activities—including breathing, thinking, and running—while clearing away toxic byproducts. But in the moments after blood flow stops, called ischemia, this balance shifts. The mitochondria burn through dwindling supplies of nutrients and accumulate waste that eventually poisons and kills the cell.
Although mitochondria generally produce energy with the help of oxygen, they can switch to a less efficient, low-oxygen process, and use the body’s fuel reserves while they last—typically five minutes or so. When energy levels invariably plummet, an early casualty is the cell’s ion balance, which controls cell-to-cell communication and energy production.
“Like a ship that needs to continually pump out water to avoid sinking, cells have pumps that constantly throw out calcium and sodium,” Parnia explains. Without energy powering them, however, the pumps—located in the membrane of the cell—fail, and calcium, sodium, and water rush in.
Rising calcium activates enzymes that break down DNA and that chew through the cytoskeleton, which gives the cell its structure. High concentrations of calcium also trigger the mitochondria’s self-destruct buttons, or apoptosis. “But apoptosis is a process that occurs over the course of up to 72 hours, on average,” Parnia says.
At the same time, free radicals—unstable molecules like hydrogen peroxide and superoxide—cause havoc by rupturing the membranes of the cell and deactivating enzymes.
If CPR or another lifesaving measure suddenly restores blood flow, it can, paradoxically, set off a second, more devastating wave of destruction: Blood vessels leak, tissues swell, and cell death accelerates.
Parnia compares this phenomenon to the ruin wrought by earthquakes followed by tsunamis. The earthquake sets the scene, but it’s the tsunami that often inflicts the most harm. “By instituting anti-tsunami measures, or treatments against the secondary injury process, we can save brain function, and that opens up a whole new field of medicine,” Parnia says. “And what the Yale group has shown very beautifully, is exactly that phenomenon”—the benefits of controlling how blood and oxygen are restored to the tissues.
Clinical practice, however, often trails science. Most people, including many physicians and scientists, have an outdated understanding of death, according to Parnia. “We're all brought up with this idea that death is a permanent end—not recognizing that it's the permanent end only because we don't have treatments. It's not necessarily the cellular permanent end,” he says.
A new way to rescue dying organs
To demonstrate that cells and organs can be recovered long after conventionally believed, the Yale team induced cardiac arrest in pigs—animals chosen for their similarities, like size, to humans—and left the bodies on the operating table at room temperature for an hour.
After an hour passed, the researchers attached an IV to the pig and infused a sapphire blue solution—OrganEx—into the circulatory system. The perfusate is a proprietary mix containing “amino acids, vitamins, metabolites, and a drug cocktail of 13 different compounds that have been optimized to promote cellular health, decrease cell stress and death, and suppress inflammation,” according to Andrijevic. The solution mixes with the animal’s own blood as it’s circulated for six hours with the aid of a machine—similar to the ECMO heart-lung devices used to provide temporary cardiovascular support to injured patients. But this device contains special pumps to deliver OrganEx without shredding capillaries, a dialysis unit to filter out toxins, and sensors to monitor fluid pressure and flow.
As controls, some animals were untreated; others were treated with ECMO, after the hour elapsed—which was used to pump blood infused with oxygen and free of carbon dioxide, through the body.
Designed with the input of an external advisory committee and other experts, the experiments followed humane animal treatment standards; the pigs were anesthetized and given neuronal blockers to prevent them from regaining consciousness. “We wanted to see to what extent we could restore or reverse the demise of cells in damaged organs. Our job was not to revive the animal,” Sestan says.
When the team examined slices of OrganEx-treated brain, heart, liver, and kidneys under the microscope, they found that they looked more like healthy tissue than the disintegrating tissue from control animals.
Single-cell RNA sequencing—which provides a real-time snapshot of the molecular processes happening inside the cell—indicated that organs from OrganEx-treated pigs resumed basic functions like DNA repair and maintaining cell structure while preventing cell death. In addition, heart cells began to beat, and liver cells resumed their task of absorbing glucose from the blood.
However, Sestan urges caution when interpreting the results. “We can say that the heart is beating, but to what extent it’s beating like a healthy heart—that will require more studies.”
Future goals: Banking and improving organs
Ultimately the goal of transplant scientists isn’t just to save donor organs, but to improve them before placing in the recipient, says Abbas Ardehali, a cardiothoracic surgeon at UCLA, who helmed the clinical trials of so-called organ-in-the-box systems—a machine that maintains physiological conditions for an organ when it is outside the body—for the heart and lungs. “In the next decade or so, I envision that the organ we harvest is going to be very different from the organ that we’ll transplant,” he says.
Gene therapy, for example, might someday transform a donor organ so that it matches the recipient’s biology. “Imagine what the future will be like. You come in, get your new kidney, and then go home—with no need to take immunosuppressants,” Ardehali says.
Other researchers like Hanane Hadj-Moussa, a molecular biologist at the Babraham Institute in Cambridge, England, take their cues from nature—drawing inspiration for organ-preservation strategies from the wood frog and the naked mole rat, animals that can survive in environments of freezing cold or low oxygen—similar to what a human body experiences when the heart no longer circulates blood. “For example, to conserve energy during hibernation, they turn off a lot of non-essential processes,” Hadj-Moussa says. Learning how to shut down these processes in donor organs could help preserve them.
Brandacher is exploring whether anti-freeze proteins from a species of Arctic fish can prevent ice crystals—which can rupture cells—from forming in organs. He and his partners have now shown that adding anti-freeze proteins into preservation solutions allow them to store organs between minus 6 and 8 degrees Celsius, Brandacher says. His group is also using these proteins to see whether they can lower organ temperatures to minus 150 degrees Celsius—at which point, biological time stops and “we’d be able to consider organ banking.” So far, Brandacher’s research has been confined to animals, but he anticipates that studies to treat human organs with anti-freeze proteins are on the horizon in the next year or so.
Experts say advances that could heal damaged organs for transplant could potentially help patients too.
But Sestan is not yet entertaining the potential clinical implications, preferring to focus on organ transplants. His next goal is to test Organ-Ex-treated organs—including transplanting them into recipient pigs to evaluate how well they function in a live animal. “We have to be careful,” he says, “not to speculate when something can really affect and transform society.”