
More Than Ebola, Other Tropical Diseases Pose Growing Threat to U.S.
Three tropical diseases—dengue, chagas, and chikungunya—may establish U.S. footholds.
The United States' latest brush with Ebola shows that, more than ever, diseases are global travelers.
A physician died at a Nebraska hospital on Monday after contracting the disease in Sierra Leone, where he was working. A New York physician came down with Ebola last month after working in West Africa, sparking quarantines for returning health workers in some states. Earlier in October, a man died in Dallas after becoming infected in Liberia.
But Ebola isn't the tropical disease that's most likely to cause health problems in the United States—not by a long shot. A handful of other tropical diseases pose much more realistic threats. And they're spread by insects, which can't be quarantined.
Until now, most of the cases in the U.S. have been diagnosed in travelers. But infectious disease specialists worry that these tropical diseases could gain a foothold in local insect populations, spread to more people locally, and become a much bigger problem in the near future.
RELATED: "Graphic: As Ebola's Death Toll Rises, Remembering History's Worst Epidemics"
Here are three of the biggest threats:
Chagas Disease
Chagas disease is a parasitic disease that's spread in a particularly disgusting way: by kissing bugs that bite people's faces at night (mostly around the mouth, to which they're attracted by exhaled breath) and leave poop behind.
The parasite known as Trypanosoma cruzi, carried in the bug's feces, enters the victim's body through the bites or via the eyes or mouth. The parasite can also be spread in more ordinary ways: from mother to child, and through contaminated blood or organ donations. (The blood supply has been screened for T. cruzi since 2007.)
Chagas disease is particularly insidious because it may not cause symptoms initially. But eventually, according to the U.S. Centers for Disease Control and Prevention, 20 to 30 percent of infected people develop heart or digestive problems, some of which can be debilitating and life-threatening without treatment. An estimated six million to eight million people worldwide live with Chagas disease, which causes about 12,000 deaths a year, according to the World Health Organization.
Chagas is too rare in the U.S. to motivate big pharmaceutical companies to research and develop drugs for prevention and treatment. The CDC estimates that it affects approximately 300,000 people in the U.S., though other estimates run as high as one million.
Most patients in the U.S. acquired the parasite in their home countries—it's endemic in Latin America—before arriving in the U.S. But kissing bugs live in the southern U.S., too, and research describing five locally acquired cases in east Texas was published earlier this month in the American Journal of Tropical Medicine and Hygiene, providing new evidence that some cases are originating domestically.
Peter Hotez, the founding dean of the National School of Tropical Medicine at Baylor College of Medicine in Houston, fears that the cases reported so far are just the tip of the iceberg—or the "ears of the armadillo," he says, to use a more local metaphor—and that there's a huge need to look harder for local infections in Texas and elsewhere in the South. Many people who are infected don't know they carry the parasite.
The CDC has sought to raise awareness and improve diagnostic tools for Chagas as well as four other neglected parasitic infections (cysticercosis, toxocariasis, toxoplasmosis, and trichomoniasis). The CDC doesn't mandate that states report cases of Chagas, but four states do, including Texas.
Chagas, like other neglected parasitic infections in the U.S., is associated with poverty. Why that should be isn't entirely known, says Hotez, but substandard housing and sanitation are likely contributors.
The drugs currently used to treat the disease—the antiparasitics benznidazole and nifurtimox—are not approved by the U.S. Food and Drug Administration and need to be obtained directly from the CDC. Nonprofit groups are working to find new treatments and a vaccine.

Chikungunya
Americans traveling to the Caribbean are increasingly picking up a nasty souvenir: a case of chikungunya, a disease transmitted by mosquitoes that produces fever, joint and muscle pain, headache, lethargy, and rash. It's rarely fatal, but some cases can lead to chronic pain and arthritis. (Older patients and females seem to be at highest risk.)
Chikungunya, which the World Health Organization says was first reported in southern Tanzania in 1952, was not a problem in the Western Hemisphere until late last year, when the first local case popped up in the Caribbean, on the French side of St. Martin. It's now all over the Caribbean, and as of the end of last month there were more than 780,000 suspected cases in those islands and in the Americas.
And yes, that includes North America. In the United States alone, 1,627 cases have been reported so far this year.
Most were acquired by travelers. But in a handful of cases—11 in Florida, at the CDC's last count—the victims had never left the country. Chikungunya is not nationally reportable, but the CDC wants states to keep an eye on it, and academic and research organizations are also gathering data.
"What happens is that people come back from the Caribbean to Florida with virus in their blood," explains Stephen Higgs, director of the Biosecurity Research Institute at Kansas State University, in Manhattan. "Local mosquitoes feed on them, and then develop an infection." Then those mosquitoes bite someone else.
The chikungunya virus is carried by two types of mosquitoes, the yellow fever mosquito and the Asian tiger mosquito. So far—luckily—the virus strain circulating in the Americas is primarily spread by the less-common yellow fever mosquito (Aedes aegypti).
But what if that virus mutates and comes to prefer the Asian tiger mosquito? That's what scientists worry about, since the Asian tiger mosquito (Aedes albopictus) has a much wider geographical range in the United States, reaching as far north as New Jersey, New York, and Pennsylvania.
It's also more of an all-day eater, says Rebecca Christofferson, a research assistant professor and infectious disease specialist at Louisiana State University, in Baton Rouge. That raises the question of whether chikungunya could someday become as common in the U.S. as the more familiar West Nile virus.
Luckily, says Higgs, chikungunya doesn't hide out in the local bird and mammal population the way West Nile does, which means it might be easier to stop, since focusing on the mosquito vector would be effective.
There's no treatment for chikungunya, and no vaccine, though researchers are working on that. For now, the key to keeping a lid on the disease is mosquito eradication. That involves spraying by local authorities and individuals taking steps to protect themselves: avoiding bites with approved insect repellants, wearing long-sleeved shirts, getting rid of stagnant water on their property, and staying away from mosquito-infested areas.

Dengue
More familiar than Chagas or chikungunya is dengue, the mosquito-borne virus that the World Health Organization estimates infects some 100 million people per year around the world. That's just the active cases; according to an estimate published last year in Nature, there are 96 million active infections per year, with another 294 million that are mild or asymptomatic. Dengue is a reportable disease in the U.S.
Symptoms include intense joint and muscle pain (the disease is commonly known as "breakbone fever"), as well as high fever, headache, and eye pain. It can progress to severe dengue or dengue hemorrhagic fever. If untreated, people can die from shock, as the capillaries start to leak blood into the abdomen and chest cavity.
Severe dengue has a mortality rate of about one percent with early detection and supportive treatment such as fluid replacement, and 10 to 20 percent without.
The more serious dengue hemorrhagic fever often does not occur until the second time someone is infected. And that's where the danger lies.
The dengue virus has four variations, known as serotypes. Often the first infection is relatively mild, and can even be hidden altogether and cause no symptoms. So the fear, as Christofferson explains, is that people will be infected once—knowingly or not—and then somewhere down the line, if another strain comes to town, they can become dangerously ill.
Like chikungunya, dengue is spread by mosquitoes—in this case, mostly the yellow fever variety. As with chikungunya, dengue is usually found in travelers. Dengue is common in Southeast Asia, the western Pacific islands, and Latin America.
But local mosquitoes can also pick up the disease from infected travelers and spread it to people in the U.S. Locally acquired dengue cropped up in outbreaks in Florida and Texas in 2013, raising the specter of further geographic spread in the South, where the mosquito typically lives—or elsewhere, if its range expands. It already shows signs of expanding: Yellow fever mosquitoes were found in California in 2013.
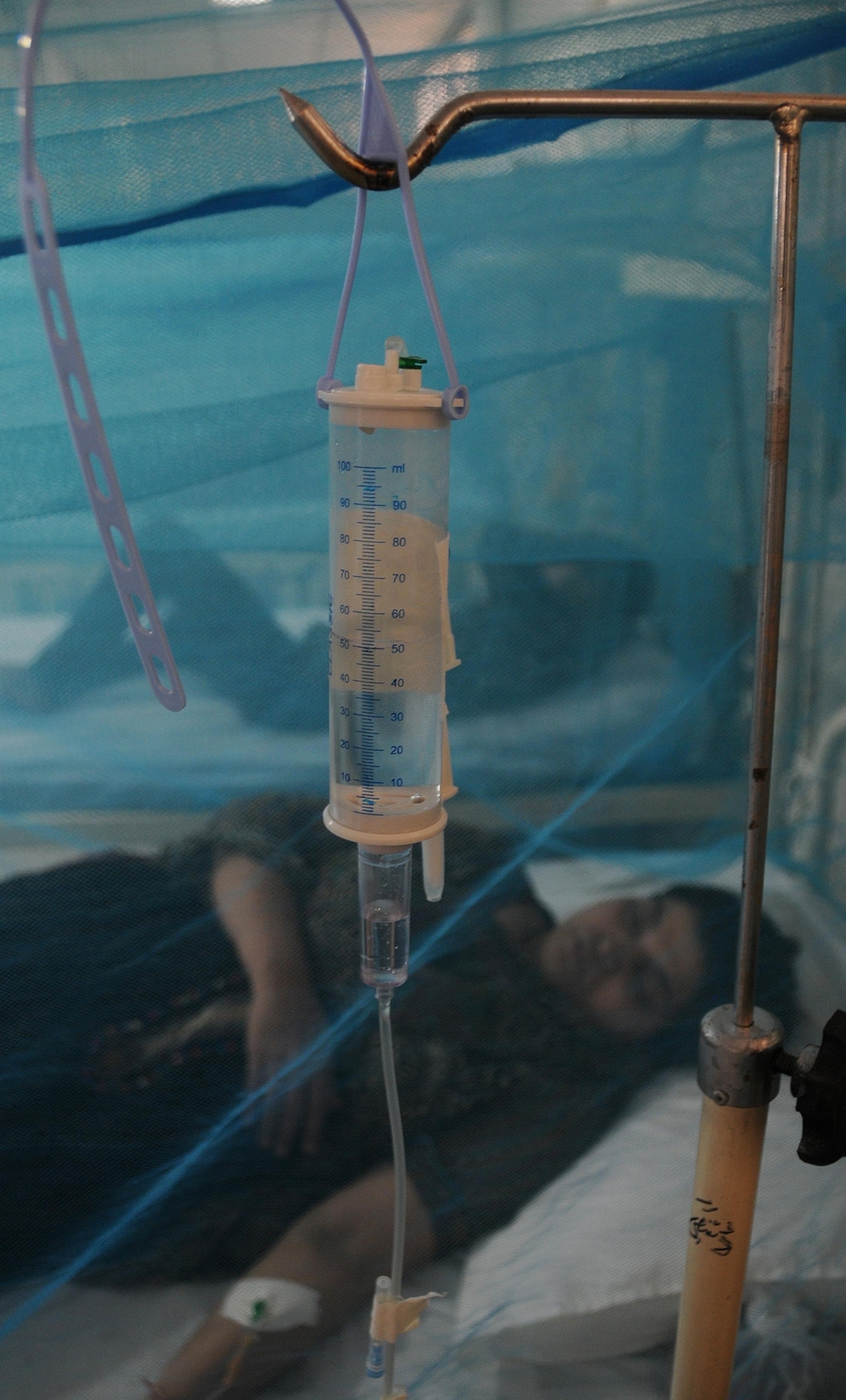
As with chikungunya, the key to stamping out dengue is mosquito control. Researchers in Australia are trying a novel strategy: releasing mosquitoes infected with a bacterium that prevents them from transmitting dengue. And a vaccine is on the horizon.
What's most worrisome to researchers is how much is still unknown about all three of these infections.
"What does it take to break the transmission cycle?" asks Christofferson. "And what does it take to break the cycle at different points?" Until such questions are answered, Chagas, chikungunya, and dengue loom as significant potential threats to U.S. residents.