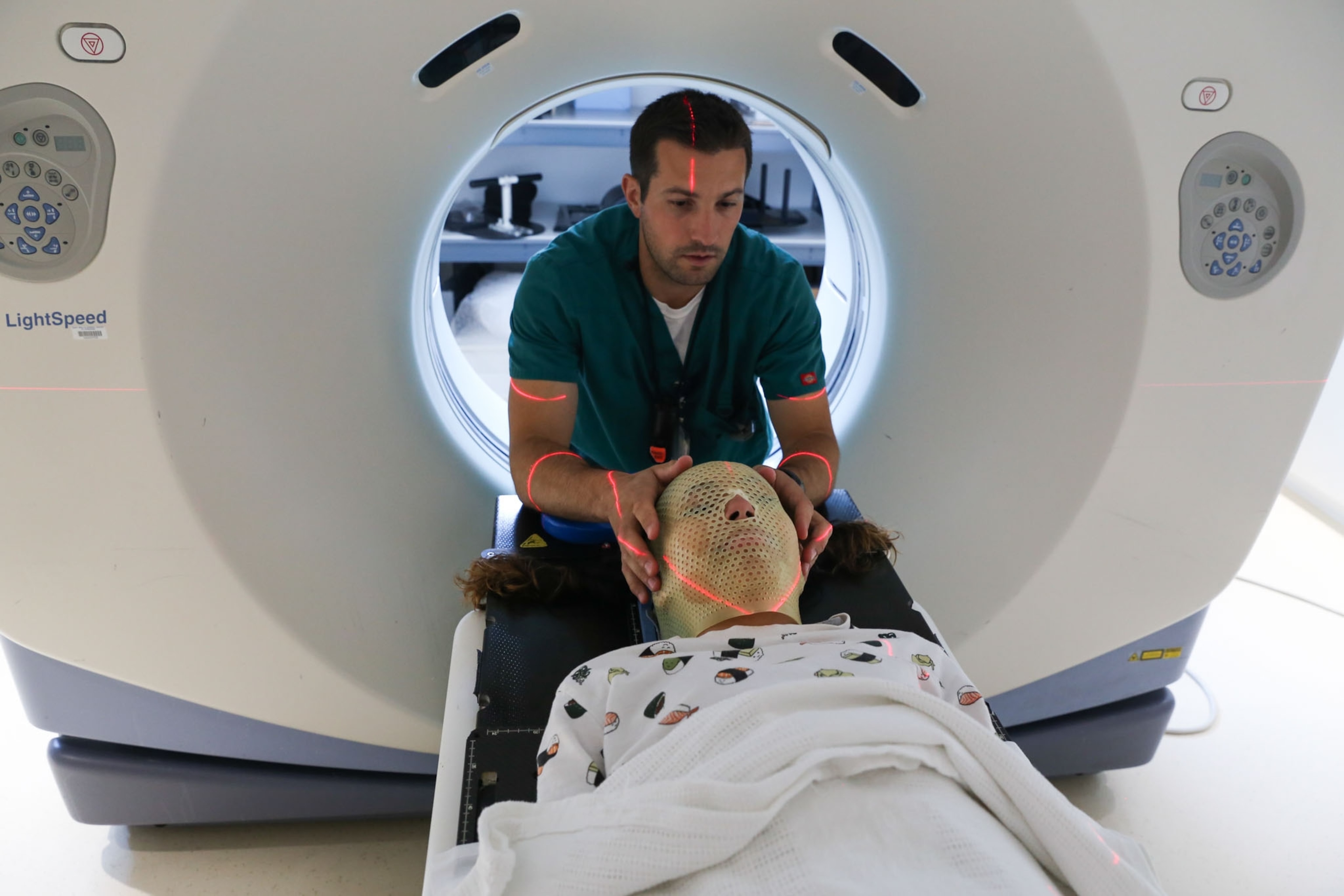
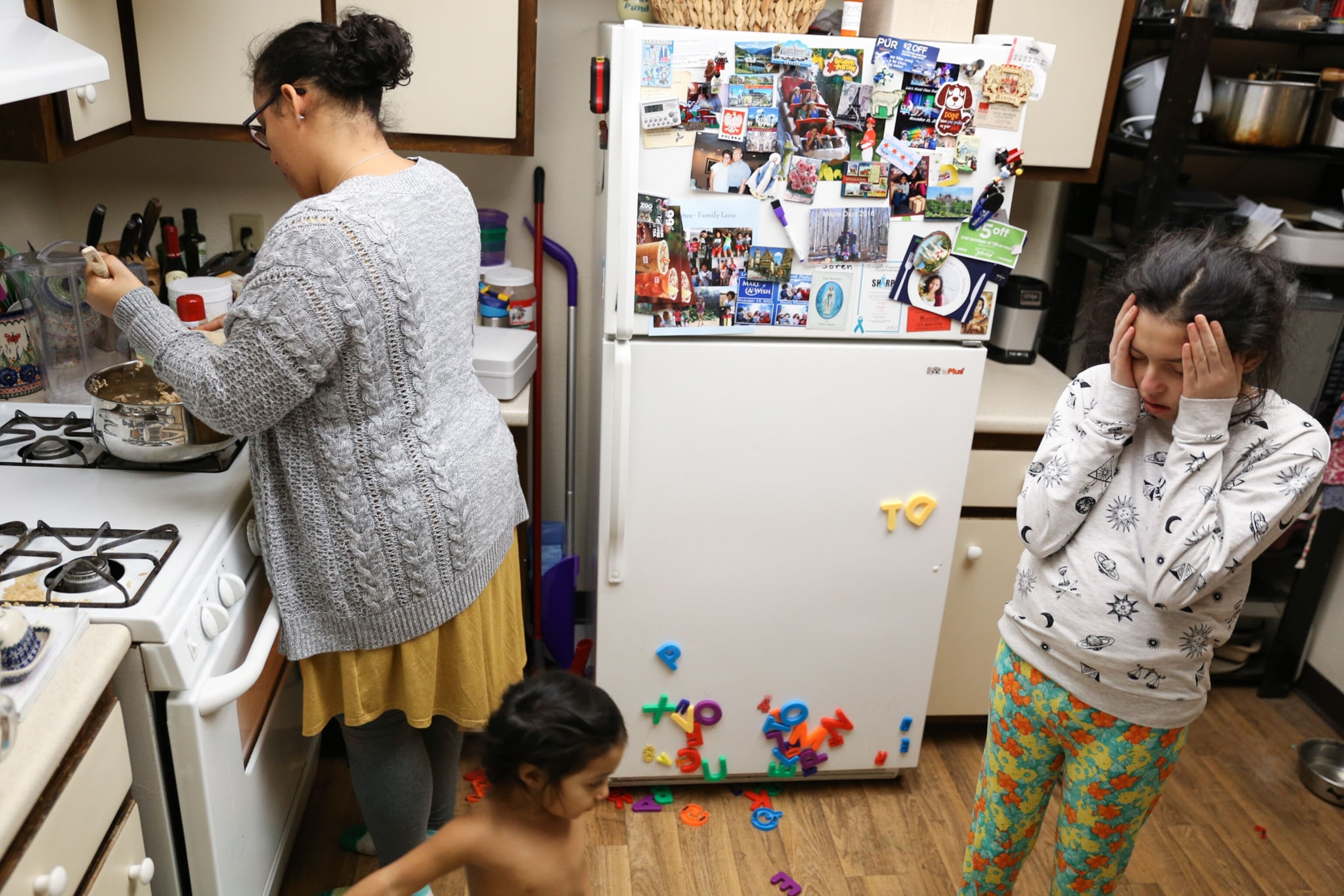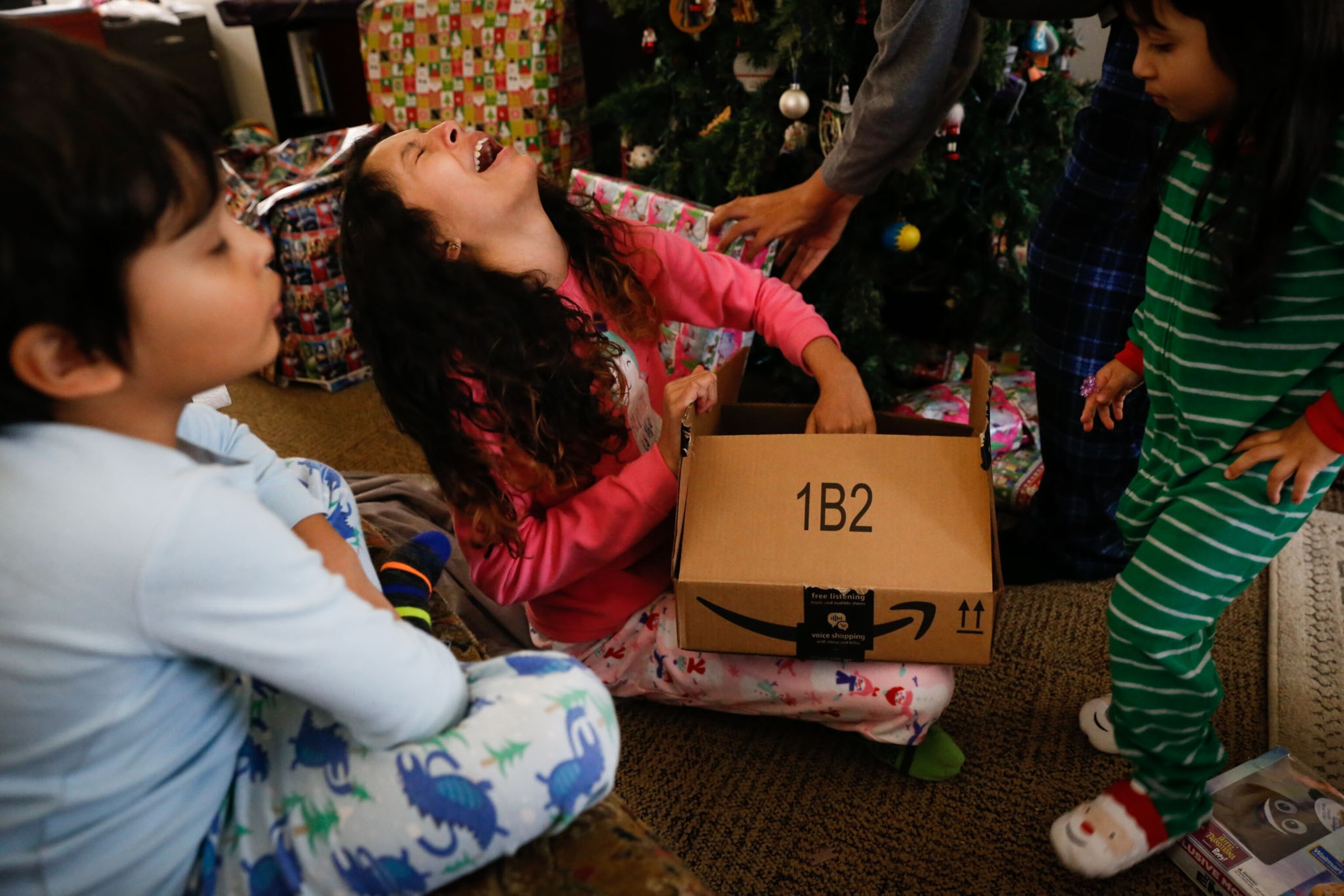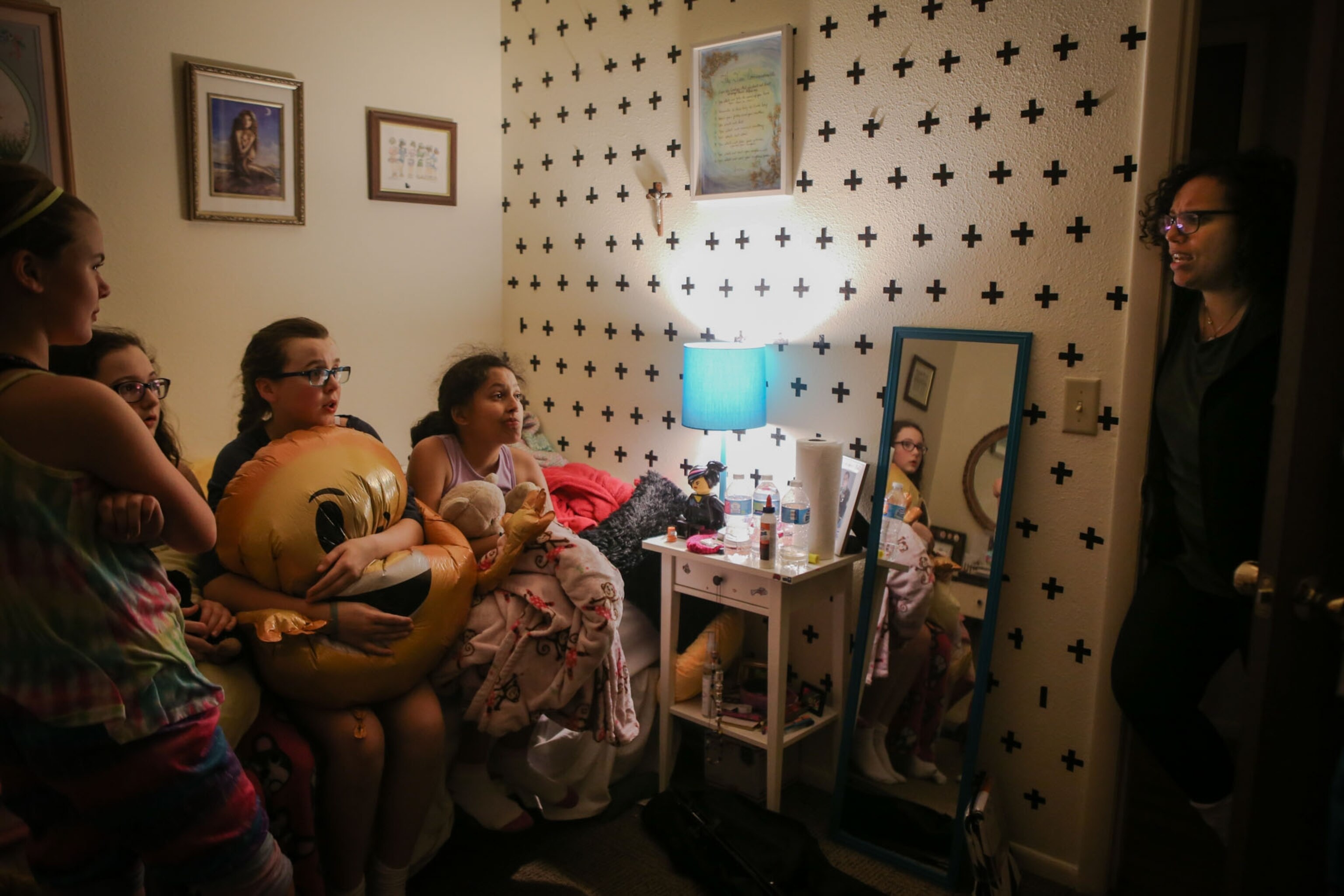At age 12, Lola Muñoz made a daunting decision: She chose to enter a clinical trial to test a new combination of chemotherapy drugs.
Lola had been diagnosed with diffuse intrinsic pontine glioma (DIPG), a rare and aggressive type of brain tumor in children that affects part of the brainstem. She knew the chances that the trial would help her condition were slim. She knew that the treatments would make her very sick. But she did it anyway.
“I wasn't doing it for me. I was doing it for all the other kids who suffered,” she told photojournalist Moriah Ratner about a month after starting the trial. Ratner spent almost a year and a half with Lola and her family capturing every aspect of their lives. Her images paint a vibrant picture of Lola's energy and passion for life—and her determination to do good.
Deadly Disease
Lola is among some 300 children diagnosed with DIPG every year. It's a deadly disease; the vast majority of patients survive for less than a year after diagnosis. The tumor grows on a part of the brainstem called the pons, which is kind of like a neural superhighway linking the nerves in the brain to the rest of the body and controlling many vital functions, including breathing and heart beating.
“In my mind it was operable. Like, you just cut it out, 'cause that’s what you do,” Melissa Muñoz, Lola's mother, told Ratner. But that's not the case with DIPG. The tumor weaves itself through the neural threads, making operation impossible.
For decades, progress with DIPG had stalled due in part to the precarious location of the tumor. Researchers had long been hesitant to take biopsies, which limited the biological understanding of DIPG, explains Melanie Comito, the pediatric hematologist and oncologist at Upstate Medical University in Syracuse, New York, who cared for Lola through much of her journey. Autopsies helped, but without a snapshot of early tumor development, scientists largely remained in the dark. Many of the early clinical tests were trial and error.
“It’s like curing cancer with a dart board,” says Keith Desserich, founder and chairman of The Cure Starts Now, a nonprofit dedicated to supporting and advancing children's cancer research.
Better biological info and a centralized database to share information have brought some answers, along with many more questions. For instance, why DIPG grows in the first place remains unknown. It doesn't seem to be genetic, nor does it have environmental causes.
Radiation therapy is the most common course of treatment, and for most patients it shrinks the tumor mass. “But radiation often just resets the clock,” says Comito. Even after radiation, it's almost guaranteed the tumor will return, generally within half a year.

Testing is still ongoing for the effectiveness of alternative treatments like chemotherapy, but the outlook is bleak. In the roughly 40 years since DIPG research began, scientists have conducted more than 250 clinical trials for new therapies. None have improved survival rates.
In recent years, though, advances in our biological understanding of the disease, coupled with the strong support of families advocating for their children, have been helping to inch the work forward.
“You don't like to hear the same narrative over and over,” says Comito. “We need the story to change.”

The Right Mix
For Lola, the problem started with what seemed to be a lazy eye. Then her face began to droop. The array of possible diagnoses that followed grew increasingly severe—Lyme disease, facial nerve palsy, and cerebral palsy, among others. Finally, the Muñoz family learned it was DIPG.
Lola went through radiation, and the family was then presented with a decision: Should she do a clinical trial?




“We felt like Lola is old enough, it’s her body” her father, Agustin Muñoz, told Ratner. “We’re not going to make decisions for her.” The family debated the risks of the three trials she qualified for, and Lola decided to head to St. Jude Children's Research Hospital in Memphis, Tennessee.
For their trial, doctors at St. Jude were searching for drugs that could halt the tumor's advancement, says Comito. Equipped with the latest biological and genetic information from autopsies and biopsies, the researchers had selected two targeted chemotherapy drugs: Crizotinib and Dasatinib.
Dasatinib was originally used to treat adult leukemia, but recent studies suggested that it might be effective against DIPG, says Alberto Broniscer, who led the clinical trial at St. Jude. Crizotinib is designed to treat lung cancer. Both are FDA approved for adults and have been individually deemed safe in children, but the drugs had never been tested in tandem. The researchers wanted to know what combined dose children can tolerate before the side effects—including nausea, headaches, vomiting, and exhaustion—became too much to bear.
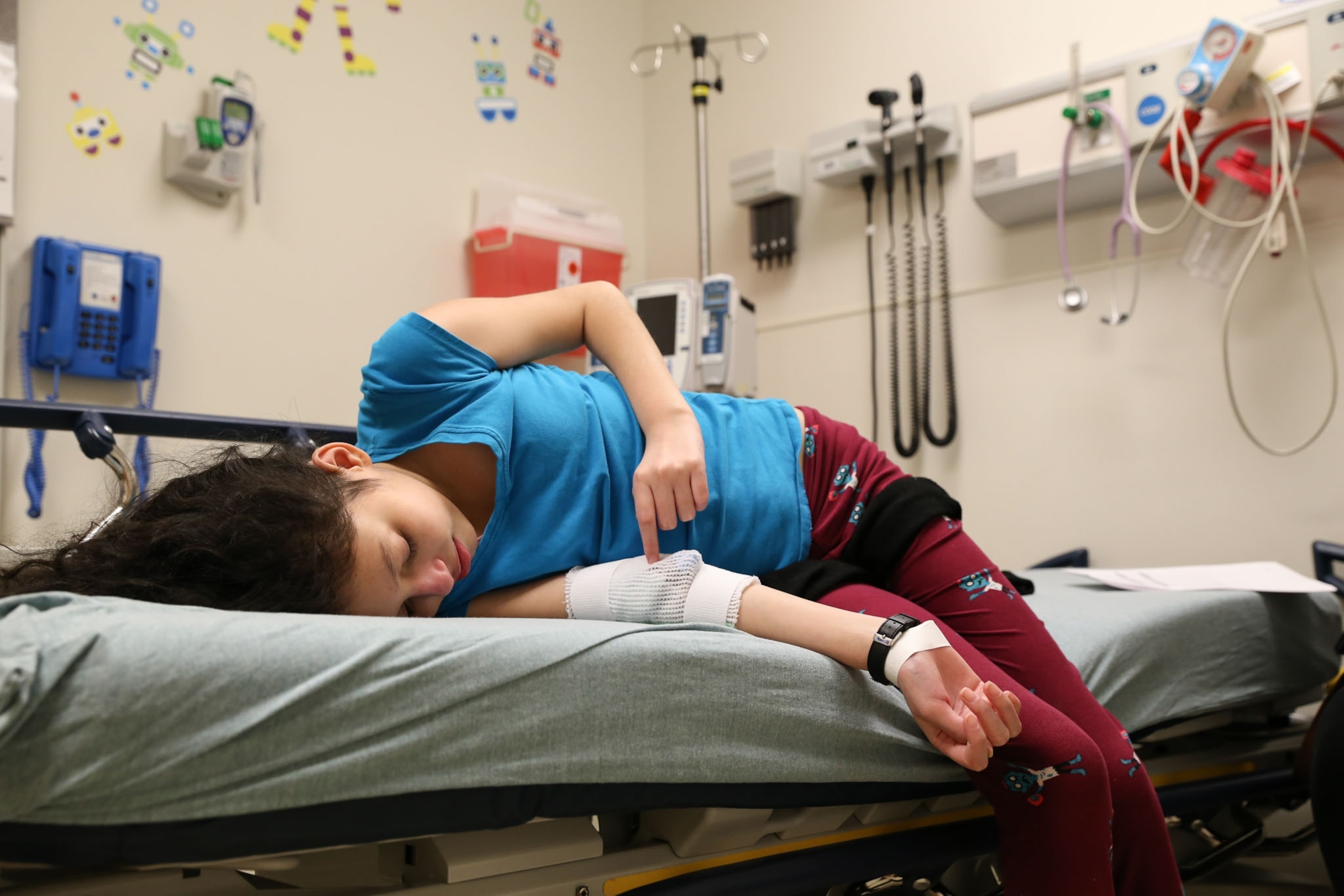
Though Lola was stalwart in her desire to help, the trial was far from easy. The chemo medications made her very sick, but she took them even knowing intense nausea and other symptoms were sure to follow.
“It kills me, because I'm ready for her to stop,” her mother told Ratner about a month after the trial began. “She's sick all the time.” Lola stuck it out for five months, but eventually she “hit her breaking point,” Ratner says.
From the first half of the trial, the researchers had learned that the cocktail of medications was too toxic to give children at the initial doses tested, says Broniscer, who is now the director of neuro-oncology at the Children's Hospital of Pittsburgh. The researchers had scaled back the doses by the time Lola joined the trial, but the results from the second phase have not yet been made public.
Racing for Answers
After she ended the trial, Lola had what's known as a honeymoon period, when she started to feel better before she declined—and she didn't waste a second. She won her school walkathon, camped at Niagara Falls, and even finished a 6K fundraiser for DIPG.
“She started off sprinting, and I couldn’t even keep up with her,” Ratner wrote in her journal after the race. “She did so well, I felt like I could see the real Lola.”

Lola died on April 2, 2018, a mere 19 months after her diagnosis—though longer than anyone expected her to live. She never wanted pity; she wanted solutions, so another child would not have to walk down the same dark path. “I want people to start thinking smarter,” she once told Ratner about DIPG research.
With each trial and test, doctors are learning more. A growing number of children and families touched by DIPG are also fighting for awareness and helping to find treatments for this deadly disease, including Lauren Hill, Piper Waneka, Michael Mosier, and more. “These are the children that are actually going to be the ones that find that cure,” Desserich says.
“In some ways, you watch these families live in a way you wish we live every day,” Comito adds. “And Lola is a perfect example of that.”